Article: Nutrition Myths and Healthy Dietary Advice in Clinical Practice
Issue Date: May 1, 2015
See additional reader comments at: https://www.aafp.org/afp/2015/0501/p634.html
to the editor: Lesser and colleagues should be commended for addressing nutrition, an often neglected subject in family medicine. However, I question the assertion that consuming whole foods containing saturated fat is inversely associated with incident cardiovascular disease and type 2 diabetes mellitus. Although they suggest that consuming more dietary fiber in the form of whole foods may help prevent cardiovascular disease and diabetes, they do not advise an upper limit for saturated fatty acid (SFA) intake. These recommendations may cause patients to replace high-fiber whole plant foods with foods containing SFAs and protein, resulting in meat-based “low-carb” diets, which are associated with greater all-cause mortality (Table 1).1
Table 1. Adjusted risk ratios for all-cause mortality associated with low-carbohydrate diets. Analysis was based on low-carbohydrate and low-carbohydrate/high-protein scores. Boxes = estimated risk ratios; bars = 95% CIs; diamonds = random-effects model risk ratios; width of diamonds; pooled CIs. The size of each box is proportional to the weight of each study in the meta-analysis. (CI = confidence interval.)
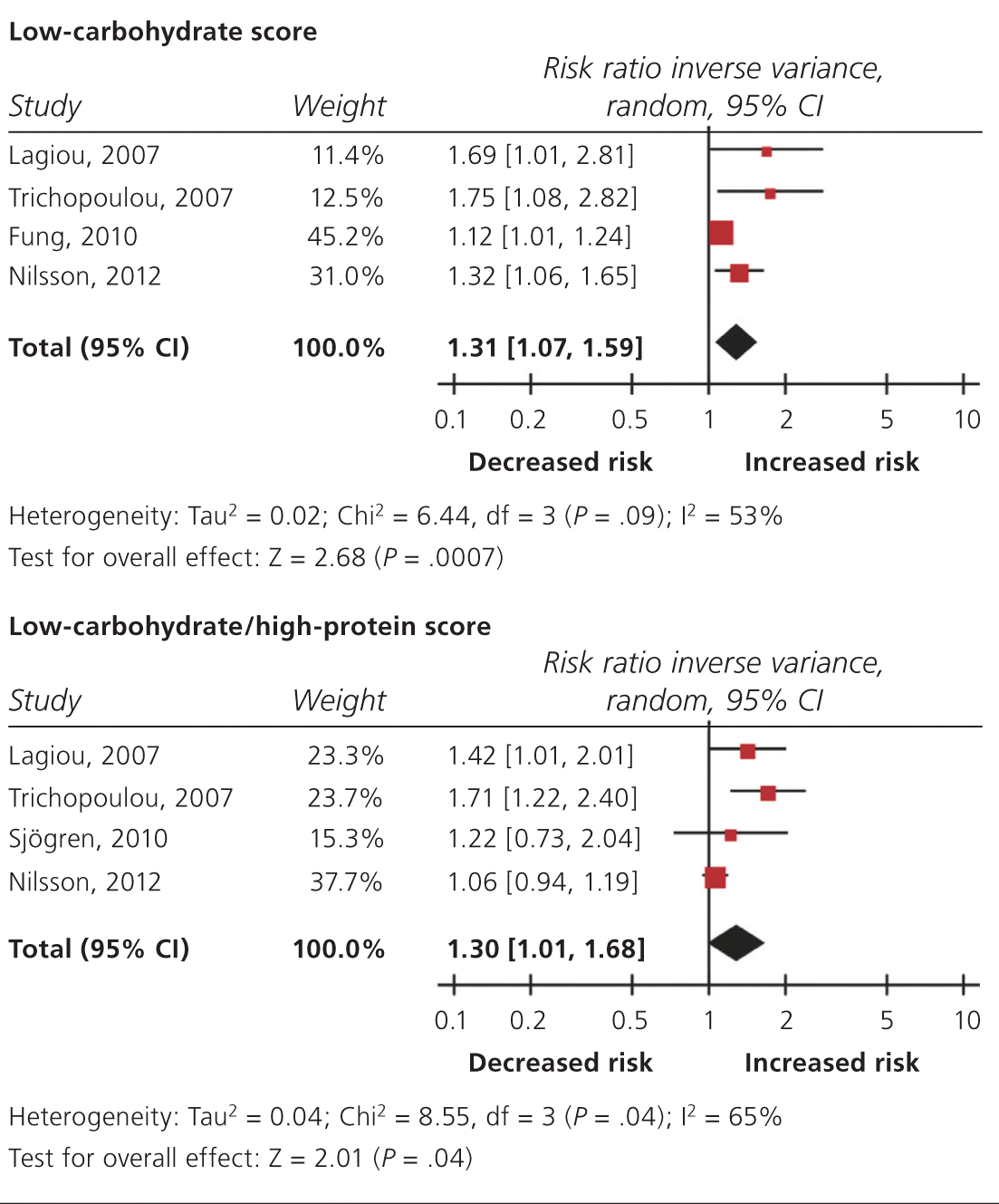
Adapted from Noto H, et al. Low-carbohydrate diets and all-cause mortality: a systematic review and meta-analysis of observational studies. PLoS One. 2013;8(1):e55030.
Although the authors highlight the association between processed meat and cardiovascular and all-cause mortality, two of their references show a similar association for unprocessed meat. One study observed dose-response relationships for unprocessed and processed meat across mortality categories,2 and the other reported a 31% increase in risk of cardiovascular disease for each 5 g per day of total energy from meat SFA.3 Although the authors' proposed alternatives to processed foods (pastured meat or eggs, wild game) contain a more favorable fatty acid profile, no evidence shows any patient-oriented benefit over unprocessed meat.
Although pointing out that simply substituting SFAs with refined carbohydrates does not improve outcomes, the authors dispute the value of substituting SFAs with polyunsaturated fatty acids. The cited Cochrane review concluded the exact opposite: “Lifestyle advice to all those at risk of cardiovascular disease … should continue to include permanent reduction of dietary saturated fat and partial replacement by unsaturates.”4 The review found a 14% reduction in cardiovascular events at six months after reducing SFA by reducing and/or modifying dietary fat, along with other lifestyle changes, and this increased to 22% after two years. This relative risk reduction is comparable to that achieved by pharmacologic treatment of mild to moderate hypertension.
Finally, the authors state that consuming dairy foods may lower the risk of type 2 diabetes, obesity, and cardiovascular disease. However, two of the provided meta-analyses supporting this assertion have coauthors funded by the National Dairy Council, and more recent studies about dairy have been mixed.5,6 Such a body of evidence is not sufficient to disregard American College of Cardiology and American Heart Association recommendations to not exceed 6% of total calories from SFAs, or the American Diabetes Association's recommended upper limit of 10%.
in reply: We thank Dr. Sherwood for the letter and hope he and other readers take away from our article that humans should eat mostly plants in minimally processed form. That said, individuals can include foods from animals if they choose and still have a healthy diet. Dr. Sherwood worries that we do not set a limit for SFA intake. One reason we do not is that SFAs are a heterogeneous group of compounds with nonuniform effects.1 It makes little sense to lump different SFAs in a group (just as it would make little sense to lump SFAs in a group with unsaturated fatty acids). Nonetheless, many studies consider SFAs collectively. Perhaps the most rigorous review of such studies found no effects on cardiovascular or all-cause mortality with reduction of SFAs or with substituting saturated fat with other fats.2 The abstract of this review makes the recommendation Dr. Sherwood notes, but the only direct association with SFAs in the text is to cardiovascular events, and this association was statistically insignificant when authors removed biased studies (i.e., those having differences between intervention and control arms other than related to dietary fats).2 Another issue with an SFA limit is that people eat foods, not isolated SFAs. Dr. Sherwood conflates SFAs with meat and dairy, but plenty of other foods contain SFAs (e.g., nuts, which are associated with decided health benefits).3
Regarding meat, our two cited meta-analyses do indeed show direct associations between unprocessed meat consumption and cardiovascular risk or mortality. However, effects may depend on patient characteristics (e.g., as per the meta-analysis by O'Sullivan and colleagues, some populations show decreased mortality with meat consumption) and on meat quality (nutritional composition varies considerably with how animals are raised4; existing studies on adverse effects do not consider this nuance). As for dairy, we agree that the funding source may bias conclusions.5 However, consistent evidence suggests that dairy is not harmful (e.g., the meta-analysis by O'Sullivan and colleagues) and may even be beneficial (with potential benefits possibly mediated by the SFAs themselves6).
Dr. Sherwood also raises concern about low-carbohydrate diets and mortality. We do not recommend focusing on carbohydrates, just like we do not recommend focusing on SFAs (or any other food constituent). We believe the focus should be on foods and food combinations. We advise eating real foods, mostly from plants, but allow for inclusion of well-raised meats and other animal products per individual preferences.

