An occupational illness is an event or exposure that occurs in the workplace that causes or contributes to a condition or worsens a preexisting condition. If an occupational disorder is suspected, a directed history should be taken with particular attention to establishing a temporal relationship of symptoms and exposure at work. Occupational asthma is the most prevalent occupational lung disorder in industrialized countries and presents with classic asthma symptoms (cough, difficulty breathing, chest tightness, wheezing). Occupational chronic obstructive pulmonary disease has been linked with exposure to nonspecific vapors, gases, dusts, fumes, and cigarette smoke. Occupational contact dermatitis is the most common dermal exposure. It can be caused by exposure to a variety of agents, including primary irritants or sensitizers, physical agents, mechanical trauma, and biologic agents. Occupational musculoskeletal disorders include many common repetitive injuries such as carpal tunnel syndrome and medial or lateral epicondylitis. Treatment of occupational disorders is generally the same as for nonoccupational disorders. Ideally, the exposure should be controlled to protect the worker. The impact of an occupational injury reaches beyond lost wages and can have a negative impact on quality of life.
Occupational disorder is an event or exposure that occurs in the workplace that causes or contributes to a condition or worsens a preexisting condition. Occupational disorders are underreported, with upwards of 69% of these injuries and illnesses not being reported.1 In 2013, the U.S. Bureau of Labor Statistics reported about 3 million nonfatal occupational injuries and illnesses.2 In 2007, the estimated medical costs for nonfatal occupational illness in the United States was $67 billion.3 Common occupational disorders are summarized in eTable A.
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Avoiding exposure to the offending agent is associated with greater likelihood of improvement in cases of occupational asthma and occupational dermatitis. | C | 4, 7, 9, 13, 14 |
| Routine application of fragrance-free postwork creams can help prevent occupational contact dermatitis. Prework creams are generally not helpful and may lead to complacency in other, more beneficial preventive measures. | C | 6, 7, 9 |
| Employers should consider offering workers with carpal tunnel syndrome differently configured keyboards. | C | 41 |
| Employers should consider offering temporarily modified duties to workers with carpal tunnel syndrome or epicondylitis that is aggravated by work to allow time for the condition to improve. | C | 41 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN OCCUPATIONAL MEDICINE: RECOMMENDATIONS FROM THE CHOOSING WISELY CAMPAIGN

| Recommendation | Sponsoring organization |
|---|---|
| Do not initially obtain radiographs for injured workers with acute nonspecific low back pain. | American College of Occupational and Environmental Medicine |
| Do not prescribe opioids for treatment of chronic or acute pain for workers who perform safety-sensitive jobs, such as operating motor vehicles, forklifts, cranes, or other heavy equipment. | American College of Occupational and Environmental Medicine |
Source: For more information on the Choosing Wisely Campaign, see http://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
eTable A. Overview of Common Occupational Disorders
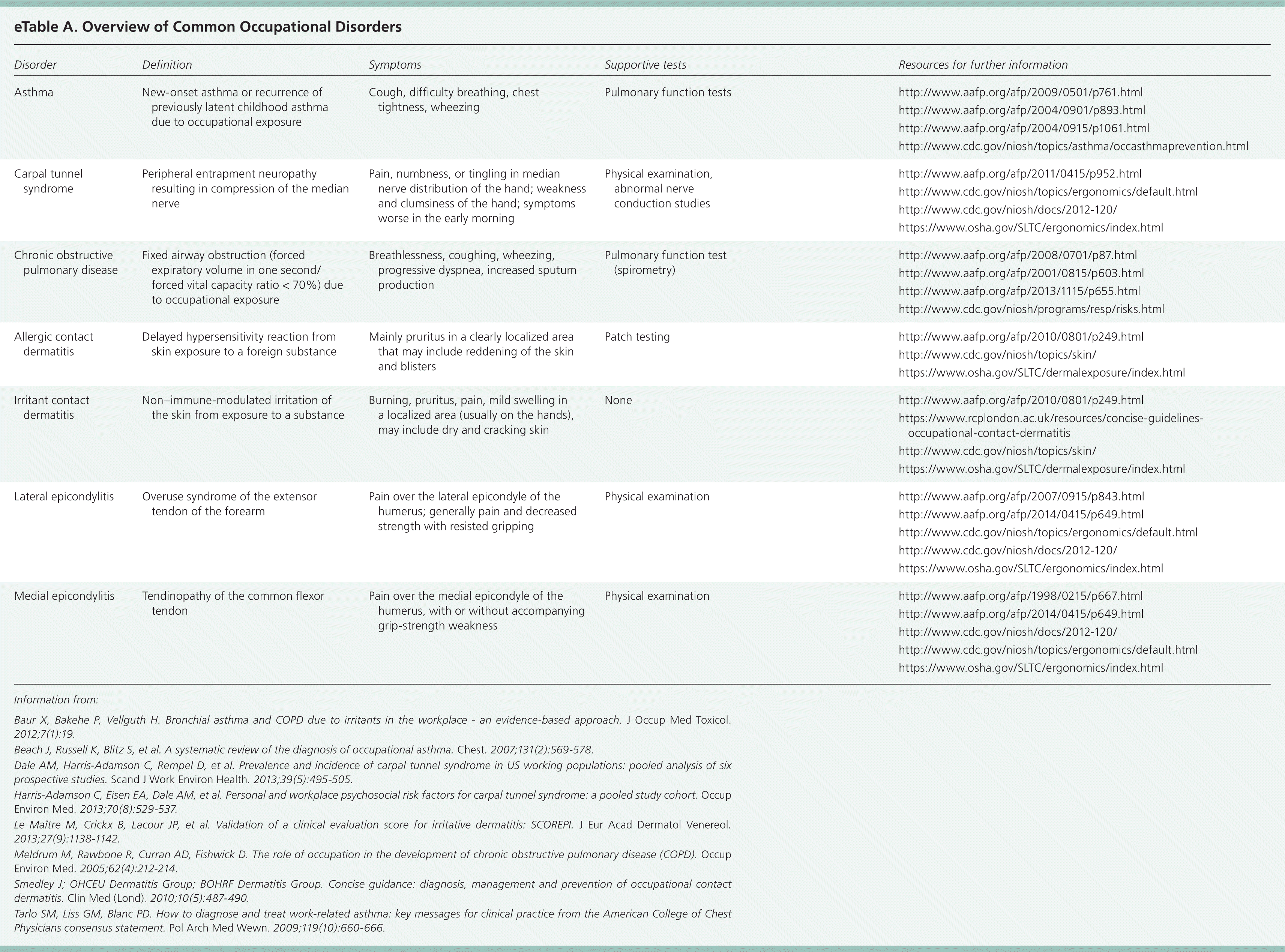
| Disorder | Definition | Symptoms | Supportive tests | Resources for further information |
|---|---|---|---|---|
| Asthma | New-onset asthma or recurrence of previously latent childhood asthma due to occupational exposure | Cough, difficulty breathing, chest tightness, wheezing | Pulmonary function tests | |
| Carpal tunnel syndrome | Peripheral entrapment neuropathy resulting in compression of the median nerve | Pain, numbness, or tingling in median nerve distribution of the hand; weakness and clumsiness of the hand; symptoms worse in the early morning | Physical examination, abnormal nerve conduction studies | |
| Chronic obstructive pulmonary disease | Fixed airway obstruction (forced expiratory volume in one second/forced vital capacity ratio < 70%) due to occupational exposure | Breathlessness, coughing, progressive dyspnea, increased sputum wheezing, production | Pulmonary function test (spirometry) | |
| Allergic contact dermatitis | Delayed hypersensitivity reaction from skin exposure to a foreign substance | Mainly pruritus in a clearly localized area that may include reddening of the skin and blisters | Patch testing | |
| Irritant contact dermatitis | Non–immune-modulated irritation of the skin from exposure to a substance | Burning, pruritus, pain, mild swelling in a localized area (usually on the hands), may include dry and cracking skin | None | |
| Lateral epicondylitis | Overuse syndrome of the extensor tendon of the forearm | Pain over the lateral epicondyle of the humerus; generally pain and decreased strength with resisted gripping | Physical examination | |
| Medial epicondylitis | Tendinopathy of the common flexor tendon | Pain over the medial epicondyle of the humerus, with or without accompanying grip-strength weakness | Physical examination |
Information from: Baur X, Bakehe P, Vellguth H. Bronchial asthma and COPD due to irritants in the workplace - an evidence-based approach. J Occup Med Toxicol. 2012;7(1):19.
Beach J, Russell K, Blitz S, et al. A systematic review of the diagnosis of occupational asthma. Chest. 2007;131(2):569–578.
Dale AM, Harris-Adamson C, Rempel D, et al. Prevalence and incidence of carpal tunnel syndrome in US working populations: pooled analysis of six prospective studies. Scand J Work Environ Health. 2013;39(5):495–505.
Harris-Adamson C, Eisen EA, Dale AM, et al. Personal and workplace psychosocial risk factors for carpal tunnel syndrome: a pooled study cohort. Occup Environ Med. 2013;70(8):529–537.
Le Maître M, Crickx B, Lacour JP, et al. Validation of a clinical evaluation score for irritative dermatitis: SCOREPI. J Eur Acad Dermatol Venereol. 2013;27(9):1138–1142.
Meldrum M, Rawbone R, Curran AD, Fishwick D. The role of occupation in the development of chronic obstructive pulmonary disease (COPD). Occup Environ Med. 2005;62(4):212–214.
Smedley J; OHCEU Dermatitis Group; BOHRF Dermatitis Group. Concise guidance: diagnosis, management and prevention of occupational contact dermatitis. Clin Med (Lond). 2010;10(5):487–490.
Tarlo SM, Liss GM, Blanc PD. How to diagnose and treat work-related asthma: key messages for clinical practice from the American College of Chest Physicians consensus statement. Pol Arch Med Wewn. 2009;119(10):660–666.
Family physicians who practice occupational medicine must be familiar with Occupational Safety and Health Administration and local standards for identification and reporting of occupational health hazards. However, all family physicians should feel comfortable screening patients for suspected occupational exposures. An occupational history can provide clinical clues (Table 1).4–9 When physicians identify an occupational disorder, federal and state law mandate obligatory reporting. Requirements for each state can be located on medical licensing websites, the Occupational Safety and Health Administration's website ( https://www.osha.gov/dts/oom/clinicians/), or individual state websites.
Table 1. Key Elements of the Occupational History in the Evaluation of Occupational Disorders

| Element | Significance |
|---|---|
| All patients | |
| What type of work do you do? | Exposures are common in the following occupations: agricultural workers, beauticians, chemical workers, cleaners, construction workers, food industry workers, health care workers, machine operators, mechanics, metal workers, auto industry workers |
| In your job, have you been exposed (currently or in the past) to chemicals, dusts, metals, radiation, noise, or repetitive work? | Common exposures include acrylics, alcohols, chromium/chromates, cleansers, cobalt, cosmetics, cutting oils, degreasers, disinfectants, epoxy resins, nickel, petroleum, plants, preservatives, resins, solvents, wet work |
| Are any of your coworkers experiencing similar symptoms? | Increased likelihood of a common occupational exposure |
| Full occupational history for patients with suspected occupational illness | |
| Review of lifetime occupations and duties, including military history | Exposures may predate current occupation |
| Assessment of hazard exposure | Route, duration, concentration of hazard |
| Presence of controls | Use of personal protective equipment, ventilation, diverting conveyors, enclosures, ergonomic workstations, devices to redistribute weight |
| Timing of symptoms in relation to work | Temporal relationship is crucial; however, many times, improvement away from work is not appreciated |
| Exposure to nonoccupational hazards | Home environment, hobbies, recreational activities |
The Centers for Disease Control and Prevention and the National Institute for Occupational Safety and Health advocate the implementation of controls to protect workers10 (eFigure A). The first control is elimination, which involves removal of the hazard. If elimination is not possible, the hazard should be substituted. Next, engineering controls should isolate the worker from the hazard. At the same time, administrative controls can be instituted, including shortening shifts, rescheduling breaks, rotating workers, and providing employee training on recognizing risk factors. The last control is use of personal protective equipment.
eFigure A. Hierarchy of Controls

Hierarchy of controls to protect workers from occupational injuries and illnesses.
Adapted from Centers for Disease Control and Prevention. The National Institute for Occupational Safety and Health. Hierarchy of controls. http://www.cdc.gov/niosh/topics/hierarchy/. Accessed February 2015.
Occupational Asthma
Occupational asthma is the most prevalent occupational lung disorder in industrialized countries, accounting for approximately 15% of new asthma cases in adults.4,5,11,12 A 2012 survey of more than 200,000 patients in 22 states indicated that there were an estimated 1.9 million new cases of occupational asthma.12 Occupational asthma results in approximately 38,000 deaths and 1.6 million disability-adjusted life-years annually.13 More than 250 triggers for occupational asthma have been identified.5 Common triggers are listed in Table 2.4,5,11,14–17 Most cases (90%) are caused by sensitizers (substances that produce an immune-mediated response), and 10% of cases are caused by irritants (substances that produce direct cell damage and inflammation in the absence of sensitization).13 High-molecular-weight sensitizers are more common and consist of proteins and glycopeptides that induce an immunoglobulin E response.4,15 Low-molecular-weight sensitizers tend to be chemicals that produce a response through poorly understood pathophysiologic processes.4,15
Table 2. Common Agents Associated with Occupational Asthma

| Agent | Occupations/industries |
|---|---|
| Irritant-induced asthma (cough, shortness of breath, wheezing typically within 24 hours of exposure) | |
| Chlorine | Paper mill workers |
| High-level-irritant dust | Construction workers, rescue workers |
| Smoke | Firefighters and other rescue workers |
| Sensitizer-induced asthma*: high-molecular-weight agents (respiratory symptoms often accompanied by rhinitis; a latency period of two years may be observed) | |
| Animals | Farmers, laboratory workers |
| Bioaerosols | Health care workers, researchers |
| Drugs | Health care workers, researchers |
| Enzymes | Bakers, house cleaners |
| Latex | Health care workers, laboratory workers |
| Plants | Farmers, bakers, field workers |
| Seafood | Seafood processing |
| Sensitizer-induced asthma*: low-molecular-weight agents (symptoms similar to those caused by high-molecular-weight agents, but there may be a delayed response) | |
| Acid anhydrides | Epoxy resin workers |
| Diisocyanates | Plastic industry, insulation workers, spray painters |
| Isocyanates | Painters |
| Metals | Metal refinery, metal alloy production, electroplating, welding |
| Persulfate | Hairdressers |
| Reactive dyes | Textile workers, food industry workers |
| Rosin | Metal working |
| Wood dusts | Carpenters, sawmill workers |
*—High-molecular-weight agents are more common and consist of proteins and glycopeptides that induce an immunoglobulin E response. Low-molecular-weight agents tend to be chemicals that produce a response through poorly understood pathophysiologic processes.4,15
DIAGNOSIS
Because of the high prevalence of occupational asthma, it should be considered in any adult with new-onset asthma.4,16 Symptoms of occupational asthma are similar to those of nonoccupational asthma, such as cough, difficulty breathing, chest tightness, and wheezing. A full occupational history should be taken (Table 1).4–9 The question “Do your symptoms improve on days away from work?” has been shown to have the highest sensitivity for the diagnosis of occupational asthma.15,18 Once the occupational history is verified, occupational asthma should be confirmed using objective measures of airway function, including serial peak expiratory flow monitoring, spirometry, skin prick tests, methacholine challenge, or specific inhalation challenge.4,11,14
MANAGEMENT
The preferred initial management strategy for occupational asthma is complete avoidance of the agent.4,14 However, bronchial hyperresponsiveness persists in up to 70% of patients even years after cessation of exposure.4 Personal respiratory equipment can result in a temporary improvement of respiratory symptoms, but not complete suppression.14 Therefore, it is most useful as an interim measure while implementing efforts to control exposures at the source or in the environment.4,11,14 The pharmacologic treatment of occupational asthma is the same as for asthma in general and includes inhaled corticosteroids, bronchodilators, and leukotriene modifiers.11
Figure 1. Diagnosis of Occupational Asthma
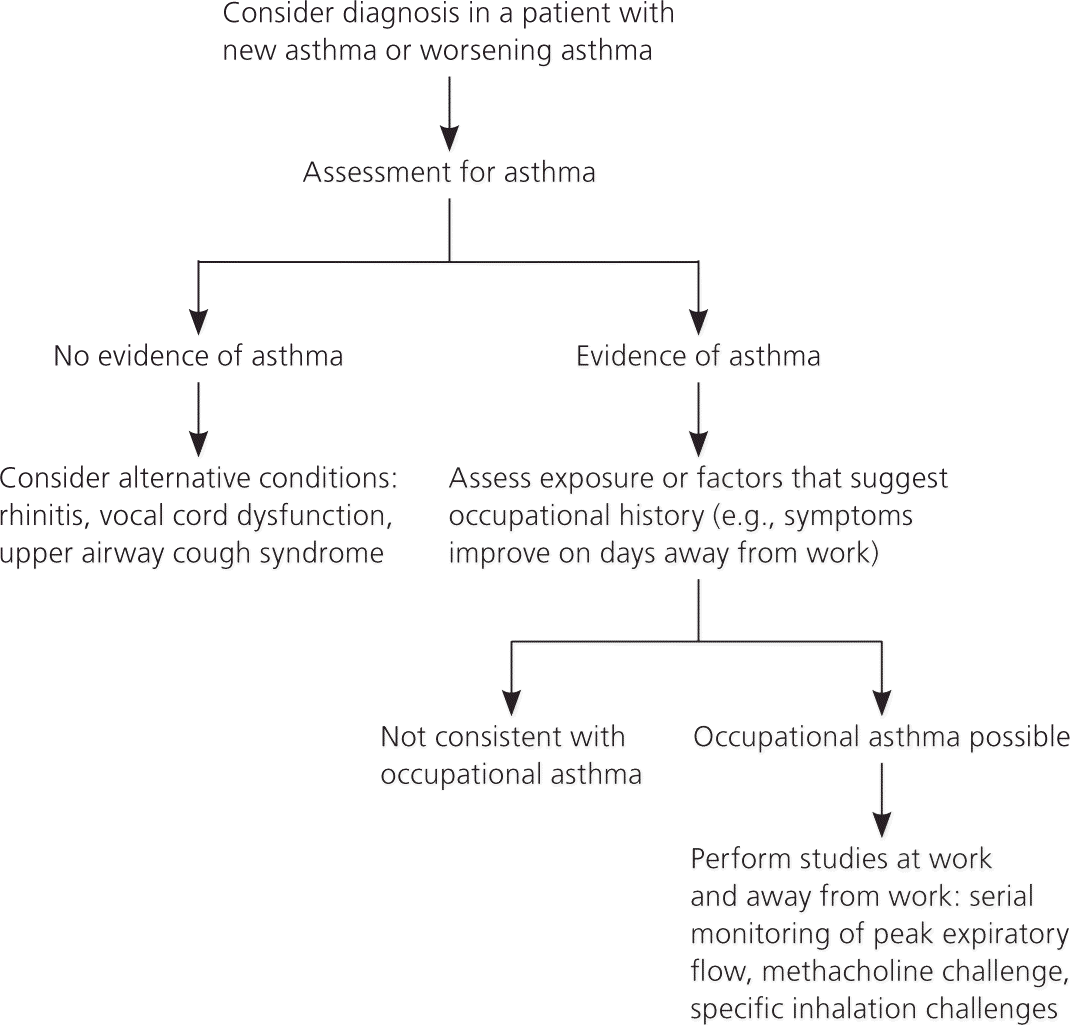
Algorithm for the diagnosis of occupational asthma.
Information from references 4 and 19.
The prognosis of patients with occupational asthma is generally poor, with only about one-third achieving long-term symptomatic recovery or resolution of objective measures of airway dysfunction even after complete avoidance of exposure.20
Occupational COPD
Chronic obstructive pulmonary disease (COPD) is the fourth leading cause of death worldwide, and approximately 15% of COPD cases are attributable to occupational exposures.17,21,22 An analysis of data from the National Health and Nutrition Examination Survey concluded that approximately 19% of all COPD cases were attributable to multiple occupational exposures (31% among never smokers).23 Although there is no official definition for occupational COPD, robust data favor nonsmoking occupational exposures as a cause.22,23 The most commonly implicated agents in occupational COPD are nonspecific vapors, gases, dusts, and fumes, with dusts showing a more consistent relationship.24 The evidence is strongest for workers exposed to coal dust, silica, cotton dust, or cadmium fumes.25 Concurrent exposure to cigarette smoke in these workers has a synergistic effect, leading to a higher risk than would be expected by multiplying the risks of the exposures alone.26 A recent case-control study concluded that there is an increased risk of occupational COPD with increasing age (older than 65 years), number of cigarettes smoked, and duration of exposure.24
DIAGNOSIS
The diagnosis of occupational COPD varies, but it is generally made using spirometry, the Global Initiative for Chronic Obstructive Lung Disease criteria used for non-occupational COPD (forced expiratory volume in one second/forced vital capacity ratio of less than 70%), and an appropriate occupational history. Spirometry should be conducted with precision to avoid underdiagnosis that could delay diagnosis and management.25,27
Workers with potential occupational COPD first report breathlessness, which may progress to coughing and wheezing.23 The long latency period from exposure to symptom onset and then to fixed obstruction can complicate the diagnosis and primary prevention efforts.21,23 There is no single standardized tool to assist in the diagnosis of occupational COPD, but the use of a questionnaire is an important part of the assessment.28 A list of available questionnaires can be found on the American Thoracic Society website at http://qol.thoracic.org/sections/specific-diseases/copd.html.
MANAGEMENT
Clear guidelines for the treatment of occupational COPD are currently lacking.26 Physicians should work with patients and employers to eliminate respiratory exposures. Primary prevention strategies include identification of workplace hazards and use of personal protective equipment, and secondary prevention focuses on medical surveillance with the use of symptom questionnaires.26,27 Family physicians should encourage and support smoking cessation. There is no evidence that the use of inhaled corticosteroids, long-acting beta agonists, or leukotriene modifiers changes the prognosis of occupational COPD.27
Occupational Dermatitis
Occupational skin exposure is the second most common cause of occupational disorders, with a rate of 2.3 injuries per 10,000 workers.2 More than 13 million U.S. workers annually are potentially exposed to chemicals absorbed through the skin.29 Most recently, a decrease in the incidence of occupational dermatitis has been reported in 10 European countries.30 The following discussion focuses on occupational contact dermatitis because it accounts for 90% to 95% of occupational skin disorders.6,7,29,31,32 Table 3 lists occupational skin disorders and associated occupations.6–8,29,31–33
Table 3. Occupational Skin Disorders and Associated Occupations
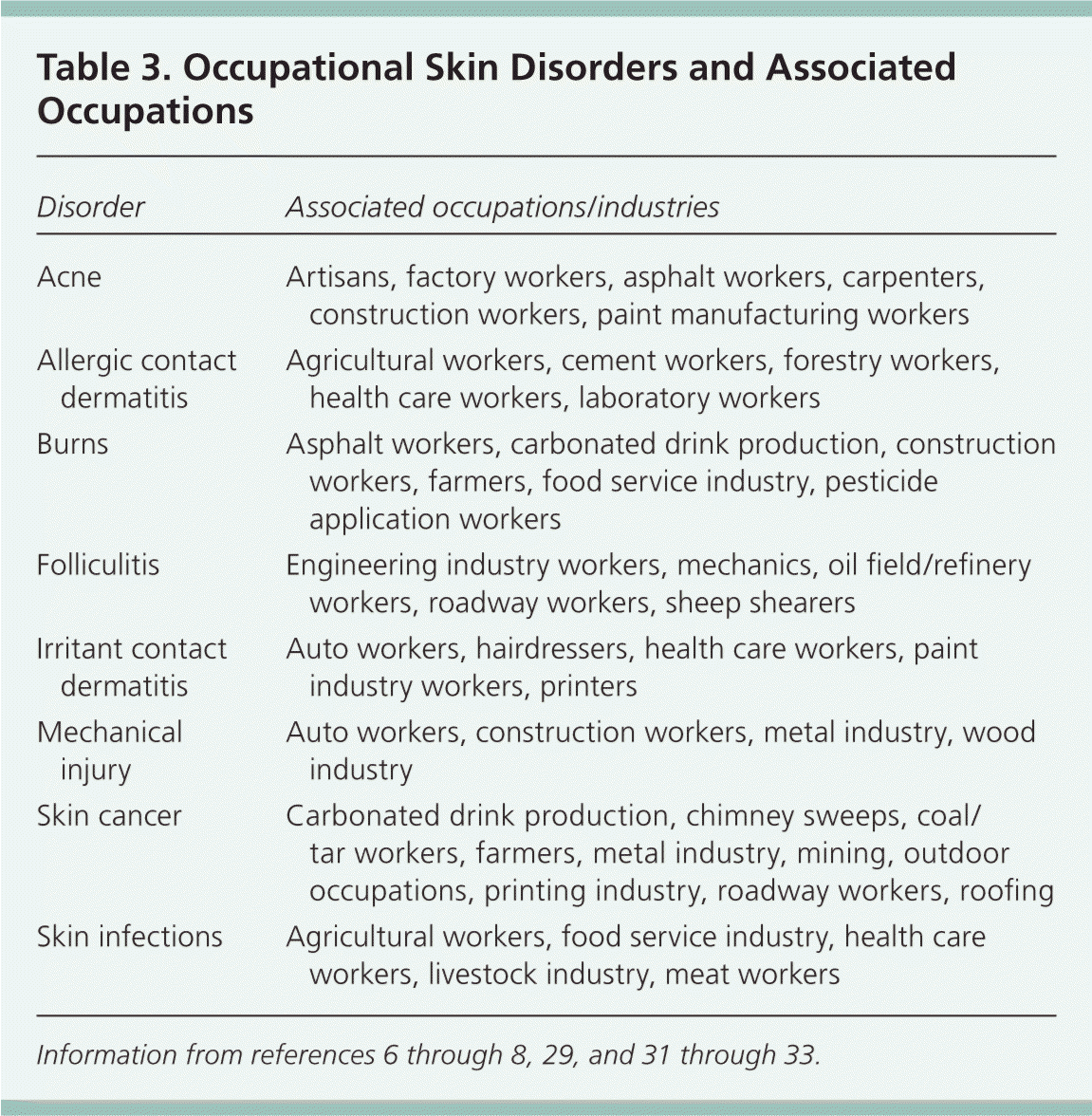
| Disorder | Associated occupations/industries |
|---|---|
| Acne | Artisans, factory workers, asphalt workers, carpenters, construction workers, paint manufacturing workers |
| Allergic contact dermatitis | Agricultural workers, cement workers, forestry workers, health care workers, laboratory workers |
| Burns | Asphalt workers, carbonated drink production, construction workers, farmers, food service industry, pesticide application workers |
| Folliculitis | Engineering industry workers, mechanics, oil field/refinery workers, roadway workers, sheep shearers |
| Irritant contact dermatitis | Auto workers, hairdressers, health care workers, paint industry workers, printers |
| Mechanical injury | Auto workers, construction workers, metal industry, wood industry |
| Skin cancer | Carbonated drink production, chimney sweeps, coal/tar workers, farmers, metal industry, mining, outdoor occupations, printing industry, roadway workers, roofing |
| Skin infections | Agricultural workers, food service industry, health care workers, livestock industry, meat workers |
Information from references 6 through 8, 29, and 31 through 33.
DIAGNOSIS
Occupational contact dermatitis can be divided into irritant and allergic types. Irritant contact dermatitis is inflammation due to phototoxic reactions or skin contact with a chemical agent such as acids, bases, oxidizing or reducing agents, water, detergents, and cleaning agents. Exposure to wet work accounts for 68% of occupational contact dermatitis cases.29 Allergic contact dermatitis is caused by an allergic skin reaction. Common causes include metals, epoxy, acrylic resins, rubber additives, agrochemicals, and commercial chemicals. Nickel exposure occurs in many occupations with the use of stainless steel, magnets, metal plating, coinage, and certain alloys. Some substances can produce both irritant and allergic contact dermatitis.
Differentiating occupational from nonoccupational contact dermatitis relies on a careful occupational history. Irritant and allergic contact dermatitis can have similar presentations. A validated scoring tool for the severity of irritant contact dermatitis has been developed using clinical findings of erythema, desquamation, cracked skin, and the amount of skin affected.8 There is some genetic disposition for irritant contact dermatitis in patients with filaggrin mutation (a protein defect associated with diseases of keratinization), a history of adult atopic dermatitis, or nickel sensitivity. Patients with both filaggrin mutation and atopic dermatitis have the highest risk of developing irritant contact dermatitis.6,31,33 Patch testing can help identify allergic contact dermatitis and should be considered when occupational contact dermatitis has not improved after three months of treatment and a contact allergy is suspected.6,7
Occupational contact dermatitis can develop at any point during a person's career7 and has a variable clinical course: one-third of patients have resolution of skin symptoms, one-third have partial improvement but persistence of symptoms, one-fourth have no change, and a few experience worsening of symptoms.34 However, quality of life and daily function are affected in nearly 50% of workers with occupational contact dermatitis.32,33
MANAGEMENT
Prevention programs are vital for the treatment of occupational contact dermatitis and should be used in conjunction with the hierarchy of controls10 (eFigure A). Although prevention recommendations (Table 46,7,9,31 ) are generally supported, proving significant clinical outcomes has been difficult.31 Routine application of fragrance-free postwork creams can help prevent dermatitis, but application of prework creams is generally not helpful and may lead to complacency in other, more beneficial preventive measures.6,7,9,31,33 Treatment is similar to that of nonoccupational contact dermatitis, relying heavily on topical steroids. Physicians should provide patient education on how to reduce hazard exposure. Patients should be referred when appropriate therapy fails, a causative agent cannot be identified, or the diagnosis is unclear.
Table 4. Prevention Strategies for Occupational Contact Dermatitis

| Avoid allergens and irritants |
| Substitute a safer alternative or product for the exposure |
| Limit wearing of gloves (but encourage use with wet tasks; if glove use is prolonged, use cotton liners) |
| Promote alcohol-based cleansers rather than traditional soap and water when appropriate (especially for health care workers) |
| Regularly apply fragrance-free postwork cream |
| Avoid prework creams (generally not useful and can lead to complacency in other preventive measures) |
| Implement engineering controls (ventilation, automation, use of personal protective equipment) |
| Provide workers with appropriate health and safety information |
Occupational Musculoskeletal Disorders
Occupational musculoskeletal disorders are injuries or disorders of the muscles, tendons, joints, cartilage, and nerves that are caused or exacerbated by sudden exertion or prolonged exposure to physical factors such as repetitive movement, force, vibration, or awkward positions. Common upper-limb disorders include shoulder disorders, lateral epicondylitis, wrist tendinitis, and carpal tunnel syndrome, in addition to nonspecific strains, sprains, muscle tears, back pain, and hernias. Approximately one-half of occupational musculoskeletal disorders occur in those working in the manufacturing and services industries.35 According to 2011 data, musculoskeletal disorders accounted for 33% of all occupational injuries and illnesses.36 The true prevalence of occupational musculoskeletal disorders is difficult to determine because studies use different definitions.37 Risk is measured based on level of hand activity and forceful exertion, awkward positions, and hand-transmitted vibration.
Family physicians should inquire about routine heavy lifting, daily exposure to vibrations, routine overhead work, and repetitive forceful tasks. Workers at risk of occupational musculoskeletal disorders should be encouraged to engage in physical activity and maintain a healthy weight to reduce disease progression. Workplace adaption is critical for prevention and treatment of occupational musculoskeletal disorders. Ideally, the hazard should be removed. Engineering controls should alter factors of applied force, fixed body position, and pace of work. Administrative controls can protect workers through job rotation, forced breaks, and alteration of work pace. A systematic review of workplace-based interventions for the prevention of upper-extremity musculoskeletal disorders showed a positive effect of resistance exercise (dumbbell or kettlebell exercises).38
CARPAL TUNNEL SYNDROME
Among occupational disorders, carpal tunnel syndrome is the most expensive upper-extremity disorder in terms of days away from work and treatment costs. Although many occupations pose a risk of carpal tunnel syndrome, there are some individual risk factors, such as body mass index (more than 30 kg per m2); age (older than 50 years); female sex (hazard ratio = 1.30; 95% confidence interval, 0.98 to 1.72); being a new employee (less than 3.5 years at the occupation); and comorbidity with rheumatoid arthritis, diabetes mellitus, or thyroid disease.39,40 Additional occupational risk factors include no varied pace over work, lack of variety of work, high job strain, and inability to schedule breaks.39 Social support has a protective factor (hazard ratio = 0.54; 95% confidence interval, 0.31 to 0.95).39
Treatment is mainly conservative with rest, activity modification, splinting at the wrist/elbow, physical therapy, nonsteroidal anti-inflammatory drugs, and steroid injections. Using a differently configured keyboard may be beneficial.41 General recommendations with poor evidence include modifying duties, evaluating the workstation, and decreasing exposure to hand vibration.41 Surgery is reserved for severe, refractory cases.42
EPICONDYLITIS
Epicondylitis occurs with medial or lateral repetitive motion injuries. Lateral epicondylitis is characterized by pain over the lateral epicondyle of the humerus and is commonly referred to as tennis elbow. Medial epicondylitis occurs on the medial epicondyle and is commonly referred to as golfer's elbow. Workers with medial epicondylitis have an increased risk of other associated upper-limb musculoskeletal disorders. Forceful work, such as wrist bending/twisting and forearm twisting/rotating, is a risk factor for medial epicondylitis and is common in assembly-line workers.43,44 Women have been shown to have a higher incidence of lateral epicondylitis.43 Epicondylitis can have a significant psychological impact outside of physical injury, manifesting as job strain.43
Treatment for epicondylitis is mainly conservative with rest, acupuncture, splinting, and topical and oral nonsteroidal anti-inflammatory drugs. As with nonoccupational epicondylitis, surgery is generally reserved for severe cases.41,45 Although modifying duties is generally recommended, high-quality evidence is lacking. Medial epicondylitis has a good prognosis with a three-year recovery rate of 81%.44
Data Sources: A PubMed search was completed using the keywords occupational disorders, occupational asthma, occupational COPD, occupational skin disorders, occupational dermatitis, occupational musculoskeletal disorders, and repetitive motion injuries. Also searched were the Cochrane database, Essential Evidence Plus, Agency for Healthcare Research and Quality Evidence Reports, National Guideline Clearinghouse, the Centers for Disease Control and Prevention website, and the National Institute for Occupational Safety and Health website. Search dates: April 2013, May 2013, July 2013, and February 2016.
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the U.S. Air Force Medical Department or the U.S. Air Force at large.

