
Am Fam Physician. 2017;95(6):389-390
Author disclosure: No relevant financial affiliations.
A civilian contractor working in Iraq presented with two days of unilateral eye pain and redness. The symptoms began after a cloud of dust blew into his face while fixing an old generator. He was wearing safety glasses but not goggles. Initially, he had mild bilateral eye irritation and rinsed his eyes with water, but his eyes became red with increasing pain in the right eye. He tried over-the-counter eye drops without relief. His medical history was significant for hypertension. He had no history of vision changes, previous eye injury, or contact lens use.
On physical examination, his vital signs were normal. Visual acuity was 20/40 for the left eye, right eye, and both eyes together. Eye examination revealed temporal and inferior conjunctival injection of the right eye. There was a 1.5-mm, brownish, circular lesion along the iris (Figure 1). The patient reported pain with eye movement when his eyes were closed. There were no foreign bodies or lesions on the underside of the eyelid, and his left eye appeared normal. His pupils were equal, round, and reactive to light bilaterally.
Fluorescein staining of the right eye demonstrated circumferential uptake around the lesion with punctate uptake across the inferior conjunctiva. There was no evidence of an ocular leak. Slit-lamp examination was negative for cells within the anterior chamber. A cotton-tipped applicator was used to remove a 1-mm, black, irregularly shaped foreign body.
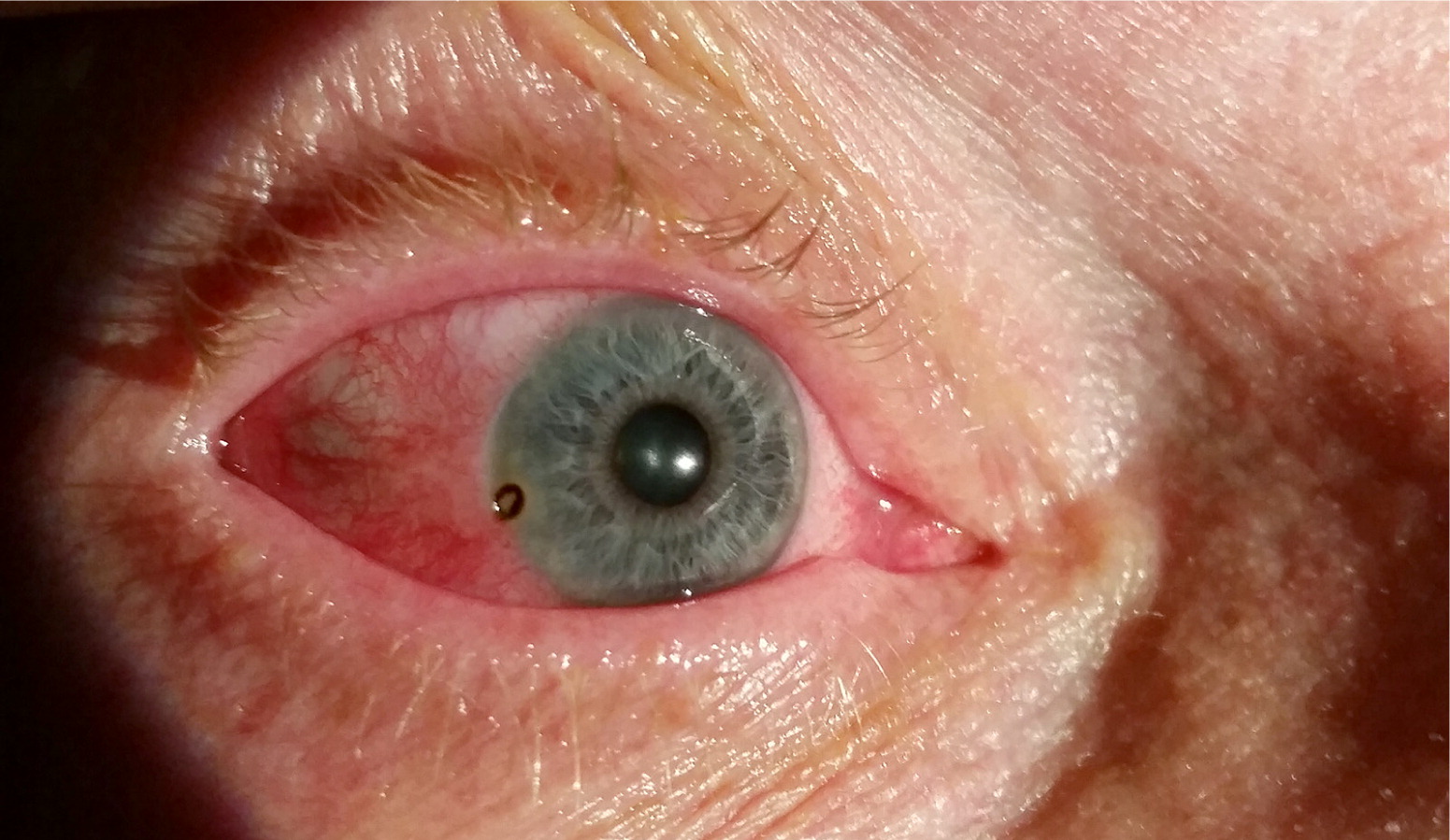
Question
Discussion
The answer is B: corneal rust ring. A foreign body containing iron that embeds in the cornea can create a defect in corneal epithelium known as a rust ring. When the iron is oxidized within the surrounding exposed stroma, it produces the classic brown-orange discoloration that encircles the defect, creating a ring appearance.1 This can occur within a few hours of contact.1 The ring persists after removal of the foreign body but will dissipate over several weeks without intervention.1
The rust ring should be debrided at the time of foreign body removal to prevent chronic inflammation or scarring,2,3 which can cause visual impairment if the lesion falls within the visual field. After foreign body removal and debridement, topical antibiotics should be prescribed to prevent infection while the cornea is healing.
A Bitot spot is a conjunctival lesion caused by vitamin A deficiency that is most common in children three to six years of age. It appears at the temporal aspect of the eye and has a white “foamy” appearance.4
Herpetic keratitis is inflammation of the corneal epithelium caused by herpes simplex virus infection. Fluorescein staining usually shows a classic dendritic branching pattern, although it may also appear as coarse punctate ulcerations. The cornea is a rare site for primary herpes simplex virus infection and would likely also present with regional lymphadenitis and cutaneous vesicular lesions.2
Hyphema is a hemorrhage within the anterior chamber of the eye. It is typically associated with blunt trauma but may occur postoperatively or spontaneously. Hyphema may be seen only on slit-lamp examination, but large bleeds may be visible on gross examination as it obstructs the iris.2,3 Patients with a coagulopathy or who are taking anticoagulants are at increased risk of hyphema formation.3
Perforation of the globe is a full-thickness laceration of the cornea or sclera caused by trauma, often a penetrating foreign body. Some may be small enough to require minimal intervention. A perforation is suggested on examination by a Seidel test demonstrating an ocular leak, decreased visual acuity, decreased intraocular pressure, flattening of the anterior chamber, or changes in the contour of the iris or pupil.2,3

| Condition | Characteristics |
|---|---|
| Bitot spot | White “foamy” conjunctival lesion caused by vitamin A deficiency; mainly occurs in children three to six years of age |
| Corneal rust ring | An embedded foreign body containing iron causes a brown-orange discoloration encircling the defect (rust ring); can form within a few hours of contact |
| Herpetic keratitis | Inflammation of the corneal epithelium caused by herpes simplex virus infection; associated cutaneous vesicular lesions; classic dendritic pattern on fluorescein stain |
| Hyphema | Hemorrhage within the anterior chamber of the eye; typically associated with blunt trauma but may occur postoperatively or spontaneously; patients with a coagulopathy or who are taking anticoagulants are at increased risk |
| Perforation of the globe | Full-thickness laceration of the cornea or sclera caused by trauma, often a penetrating foreign body; signs may include a positive Seidel test result, decreased visual acuity, decreased intraocular pressure, flattening of the anterior chamber, and changes in the contour of the iris or pupil |
The opinions and assertions contained herein are the private views of the author and are not to be construed as official or as reflecting the views of the U.S. Army Medical Department or the U.S. Army at large.
