Chronic constipation is common in adults older than 60 years, and symptoms occur in up to 50% of nursing home residents. Primary constipation is also referred to as functional constipation. Secondary constipation is associated with chronic disease processes, medication use, and psychosocial issues. Fecal impaction should be treated with mineral oil or warm water enemas. Most patients are initially treated with lifestyle modifications, such as scheduled toileting after meals, increased fluid intake, and increased dietary fiber intake. Additional fiber intake in the form of polycarbophil, methylcellulose, or psyllium may improve symptoms. Fiber intake should be slowly increased over several weeks to decrease adverse effects. The next step in the treatment of constipation is the use of an osmotic laxative, such as polyethylene glycol, followed by a stool softener, such as docusate sodium, and then stimulant laxatives. Long-term use of magnesium-based laxatives should be avoided because of potential toxicity. If symptoms do not improve, a trial of linaclotide or lubiprostone may be appropriate, or the patient may be referred for further diagnostic evaluation. Peripherally acting mu-opioid antagonists are effective for opioid-induced constipation but are expensive.
Chronic constipation occurs in 16% of adults, with older patients experiencing constipation more often.1 About one-third of adults 60 years or older report at least occasional constipation1, and in nursing home residents, the prevalence is 50% or more.2 Approximately 33 million adults in the United States have constipation resulting in 2.5 million physician visits and 92,000 hospitalizations each year.3
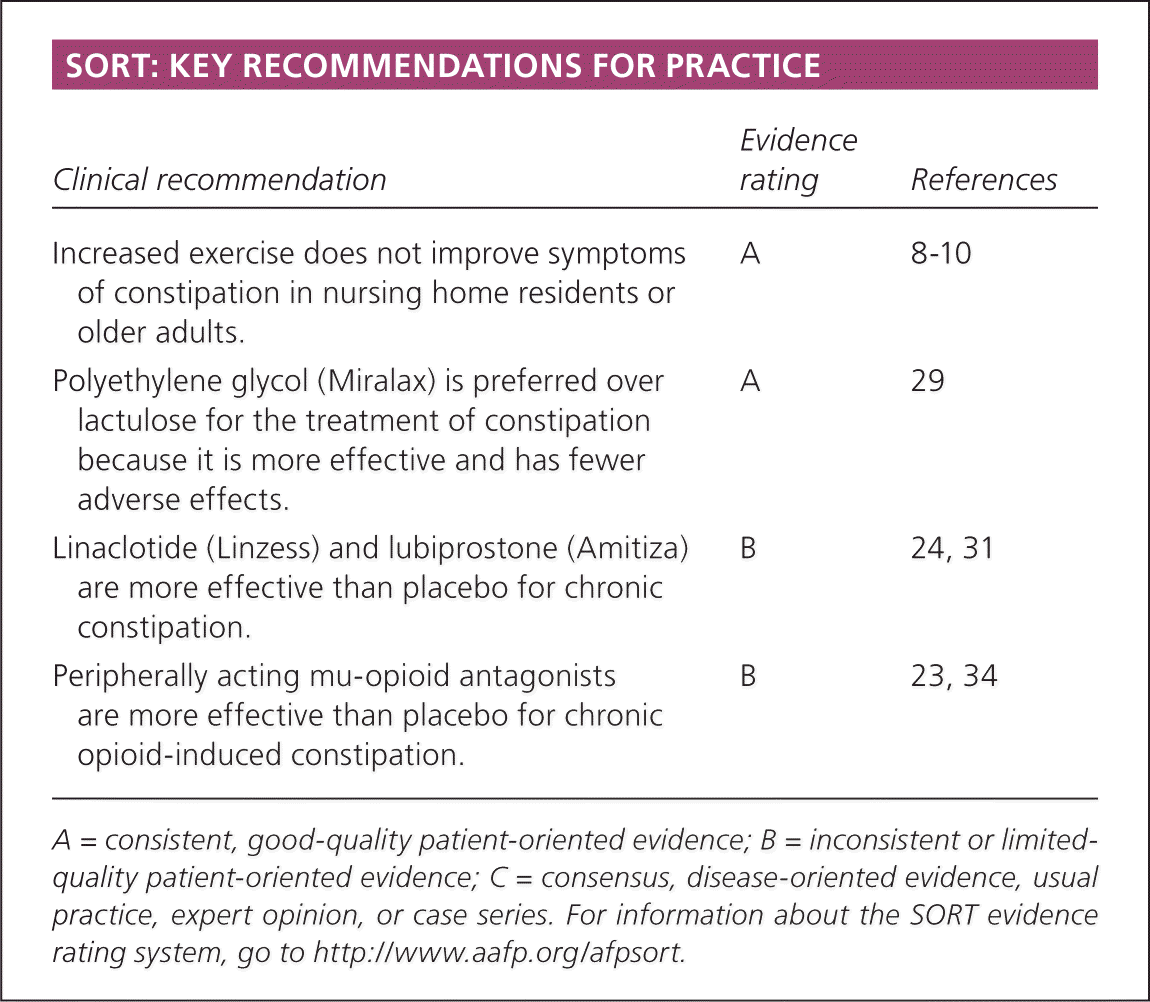
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Increased exercise does not improve symptoms of constipation in nursing home residents or older adults. | A | 8–10 |
| Polyethylene glycol (Miralax) is preferred over lactulose for the treatment of constipation because it is more effective and has fewer adverse effects. | A | 29 |
| Linaclotide (Linzess) and lubiprostone (Amitiza) are more effective than placebo for chronic constipation. | B | 24, 31 |
| Peripherally acting mu-opioid antagonists are more effective than placebo for chronic opioid-induced constipation. | B | 23, 34 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Definitions
Constipation is a clinical diagnosis based on symptoms of incomplete elimination of stool, difficulty passing stool, or both. Patients typically experience other symptoms such as hard stools, abdominal bloating, pain, and distention. Constipation may be present with normal stool frequency, defined as at least one stool three times per week, or with daily bowel movements.1 Chronic constipation is characterized by the presence of symptoms for at least three months out of the preceding 12 months.
PRIMARY CONSTIPATION
Primary constipation, or functional constipation, is classified into three subtypes: normal transit constipation, slow transit constipation, and disorders of defecation. Often, more than one subtype occurs simultaneously.4 Normal transit constipation is the most common. Patients report hard stool or difficulty with defecation, but have normal stool frequency.4 Slow transit constipation, caused by abnormal innervation of the bowel or visceral myopathy, leads to increased transit time of stool through the colon with infrequent defecation, bloating, and abdominal discomfort.5 Disorders of defecation can occur in any age group but are particularly common in older patients.6 Defecation may be impaired by decreased smooth muscle contraction in the rectum or the inability to relax the muscles of defecation. In older adults, rectal receptors may have a diminished response to stretching, blunting the urge to defecate despite accumulation of large quantities of stool.
SECONDARY CONSTIPATION
Causes of secondary constipation include medication use, chronic disease processes, and psychosocial issues. A previous article in American Family Physician reviewed the diagnostic approach to chronic constipation in older adults (https://www.aafp.org/afp/2011/0801/p299.html).
Initial Management
Clinicians should discuss goals of treatment with patients and caregivers. The primary goal should be symptom improvement, and the secondary goal should be the passage of soft, formed stool without straining at least three times per week.4 Initially, any fecal impaction should be treated with enemas or manual disimpaction. Fecal impaction is suggested by a history of constipation with overflow diarrhea, and is confirmed by rectal examination with a plain abdominal radiograph, if needed.
Nonpharmacologic Interventions
BEHAVIORAL INTERVENTIONS
To take advantage of the gastrocolic reflex, patients should schedule toileting after meals.4 They should place their feet on a small step stool instead of on the floor to straighten the anorectal junction. Patients in long-term care facilities should be allowed adequate time and privacy for bowel movements, and should avoid using bedpans to defecate.7
Exercise programs do not improve symptoms of constipation in nursing home residents and older adults8–10; however, lifestyle education, including exercise and advice on increasing fluid and fiber intake, decreased constipation in one small study.11
There are no randomized controlled trials (RCTs) evaluating the benefit of water supplementation alone to treat constipation, although water supplementation totaling 1.5 to 2 L per day improved stool frequency in middle-aged adults on a high-fiber diet.12
The recommended daily fiber intake is 20 to 35 g per day. Intake should be slowly increased over several weeks to decrease adverse effects, including flatulence, abdominal cramping, and bloating.13
BIOFEEDBACK
Biofeedback to retrain the defecation muscles may be effective for treating constipation caused by pelvic floor dysfunction. With this technique, anorectal electromyography or a manometry catheter is used to give patients feedback when evacuating a rectal balloon. One systematic review concluded that there is insufficient evidence from high-quality trials to support the effectiveness of biofeedback.14 Since the publication of this review, a randomized trial of 88 persons with obstructive constipation found that biofeedback-guided pelvic floor exercises were superior to polyethylene glycol (PEG; Miralax) in improving constipation symptoms at six-month follow-up.15 Biofeedback may be appropriate for patients who are physically and mentally capable of participating.
Pharmacologic Treatment
Most older adults with chronic constipation eventually require a laxative to alleviate symptoms. A systematic review of laxative treatment in older persons showed varying degrees of effectiveness and concluded that therapy should be individualized.16 There are limited data on long-term use of medications for constipation in older persons. Medications for constipation are listed in Table 1.16–24 Figure 1 provides a suggested approach to the management of chronic constipation in older adults. In patients with a poor response to behavioral interventions and laxatives, referral may be warranted for assessment of colonic transit times and for rectal manometry to evaluate for disorders of defecation.
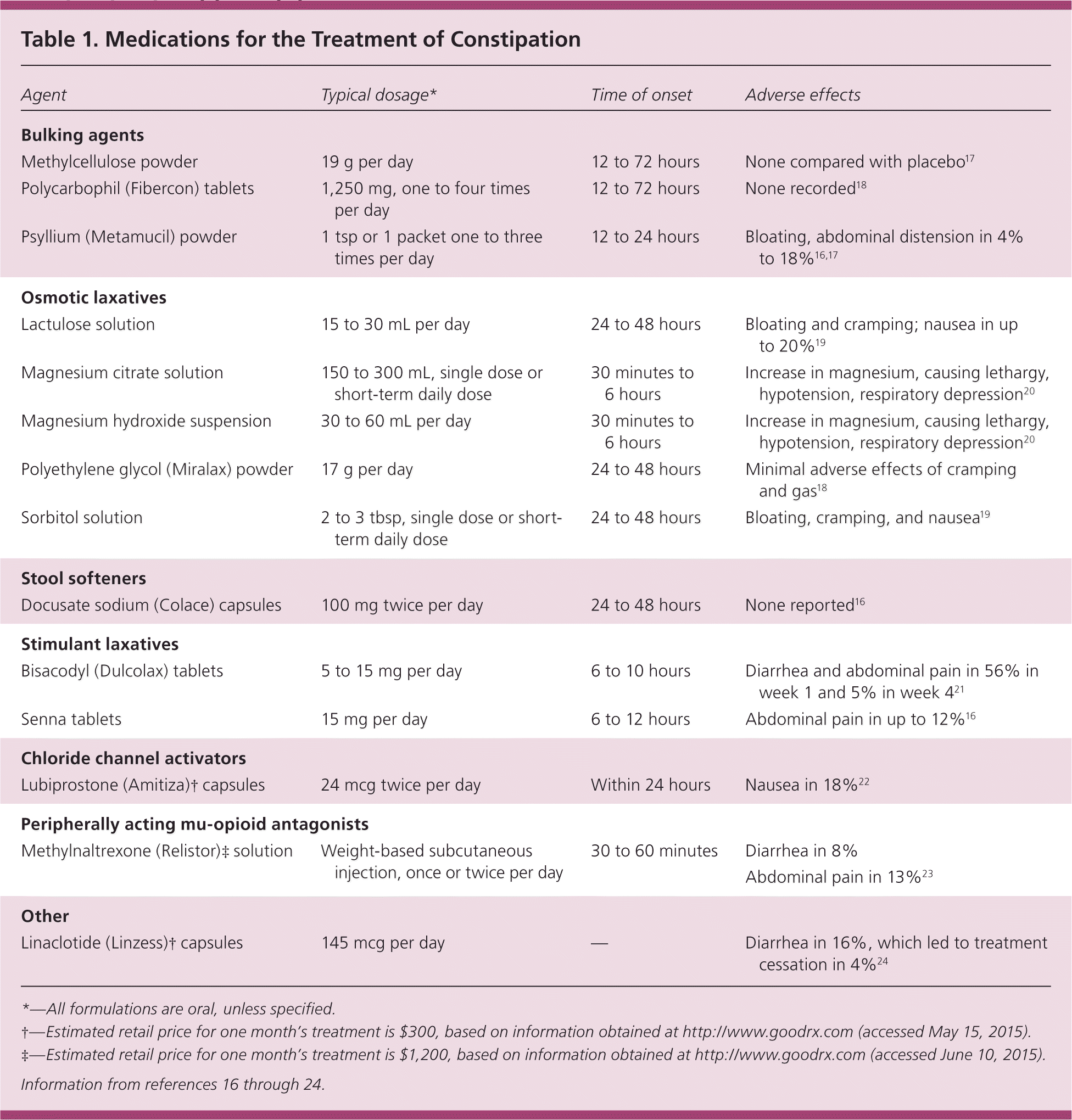
Table 1. Medications for the Treatment of Constipation
| Agent | Typical dosage* | Time of onset | Adverse effects |
|---|---|---|---|
| Bulking agents | |||
| Methylcellulose powder | 19 g per day | 12 to 72 hours | None compared with placebo17 |
| Polycarbophil (Fibercon) tablets | 1,250 mg, one to four times per day | 12 to 72 hours | None recorded18 |
| Psyllium (Metamucil) powder | 1 tsp or 1 packet one to three times per day | 12 to 24 hours | Bloating, abdominal distension in 4% to 18%16,17 |
| Osmotic laxatives | |||
| Lactulose solution | 15 to 30 mL per day | 24 to 48 hours | Bloating and cramping; nausea in up to 20%19 |
| Magnesium citrate solution | 150 to 300 mL, single dose or short-term daily dose | 30 minutes to 6 hours | Increase in magnesium, causing lethargy, hypotension, respiratory depression20 |
| Magnesium hydroxide suspension | 30 to 60 mL per day | 30 minutes to 6 hours | Increase in magnesium, causing lethargy, hypotension, respiratory depression20 |
| Polyethylene glycol (Miralax) powder | 17 g per day | 24 to 48 hours | Minimal adverse effects of cramping and gas18 |
| Sorbitol solution | 2 to 3 tbsp, single dose or short-term daily dose | 24 to 48 hours | Bloating, cramping, and nausea19 |
| Stool softeners | |||
| Docusate sodium (Colace) capsules | 100 mg twice per day | 24 to 48 hours | None reported16 |
| Stimulant laxatives | |||
| Bisacodyl (Dulcolax) tablets | 5 to 15 mg per day | 6 to 10 hours | Diarrhea and abdominal pain in 56% in week 1 and 5% in week 421 |
| Senna tablets | 15 mg per day | 6 to 12 hours | Abdominal pain in up to 12%16 |
| Chloride channel activators | |||
| Lubiprostone (Amitiza)† capsules | 24 mcg twice per day | Within 24 hours | Nausea in 18%22 |
| Peripherally acting mu-opioid antagonists | |||
| Methylnaltrexone (Relistor)‡ solution | Weight-based subcutaneous injection, once or twice per day | 30 to 60 minutes |
|
| Other | |||
| Linaclotide (Linzess)† capsules | 145 mcg per day | — | Diarrhea in 16%, which led to treatment cessation in 4%24 |
*—All formulations are oral, unless specified.
†—Estimated retail price for one month's treatment is $300, based on information obtained at http://www.goodrx.com (accessed May 15, 2015).
‡—Estimated retail price for one month's treatment is $1,200, based on information obtained at http://www.goodrx.com (accessed June 10, 2015).
Figure 1. Management of Chronic Constipation in Older Adults
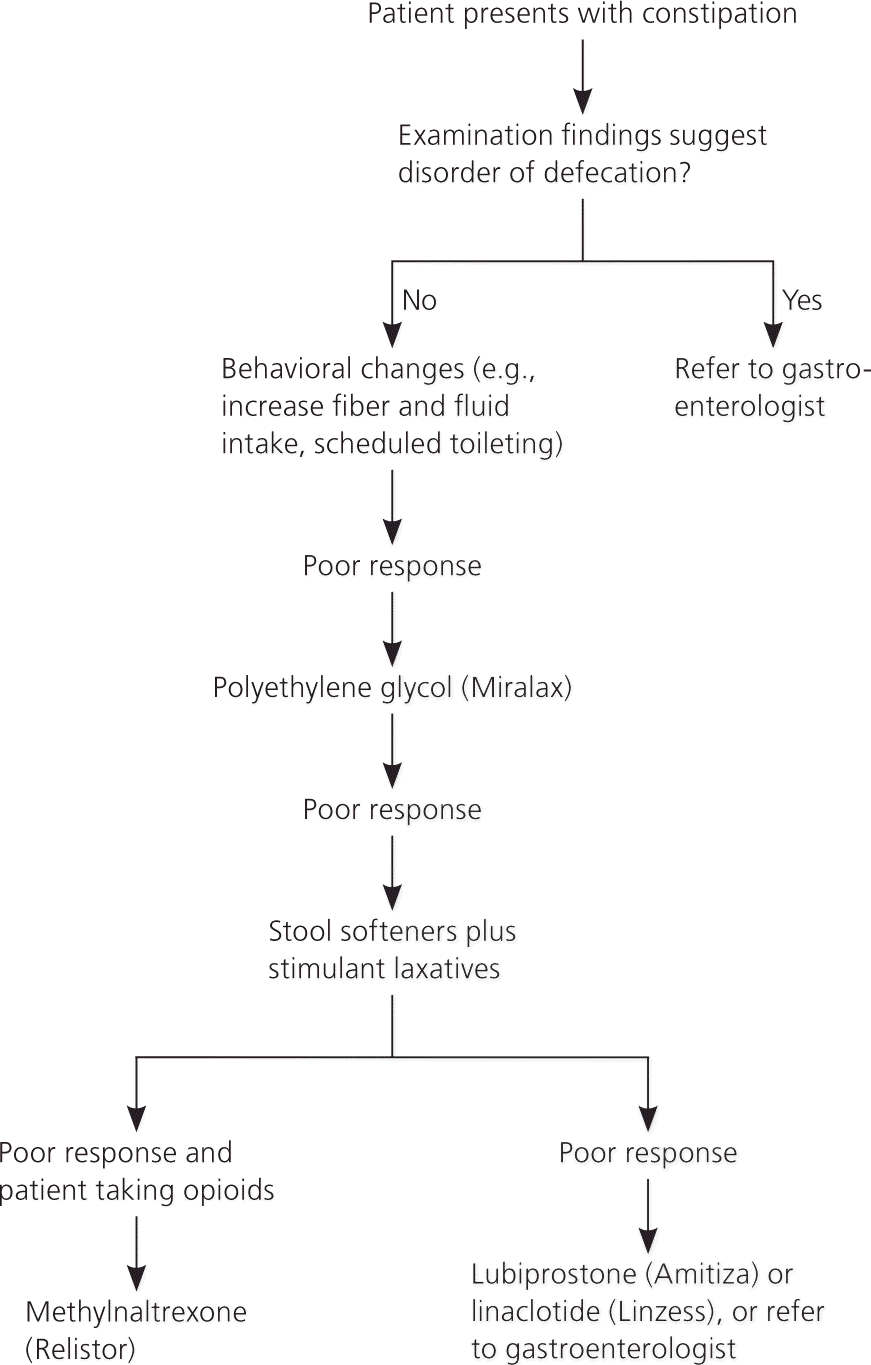
Suggested approach to management of chronic constipation in older adults.
ENEMAS AND SUPPOSITORIES
Enemas and suppositories can be useful for fecal impaction or in patients who cannot tolerate oral preparations. Phosphate enemas should be avoided in older adults because of the high risk of electrolyte disturbances, which are sometimes fatal.25 Mineral oil enemas are a safer alternative to phosphate enemas, with local adverse effects of perianal irritation or soreness. Plain warm water enemas are safe and preferable to soapsuds enemas, which may cause rectal mucosa damage.2 Glycerin suppositories are safe alternatives to enemas and have been shown to improve rectal emptying in patients with chronic constipation.26
BULKING AGENTS
Bulking agents may be soluble, such as psyllium (Metamucil), or insoluble, such as bran, methylcellulose (Citrucel), and polycarbophil (Fibercon). These agents absorb water into the intestine to soften the stool and increase bulk. Bran and psyllium improve stool frequency in older patients,18 but there is more evidence for the effectiveness of psyllium than bran in persons of all ages.17 A few small studies in older adults demonstrated equivalent effectiveness of methylcellulose and polycarbophil to psyllium.16 Adverse effects such as bloating, abdominal distention, and gas are more common with psyllium.27 Bulk laxatives should be avoided if fecal impaction is present.
OSMOTIC LAXATIVES
Osmotic laxatives are not absorbable. These laxatives draw water into the intestinal lumen. Lactulose and sorbitol are hyperosmolar sugar alcohols that increase frequency of defecation and reduce straining. They are metabolized by colonic bacteria and then absorbed by colonic mucosa. An RCT of 30 men 65 to 86 years of age showed that sorbitol and lactulose were equally effective in treating constipation.19 Another RCT of nursing home residents with an average age of 85 years found that lactulose was more effective than placebo.28 Lactulose may cause diarrhea in patients who are lactose intolerant.
PEG is an iso-osmotic agent that has been consistently effective in the treatment of constipation.18 A meta-analysis of PEG vs. lactulose for the treatment of chronic constipation in adults up to 75 years of age showed that PEG is more effective and led to fewer adverse effects than lactulose.29 A small RCT comparing PEG with ispaghula husk (psyllium) showed that PEG was more effective, with a more rapid onset of action.30
The effectiveness and safety of magnesium salts, such as magnesium hydroxide and magnesium citrate, have not been well studied in older adults. Magnesium toxicity is a concern with long-term use of these agents; it can cause ileus and worsen constipation. Magnesium salts should be avoided in patients with renal failure. Because of the limited data and potential harm, long-term use of magnesium salts is not recommended.
STOOL SOFTENERS
Three RCTs involving older patients showed a benefit of docusate sodium (Colace) over placebo in the treatment of constipation.16
STIMULANT LAXATIVES
Senna and bisacodyl (Dulcolax) promote intestinal motility and increase fluid secretion into the bowel. One RCT found bisacodyl to be more effective than placebo for chronic constipation; however, the average age of study participants was 55 years.21 Because of the possible adverse effects of long-term use in older persons, stimulant laxatives should be used only after fiber and osmotic laxatives have been tried. Long-term use of stimulant laxatives containing anthraquinone, such as senna, causes melanosis coli, which is a reversible histologic finding of brown pigmentation in the colonic mucosa.
OTHER AGENTS
Lubiprostone (Amitiza), a chloride channel activator that moves water into the intestinal lumen, is approved by the U.S. Food and Drug Administration for long-term treatment of chronic constipation in adults. It is effective and moderately well tolerated in older adults.16 A subgroup analysis of 163 patients older than 65 years found that nausea was the most common adverse effect, occurring in 18% of patients.22 In one study of patients with constipation after orthopedic surgery, lubiprostone was as effective as senna.31 Lubiprostone may be reserved for constipation that does not respond to less expensive treatment options.
Linaclotide (Linzess) increases intestinal fluid secretion and motility. It is approved by the U.S. Food and Drug Administration for chronic constipation and irritable bowel syndrome. Studies with patients up to 86 years of age showed increased frequency of bowel movements and decreased abdominal pain. Diarrhea is the most common adverse effect and led to cessation of treatment in 4% of patients.24
Probiotics. A systematic review of five RCTs found that probiotics did not improve constipation in adults.32
Peripherally Acting mu-Opioid Antagonists. These agents include methylnaltrexone (Relistor), alvimopan (Entereg), and naloxegol (Movantik), which decrease the gastrointestinal effects of opioids without reducing centrally mediated analgesia, and naloxone, which is also effective for constipation but can decrease analgesia. Up to 40% of patients taking opioids are constipated; of these, only 46% have an acceptable response to laxatives more than 50% of the time.33 A systematic review of studies with patients up to 78 years of age who had malignant or nonmalignant pain found that methylnaltrexone, naloxone, and alvimopan were more effective than placebo for chronic opioid-induced constipation.23 Methylnaltrexone is administered subcutaneously and is effective for opioid-induced constipation in palliative care patients with symptoms resistant to other laxatives.34 Methylnaltrexone should not be used in patients with intestinal obstruction and should be used with caution in patients with intestinal malignancy. Alvimopan, approved for short-term treatment of postoperative ileus, is available only through a restricted prescribing program because of increased risk of myocardial infarction. Naloxegol is administered orally and is approved for opioid-induced constipation in patients who do not have cancer. Peripherally acting mu-opioid antagonists are expensive, and should be used only when other options are ineffective.
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or reflecting the views of the Department of Defense, the U.S. Army Medical Corps, or the U.S. Army at large.
Data Sources: A PubMed search was completed in Clinical Queries using the key terms constipation and elderly. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. Also searched were the Cochrane database, Database of Abstracts of Reviews of Effects, TRIP database, the National Guideline Clearinghouse database, and UpToDate. Search dates: August 2014 and June 2, 2015.

