Hypertension affects one-third of Americans and is a significant modifiable risk factor for cardiovascular disease, stroke, renal disease, and death. Severe asymptomatic hypertension is defined as severely elevated blood pressure (180 mm Hg or more systolic, or 110 mm Hg or more diastolic) without symptoms of acute target organ injury. The short-term risks of acute target organ injury and major adverse cardiovascular events are low in this population, whereas hypertensive emergencies manifest as acute target organ injury requiring immediate hospitalization. Individuals with severe asymptomatic hypertension often have preexisting poorly controlled hypertension and usually can be managed in the outpatient setting. Immediate diagnostic testing rarely alters short-term management, and blood pressure control is best achieved with initiation or adjustment of antihypertensive therapy. Aggressive lowering of blood pressure should be avoided, and the use of parenteral medications is not indicated. Current recommendations are to gradually reduce blood pressure over several days to weeks. Patients with escalating blood pressure, manifestation of acute target organ injury, or lack of compliance with treatment should be considered for hospital admission.
Hypertension affects more than 30% of adults in the United States and is a significant modifiable risk factor for cardiovascular disease, stroke, renal disease, and death.1,2 Several high-quality studies have shown that treatment of hypertension reduces long-term hypertension-related adverse outcomes and all-cause mortality.3–5
WHAT IS NEW ON THIS TOPIC: SEVERE ASYMPTOMATIC HYPERTENSION
The U.S. Preventive Services Task Force recommends out-of-office blood pressure monitoring (using home and ambulatory blood pressure monitoring devices) as an important adjunct to in-office measurements for diagnosing hypertension.
A recent trial of an outpatient population referred to the emergency department for severe asymptomatic hypertension showed that only 5% of tests ordered had abnormal results, and 2% of patients had evidence of target organ injury. Less than 1% of patients had a major adverse cardiovascular event within six months.
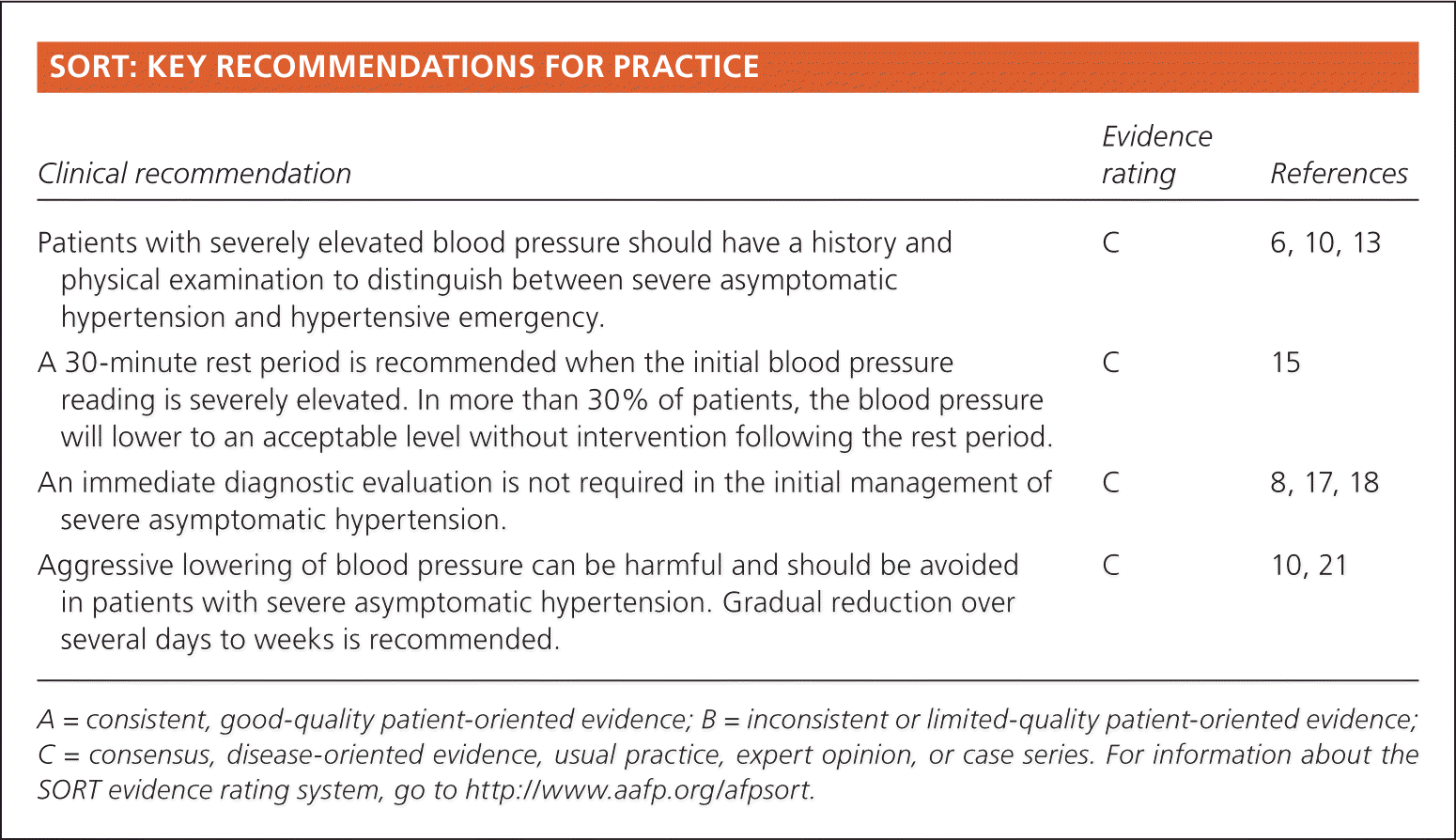
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Patients with severely elevated blood pressure should have a history and physical examination to distinguish between severe asymptomatic hypertension and hypertensive emergency. | C | 6, 10, 13 |
| A 30-minute rest period is recommended when the initial blood pressure reading is severely elevated. In more than 30% of patients, the blood pressure will lower to an acceptable level without intervention following the rest period. | C | 15 |
| An immediate diagnostic evaluation is not required in the initial management of severe asymptomatic hypertension. | C | 8, 17, 18 |
| Aggressive lowering of blood pressure can be harmful and should be avoided in patients with severe asymptomatic hypertension. Gradual reduction over several days to weeks is recommended. | C | 10, 21 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Severe asymptomatic hypertension, or hypertensive urgency, is defined as severely elevated blood pressure (180 mm Hg or more systolic, or 110 mm Hg or more diastolic) without acute target organ injury.6 Patients may still have headache, lightheadedness, nausea, shortness of breath, palpitations, epistaxis, or anxiety, depending on the acuity and severity of blood pressure elevation.
Hypertensive emergency is defined as severe blood pressure elevation in the presence of acute target organ injury, such as encephalopathy, cerebrovascular or cardiovascular events, pulmonary edema, renal injury, or aortic dissection.7 These patients require urgent evaluation and hospitalization.
A retrospective cohort study from a single multispecialty outpatient health care system showed that in 4.6% of patients, initial blood pressure measurements met diagnostic criteria for severe asymptomatic hypertension.8 Approximately 4% of emergency department (ED) visits are for the management of severe asymptomatic hypertension,9,10 and more than 4.5% of adult inpatients receive intravenous antihypertensive medications for management of blood pressure elevations.11
Severe asymptomatic hypertension most often occurs in patients previously diagnosed with hypertension. More than 60% of patients have persistent uncontrolled hypertension six months after a documented clinic visit with a systolic blood pressure of 180 mm Hg or more, or a diastolic blood pressure of 110 mm Hg or more.8 Medication noncompliance has been reported in up to 65% of patients prescribed antihypertensive medications and is a major cause of severe asymptomatic hypertension.12 In rare cases, unrecognized secondary hypertension (e.g., renal vascular hypertension; sympathetic crisis from cocaine toxicity, pheochromocytoma, or acute alcohol withdrawal; primary hyperaldosteronism) can present with severe blood pressure elevations.7
There is insufficient evidence to dictate the most appropriate management for severe asymptomatic hypertension. Most guidelines focus on hypertensive emergency.
Evaluation
HISTORY AND PHYSICAL EXAMINATION
A comprehensive history is essential in the initial evaluation of patients with severe asymptomatic hypertension (Table 1).6 A medication history should include any new medications; illicit substances (e.g., sympathomimetics, cocaine); and, most importantly, compliance with current prescriptions.13 A targeted symptom history should be obtained to identify a potential hypertensive emergency. Severe blood pressure elevations may cause mild symptoms (e.g., headache, lightheadedness, nausea, shortness of breath, palpitations, epistaxis, anxiety) without acute target organ injury, although patients with chest pain should receive appropriate evaluation for chest pain, not severe asymptomatic hypertension.
Table 1. Medical History in the Evaluation of Severe Asymptomatic Hypertension

| Previous hypertension (duration and levels) |
| Personal history: coronary artery disease, congestive heart failure, cerebrovascular disease, chronic kidney disease, peripheral vascular disease, diabetes mellitus, sleep apnea |
| Risk factors: family history of hypertension, hyperlipidemia, diabetes, tobacco use, dietary habits, weight gain, sedentary lifestyle |
| Secondary causes: family history of kidney disease, personal history of renal disease, medications and illicit drug use, clinical features of metabolic disorders (e.g., thyroid disease, pheochromocytoma, hyperaldosteronism) |
| Target organ injury: neurologic (headache, vision changes, seizure, neurologic deficits), cardiovascular (chest pain, shortness of breath, myocardial infarction, syncope, history of palpitations or arrhythmias), renal (oliguria, anuria), peripheral arteries (claudication, cold extremities, weak distal pulses), pulmonary (sleep apnea, chronic lung disease) |
| Concurrent medication/drug use: nonsteroidal anti-inflammatory drugs, antidepressants, oral contraceptives, cold medications, sympathomimetics (amphetamines, cocaine, phencyclidine), corticosteroids, herbal remedies |
| Compliance with antihypertensive therapy |
Information from reference 6.
Physical examination findings are often normal in patients with severe asymptomatic hypertension. However, attention should be directed toward signs of target organ injury. These signs can be neurologic (motor or sensory deficits), ophthalmologic (arteriolar narrowing, hemorrhage, papilledema), cardiovascular (arrhythmia, displaced point of maximal impulse, murmur, third heart sound gallop), pulmonary (rales, hypoxia, tachypnea), or vascular (diminished or absent peripheral pulses, abdominal bruits, unequal pulses or blood pressure, jugular venous distension).4,10,13 Clinical examination findings that suggest acute target organ injury (new or evolving neurologic deficits, papilledema, pulmonary edema) are regarded as a hypertensive emergency until proven otherwise.
Proper technique should be used for all blood pressure measurements 6,10,14 (Table 214 ). If the blood pressure measurement is severely elevated, the patient should be allowed to quietly rest. In more than 30% of patients with severe asymptomatic hypertension, blood pressure lowers to an acceptable level (mean of 160/89 mm Hg) without intervention following a 30-minute rest period.15
Table 2. Proper Technique for Blood Pressure Measurements

| An appropriately sized automated electronic arm cuff device should be used. |
| Initially, a measurement should be obtained in both arms, and the higher blood pressure should be used (significant differences between arms occur in aortic coarctation, subclavian artery stenosis). |
| The patient should have an empty bladder and remain seated with legs uncrossed for five minutes before the measurement. |
| The measurement should occur at the level of the heart with the arm resting on a table. |
| Postural blood pressure should be obtained in older adults. |
| A minimum of two readings should be obtained one to two minutes apart and averaged. |
| The diagnosis of hypertension should be confirmed at a subsequent visit unless the blood pressure reading is very high or the patient is symptomatic. |
| Evaluation of white coat hypertension (elevated clinic blood pressure and normal ambulatory blood pressure) and masked hypertension (normal clinic blood pressure and elevated ambulatory blood pressure) should be considered as clinically indicated. |
Information from reference 14.
HOME AND AMBULATORY BLOOD PRESSURE MONITORING
The U.S. Preventive Services Task Force recommends out-of-office blood pressure monitoring (using home and ambulatory blood pressure monitoring devices) as an important adjunct to in-office measurements for diagnosing hypertension.16 A major advantage of out-of-office monitoring is the ability to obtain multiple readings over time. Specific indications for out-of-office monitoring in the setting of severe asymptomatic hypertension include suspected white coat hypertension (isolated clinic hypertension) and highly variable in-office blood pressure readings. Additionally, out-of-office monitoring is useful to assess compliance with antihypertensive therapy.
DIAGNOSTIC EVALUATION
Patients presenting with severe asymptomatic hypertension rarely require diagnostic evaluation, although subsequent office visits should include evaluation for long-term hypertension risks based on current guidelines.4,6 Patients with symptoms or clinical findings suggesting acute target organ injury require appropriate diagnostic testing and evaluation for possible hypertensive emergency. A recent trial of an outpatient population referred to the ED for severe asymptomatic hypertension showed only 5% of tests ordered had abnormal results, and only 2% of patients had evidence of target organ injury. The most commonly ordered tests were basic or complete metabolic panel (64% of patients; abnormal in five out of 247 patients), urinalysis (30% of patients; abnormal in 20 out of 115 patients), cardiac enzymes (35% of patients; abnormal in two out of 137 patients), chest radiography (35% of patients; abnormal in five out of 137 patients), and computed tomography of the head (13% of patients; no abnormalities). Electrocardiography was performed in less than 1% of patients.8
A cross-sectional study of two urban EDs enrolled 167 asymptomatic patients with triage diastolic blood pressure of 100 mm Hg or more. A basic metabolic panel was performed for all patients, of which 12 (7%) had unanticipated abnormalities resulting in hospitalization, primarily for renal dysfunction.17 The American College of Emergency Physicians does not recommend routine laboratory testing in patients with severe asymptomatic hypertension.18 No other organization or policy guideline has provided recommendations to assist in the diagnostic evaluation. Without sufficient clinical evidence, diagnostic evaluation for severe asymptomatic hypertension is largely anecdotal.
Treatment
There are currently no validated policies or nationally recognized clinical guidelines to assist in the management of severe asymptomatic hypertension. A suggested approach is shown in Figure 1. When managing severe asymptomatic hypertension, several important key questions should be considered.
Figure 1. Management of Severe Asymptomatic Hypertension
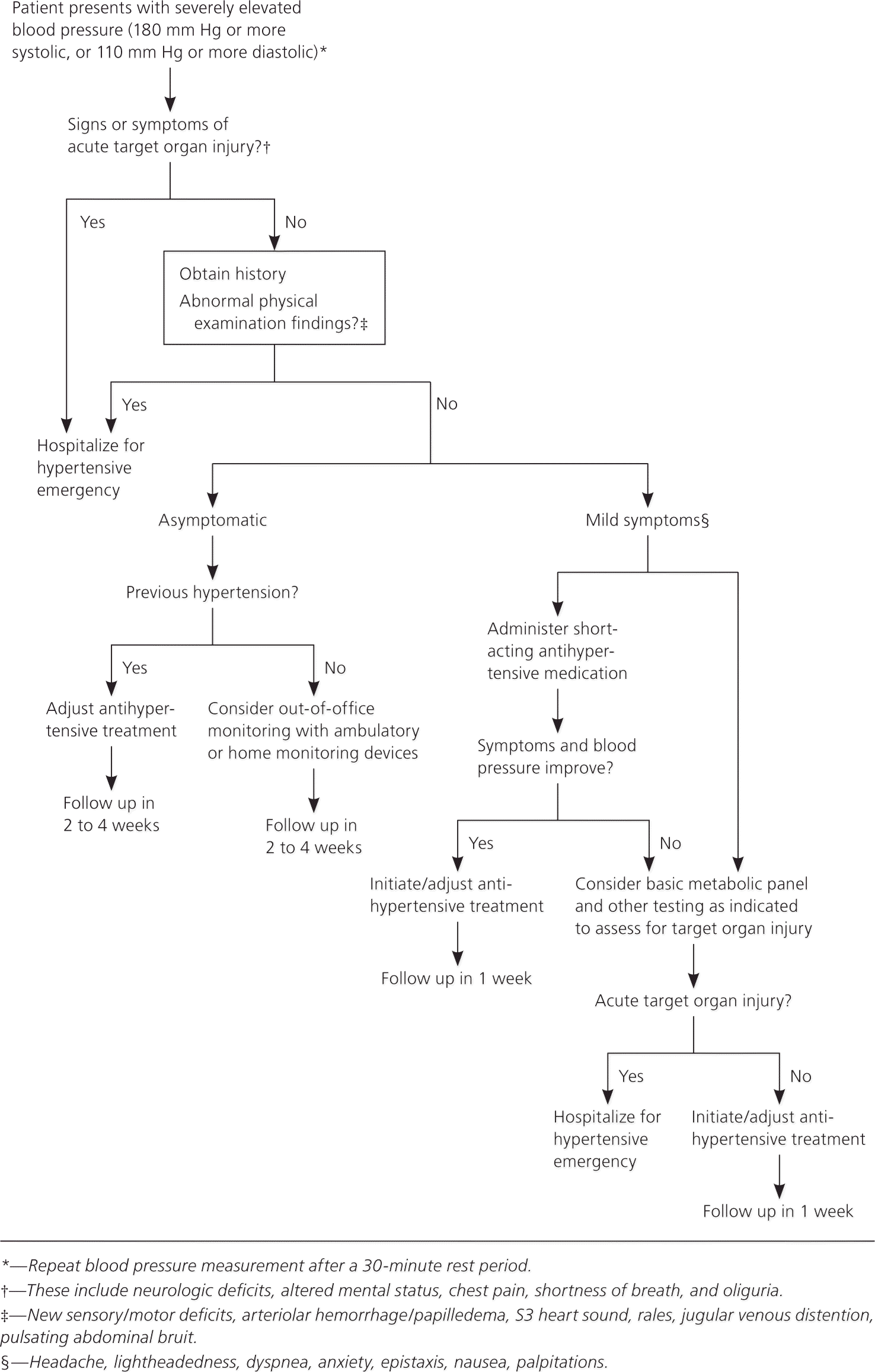
Suggested approach to the management of severe asymptomatic hypertension.
DOES ACUTE MEDICAL MANAGEMENT AFFECT SHORT-TERM ADVERSE OUTCOMES?
Serious adverse events related to poorly controlled hypertension (e.g., death, acute renal injury, cardiovascular complications, ruptured aortic aneurysms) are rare even when follow-up is delayed for several months.19
A retrospective outpatient study (n = 58,535) evaluated the short-term outcomes of patients with severe asymptomatic hypertension. Patients had a mean systolic blood pressure of 183 mm Hg (10% of patients had a measurement greater than 200 mm Hg) and mean diastolic blood pressure of 96 mm Hg (6% of patients had a measurement of 120 mm Hg or more). From the outpatient clinic, 426 patients (0.7%) were referred to the hospital (387 went to the ED, and 39 were directly admitted) for blood pressure management. The remainder of patients were sent home. Outcomes measured were the rate of major adverse cardiovascular events within seven days, eight to 30 days, and six months. The overall rate of major adverse cardiovascular events in both groups was low (less than 1%) with no significant differences at seven days, eight to 30 days, and six months. Patients who were sent home had a lower rate of subsequent hospital admission at seven days and at eight to 30 days compared with those originally sent to the hospital. Less than 1% of patients were referred to the hospital, validating that outpatient management is an appropriate, cost-effective approach. A limitation of this study is that 20% of patients were lost to follow-up, and their outcomes were not included in the analysis.8
A prospective observational study (n = 146) investigated the risk of short-term adverse effects of severe asymptomatic hypertension (mean blood pressure of 217/112 mm Hg at presentation) following discharge from the ED. Antihypertensive treatment was given to 90% of patients in the ED, and 92% were discharged with prescriptions (80% got prescriptions for two medications). More than 35% of patients still had blood pressure of more than 190/100 mm Hg at discharge, regardless of whether they were treated or observed in the ED. At the 10-day follow-up, the mean blood pressure significantly improved (160/90 mm Hg) with no serious adverse outcomes. The authors concluded that attempts to lower blood pressure acutely may not be necessary. Discharging patients with antihypertensive medications is a reasonable and safe option.20
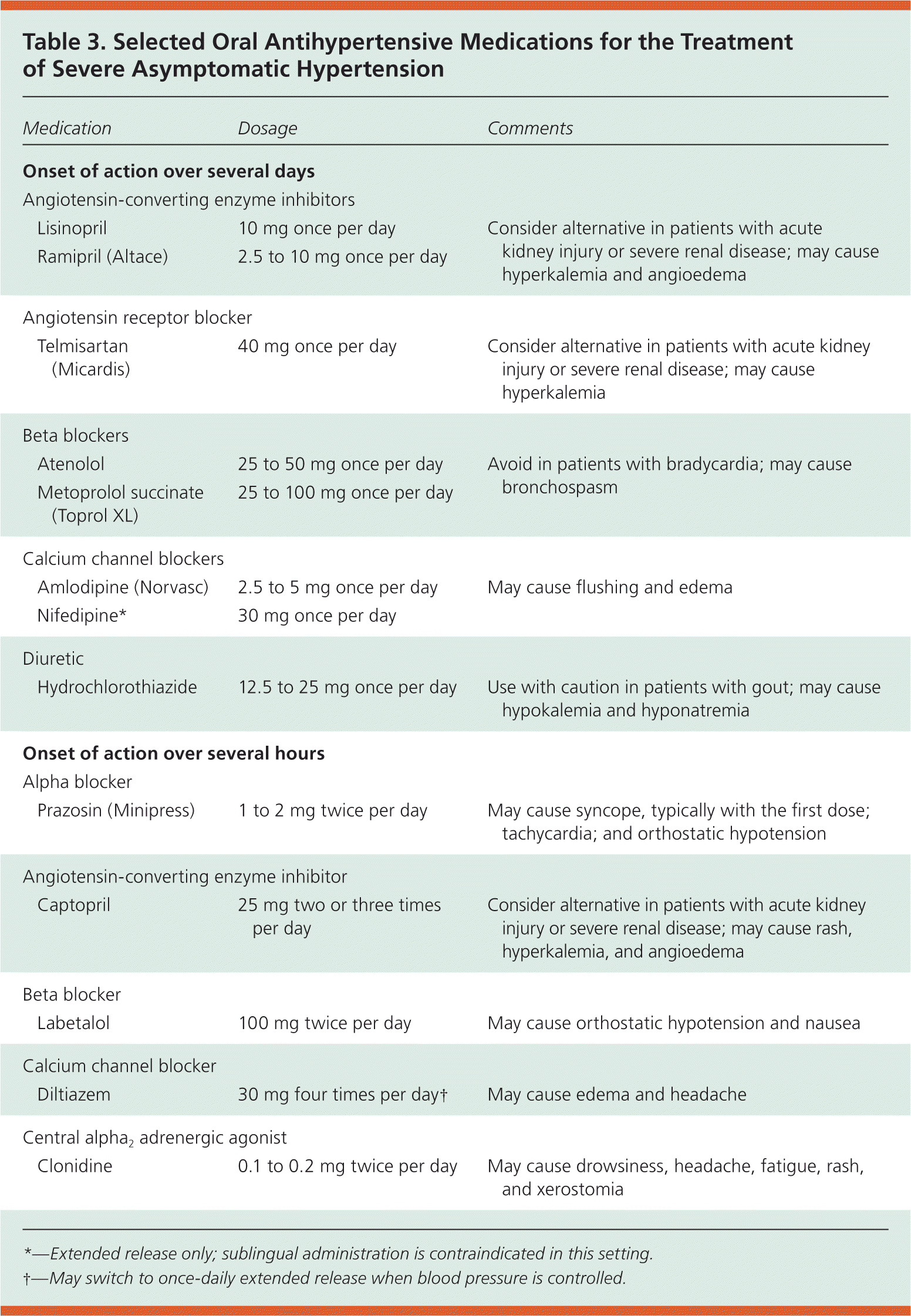
Despite the lack of evidence of an immediate increase in risk of major adverse cardiovascular events, primary care physicians often are hesitant to send patients with severe blood pressure elevations home. As a result, it remains common practice to acutely lower blood pressure using short-acting antihypertensives. Patients with symptoms such as headache, lightheadedness, shortness of breath, epistaxis, or anxiety are more likely to benefit from these agents.14,15,21 When blood pressure improves, long-acting antihypertensive therapy should be initiated, restarted, or adjusted.22 Table 3 includes selected oral antihypertensives for the treatment of severe asymptomatic hypertension.
Table 3. Selected Oral Antihypertensive Medications for the Treatment of Severe Asymptomatic Hypertension
| Medication | Dosage | Comments | |
|---|---|---|---|
| Onset of action over several days | |||
| Angiotensin-converting enzyme inhibitors | |||
| Lisinopril | 10 mg once per day | Consider alternative in patients with acute kidney injury or severe renal disease; may cause hyperkalemia and angioedema | |
| Ramipril (Altace) | 2.5 to 10 mg once per day | ||
| Angiotensin receptor blocker | |||
| Telmisartan (Micardis) | 40 mg once per day | Consider alternative in patients with acute kidney injury or severe renal disease; may cause hyperkalemia | |
| Beta blockers | |||
| Atenolol | 25 to 50 mg once per day | Avoid in patients with bradycardia; may cause bronchospasm | |
| Metoprolol succinate (Toprol XL) | 25 to 100 mg once per day | ||
| Calcium channel blockers | |||
| Amlodipine (Norvasc) | 2.5 to 5 mg once per day | May cause flushing and edema | |
| Nifedipine* | 30 mg once per day | ||
| Diuretic | |||
| Hydrochlorothiazide | 12.5 to 25 mg once per day | Use with caution in patients with gout; may cause hypokalemia and hyponatremia | |
| Onset of action over several hours | |||
| Alpha blocker | |||
| Prazosin (Minipress) | 1 to 2 mg twice per day | May cause syncope, typically with the first dose; tachycardia; and orthostatic hypotension | |
| Angiotensin-converting enzyme inhibitor | |||
| Captopril | 25 mg two or three times per day | Consider alternative in patients with acute kidney injury or severe renal disease; may cause rash, hyperkalemia, and angioedema | |
| Beta blocker | |||
| Labetalol | 100 mg twice per day | May cause orthostatic hypotension and nausea | |
| Calcium channel blocker | |||
| Diltiazem | 30 mg four times per day† | May cause edema and headache | |
| Central alpha2 adrenergic agonist | |||
| Clonidine | 0.1 to 0.2 mg twice per day | May cause drowsiness, headache, fatigue, rash, and xerostomia | |
*—Extended release only; sublingual administration is contraindicated in this setting.
†—May switch to once-daily extended release when blood pressure is controlled.
HOW QUICKLY SHOULD BLOOD PRESSURE BE LOWERED?
In the absence of acute target organ injury, blood pressure should be lowered gradually to less than 160/100 mm Hg, but not acutely by more than 20% to 25% of the mean arterial blood pressure over several days to weeks.21 Every two to four weeks, antihypertensive intensification is recommended to achieve target blood pressure goals.23 Aggressive blood pressure lowering in patients with severe asymptomatic hypertension can lead to adverse events, such as myocardial infarction, cerebrovascular accident, or syncope. Parenteral medication is not indicated and should be reserved for the management of hypertensive emergencies.13
Patients who have not been compliant often can safely resume their outpatient medications.10 Dosing adjustments and additions are recommended for those already on antihypertensive therapy. No specific medication classes are recommended for the initial management of severe asymptomatic hypertension. The Eighth Joint National Committee Report on Prevention, Detection, Evaluation, and Treatment of Hypertension (JNC 8) recommendations for the treatment of essential hypertension, which are based on quality randomized controlled trials, should be considered when initiating long-term therapy for severe asymptomatic hypertension.
In the general nonblack population, thiazide-type diuretics, calcium channel blockers, angiotensin-converting enzyme inhibitors, or angiotensin receptor blockers are recommended for initial treatment. In the black population, thiazide-type diuretics or calcium channel blockers are recommended. In patients with chronic kidney disease, an angiotensin-converting enzyme inhibitor or angiotensin receptor blocker improves renal outcomes.24 Additionally, a patient's preexisting comorbid conditions may dictate the preference of antihypertensive class 6,25 (Table 46 ). Severe asymptomatic hypertension generally requires two-drug therapy, and several meta-analyses clearly show superior blood pressure reduction with combination therapy vs. monotherapy.26
Table 4. Medication Preferences for Severe Asymptomatic Hypertension Based on Known Preexisting Factors

| Condition | Preferred medication class |
|---|---|
| Angina pectoris | Beta blockers, calcium channel blockers |
| Aortic aneurysm | Beta blockers |
| Asian or black race | Diuretics, calcium channel blockers |
| Atrial fibrillation | Beta blockers, calcium channel blockers (nondihydropyridine) |
| Cerebrovascular accident | All classes |
| Chronic obstructive pulmonary disease | All classes except beta blockers |
| Congestive heart failure | Diuretics, beta blockers, ACE inhibitors, ARBs, mineralocorticoid receptor antagonists |
| Diabetes mellitus | ACE inhibitors, ARBs |
| Left ventricular hypertrophy | ACE inhibitors, ARBs, calcium channel blockers |
| Myocardial infarction | Beta blockers, ACE inhibitors, ARBs |
| Peripheral vascular disease | ACE inhibitors, calcium channel blockers |
| Stable chronic kidney disease | ACE inhibitors, ARBs |
ACE = angiotensin-converting enzyme; ARB = angiotensin receptor blocker.
Adapted with permission from Mancia G, Fagard R, Narkiewicz K, et al. 2013 ESH/ESC guidelines for the management of arterial hypertension: the Task Force for the Management of Arterial Hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). Eur Heart J. 2013;34(28):2190.
WHO SHOULD BE HOSPITALIZED?
Hospitalization is rarely required for patients with severe asymptomatic hypertension. However, those with escalating blood pressure measurements, progressive symptoms of target organ injury, or evolving clinical evidence of acute target organ injury should be hospitalized.
There are no published data to determine what blood pressure measurement is too high. A Veterans Administration Cooperative trial from 1967 followed patients with diastolic blood pressure averaging between 115 and 129 mm Hg. No patients had a major adverse cardiovascular event within two months of enrollment.19 Although scientific evidence is lacking, patients with sustained diastolic blood pressure of 130 mm Hg or more should be considered for treatment with short-acting antihypertensives followed by long-acting agents. Symptomatic patients with persistent systolic blood pressure elevations exceeding 240 mm Hg or diastolic blood pressure greater than 130 mm Hg despite appropriate rest and treatment with short-acting antihypertensives may benefit from hospitalization.
HOW SHOULD HOSPITALIZED PATIENTS WITH SEVERE ASYMPTOMATIC HYPERTENSION BE MANAGED?
Inpatient treatment of acute hypertension is often aggressive, and intravenous antihypertensives are commonly used when blood pressure readings are only modestly elevated (151 to 170/101 to 110 mm Hg). However, there is no evidence that acute inpatient treatment of severe asymptomatic hypertension improves outcomes, and one study demonstrated increased hospital stays when intravenous antihypertensives were used.11
Blood pressure elevations during hospitalization are often exacerbated by pain, anxiety, or acute illness. When these factors have been excluded and the patient remains hypertensive, it is best practice to reinitiate or adjust oral antihypertensive therapy in those with preexisting hypertension. In patients without previous hypertension, oral antihypertensive therapy can be initiated during the hospitalization with close outpatient follow-up. Although there is often reluctance to discharge patients with systolic blood pressure of more than 180 mm Hg or diastolic blood pressure of more than 100 mm Hg, these values in the ambulatory clinic are appropriately managed in the outpatient setting.27 A significant benefit for hospitalized patients is the opportunity to recognize severe blood pressure elevations and improve transitional care for the primary care physician.28
Data Sources: We searched OvidSP, PubMed, Essential Evidence Plus, National Guideline Clearinghouse, Up-To-Date, and U.S. Preventive Services Task Force guidelines using the key words asymptomatic, elevated blood pressure, hypertension, hypertensive urgency, hypertensive emergency, emergency department, guidelines, antihypertensive agents, resistant hypertension, cardiovascular risk, assessment, management, pharmacologic, treatment, white-coat hypertension, screening, compliance, prevalence, evaluation, inpatient. Search dates: November 27, 2015; August 4, 2016; and January 25, 2017.
The opinions and assertions contained herein are the private views of the author and are not to be construed as official or as reflecting the views of the U.S. Army Medical Department or the U.S. Army Service at large.

