A 58-year-old man presented with generalized pruritus and an erythematous rash across his trunk, back, and extremities, including his palms and soles. The rash was not painful. Because of memory difficulties, he could not recall when the rash first appeared. He had no recent illness or fever. He had recently been evaluated for ataxia, upper extremity tremors, and hearing loss, and was presumed to have Parkinson disease. His medical history was significant for past alcohol abuse and placement of a pacemaker. He did not use intravenous drugs, and his wife was his only sex partner over the previous 16 years. He had areas of hypopigmentation across his distal extremities that were previously diagnosed as vitiligo.
On physical examination, he was confused and had difficulty hearing. He was afebrile. The skin examination revealed an erythematous, flat, maculopapular rash (Figures 1 and 2). There was no involvement of the gingiva or oral mucosa. Excoriations were present with areas of desquamation on the buttocks.
Figure 1.
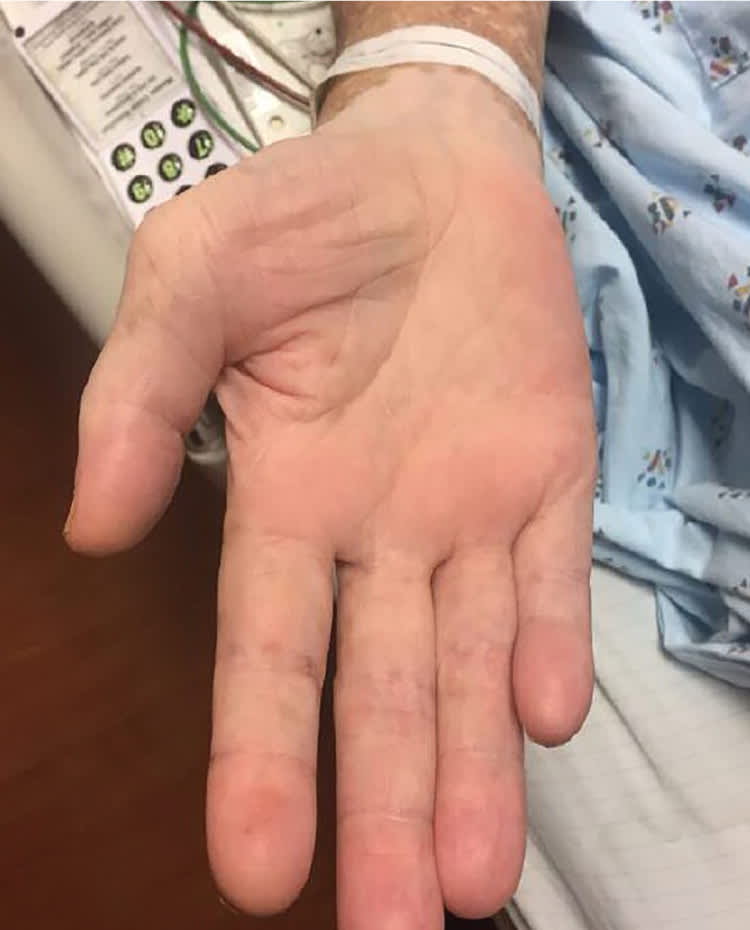
Figure 2.
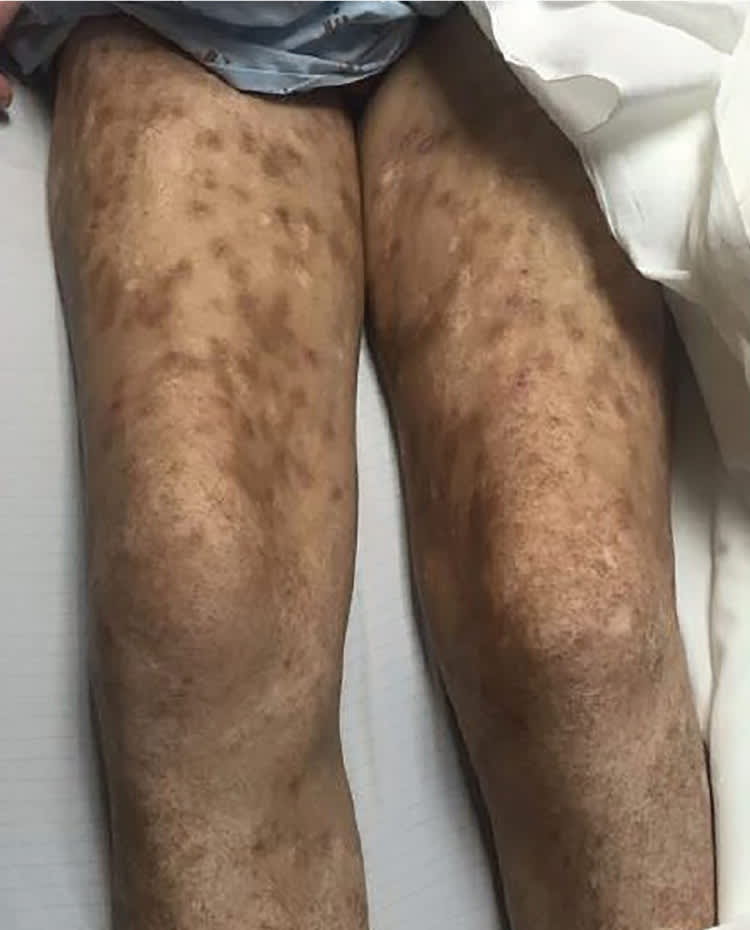
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Erythema multiforme.
B. Neurocutaneous manifestation of syphilis.
C. Septic emboli from infective endocarditis.
D. Stevens-Johnson syndrome.
E. Subacute cutaneous lupus erythematosus.
Discussion
The answer is B: neurocutaneous manifestation of syphilis. Neurologic and cutaneous manifestations are consistent with secondary syphilis. The clinical findings of secondary syphilis can vary greatly, but skin manifestations are most common.1 They are typically well-defined, small, erythematous, and hyperpigmented macules that may become generalized. The presentation evolves to include a more widespread papulosquamous eruption that can involve the trunk, extremities, and palmar and plantar surfaces.2 Acral involvement of papulosquamous lesions should be considered features of secondary syphilis until proven otherwise.2
The cutaneous findings of secondary syphilis typically occur two to eight weeks after the appearance of a painless primary genital chancre3 and result from dissemination of the infective spirochete. There has been an increase in prevalence of primary and secondary syphilis in recent years because of coinfection with human immunodeficiency virus. Other symptoms of secondary syphilis include low-grade fever, malaise, headaches, painless adenopathy, conjunctivitis, and arthralgias.2 The central nervous system may become involved in 40% of cases because of early spirochetemia.3
Diagnosis is made through a combination of serologic testing, with nontreponemal antigen testing and treponemal antigen confirmation.4 This patient's presentation of a rash with recent neurologic changes suggests syphilis. Laboratory results included positive findings on plasma reagin and human immunodeficiency virus antibody testing. A lumbar puncture was also performed and revealed Venereal Disease Research Laboratories titers of 1:128, which is consistent with neurosyphilis.
Erythema multiforme is an acute inflammatory reaction that typically presents as targetoid or ringlike lesions on the extremities with occasional involvement of the palms and soles. It may also include mucocutaneous erosions or bullae. The target lesions usually appear within approximately a 72-hour period, remain fixed, and then show signs of healing. Erythema multiforme usually occurs after an infection and has a benign course.5
Septic emboli are most commonly associated with vegetations on the mitral valve and typically present with fever. Skin findings may include palpable purpura, petechiae, and nodular lesions (Osler nodes and Janeway lesions). These are considered pathognomonic for bacterial endocarditis.6
Stevens-Johnson syndrome is a severe, acute mucocutaneous eruption often caused by use of medications, such as sulfonamide antibiotics, allopurinol, nonsteroidal anti-inflammatory drugs, and antiepileptic drugs (phenytoin [Dilantin], carbamazepine (Tegretol), and lamotrigine [Lamictal]). The syndrome causes pruritic papules on the face, neck, and central trunk,7 and the palms and soles may be involved. The hallmark is full-thickness epidermal necrosis with resultant desquamation and mucocutaneous blistering. If skin detachment involves more than 30% of the body surface area, the reaction is called toxic epidermal necrolysis.8
Subacute cutaneous lupus erythematosus is a subtype of lupus erythematosus with erythematous macules or plaques on sun-exposed skin (upper back, shoulders, extensor aspects of the arms). These lesions can evolve into hyperkeratotic papulosquamous or annular plaques, with gray-white hypopigmentation and telangiectasis.9
Summary Table

| Condition | Characteristics |
|---|---|
| Erythema multiforme | Targetoid or ringlike lesions on the extremities, with occasional involvement of the palms and soles; various stages of healing |
| Secondary syphilis | Maculopapular rash involving the trunk and extremities, including the palms and soles; rash develops after the appearance of the painless primary genital chancre |
| Septic emboli | Palpable purpura, petechiae, and nodular lesions (Osler nodes and Janeway lesions) |
| Stevens-Johnson syndrome | Full-thickness desquamation and mucocutaneous blistering; purpuric papules that progress to epidermal necrosis |
| Subacute cutaneous lupus | Erythematous macules or plaques on sun-exposed skin; progression to hyperkeratotic papulosquamous or annular plaques, with gray-white hypopigmentation and telangiectasis |

