In the United States, there are 212.6 million physically active persons older than six years (eFigure A), including 36 million youths and 7.8 million high school sports participants at approximately 36,000 secondary schools.1–4 Although physical activity clearly improves health outcomes, it also carries inherent risks, including injury, illness, and, rarely, death. Although a small percentage of family physicians currently hold a sports medicine certificate of added qualifications,5 most family physicians treat active patients or athletes, and many serve as team physicians. Given the limited attention paid to the role and importance of physical activity in medical schools6 and the limited exposure to sports medicine and musculoskeletal problems during residency, many physicians would likely benefit from additional knowledge to improve their ability to prevent and treat injuries from sports and physical activity.
eFigure A.
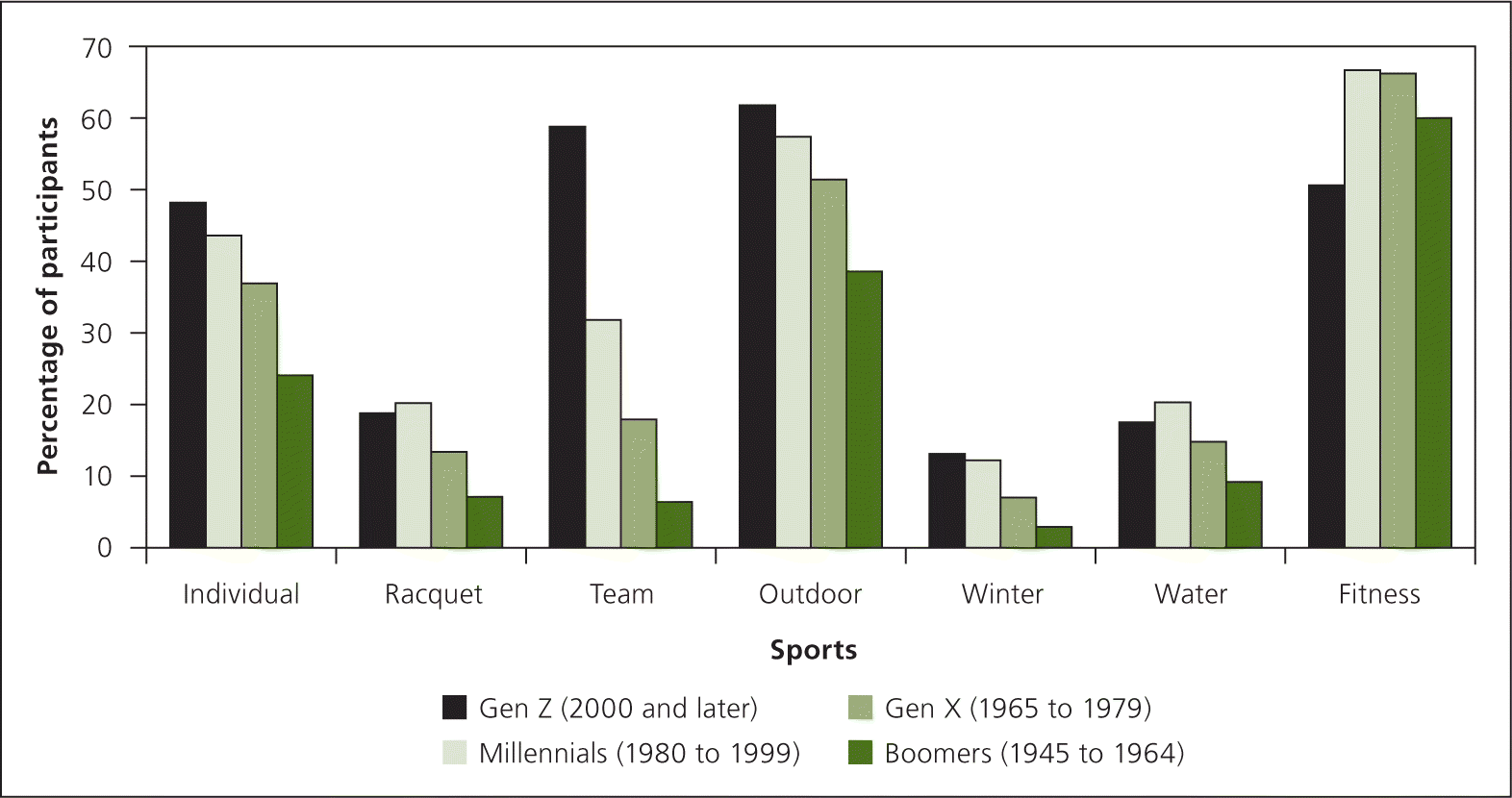
Participation in various categories of sports by generational divide.
Adapted with permission from the Physical Activity Council 2016 participation report. http://www.physicalactivitycouncil.com/pdfs/current.pdf. Accessed October 25, 2016.
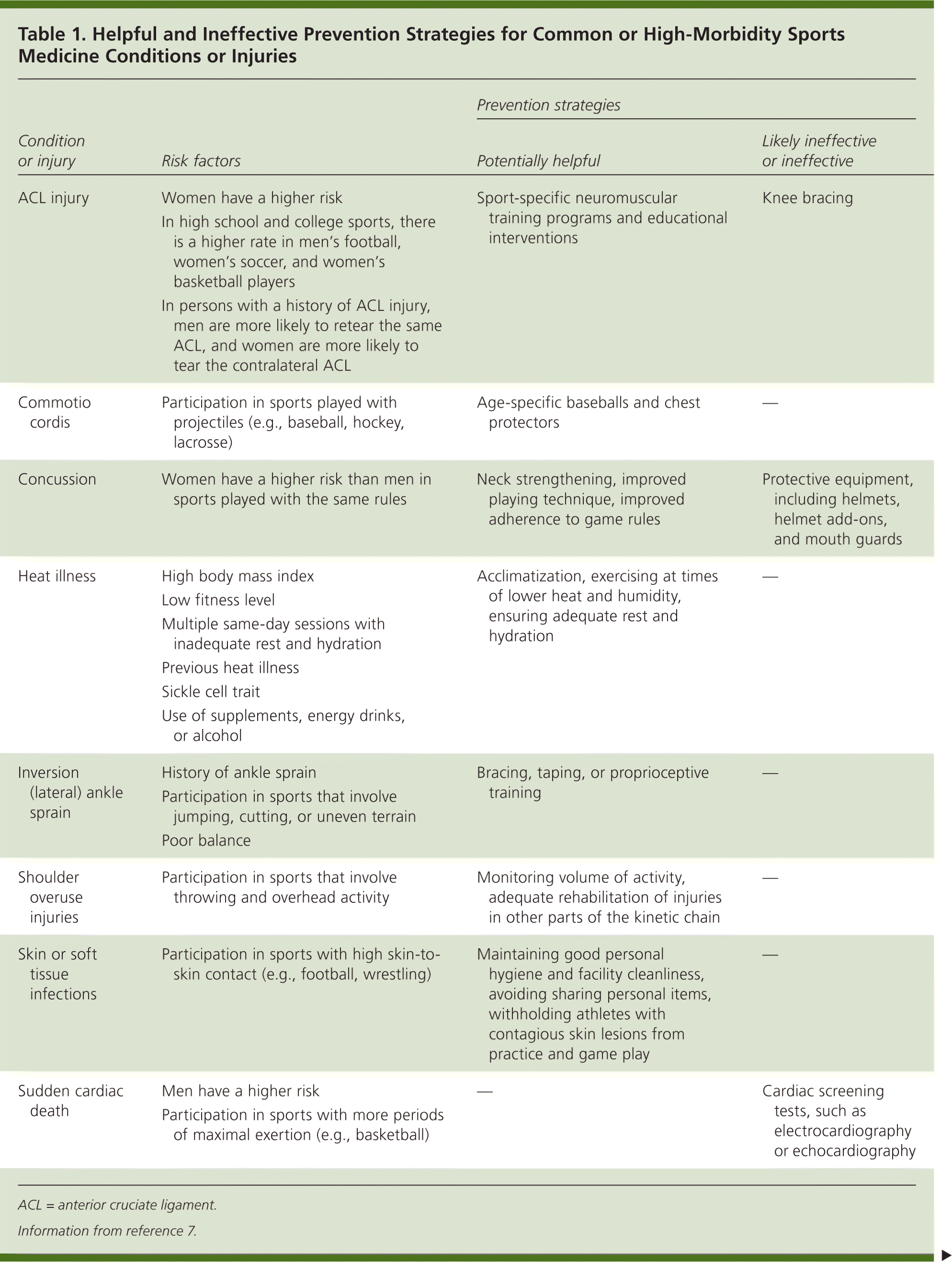
The Team Physician Consensus Conference Statements (http://www.acsm.org/public-information/team-physician-consensus-conference-statements), which represent an ongoing collaboration between six major medical societies concerned with clinical sports medicine issues, is one helpful resource for physicians caring for athletes. The most recent version addresses the team physician's role in preventing illness and injury, and discusses potentially helpful and ineffective or unproven strategies for preventing common or serious conditions and injuries that can result from physical activity (Table 1).7
Table 1. Helpful and Ineffective Prevention Strategies for Common or High-Morbidity Sports Medicine Conditions or Injuries
| Prevention strategies | |||
|---|---|---|---|
| Condition or injury | Risk factors | Potentially helpful | Likely ineffective or ineffective |
| ACL injury | Women have a higher risk | Sport-specific neuromuscular training programs and educational Interventions | Knee bracing |
| In high school and college sports, there is a higher rate in men's football, women's soccer, and women's basketball players | |||
| In persons with a history of ACL injury, men are more likely to retear the same ACL, and women are more likely to tear the contralateral ACL | |||
| Commotio cordis | Participation in sports played with projectiles (e.g., baseball, hockey, lacrosse) | Age-specific baseballs and chest protectors | — |
| Concussion | Women have a higher risk than men in sports played with the same rules | Neck strengthening, improved playing technique, improved adherence to game rules | Protective equipment, including helmets, helmet add-ons, and mouth guards |
| Heat illness | High body mass index | Acclimatization, exercising at times of lower heat and humidity, ensuring adequate rest and hydration | — |
| Low fitness level | |||
| Multiple same-day sessions with inadequate rest and hydration | |||
| Previous heat illness | |||
| Sickle cell trait | |||
| Use of supplements, energy drinks, or alcohol | |||
| Inversion (lateral) ankle sprain | History of ankle sprain | Bracing, taping, or proprioceptive training | — |
| Participation in sports that involve jumping, cutting, or uneven terrain | |||
| Poor balance | |||
| Shoulder overuse Injuries | Participation in sports that involve throwing and overhead activity | Monitoring volume of activity, adequate rehabilitation of injuries in other parts of the kinetic chain | — |
| Skin or soft tissue infections | Participation in sports with high skin-to-skin contact (e.g., football, wrestling) | Maintaining good personal hygiene and facility cleanliness, avoiding sharing personal items, withholding athletes with contagious skin lesions from practice and game play | — |
| Sudden cardiac death | Men have a higher risk Participation in sports with more periods of maximal exertion (e.g., basketball) | — | Cardiac screening tests, such as electrocardiography or echocardiography |
ACL = anterior cruciate ligament.
Information from reference 7.
One important area to address is the preparticipation evaluation. Although this evaluation has not been proven to prevent injury or death, most states require them for youth athletes. The fourth edition of the American Academy of Pediatrics' preparticipation physical evaluation recommendations, which was previously reviewed in American Family Physician (https://www.aafp.org/afp/2015/0901/p371.html), provides several practical tools and forms for the team physician, as well as guidance on screening young athletes prior to sports participation.8 The American College of Sports Medicine's (ACSM's) revised criteria on exercise preparticipation health screening offer clearer and more succinct advice for exercise testing in adult patients.9 The criteria state that to help eliminate barriers, excessive referrals, and overuse of medical resources, physicians should perform exercise testing only in persons at high risk of exercise-related complications who are starting a vigorous physical activity program. The Physical Activity Readiness Questionnaire (http://www.csep.ca/cmfiles/publications/parq/par-q.pdf) is a free self-screening tool commonly used to determine whether a patient should see a physician prior to physical activity.
There are several live and online continuing medical education programs. Physicians with limited experience and background knowledge in sports medicine might begin with the ACSM Team Physician Course (http://www.acsm.org/attend-a-meeting/acsm-team-physician-course). The American Academy of Family Physicians (AAFP) offers the Practical Advances in Musculoskeletal and Sports Care course (https://www.aafp.org/cme/cme-topic/all/sports-live.html), which mixes didactic learning with hands-on practical experience, including field-side emergency management training and sessions at the AAFP's Family Medicine Experience (https://www.aafp.org/events/fmx.html).
Highly experienced physicians may find more value in an advanced team physician course. This type of course is offered by the ACSM, American Medical Society for Sports Medicine, and American Orthopedic Society for Sports Medicine (http://www.sportsmed.org/aossmimis/Members/Education/Meeting_Resources/ATPC2016/Advanced-Team-Physician-Course.aspx), and by the International Olympic Committee (http://www.ioc-preventionconference.org/atpc2016/). Online continuing medical education through webinars and stored lectures, such as the AAFP self-study programs (https://www.aafp.org/cme/browse/topics.tag-sports.html), offer a self-paced and potentially more economic alternative.
Family physicians may join national sports medicine organizations to stay current and interact with individuals with similar interests. The ACSM (http://acsm.org/), which is open to physicians, scientists, and allied health professionals, and the American Medical Society for Sports Medicine (http://www.amssm.org/), which is open to physicians only, are broad sports medicine organizations. Those interested in particular topics might join more specialized associations. For instance, the American Medical Athletic Association (http://www.amaasportsmed.org/) focuses primarily on sports medicine related to runners, and sponsors symposia at the Marine Corps and Boston Marathons.
Family physicians can meet the needs of their communities, including those related to sports injuries. Table 2 includes resources that can help physicians fill the knowledge gap needed to provide effective care for athletes.
Table 2. Selected Sports Medicine Resources for Family Physicians

| Continuing medical education |
American Academy of Family Physicians
|
American College of Sports Medicine
|
International Olympic Committee
|
| Other resources |
American Academy of Pediatrics
|
American College of Sports Medicine
|
American Family Physician
|
American Medical Society for Sports Medicine
|
American Orthopaedic Society for Sports Medicine
|
University of California, San Diego
|
Wheeless' Textbook of Orthopaedics (Duke Orthopaedics)
|

