Cardiovascular disease is the leading cause of death and disability in postmenopausal women older than 50 years. Clinicians should use the pooled cohort risk assessment equations or another risk calculator every three to five years to estimate a woman's 10-year risk of atherosclerotic cardiovascular disease, including myocardial infarction and stroke. Major guidelines concur that women at average risk of breast cancer benefit from screening mammography at least every other year from 50 to 74 years of age. Several effective options for colorectal cancer screening are recommended for women 50 to 75 years of age. Cervical cancer screening should occur at three- or five-year intervals depending on the test used, and can generally be discontinued after 65 years of age or total hysterectomy for benign disease. Screening for ovarian cancer is not recommended. Clinicians should consider screening for sexually transmitted infections in older women at high risk. Postmenopausal women should be routinely screened for depression, alcohol abuse, and intimate partner violence.
Postmenopausal women have a number of unique health-promotion and disease-prevention needs. However, many effective preventive health strategies for postmenopausal women are underutilized.1 This article reviews evidence-based preventive services recommendations for asymptomatic post-menopausal women from the U.S. Preventive Services Task Force (USPSTF), which are supported by the American Academy of Family Physicians. Relevant guidelines from other professional groups are also described.
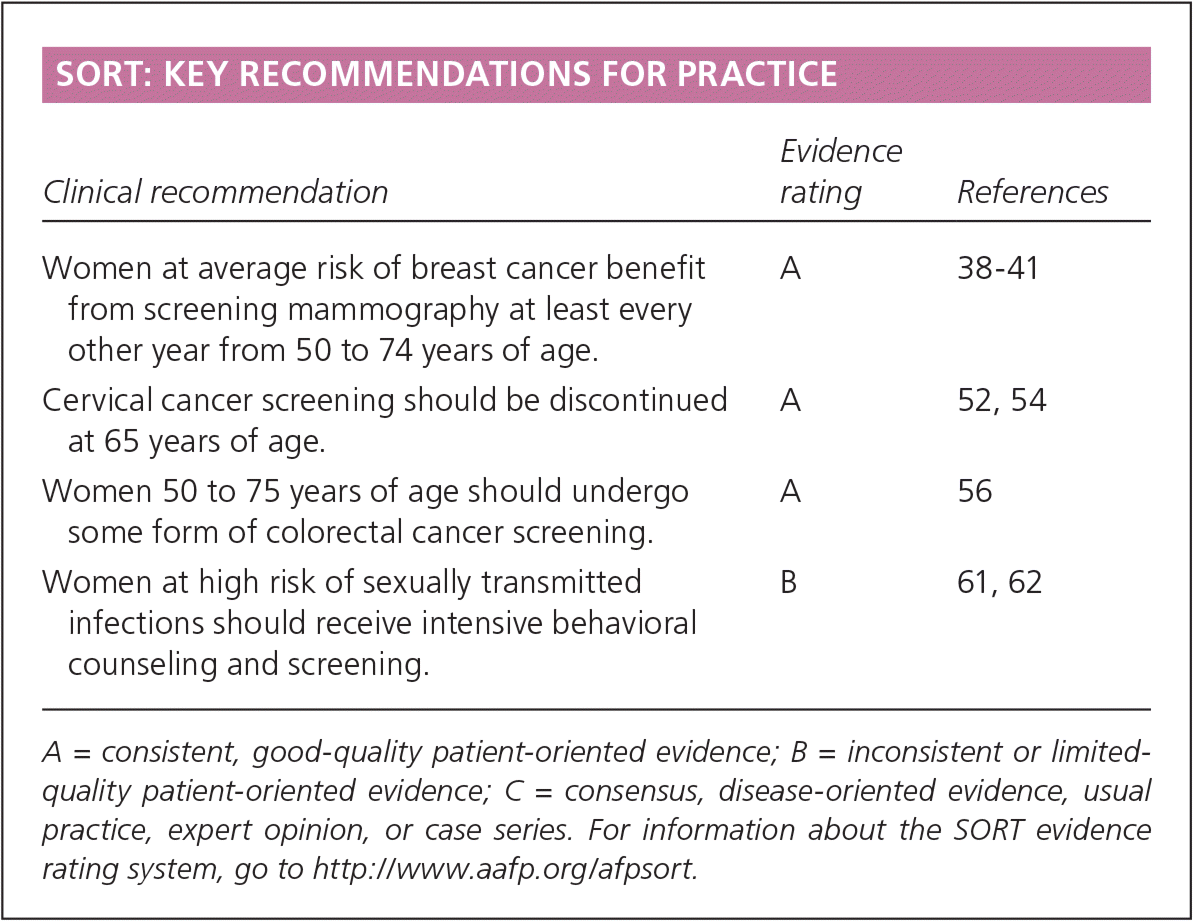
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Women at average risk of breast cancer benefit from screening mammography at least every other year from 50 to 74 years of age. | A | 38–41 |
| Cervical cancer screening should be discontinued at 65 years of age. | A | 52, 54 |
| Women 50 to 75 years of age should undergo some form of colorectal cancer screening. | A | 56 |
| Women at high risk of sexually transmitted infections should receive intensive behavioral counseling and screening. | B | 61, 62 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
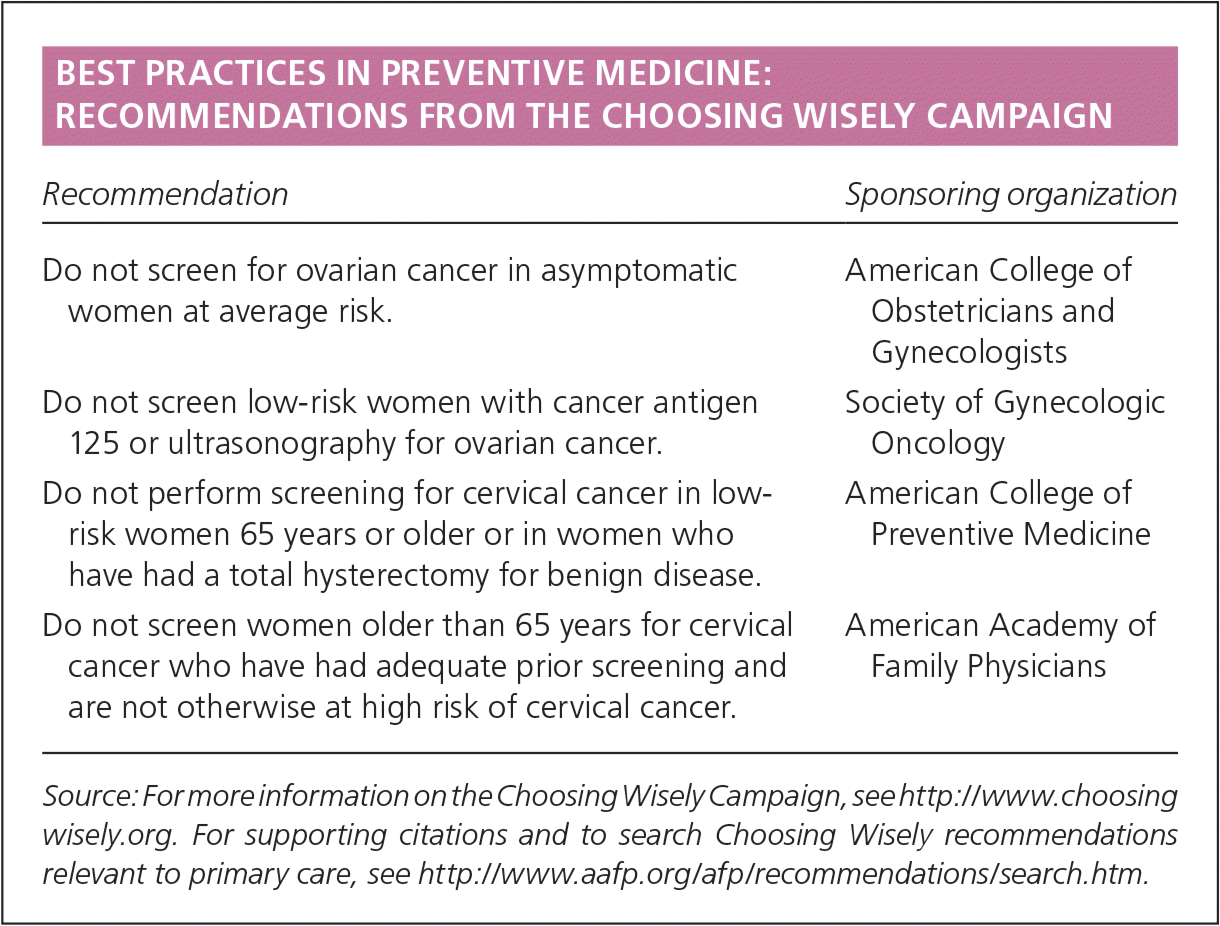
BEST PRACTICES IN PREVENTIVE MEDICINE: RECOMMENDATIONS FROM THE CHOOSING WISELY CAMPAIGN
| Recommendation | Sponsoring organization |
|---|---|
| Do not screen for ovarian cancer in asymptomatic women at average risk. | American College of Obstetricians and Gynecologists |
| Do not screen low-risk women with cancer antigen 125 or ultrasonography for ovarian cancer. | Society of Gynecologic Oncology |
| Do not perform screening for cervical cancer in low-risk women 65 years or older or in women who have had a total hysterectomy for benign disease. | American College of Preventive Medicine |
| Do not screen women older than 65 years for cervical cancer who have had adequate prior screening and are not otherwise at high risk of cervical cancer. | American Academy of Family Physicians |
Source: For more information on the Choosing Wisely Campaign, see http://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
Cardiovascular Disease Screening and Prevention
Cardiovascular disease (CVD) is the leading cause of death and disability in women older than 50 years, exceeding the number of deaths from malignant neoplasms, diabetes mellitus, and chronic lower respiratory diseases combined.2 The prevalence of CVD increases rapidly at the onset of menopause and continues to increase through the post-menopausal period.
CARDIOVASCULAR RISK STRATIFICATION
Periodic cardiovascular risk assessment in postmenopausal women can identify risk factors and enable implementation of risk-reduction strategies (Table 13–16 and Table 217,18 ). The 2013 American College of Cardiology/American Heart Association (ACC/AHA) guideline recommends using the pooled cohort risk assessment equations (http://tools.acc.org/ASCVD-Risk-Estimator/) every three to five years to calculate the 10-year risk of atherosclerotic CVD, including myocardial infarction and stroke.6,19–21 The guideline supports the use of statins for primary prevention of atherosclerotic CVD in high-risk patients and for secondary prevention in all patients with a history of atherosclerotic CVD. Although concerns have been raised that the pooled cohort equations overestimate risk, other risk scores, including the traditional Framingham risk score, also overestimate risk by 25% to 115%.22,23 The pooled cohort equations and Framingham risk score apply only to women younger than 80 years, limiting their use in the older population.
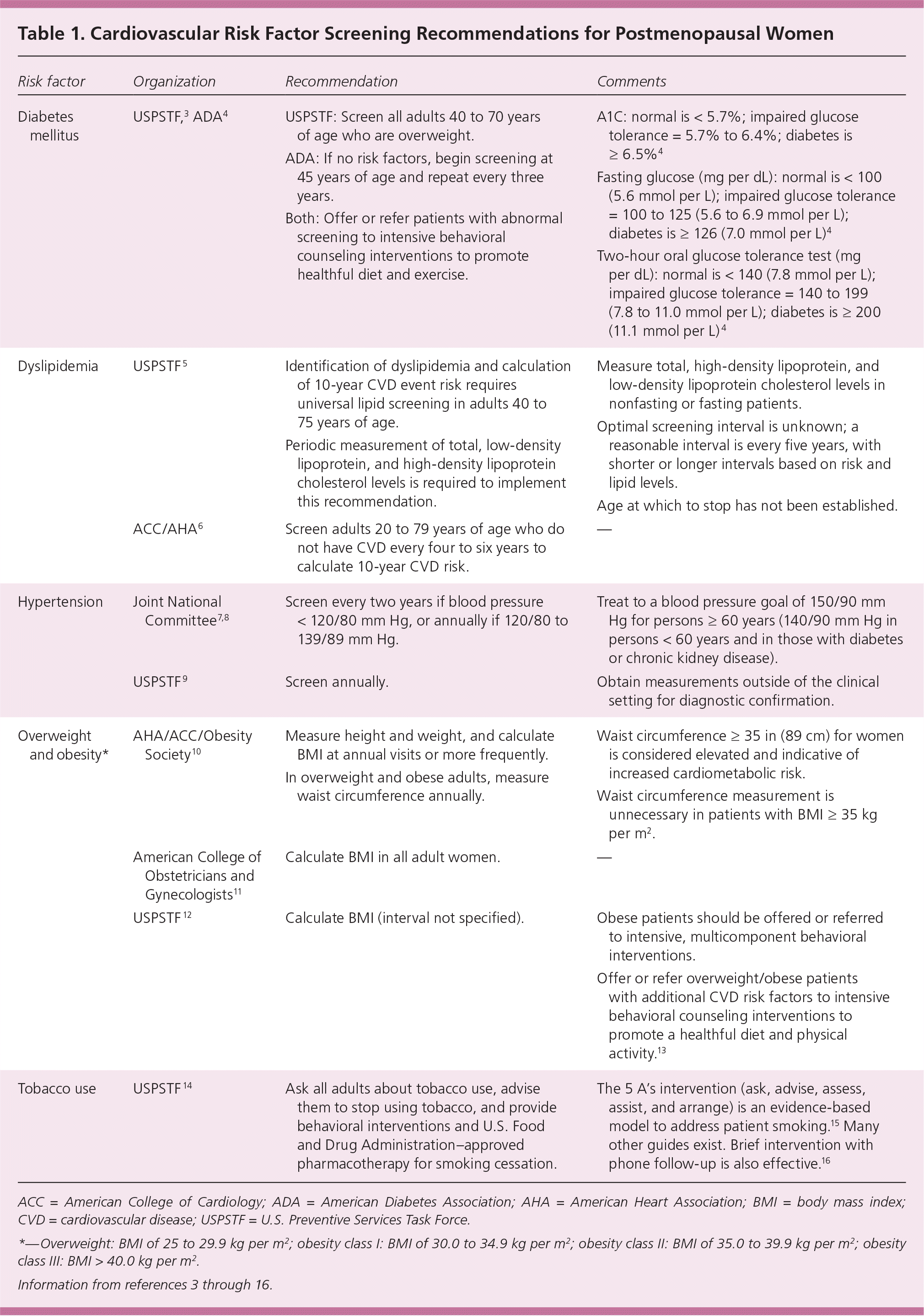
Table 1. Cardiovascular Risk Factor Screening Recommendations for Postmenopausal Women
| Risk factor | Organization | Recommendation | Comments |
|---|---|---|---|
| Diabetes mellitus | USPSTF,3 ADA4 | USPSTF: Screen all adults 40 to 70 years of age who are overweight. | A1C: normal is < 5.7%; impaired glucose tolerance = 5.7% to 6.4%; diabetes is ≥ 6.5%4 |
| ADA: If no risk factors, begin screening at 45 years of age and repeat every three years. | Fasting glucose (mg per dL): normal is < 100 (5.6 mmol per L); impaired glucose tolerance = 100 to 125 (5.6 to 6.9 mmol per L); diabetes is ≥ 126 (7.0 mmol per L)4 | ||
| Both: Offer or refer patients with abnormal screening to intensive behavioral counseling interventions to promote healthful diet and exercise. | Two-hour oral glucose tolerance test (mg per dL): normal is < 140 (7.8 mmol per L); impaired glucose tolerance = 140 to 199 (7.8 to 11.0 mmol per L); diabetes is ≥ 200 (11.1 mmol per L)4 | ||
| Dyslipidemia | USPSTF5 | Identification of dyslipidemia and calculation of 10-year CVD event risk requires universal lipid screening in adults 40 to 75 years of age. | Measure total, high-density lipoprotein, and low-density lipoprotein cholesterol levels in nonfasting or fasting patients. |
| Periodic measurement of total, low-density lipoprotein, and high-density lipoprotein cholesterol levels is required to implement this recommendation. | Optimal screening interval is unknown; a reasonable interval is every five years, with shorter or longer intervals based on risk and lipid levels. | ||
| Age at which to stop has not been established. | |||
| ACC/AHA6 | Screen adults 20 to 79 years of age who do not have CVD every four to six years to calculate 10-year CVD risk. | — | |
| Hypertension | Joint National Committee7,8 | Screen every two years if blood pressure < 120/80 mm Hg, or annually if 120/80 to 139/89 mm Hg. | Treat to a blood pressure goal of 150/90 mm Hg for persons ≥ 60 years (140/90 mm Hg in persons < 60 years and in those with diabetes or chronic kidney disease). |
| USPSTF9 | Screen annually. | Obtain measurements outside of the clinical setting for diagnostic confirmation. | |
| Overweight and obesity* | AHA/ACC/Obesity Society10 | Measure height and weight, and calculate BMI at annual visits or more frequently. | Waist circumference ≥ 35 in (89 cm) for women is considered elevated and indicative of increased cardiometabolic risk. |
| In overweight and obese adults, measure waist circumference annually. | Waist circumference measurement is unnecessary in patients with BMI ≥ 35 kg per m2 | ||
| American College of Obstetricians and Gynecologists11 | Calculate BMI in all adult women. | — | |
| USPSTF12 | Calculate BMI (interval not specified). | Obese patients should be offered or referred to intensive, multicomponent behavioral interventions. | |
| Offer or refer overweight/obese patients with additional CVD risk factors to intensive behavioral counseling interventions to promote a healthful diet and physical activity.13 | |||
| Tobacco use | USPSTF14 | Ask all adults about tobacco use, advise them to stop using tobacco, and provide behavioral interventions and U.S. Food and Drug Administration–approved pharmacotherapy for smoking cessation. | The 5 A's intervention (ask, advise, assess, assist, and arrange) is an evidence-based model to address patient smoking.15 Many other guides exist. Brief intervention with phone follow-up is also effective.16 |
ACC = American College of Cardiology; ADA = American Diabetes Association; AHA = American Heart Association; BMI = body mass index; CVD = cardiovascular disease; USPSTF = U.S. Preventive Services Task Force.
*—Overweight: BMI of 25 to 29.9 kg per m2; obesity class I: BMI of 30.0 to 34.9 kg per m2; obesity class II: BMI of 35.0 to 39.9 kg per m2; obesity class III: BMI > 40.0 kg per m2.
Table 2. Lifestyle Recommendations for Postmenopausal Women

| Topic | Organization | Recommendation |
|---|---|---|
| Diet | AHA/ACC17 | Recommended diets should include vegetables, fruits, and whole grains, and should limit sweets, sugar-sweetened beverages, and red meats; no more than 5% to 6% of calories should come from saturated fat and/or trans fat. |
| Diets should be adapted to personal and cultural food preferences. | ||
| Physical activity | AHA/ACC17 | Adults should engage in moderate- to vigorous-intensity aerobic physical activity for an average of 40 minutes three or four times per week. |
| American College of Sports Medicine/AHA18 | All healthy adults 18 to 65 years of age should engage in moderate-intensity aerobic physical activity (e.g., brisk walking) for at least 30 minutes on five days per week, or vigorous-intensity aerobic physical activity (e.g., jogging) for at least 20 minutes on three days per week. |
ACC = American College of Cardiology; AHA = American Heart Association.
CORONARY HEART DISEASE
The complex effects of hormones on the cardiovascular system result in different presentations of coronary heart disease in women, with a higher incidence of angina, a lower burden of obstructive coronary artery disease (CAD) on angiography, and a poorer prognosis compared with men. In addition, post-menopausal women are more likely to develop heart failure with preserved ejection fraction.24 Table 3 provides a summary of screening recommendations for CVD risk factors.25–30
Table 3. Cardiovascular Screening Recommendations for Postmenopausal Women

| Condition | Organization | Screening modality | Recommendation | |
|---|---|---|---|---|
| Asymptomatic carotid stenosis | ACC Foundation/AHA, et al.25 | Duplex ultrasonography | Screening is not recommended in the general population. | |
| USPSTF26 | Duplex ultrasonography | Screening is not recommended in the general population. | ||
| Coronary artery disease | ACC/AHA27 | Exercise testing | Consider screening exercise testing in patients with multiple risk factors for CHD to guide risk-reduction therapy, in women older than 55 years who are sedentary and plan to start a vigorous exercise program, and in patients with public safety occupations. | |
| USPSTF28 | Resting or exercise electrocardiography | Do not routinely screen adults at low risk of CHD events. | ||
| Evidence is insufficient to recommend for or against routine screening in adults at increased risk of CHD events. | ||||
| Lower extremity peripheral artery disease | ACC Foundation/AHA29 | Ankle-brachial index | Consider screening if:
| |
| USPSTF30 | Ankle-brachial index | Evidence is insufficient to screen for peripheral artery disease and cardiovascular risk factors with the ankle-brachial index in adults. | ||
ACC = American College of Cardiology; AHA = American Heart Association; CHD = coronary heart disease; USPSTF = U.S. Preventive Services Task Force.
STROKE AND ATRIAL FIBRILLATION
Cerebrovascular disease accounts for a higher proportion of cardiovascular events and mortality in women, with 50,000 more U.S. women than men dying from strokes each year.2 Unique risk factors for stroke in post-menopausal women include the use of hormone therapy and a higher prevalence of hypertension in older persons. In a nationwide study of Finnish women who discontinued menopausal hormone therapy, the risk of cardiac- or stroke-related death increased 26% to 66% in the first year after discontinuation.31 Women have a higher stroke risk and mortality in the setting of atrial fibrillation compared with men. Risk assessment for stroke using the CHA2DS2-VASc score (http://reference.medscape.com/calculator/chads-vasc-af-stroke) accounts for this increased risk by adding an extra point for women.24,32,33
ASPIRIN AND STATINS FOR PRIMARY PREVENTION
The USPSTF and ACC/AHA recommend aspirin and statins for primary prevention of CVD in select high-risk patients who are at low risk of adverse effects from these medications5,6,34 (Table 45,6,22,34–37 ).
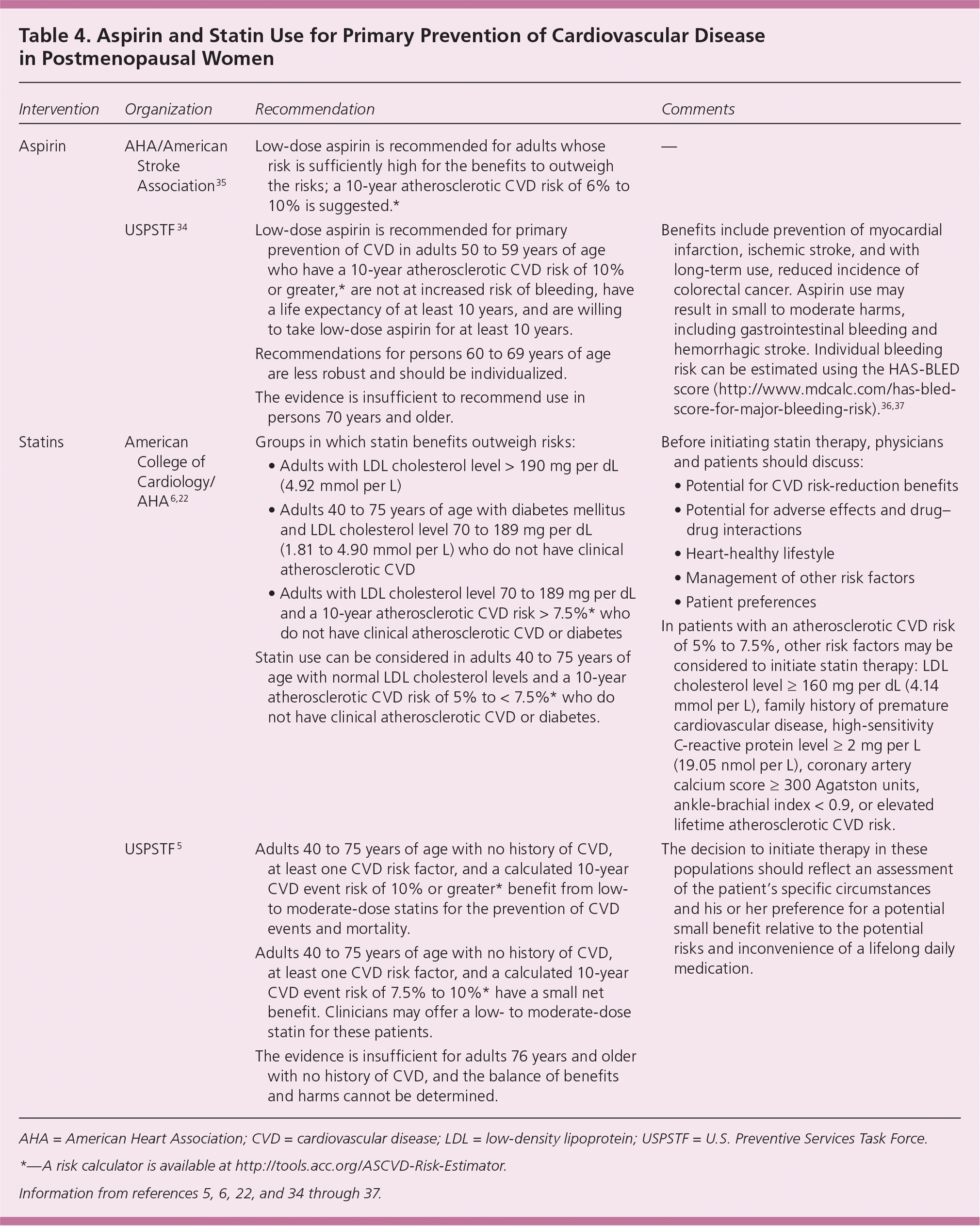
Table 4. Aspirin and Statin Use for Primary Prevention of Cardiovascular Disease in Postmenopausal Women
| Intervention | Organization | Recommendation | Comments |
|---|---|---|---|
| Aspirin | AHA/American Stroke Association35 | Low-dose aspirin is recommended for adults whose risk is sufficiently high for the benefits to outweigh the risks; a 10-year atherosclerotic CVD risk of 6% to 10% is suggested.* | — |
| USPSTF34 | Low-dose aspirin is recommended for primary prevention of CVD in adults 50 to 59 years of age who have a 10-year atherosclerotic CVD risk of 10% or greater,* are not at increased risk of bleeding, have a life expectancy of at least 10 years, and are willing to take low-dose aspirin for at least 10 years. | Benefits include prevention of myocardial infarction, ischemic stroke, and with long-term use, reduced incidence of colorectal cancer. Aspirin use may result in small to moderate harms, including gastrointestinal bleeding and hemorrhagic stroke. Individual bleeding risk can be estimated using the HAS-BLEDscore (http://www.mdcalc.com/has-bled-score-for-major-bleeding-risk).36,37 | |
| Recommendations for persons 60 to 69 years of age are less robust and should be individualized. | |||
| The evidence is insufficient to recommend use in persons 70 years and older. | |||
| Statins | American College of Cardiology/AHA6,22 | Groups in which statin benefits outweigh risks:
| Before initiating statin therapy, physicians and patients should discuss:
|
| Statin use can be considered in adults 40 to 75 years of age with normal LDL cholesterol levels and a 10-year atherosclerotic CVD risk of 5% to < 7.5%* who do not have clinical atherosclerotic CVD or diabetes. | In patients with an atherosclerotic CVD risk of 5% to 7.5%, other risk factors may be considered to initiate statin therapy: LDL cholesterol level ≥ 160 mg per dL (4.14 mmol per L), family history of premature cardiovascular disease, high-sensitivity C-reactive protein level ≥ 2 mg per L (19.05 nmol per L), coronary artery calcium score ≥ 300 Agatston units, ankle-brachial index < 0.9, or elevated lifetime atherosclerotic CVD risk. | ||
| USPSTF5 | Adults 40 to 75 years of age with no history of CVD, at least one CVD risk factor, and a calculated 10-year CVD event risk of 10% or greater* benefit from low- to moderate-dose statins for the prevention of CVD events and mortality. | The decision to initiate therapy in these populations should reflect an assessment of the patient's specific circumstances and his or her preference for a potential small benefit relative to the potential risks and inconvenience of a lifelong daily medication. | |
| Adults 40 to 75 years of age with no history of CVD, at least one CVD risk factor, and a calculated 10-year CVD event risk of 7.5% to 10%* have a small net benefit. Clinicians may offer a low- to moderate-dose statin for these patients. | |||
| The evidence is insufficient for adults 76 years and older with no history of CVD, and the balance of benefits and harms cannot be determined. |
AHA = American Heart Association; CVD = cardiovascular disease; LDL = low-density lipoprotein; USPSTF = U.S. Preventive Services Task Force.
*—A risk calculator is available at http://tools.acc.org/ASCVD-Risk-Estimator.
Cancer Screening
BREAST CANCER
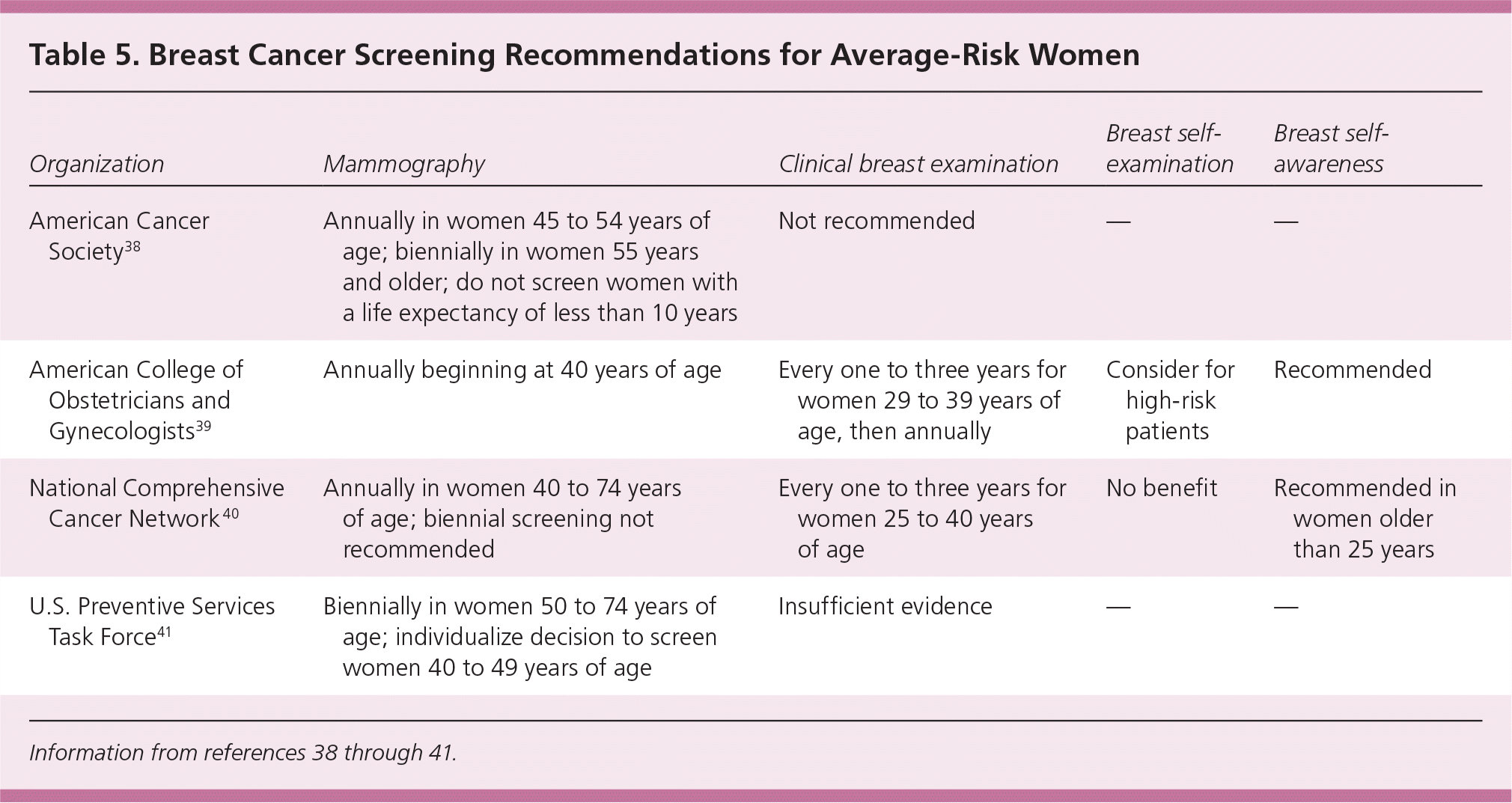
There is agreement across multiple organizational guidelines that average-risk women benefit from screening mammography at least every other year from 50 to 74 years of age (Table 5).38–41 For high-risk women, the USPSTF found insufficient evidence to judge the balance of benefits and harms for screening magnetic resonance imaging.41 The American Cancer Society and the National Comprehensive Cancer Network recommend considering the addition of annual magnetic resonance imaging in women whose lifetime breast cancer risk is at least 20%, as defined by models largely dependent on family history, a history of atypical hyperplasia on breast biopsy, or who were exposed as a child to therapeutic chest radiation.38,40
Table 5. Breast Cancer Screening Recommendations for Average-Risk Women
| Organization | Mammography | Clinical breast examination | Breast self-examination | Breast self-awareness |
|---|---|---|---|---|
| American Cancer Society38 | Annually in women 45 to 54 years of age; biennially in women 55 years and older; do not screen women with a life expectancy of less than 10 years | Not recommended | — | — |
| American College of Obstetricians and Gynecologists39 | Annually beginning at 40 years of age | Every one to three years for women 29 to 39 years of age, then annually | Consider for high-risk patients | Recommended |
| National Comprehensive Cancer Network40 | Annually in women 40 to 74 years of age; biennial screening not recommended | Every one to three years for women 25 to 40 years of age | No benefit | Recommended in women older than 25 years |
| U.S. Preventive Services Task Force41 | Biennially in women 50 to 74 years of age; individualize decision to screen women 40 to 49 years of age | Insufficient evidence | — | — |
The USPSTF recommends that postmenopausal women at high risk of breast cancer and low risk of medication adverse effects be offered tamoxifen or raloxifene (Evista).42 Based on expert opinion, the American Cancer Society and the National Comprehensive Cancer Network include aromatase inhibitors, exemestane (Aromasin), or anastrozole (Arimidex) as additional options.38,43
Breast cancer prevention trials historically defined high-risk women as those with a 1.66% or greater five-year risk of invasive breast cancer as calculated by the Gail model (Breast Cancer Risk Assessment Tool, http://www.cancer.gov/bcrisktool/Default.aspx).44 However, this cutoff includes almost all women older than 65 years, many of whom will not experience a net benefit from the use of risk-reducing medication.42 A 3% or greater five-year risk of invasive breast cancer is more likely to identify postmenopausal candidates for chemoprophylaxis.45 The Tyrer-Cuzick model (International Breast Intervention Study breast cancer risk evaluation tool, http://www.ems-trials.org/riskevaluator) incorporates the Gail model risk factors, as well as age, use of hormone therapy, and body mass index.46 It defines high risk as more than 20% lifetime risk.
The USPSTF recommends genetic counseling and, if indicated, BRCA testing in women with Ashkenazi Jewish ethnicity or a family history of breast cancer before 50 years of age, bilateral breast cancer, breast and ovarian cancer, breast cancer in at least one male family member, multiple cases of breast cancer in the family, or one or more family member with two primary types of BRCA-related cancer.47 The American College of Obstetricians and Gynecologists advises genetic testing if risk assessment is consistent with a 20% to 25% lifetime risk of breast and ovarian cancer.39
OVARIAN CANCER
The USPSTF recommends against screening for ovarian cancer.48 Preliminary results from the U.K. Collaborative Trial of Ovarian Cancer Screening, which used a multimodal screening protocol combining history, changes in the cancer antigen 125 level over time, and high-resolution ultrasonography, suggested a possible mortality benefit.49 However, it remains uncertain if implementation of a proprietary algorithm will produce more benefits than harms.50,51
CERVICAL CANCER
Most cervical cancers arise in women who were never screened or received inadequate screening.52 Postmenopausal women should receive human papillomavirus and cytology cotesting every five years, or cytology alone every three years, until 65 years of age (eTable A). Human papillomavirus screening every three years can be considered for women older than 25 years.52,53 Screening should be discontinued in women who undergo total hysterectomy for benign disease.54 Women who undergo subtotal hysterectomy (removal of the uterus with retention of the cervix) should continue regular screening.52,54
eTable A. Cervical Cancer Screening Recommendations for Postmenopausal Women

| Age | Preferred testing methods | Acceptable testing method |
|---|---|---|
| 30 to 65 years | HPV and cytology cotesting every five years; there is no indication for annual screening in average-risk women. | Cytology alone every three years; in women older than 25 years, FDA-approved primary HPV screening every three years can be considered as an alternative to current cytology-based cervical cancer screening methods. |
| > 65 years | Screening should be discontinued at 65 years of age in women with a history of negative screening results (three consecutive negative cytology results or two consecutive negative cotesting results in the previous 10 years, with the most recent test within five years) and no history of CIN 2 or higher.* | — |
note: Women who have undergone hysterectomy (with removal of the cervix) and have no history of CIN 2 or higher do not require cytology or HPV screening regardless of age. The American Society for Colposcopy and Cervical Pathology mobile app may help in applying screening recommendations (http://www.asccp.org/Bookstore/ASCCP-Mobile-App).
CIN = cervical intraepithelial neoplasia; FDA = U.S. Food and Drug Administration; HPV = human papillomavirus.
*—Exceptions: Women with a history of CIN 2 or 3, or adenocarcinoma in situ should continue screening for 20 years after regression or management, even if screening extends beyond 65 years of age; women should continue screening even if they have had a total (cervix removed) hysterectomy if they have a history of CIN 2 or higher in the past 20 years or cervical cancer at any point (cytology alone every three years for 20 years after initial surveillance); high-risk women (e.g., those with human immunodeficiency virus infection, immunocompromised women such as solid organ transplant recipients, women exposed to diethylstilbestrol in utero) require annual screening throughout their lives.
Information from:
Committee on Practice Bulletins—Gynecology. Practice bulletin no. 168: cervical cancer screening and prevention. Obstet Gynecol. 2016;128(4):e111–e130.
Huh WK, Ault KA, Chelmow D, et al. Use of primary high-risk human papillomavirus testing for cervical cancer screening: interim clinical guidance. Obstet Gynecol. 2015;125(2):330–337.
U.S. Preventive Services Task Force. Cervical cancer: screening. March 2012. http://www.uspreventiveservicestaskforce.org/Page/Document/UpdateSummaryFinal/cervical-cancer-screening?ds=1&s=Cervix. Accessed March 1, 2016.
COLORECTAL CANCER
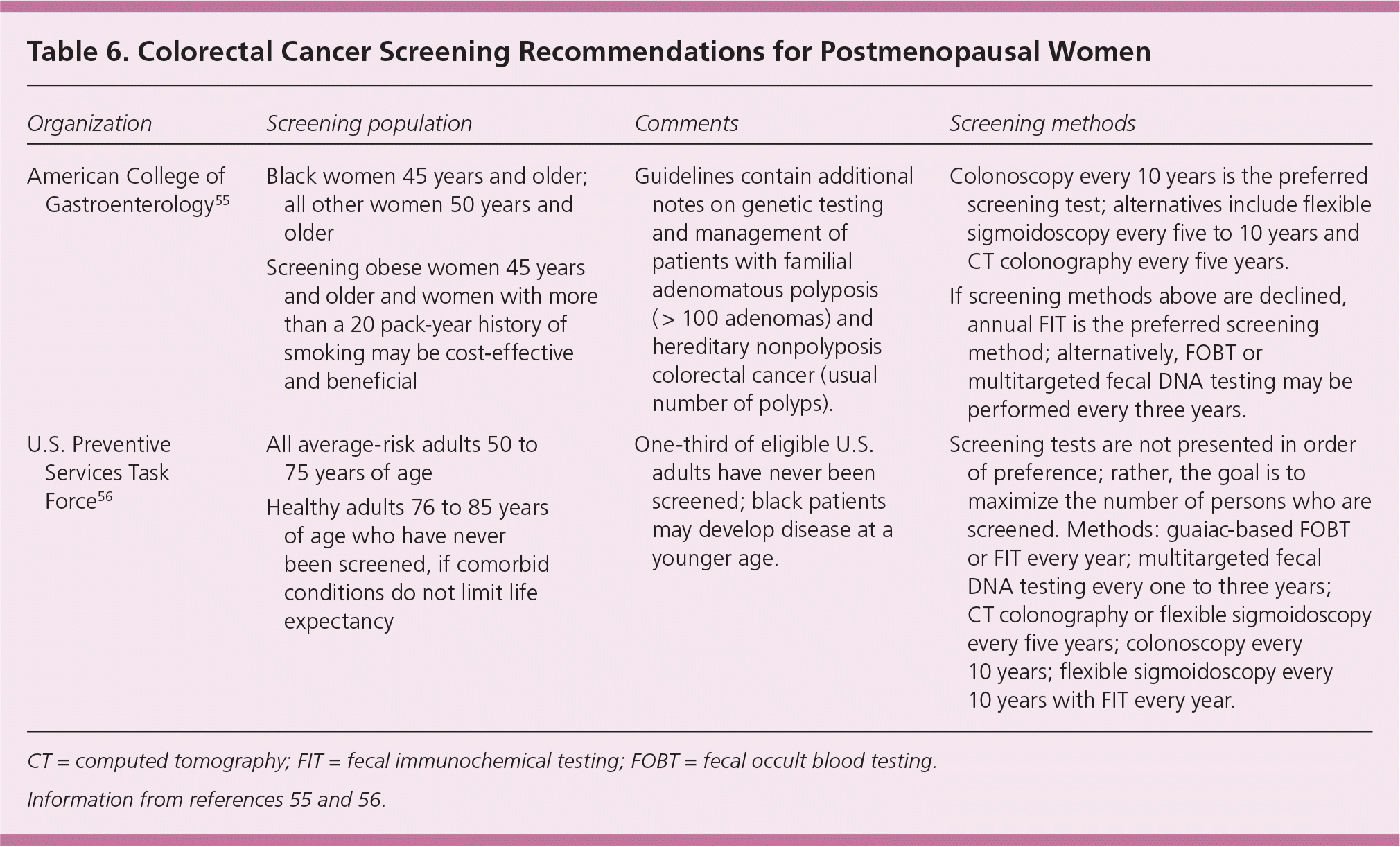
The American College of Gastroenterology recommends colonoscopy every 10 years beginning at 50 years of age in average-risk patients, including those who have a first-degree relative diagnosed with colorectal cancer or an advanced adenoma at 60 years or older.55 Patients with relatives diagnosed before 60 years of age should be screened every five years beginning at 40 years of age or 10 years younger than the relative at the time of diagnosis. The USPSTF recommends screening for colorectal cancer beginning at 50 years of age and continuing through 75 years of age, then individualized decision making in patients 76 to 85 years of age56 (Table 655,56). High-risk women who may require more intensive screening and/or genetic testing include those with a history of genetic disorders (e.g., familial adenomatous polyposis), inflammatory bowel disease, or a previous adenomatous polyp or colorectal cancer.56
Table 6. Colorectal Cancer Screening Recommendations for Postmenopausal Women
| Organization | Screening population | Comments | Screening methods |
|---|---|---|---|
| American College of Gastroenterology55 | Black women 45 years and older; all other women 50 ~years and older | Guidelines contain additional notes on genetic testing and management of patients with familial adenomatous polyposis (> 100 adenomas) and hereditary nonpolyposis colorectal cancer (usual number of polyps). | Colonoscopy every 10 years is the preferred screening test; alternatives include flexible sigmoidoscopy every five to 10 years and CT colonography every five years. |
| Screening obese women 45 years and older and women with more than a 20 pack-year history of smoking may be cost-effective and beneficial | If screening methods above are declined, annual FIT is the preferred screening method; alternatively, FOBT or multitargeted fecal DNA testing may be performed every three years. | ||
| U.S. Preventive Services Task Force56 | All average-risk adults 50 to 75 years of age | One-third of eligible U.S. adults have never been screened; black patients may develop disease at a younger age. | Screening tests are not presented in order of preference; rather, the goal is to maximize the number of persons who are screened. Methods: guaiac-based FOBT or FIT every year; multitargeted fecal DNA testing every one to three years; CT colonography or flexible sigmoidoscopy every five years; colonoscopy every 10 years; flexible sigmoidoscopy every 10 years with FIT every year. |
| Healthy adults 76 to 85 years of age who have never been screened, if comorbid conditions do not limit life expectancy |
CT = computed tomography; FIT = fecal immunochemical testing; FOBT = fecal occult blood testing.
Osteoporosis Screening
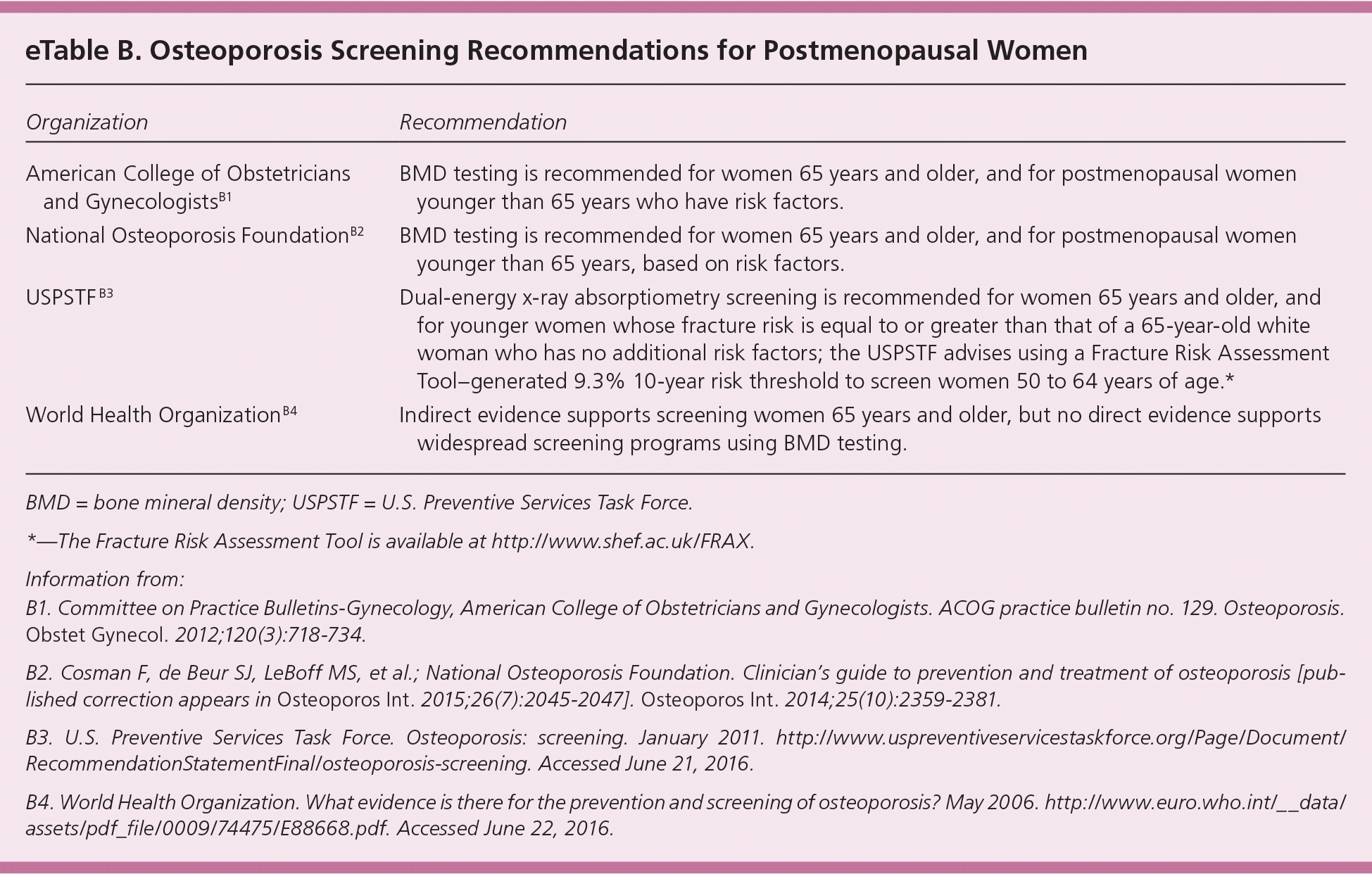
Many postmenopausal women with osteoporosis do not receive preventive care for fractures.57,58 eTable B summarizes osteoporosis screening recommendations. The optimal interval for repeat screening in postmenopausal women with normal or mildly decreased bone mineral density is uncertain.58 Diagnostic and treatment criteria for osteoporosis rely on hip and lumbar spine dual-energy x-ray absorptiometry measurements.58
eTable B. Osteoporosis Screening Recommendations for Postmenopausal Women
| Organization | Recommendation |
|---|---|
| American College of Obstetricians and GynecologistsB1 | BMD testing is recommended for women 65 years and older, and for postmenopausal women younger than 65 years who have risk factors. |
| National Osteoporosis FoundationB2 | BMD testing is recommended for women 65 years and older, and for postmenopausal women younger than 65 years, based on risk factors. |
| USPSTFB3 | Dual-energy x-ray absorptiometry screening is recommended for women 65 years and older, and for younger women whose fracture risk is equal to or greater than that of a 65-year-old white woman who has no additional risk factors; the USPSTF advises using a Fracture Risk Assessment Tool–generated 9.3% 10-year risk threshold to screen women 50 to 64 years of age.* |
| World Health OrganizationB4 | Indirect evidence supports screening women 65 years and older, but no direct evidence supports widespread screening programs using BMD testing. |
BMD = bone mineral density; USPSTF = U.S. Preventive Services Task Force.
*—The Fracture Risk Assessment Tool is available at http://www.shef.ac.uk/FRAX.
Information from:
B1. Committee on Practice Bulletins-Gynecology, American College of Obstetricians and Gynecologists. ACOG practice bulletin no. 129. Osteoporosis. Obstet Gynecol. 2012;120(3):718–734.
B2. Cosman F, de Beur SJ, LeBoff MS, et al.; National Osteoporosis Foundation. Clinician's guide to prevention and treatment of osteoporosis [published correction appears in Osteoporos Int. 2015;26(7):2045–2047]. Osteoporos Int. 2014;25(10):2359–2381.
B3. U.S. Preventive Services Task Force. Osteoporosis: screening. January 2011. http://www.uspreventiveservicestaskforce.org/Page/Document/RecommendationStatementFinal/osteoporosis-screening. Accessed June 21, 2016.
B4. World Health Organization. What evidence is there for the prevention and screening of osteoporosis? May 2006. http://www.euro.who.int/__data/assets/pdf_file/0009/74475/E88668.pdf. Accessed June 22, 2016.
In addition to adequate calcium and vitamin D intake and weight-bearing exercise, multiple drug therapies are approved by the U.S. Food and Drug Administration to reduce fracture risk, including bisphosphonates, parathyroid hormone, raloxifene, and estrogen.58
Fall Prevention
According to the USPSTF, effective fall prevention measures include daily intake of 600 to 800 IU of vitamin D, weight-bearing exercise, balance training three times per week, muscle strengthening twice per week, and 150 minutes per week of moderate-intensity or 75 minutes per week of vigorous-intensity aerobic physical activity.59 Vision correction, medication discontinuation, protein supplementation, education and counseling, and home hazard modification may be helpful in select cases, but are not routinely recommended.
STI Screening and Prevention
An estimated 65% of women 51 to 64 years of age engage in sexual intercourse at least once per week.60 Relationship transitions, the availability of erectile dysfunction treatments, and underutilization of condoms contribute to the increasing incidence of sexually transmitted infections (STIs) in older women.61,62 Thinning, less elastic postmenopausal vaginal epithelium facilitates transmission of STIs via coital trauma. One American study found that 1% of widowed women 67 to 99 years of age developed an STI during a nine-year study.63 The USPSTF recommends that high-risk sexually active women receive intensive behavioral counseling to reduce STI risk, and annual screening for chlamydia, gonorrhea, syphilis, and human immunodeficiency virus (HIV) infection.62 Regardless of risk, all women should receive HIV screening at least once before 65 years of age. Counseling resources are available through the Centers for Disease Control and Prevention at http://www.cdc.gov/std/prevention/default.htm.
Psychosocial Issues
The USPSTF recommends routinely screening postmenopausal women for depression, alcohol abuse, and intimate partner violence (eTable C).
eTable C. Psychosocial Considerations for Postmenopausal Women

| Topic | Comments | Suggested screening method |
|---|---|---|
| Alcohol misuse/abuse | The USPSTF recommends that clinicians screen persons 18 years and older for alcohol misuse and provide persons engaged in risky or hazardous drinking with brief behavioral counseling interventions to reduce alcohol misuse.C1 | CAGE questionnaire*C2
|
| Depression | The USPSTF recommends screening all adults, including older adults, for depression.C3 | Patient Health Questionnaire, Hospital Anxiety and Depression Scale, Geriatric Depression Scale |
| Depression is more common in women than in men, but not more common in postmenopausal women. | ||
| Intimate partner violence† | The U.S. Department of Health and Human Services has recommended that screening and counseling for intimate partner violence should be a core part of women's preventive health visits. More than one in three women in the United States have experienced rape, physical violence, or stalking by an intimate partnerC4; 14% of noninstitutionalized older adults experienced financial exploitation, neglect, or physical, psychological, or sexual abuse during the past yearC5; women with disabilities are four times more likely to have experienced sexual assault in the past year than women without disabilities.C6 Physicians should screen all women for intimate partner violence at periodic intervalsC7; computer-based screening may be preferred by some patients.C8 | Sample questions:
|
USPSTF = U.S. Preventive Services Task Force.
*—The CAGE questionnaire is one of several available screening instruments. Incorporating the questions into the general history is recommended rather than using the questionnaire as a stand-alone screening tool. Item responses are scored 0 or 1, with a higher score indicating alcohol problems. A total score of 2 or greater is considered clinically significant.
†—A pattern of assaultive and coercive behavior that may include physical injury, psychological abuse, sexual assault, progressive isolation, stalking, deprivation, intimidation, and reproductive coercion to control an intimate partner. Elder abuse and neglect are forms of intimate partner violence.
Information from:
C1. U.S. Preventive Services Task Force. Alcohol misuse: screening and behavioral counseling interventions in primary care. May 2013. http://www.uspreventiveservicestaskforce.org/Page/Document/UpdateSummaryFinal/alcohol-misuse-screening-and-behavioral-counseling-interventions-in-primary-care?ds=1&s=alcohol. Accessed June 23, 2016.
C2. Ewing JA. Detecting alcoholism. The CAGE questionnaire. JAMA. 1984;252(14):1905–1907.
C3. U.S. Preventive Services Task Force. Depression in adults: screening. January 2016. http://www.uspreventiveservicestaskforce.org/Page/Document/UpdateSummaryFinal/depression-in-adults-screening1?ds=1&s=depression. Accessed June 23, 2016.
C4. Centers for Disease Control and Prevention. National intimate partner and sexual violence survey: 2010 summary report. http://www.cdc.gov/violenceprevention/pdf/nisvs_report2010-a.pdf. Accessed June 20, 2016.
C5. U.S. Government Accountability Office. Elder justice: stronger federal leadership could enhance national response to elder abuse. http://www.gao.gov/products/GAO-11-208. Accessed June 22, 2016.
C6. Martin SL, Ray N, Sotres-Alvarez D, et al. Physical and sexual assault of women with disabilities. Violence Against Women. 2006;12(9):823–837.
C7. ACOG committee opinion no. 518: intimate partner violence. Obstet Gynecol. 2012;119(2 pt 1):412–417.
C8. Ahmad F, Hogg-Johnson S, Stewart DE, Skinner HA, Glazier RH, Levinson W. Computer-assisted screening for intimate partner violence and control: a randomized trial. Ann Intern Med. 2009;151(2):93–102.
Vaccinations
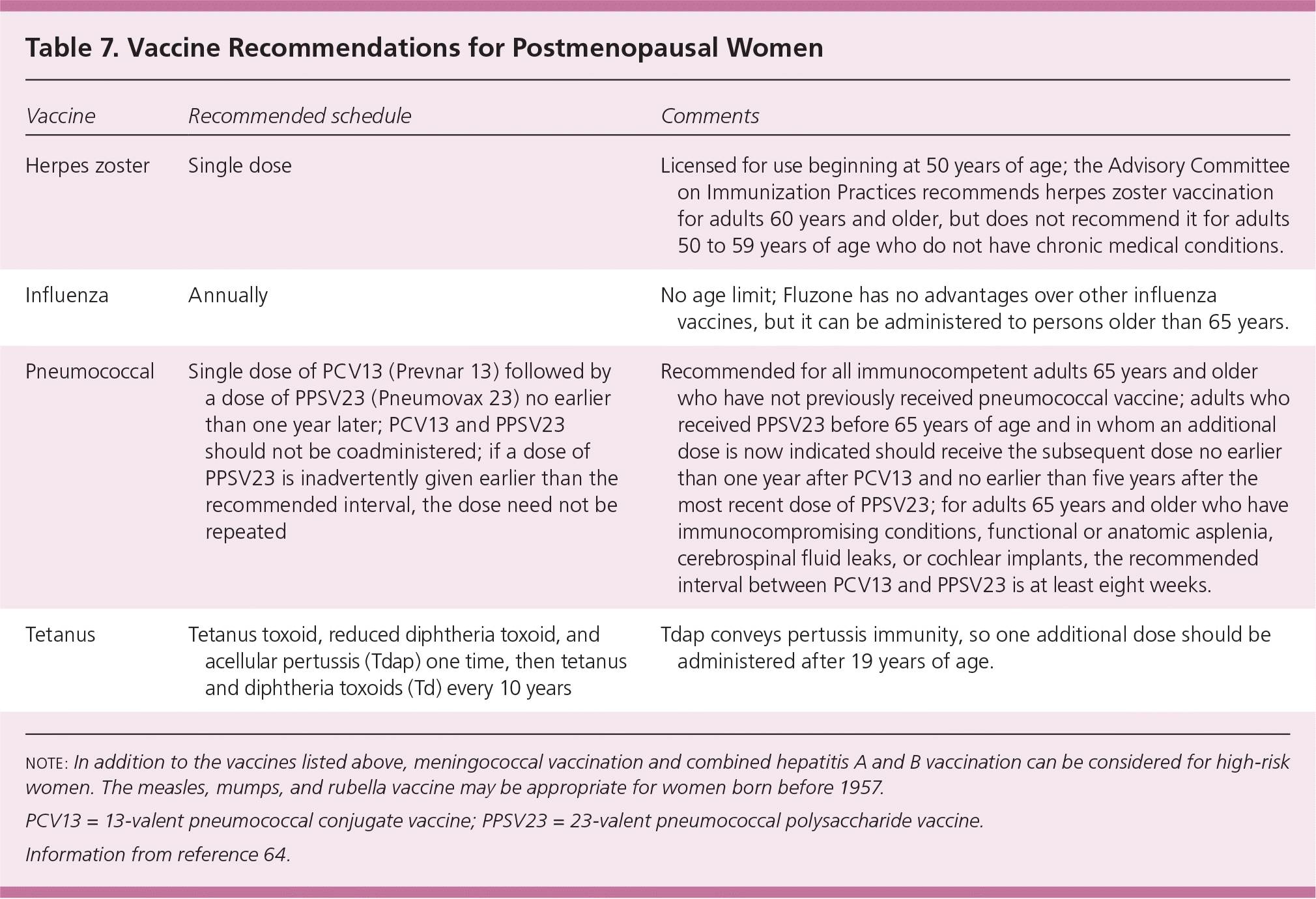
Postmenopausal women benefit from receiving vaccines recommended by the Advisory Committee on Immunization Practices, including those that provide protection against herpes zoster, influenza, pneumococcus, and tetanus, diphtheria, and pertussis (Table 7).64 The current adult immunization schedules are available at http://www.cdc.gov/vaccines/hcp/acip-recs/index.html.
Table 7. Vaccine Recommendations for Postmenopausal Women
| Vaccine | Recommended schedule | Comments |
|---|---|---|
| Herpes zoster | Single dose | Licensed for use beginning at 50 years of age; the Advisory Committee on Immunization Practices recommends herpes zoster vaccination for adults 60 years and older, but does not recommend it for adults 50 to 59 years of age who do not have chronic medical conditions. |
| Influenza | Annually | No age limit; Fluzone has no advantages over other influenza vaccines, but it can be administered to persons older than 65 years. |
| Pneumococcal | Single dose of PCV13 (Prevnar 13) followed by a dose of PPSV23 (Pneumovax 23) no earlier than one year later; PCV13 and PPSV23 should not be coadministered; if a dose of PPSV23 is inadvertently given earlier than the recommended interval, the dose need not be repeated | Recommended for all immunocompetent adults 65 years and older who have not previously received pneumococcal vaccine; adults who received PPSV23 before 65 years of age and in whom an additional dose is now indicated should receive the subsequent dose no earlier than one year after PCV13 and no earlier than five years after the most recent dose of PPSV23; for adults 65 years and older who have immunocompromising conditions, functional or anatomic asplenia, cerebrospinal fluid leaks, or cochlear implants, the recommended interval between PCV13 and PPSV23 is at least eight weeks. |
| Tetanus | Tetanus toxoid, reduced diphtheria toxoid, and acellular pertussis (Tdap) one time, then tetanus and diphtheria toxoids (Td) every 10 years | Tdap conveys pertussis immunity, so one additional dose should be administered after 19 years of age. |
note: In addition to the vaccines listed above, meningococcal vaccination and combined hepatitis A and B vaccination can be considered for high-risk women. The measles, mumps, and rubella vaccine may be appropriate for women born before 1957.
PCV13 = 13-valent pneumococcal conjugate vaccine; PPSV23 = 23-valent pneumococcal polysaccharide vaccine.
Information from reference 64.
This article updates previous articles on this topic by Rao, et al.,65 and by Riley, et al.66
Data Sources: We searched PubMed, Essential Evidence, the Cochrane Library, the Agency for Healthcare Research and Quality, and the Centers for Disease Control and Prevention for articles published since 2008 concerning postmenopausal health maintenance, annual postmenopausal health, and annual gynecologic examination. The topics of cardiovascular disease, breast cancer, cervical cancer, colon cancer, bone health, vaccination, and all other major topics of this article were also searched. Guidelines from professional organizations were consulted. Search dates: November 15, 2015, through January 2017.
The authors thank Shalu Gillum, JD, MLS, AHIP, for assistance with the preparation of the manuscript.

