
Am Fam Physician. 2017;95(9):572-579
A list of top POEMs from previous years is available at https://www.aafp.org/journals/afp/authors/ebm-toolkit/resources/top-poems.html.
Author disclosure: Dr. Ebell is cofounder and editor-in-chief of Essential Evidence Plus, published by Wiley-Blackwell, Inc. Dr. Grad has no relevant financial affiliations.
This article summarizes the top 20 original research studies and four practice guidelines of 2016, based on regular literature surveillance and as selected by members of the Canadian Medical Association. The studies, known as POEMs (patient-oriented evidence that matters), were rated highly because of their relevance, validity, and potential to change practice. Key hypertension treatment findings include reduced mortality (a benefit not demonstrated in lower-risk persons or persons with diabetes mellitus) but also an increase in harms with a more aggressive blood pressure target in high-risk persons with hypertension and without diabetes. Additionally, one study found that cardiovascular events are rare in patients who meet the criteria for hypertensive urgency. Regarding respiratory conditions, the combination of fluticasone and salmeterol is preferred to fluticasone alone in patients with moderate to severe asthma; nasal irrigation but not steam inhalation is beneficial for patients with chronic sinus symptoms; and delayed prescriptions reduce antibiotic use in patients with symptoms of acute respiratory infection. Studies on musculoskeletal topics found that of the nonsteroidal anti-inflammatory drugs currently available, diclofenac is most likely to be effective for hip or knee osteoarthritis; the benefits of opioids in patients with chronic low back pain are limited and not clearly superior to nonsteroidal anti-inflammatory drugs; and hip radiography is not helpful for diagnosing osteoarthritis of the hip. Regarding diabetes and obesity, the Mediterranean diet is more effective than a low-fat diet for weight loss, and aggressive blood pressure targets are not recommended in patients with diabetes, especially older persons. Other recommendations include use of an oral syringe rather than a medicine cup to measure liquid medications for children, and abrupt smoking cessation preceded by two weeks of nicotine replacement via a patch, rather than a slow phasing out of tobacco use. Finally, although azithromycin has a slightly higher failure rate than doxycycline for the treatment of chlamydia, it still cured 97% of patients in a randomized trial.
Each year, thousands of studies are published that are potentially relevant to primary care physicians. To help physicians identify the most important new research, the POEMs (patient-oriented evidence that matters) criteria were developed. According to these criteria, the most important research—defined as research that, if true, has the greatest potential to change practice—should be relevant and valid (i.e., at low risk of bias), and report patient-oriented outcomes such as morbidity, mortality, or quality of life.1 Since 1994, a team of primary care clinicians with expertise in evidence-based practice has performed monthly surveillance of more than 110 English-language research journals.2 Although more than 20,000 studies were published in these journals during 2016, only 264 met the POEMs criteria for validity, relevance, use of patient-oriented outcomes, and practice change. Each POEM is summarized in a structured critical appraisal written by one of the six expert reviewers and peer reviewed by faculty and fellows of the University of Missouri Department of Family Medicine. Writing and disseminating the POEMs are supported by subscriptions, without industry support.
The Canadian Medical Association (CMA) sponsors a subscription to the Daily InfoPOEMs for their members. Each member has the option to receive the daily POEM by e-mail and rate it using a brief survey called the Information Assessment Method. This validated survey is a tool to document clinical relevance, cognitive impact, use of the information in practice, and expected health benefits for patients if the results of the POEM are applied.3 This article presents the 20 POEMs of 2016 that were most highly rated by CMA members for clinical relevance to one or more of their patients.
In the sixth installment of this annual series,4–8 we summarize the clinical question and bottom-line answer for each of the 20 top-rated POEMs. The POEMs have been organized by topic, and each is accompanied by a brief discussion. The bottom-line answers have been rewritten somewhat from the original to better stand alone without the complete synopsis. We also briefly discuss four POEMs that summarize highly relevant practice guidelines.
Hypertension
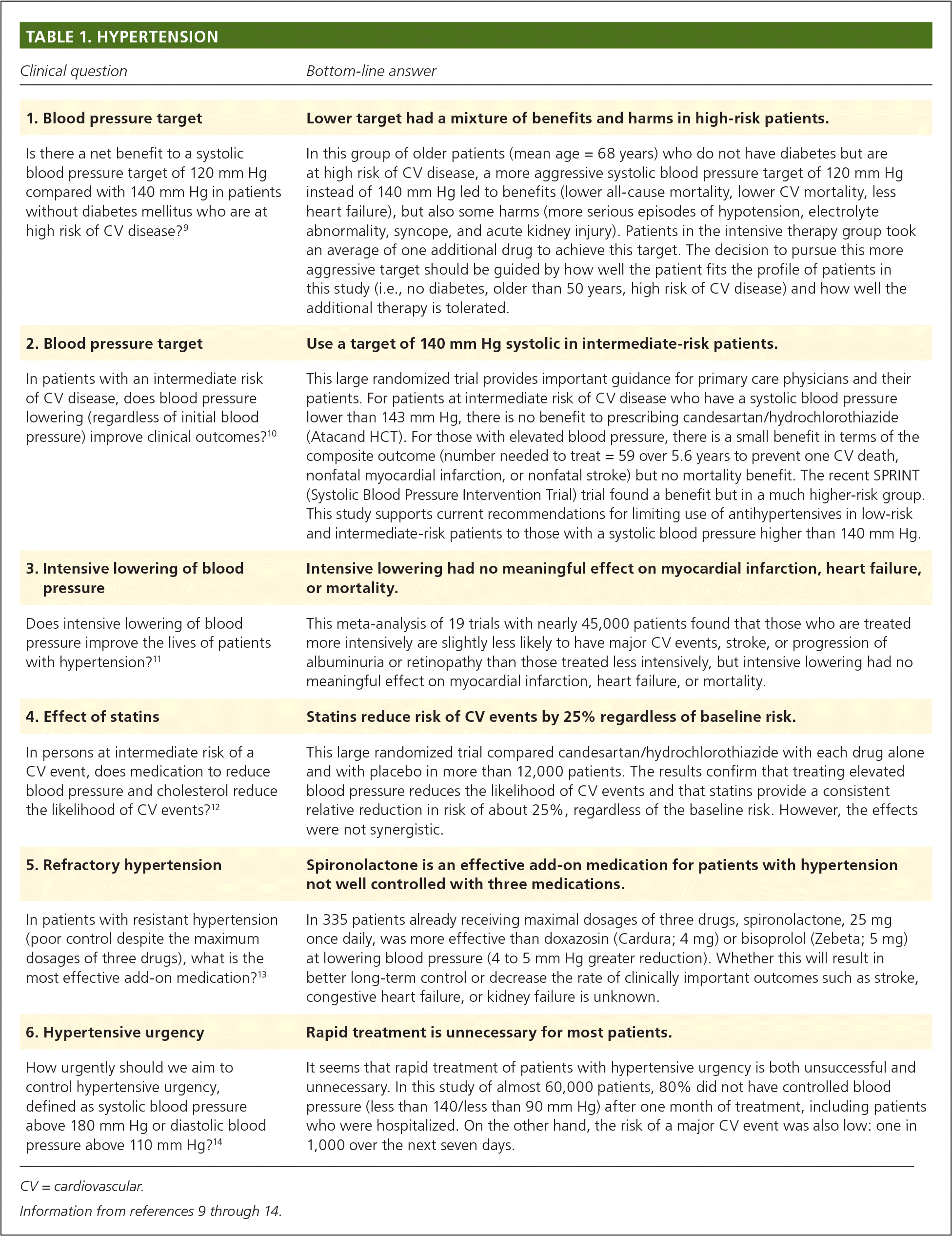
The first group of POEMs focuses on hypertension (Table 1).9–14 Study 1, the SPRINT (Systolic Blood Pressure Intervention Trial) study, reported a reduction in all-cause and cardiovascular (CV) mortality in older high-risk patients without diabetes mellitus who were randomized to a more intensive systolic blood pressure target of 120 mm Hg.9 The number needed to treat (NNT) for 3.3 years was 83 to prevent one death, but this is balanced by more harms: hypotension (number needed to harm [NNH] = 100), syncope (NNH = 200), electrolyte abnormality (NNH = 125), and acute kidney injury (NNH = 59). There was no effect on rates of myocardial infarction or stroke.
| Clinical question | Bottom-line answer |
|---|---|
| 1. Blood pressure target | Lower target had a mixture of benefits and harms in high-risk patients. |
| Is there a net benefit to a systolic blood pressure target of 120 mm Hg compared with 140 mm Hg in patients without diabetes mellitus who are at high risk of CV disease?9 | In this group of older patients (mean age = 68 years) who do not have diabetes but are at high risk of CV disease, a more aggressive systolic blood pressure target of 120 mm Hg instead of 140 mm Hg led to benefits (lower all-cause mortality, lower CV mortality, less heart failure), but also some harms (more serious episodes of hypotension, electrolyte abnormality, syncope, and acute kidney injury). Patients in the intensive therapy group took an average of one additional drug to achieve this target. The decision to pursue this more aggressive target should be guided by how well the patient fits the profile of patients in this study (i.e., no diabetes, older than 50 years, high risk of CV disease) and how well the additional therapy is tolerated. |
| 2. Blood pressure target | Use a target of 140 mm Hg systolic in intermediate-risk patients. |
| In patients with an intermediate risk of CV disease, does blood pressure lowering (regardless of initial blood pressure) improve clinical outcomes?10 | This large randomized trial provides important guidance for primary care physicians and their patients. For patients at intermediate risk of CV disease who have a systolic blood pressure lower than 143 mm Hg, there is no benefit to prescribing candesartan/hydrochlorothiazide (Atacand HCT). For those with elevated blood pressure, there is a small benefit in terms of the composite outcome (number needed to treat = 59 over 5.6 years to prevent one CV death, nonfatal myocardial infarction, or nonfatal stroke) but no mortality benefit. The recent SPRINT (Systolic Blood Pressure Intervention Trial) trial found a benefit but in a much higher-risk group. This study supports current recommendations for limiting use of antihypertensives in low-risk and intermediate-risk patients to those with a systolic blood pressure higher than 140 mm Hg. |
| 3. Intensive lowering of blood pressure | Intensive lowering had no meaningful effect on myocardial infarction, heart failure, or mortality. |
| Does intensive lowering of blood pressure improve the lives of patients with hypertension?11 | This meta-analysis of 19 trials with nearly 45,000 patients found that those who are treated more intensively are slightly less likely to have major CV events, stroke, or progression of albuminuria or retinopathy than those treated less intensively, but intensive lowering had no meaningful effect on myocardial infarction, heart failure, or mortality. |
| 4. Effect of statins | Statins reduce risk of CV events by 25% regardless of baseline risk. |
| In persons at intermediate risk of a CV event, does medication to reduce blood pressure and cholesterol reduce the likelihood of CV events?12 | This large randomized trial compared candesartan/hydrochlorothiazide with each drug alone and with placebo in more than 12,000 patients. The results confirm that treating elevated blood pressure reduces the likelihood of CV events and that statins provide a consistent relative reduction in risk of about 25%, regardless of the baseline risk. However, the effects were not synergistic. |
| 5. Refractory hypertension | Spironolactone is an effective add-on medication for patients with hypertension not well controlled with three medications. |
| In patients with resistant hypertension (poor control despite the maximum dosages of three drugs), what is the most effective add-on medication?13 | In 335 patients already receiving maximal dosages of three drugs, spironolactone, 25 mg once daily, was more effective than doxazosin (Cardura; 4 mg) or bisoprolol (Zebeta; 5 mg) at lowering blood pressure (4 to 5 mm Hg greater reduction). Whether this will result in better long-term control or decrease the rate of clinically important outcomes such as stroke, congestive heart failure, or kidney failure is unknown. |
| 6. Hypertensive urgency | Rapid treatment is unnecessary for most patients. |
| How urgently should we aim to control hypertensive urgency, defined as systolic blood pressure above 180 mm Hg or diastolic blood pressure above 110 mm Hg?14 | It seems that rapid treatment of patients with hypertensive urgency is both unsuccessful and unnecessary. In this study of almost 60,000 patients, 80% did not have controlled blood pressure (less than 140/less than 90 mm Hg) after one month of treatment, including patients who were hospitalized. On the other hand, the risk of a major CV event was also low: one in 1,000 over the next seven days. |
Study 2 found no benefit to blood pressure lowering in patients at intermediate CV risk who already had a systolic blood pressure less than 143 mm Hg.10 This trial included some patients with diabetes or impaired glucose tolerance, but overall, the patients were at lower risk than persons in the SPRINT trial (CV event rate = 0.8% vs. 2.1%). Thus, the decision to pursue a more aggressive blood pressure target should involve the patient and should be limited to patients without diabetes who are at high risk of a CV event. Study 3, a systematic review, also addresses more aggressive blood pressure control.11 Although the authors found very small reductions in CV events, many of the studies were of poor quality or did not achieve a large difference in systolic blood pressure between groups. This is an area that needs further study, and, for now, we should remain cautious about extending tight control to all patients with hypertension.
Study 4 highlights the need to consider a patient's baseline CV risk when making decisions about statin therapy.12 Statin use at the dosage given in this study reduces the likelihood of a CV event by approximately 25%. So, if the starting point is a 10-year CV event risk of 20%, statin use would reduce the risk to 15%, for an NNT of 20. If the 10-year risk is 10%, as in this study, it reduces the likelihood to 7.5%, for an NNT of 40. If the 10-year risk is only 5%, it reduces the likelihood to 3.75%, for an NNT of 80. These numbers should inform discussions with patients about their preferences for statin therapy. Study 5 compared three drugs in patients with poorly controlled hypertension who were already receiving maximal dosages of three antihypertensives.13 Spironolactone was the most effective at lowering blood pressure. Although blood pressure reduction is not a patient-oriented outcome, the study was not powered or of adequate duration to evaluate CV events or mortality. Finally, Study 6 makes us reconsider the name of the condition now known as hypertensive urgency, because CV events were rare during the week after patients presented with a blood pressure greater than 180/110 mm Hg.14 Although it is important to work with these patients to improve blood pressure control and address medication adherence (a common cause of this problem), it is rarely life threatening.
Respiratory Conditions
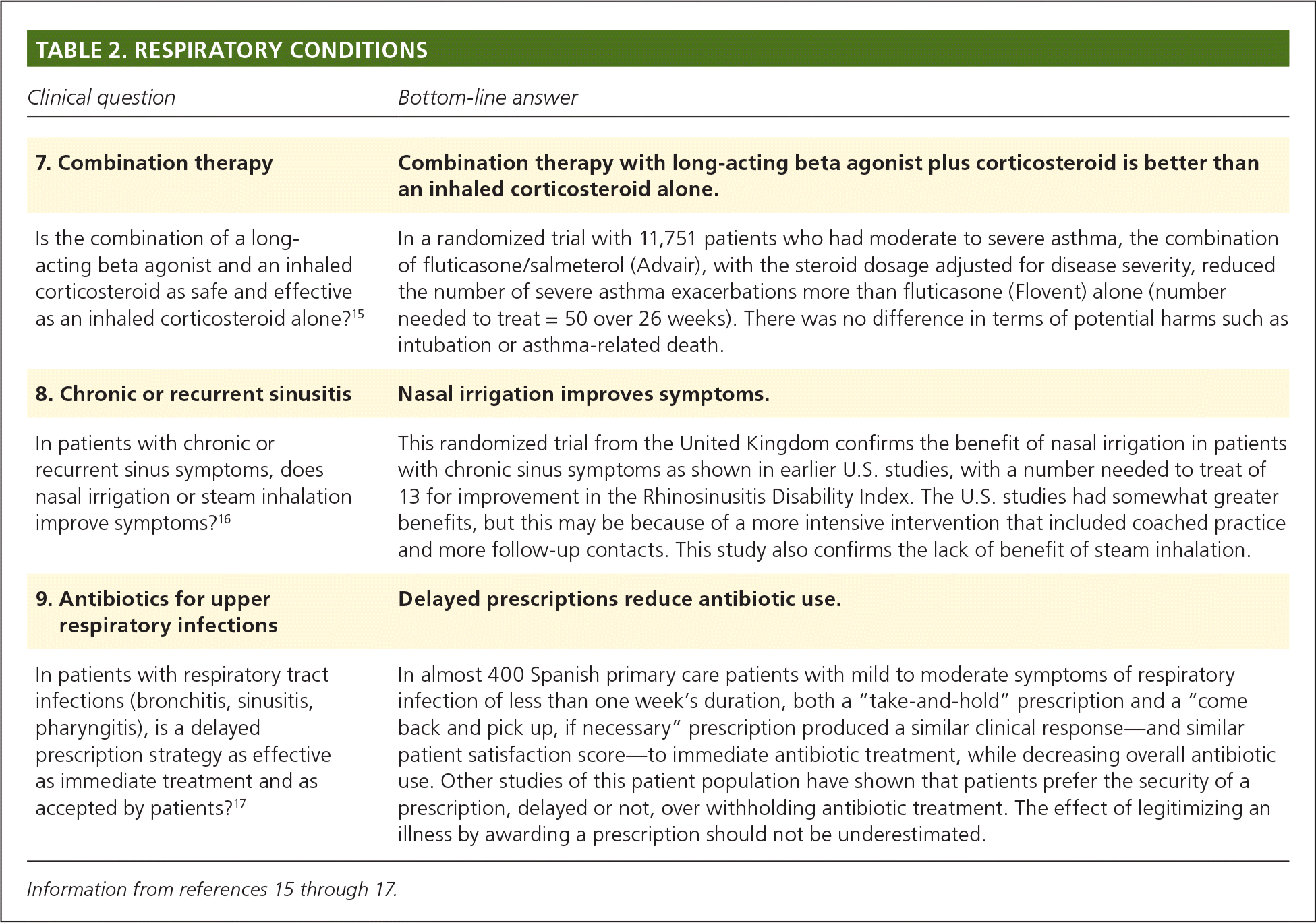
Three of the selected POEMs address respiratory conditions (Table 2).15–17 In Study 7, patients 12 years and older with moderate to severe asthma were randomized to receive twice-daily inhaled fluticasone (Flovent) alone, with a dose stratified by disease severity, or combination fluticasone/salmeterol (Advair; stratified dose/50 mcg).15 For every 50 patients who received fluticasone/salmeterol, there was one fewer severe exacerbation over a six-month study period. However, there was no difference in hospitalizations.
| Clinical question | Bottom-line answer |
|---|---|
| 7. Combination therapy | Combination therapy with long-acting beta agonist plus corticosteroid is better than an inhaled corticosteroid alone. |
| Is the combination of a long-acting beta agonist and an inhaled corticosteroid as safe and effective as an inhaled corticosteroid alone?15 | In a randomized trial with 11,751 patients who had moderate to severe asthma, the combination of fluticasone/salmeterol (Advair), with the steroid dosage adjusted for disease severity, reduced the number of severe asthma exacerbations more than fluticasone (Flovent) alone (number needed to treat = 50 over 26 weeks). There was no difference in terms of potential harms such as intubation or asthma-related death. |
| 8. Chronic or recurrent sinusitis | Nasal irrigation improves symptoms. |
| In patients with chronic or recurrent sinus symptoms, does nasal irrigation or steam inhalation improve symptoms?16 | This randomized trial from the United Kingdom confirms the benefit of nasal irrigation in patients with chronic sinus symptoms as shown in earlier U.S. studies, with a number needed to treat of 13 for improvement in the Rhinosinusitis Disability Index. The U.S. studies had somewhat greater benefits, but this may be because of a more intensive intervention that included coached practice and more follow-up contacts. This study also confirms the lack of benefit of steam inhalation. |
| 9. Antibiotics for upper respiratory infections | Delayed prescriptions reduce antibiotic use. |
| In patients with respiratory tract infections (bronchitis, sinusitis, pharyngitis), is a delayed prescription strategy as effective as immediate treatment and as accepted by patients?17 | In almost 400 Spanish primary care patients with mild to moderate symptoms of respiratory infection of less than one week's duration, both a “take-and-hold” prescription and a “come back and pick up, if necessary” prescription produced a similar clinical response—and similar patient satisfaction score—to immediate antibiotic treatment, while decreasing overall antibiotic use. Other studies of this patient population have shown that patients prefer the security of a prescription, delayed or not, over withholding antibiotic treatment. The effect of legitimizing an illness by awarding a prescription should not be underestimated. |
The next two POEMs focused on the treatment of respiratory tract infections. In Study 8, primary care patients with chronic or recurrent nasal symptoms were randomized to receive a recommendation to perform daily nasal saline irrigation or a recommendation to perform daily steam inhalation. Only the nasal saline irrigation was effective.16 This is consistent with studies of patients with chronic rhinosinusitis in the United States. Finally, Study 9 is a Spanish primary care study in which the physicians had reasonable doubt as to whether to treat a patient with an antibiotic. Patients were randomized to an immediate antibiotic, no antibiotic, or one of two delayed antibiotic strategies.17 Although the patients who did not get an antibiotic had a longer duration of symptoms, there was little difference between the delayed prescribing strategies and the immediate antibiotic group. The delayed strategies were associated with fewer days off work and similar patient satisfaction.
Musculoskeletal Conditions
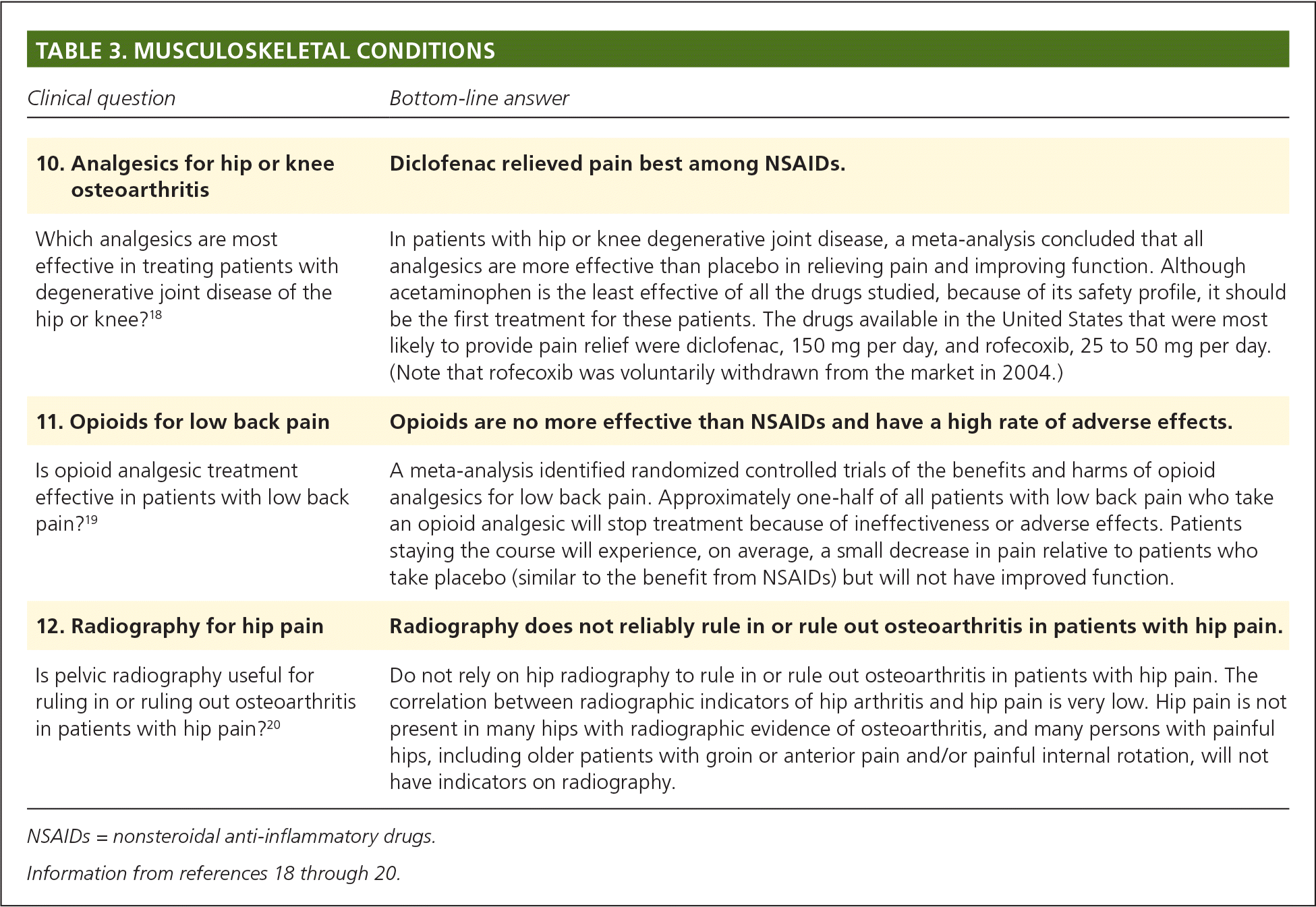
Several POEMs address care of patients with hip, knee, or back pain (Table 3).18–20 Study 10 was a meta-analysis of 74 trials with 59,000 patients comparing seven different drugs for osteoarthritis of the hips or knees.18 Although all medications were effective, including acetaminophen, the most likely to provide meaningful pain relief were diclofenac and rofecoxib (which is no longer available). However, these drugs have greater potential for harm than acetaminophen. Study 11 examined the value of opioid analgesics in patients with low back pain.19 This was a meta-analysis of 20 studies with 7,295 patients, mostly with chronic low back pain. The researchers found that the benefits of opioids were modest and that many patients discontinue treatment because of adverse effects or lack of effectiveness. Patients who dropped out were considered nonresponders, which may not be accurate as they may have dropped out because of adverse effects, despite effective pain reduction. The final musculoskeletal pain POEM, Study 12, used data from two observational studies to determine the value of radiography for the diagnosis of hip pain.20 Only 21% of patients who met the criteria for hip osteoarthritis on radiography had frequent hip pain, whereas only 16% of patients with frequent hip pain had radiographic evidence of hip osteoarthritis. Using radiography alone to guide treatment decisions about suspected hip osteoarthritis is therefore unreliable.
| Clinical question | Bottom-line answer |
|---|---|
| 10. Analgesics for hip or knee osteoarthritis | Diclofenac relieved pain best among NSAIDs. |
| Which analgesics are most effective in treating patients with degenerative joint disease of the hip or knee?18 | In patients with hip or knee degenerative joint disease, a meta-analysis concluded that all analgesics are more effective than placebo in relieving pain and improving function. Although acetaminophen is the least effective of all the drugs studied, because of its safety profile, it should be the first treatment for these patients. The drugs available in the United States that were most likely to provide pain relief were diclofenac, 150 mg per day, and rofecoxib, 25 to 50 mg per day. (Note that rofecoxib was voluntarily withdrawn from the market in 2004.) |
| 11. Opioids for low back pain | Opioids are no more effective than NSAIDs and have a high rate of adverse effects. |
| Is opioid analgesic treatment effective in patients with low back pain?19 | A meta-analysis identified randomized controlled trials of the benefits and harms of opioid analgesics for low back pain. Approximately one-half of all patients with low back pain who take an opioid analgesic will stop treatment because of ineffectiveness or adverse effects. Patients staying the course will experience, on average, a small decrease in pain relative to patients who take placebo (similar to the benefit from NSAIDs) but will not have improved function. |
| 12. Radiography for hip pain | Radiography does not reliably rule in or rule out osteoarthritis in patients with hip pain. |
| Is pelvic radiography useful for ruling in or ruling out osteoarthritis in patients with hip pain?20 | Do not rely on hip radiography to rule in or rule out osteoarthritis in patients with hip pain. The correlation between radiographic indicators of hip arthritis and hip pain is very low. Hip pain is not present in many hips with radiographic evidence of osteoarthritis, and many persons with painful hips, including older patients with groin or anterior pain and/or painful internal rotation, will not have indicators on radiography. |
Diabetes Mellitus and Obesity
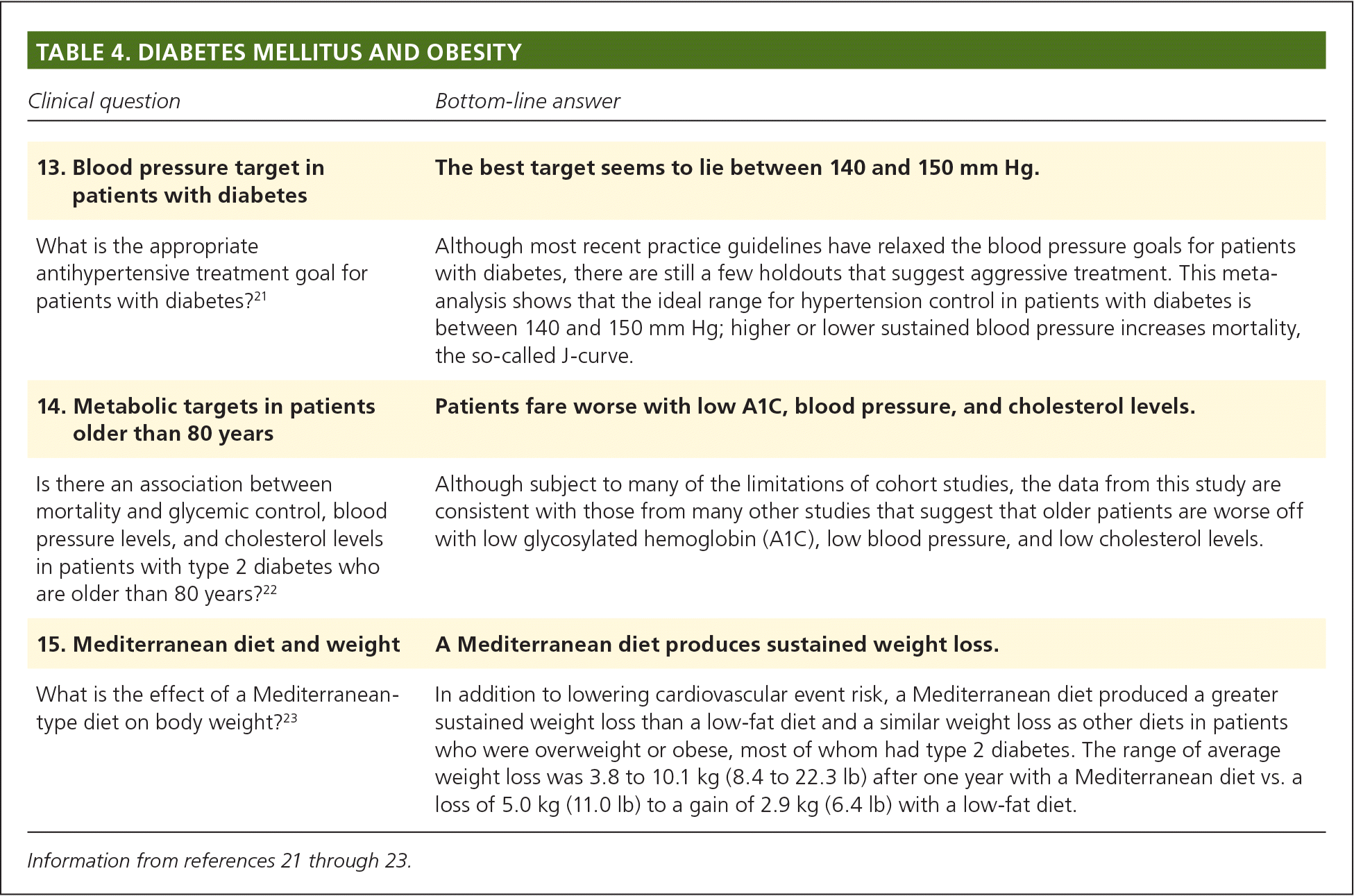
In Study 13, the first of three selected POEMs related to the treatment of diabetes and obesity (Table 421–23 ), a meta-analysis of 49 studies with 73,738 participants found that there was no benefit to giving antihypertensives to patients with a baseline blood pressure less than 140 mm Hg.21 There was some benefit to treating blood pressures greater than 140 mm Hg, with decreases in all-cause mortality, end stage renal disease, and CV mortality and events.
| Clinical question | Bottom-line answer |
|---|---|
| 13. Blood pressure target in patients with diabetes | The best target seems to lie between 140 and 150 mm Hg. |
| What is the appropriate antihypertensive treatment goal for patients with diabetes?21 | Although most recent practice guidelines have relaxed the blood pressure goals for patients with diabetes, there are still a few holdouts that suggest aggressive treatment. This meta-analysis shows that the ideal range for hypertension control in patients with diabetes is between 140 and 150 mm Hg; higher or lower sustained blood pressure increases mortality, the so-called J-curve. |
| 14. Metabolic targets in patients older than 80 years | Patients fare worse with low A1C, blood pressure, and cholesterol levels. |
| Is there an association between mortality and glycemic control, blood pressure levels, and cholesterol levels in patients with type 2 diabetes who are older than 80 years?22 | Although subject to many of the limitations of cohort studies, the data from this study are consistent with those from many other studies that suggest that older patients are worse off with low glycosylated hemoglobin (A1C), low blood pressure, and low cholesterol levels. |
| 15. Mediterranean diet and weight | A Mediterranean diet produces sustained weight loss. |
| What is the effect of a Mediterranean-type diet on body weight?23 | In addition to lowering cardiovascular event risk, a Mediterranean diet produced a greater sustained weight loss than a low-fat diet and a similar weight loss as other diets in patients who were overweight or obese, most of whom had type 2 diabetes. The range of average weight loss was 3.8 to 10.1 kg (8.4 to 22.3 lb) after one year with a Mediterranean diet vs. a loss of 5.0 kg (11.0 lb) to a gain of 2.9 kg (6.4 lb) with a low-fat diet. |
An important challenge of caring for patients with type 2 diabetes is balancing the benefits and harms of treatment. Study 14 used data from a registry of 26,000 patients in the United Kingdom who had diabetes and were older than 80 years.22 They found that the association between mortality and glycemic control was U-shaped, with the best outcomes for patients with an A1C level between 7.0% and 7.5%, and a blood pressure between 150/90 and 155/95 mm Hg. This is consistent with randomized trials showing no benefit or harm with aggressive targets for blood pressure control. Finally, Study 15, a meta-analysis of five studies with 998 patients, most of whom had type 2 diabetes, found that a Mediterranean diet was associated with an average weight loss of 3.8 to 10.1 kg (8.4 to 22.3 lb).23 This compares with a loss of 5.0 kg (11.0 lb) to a gain of 2.9 kg (6.4 lb) in studies of a low-fat diet. Other studies have shown that a Mediterranean diet, which includes olive oil, fish, vegetables, and nuts, is associated with fewer CV events.
Miscellaneous
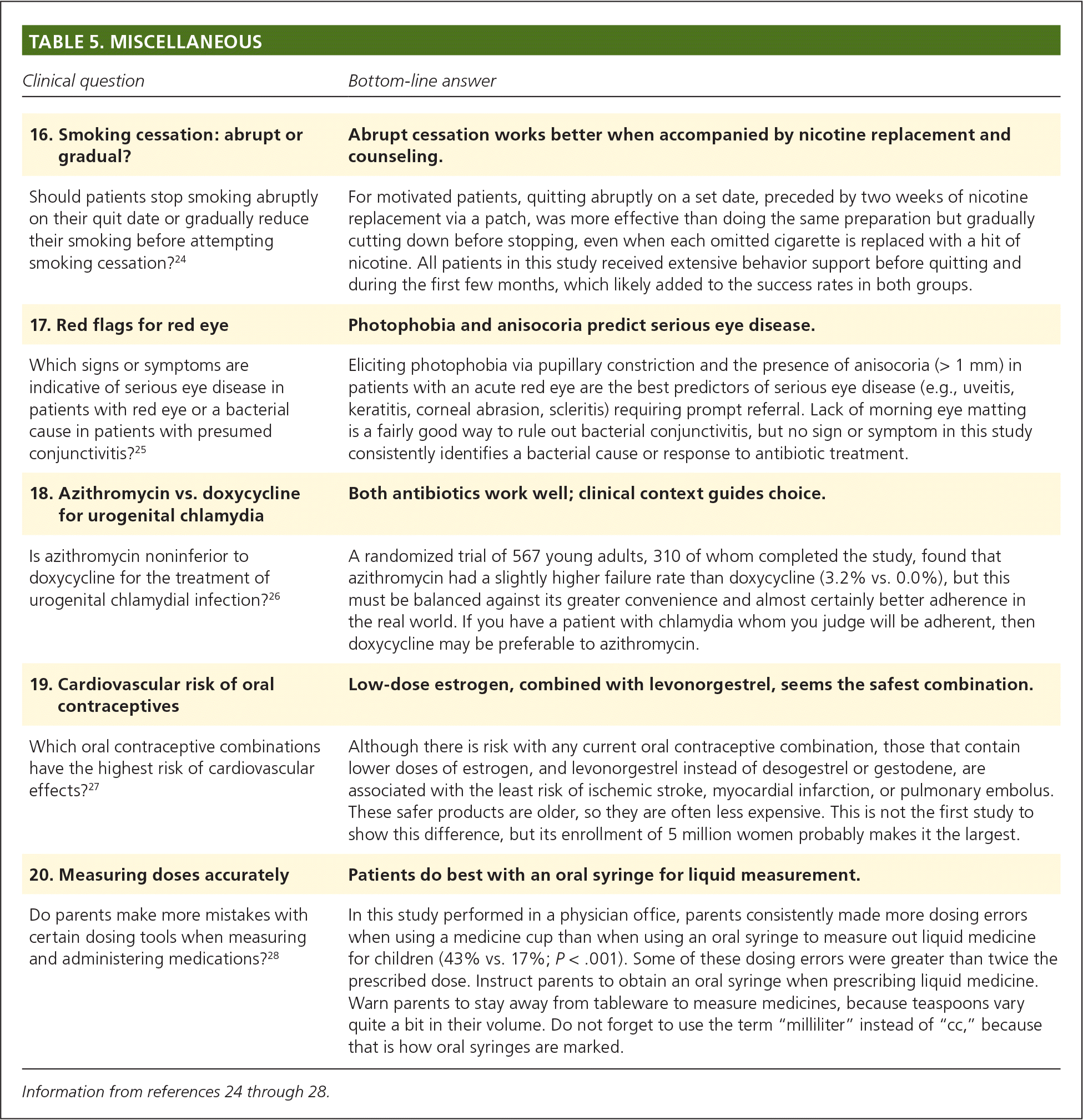
The remaining five POEMs do not fit neatly into a single category but provide useful guidance for family physicians (Table 5).24–28 Study 16 randomized patients who wanted to quit smoking to a gradual reduction in tobacco use or an abrupt quit date. Going cold turkey, preceded by two weeks of nicotine replacement patch use, was more effective, even in patients who expressed a preference for a go-slow approach.24
| Clinical question | Bottom-line answer |
|---|---|
| 16. Smoking cessation: abrupt or gradual? | Abrupt cessation works better when accompanied by nicotine replacement and counseling. |
| Should patients stop smoking abruptly on their quit date or gradually reduce their smoking before attempting smoking cessation?24 | For motivated patients, quitting abruptly on a set date, preceded by two weeks of nicotine replacement via a patch, was more effective than doing the same preparation but gradually cutting down before stopping, even when each omitted cigarette is replaced with a hit of nicotine. All patients in this study received extensive behavior support before quitting and during the first few months, which likely added to the success rates in both groups. |
| 17. Red flags for red eye | Photophobia and anisocoria predict serious eye disease. |
| Which signs or symptoms are indicative of serious eye disease in patients with red eye or a bacterial cause in patients with presumed conjunctivitis?25 | Eliciting photophobia via pupillary constriction and the presence of anisocoria (> 1 mm) in patients with an acute red eye are the best predictors of serious eye disease (e.g., uveitis, keratitis, corneal abrasion, scleritis) requiring prompt referral. Lack of morning eye matting is a fairly good way to rule out bacterial conjunctivitis, but no sign or symptom in this study consistently identifies a bacterial cause or response to antibiotic treatment. |
| 18. Azithromycin vs. doxycycline for urogenital chlamydia | Both antibiotics work well; clinical context guides choice. |
| Is azithromycin noninferior to doxycycline for the treatment of urogenital chlamydial infection?26 | A randomized trial of 567 young adults, 310 of whom completed the study, found that azithromycin had a slightly higher failure rate than doxycycline (3.2% vs. 0.0%), but this must be balanced against its greater convenience and almost certainly better adherence in the real world. If you have a patient with chlamydia whom you judge will be adherent, then doxycycline may be preferable to azithromycin. |
| 19. Cardiovascular risk of oral contraceptives | Low-dose estrogen, combined with levonorgestrel, seems the safest combination. |
| Which oral contraceptive combinations have the highest risk of cardiovascular effects?27 | Although there is risk with any current oral contraceptive combination, those that contain lower doses of estrogen, and levonorgestrel instead of desogestrel or gestodene, are associated with the least risk of ischemic stroke, myocardial infarction, or pulmonary embolus. These safer products are older, so they are often less expensive. This is not the first study to show this difference, but its enrollment of 5 million women probably makes it the largest. |
| 20. Measuring doses accurately | Patients do best with an oral syringe for liquid measurement. |
| Do parents make more mistakes with certain dosing tools when measuring and administering medications?28 | In this study performed in a physician office, parents consistently made more dosing errors when using a medicine cup than when using an oral syringe to measure out liquid medicine for children (43% vs. 17%; P < .001). Some of these dosing errors were greater than twice the prescribed dose. Instruct parents to obtain an oral syringe when prescribing liquid medicine. Warn parents to stay away from tableware to measure medicines, because teaspoons vary quite a bit in their volume. Do not forget to use the term “milliliter” instead of “cc,” because that is how oral syringes are marked. |
Primary care physicians commonly evaluate patients with eye symptoms. In Study 17, a systematic review of diagnostic studies concluded that photophobia via pupillary constriction and the presence of anisocoria are the best predictors of serious eye disease, such as uveitis, keratitis, or scleritis, whereas the absence of sticky matting in the morning helps rule out bacterial conjunctivitis.25
Options for the treatment of genital chlamydial infection include a single dose of azithromycin, 1 g, or doxycycline, 100 mg twice daily for seven days. Study 18, a randomized trial, found a slightly higher failure rate with azithromycin: five out of 155 (3.2%) patients vs. none in the doxycycline group.26 However, because the study took place in a youth correctional facility, 45% of study participants were released before the final evaluation of cure. Additionally, adherence to the study medication could be assured because of the nature of the setting; therefore, despite the slightly higher failure rate, if adherence is a concern, azithromycin may be the better option.
Study 19 used data from a large French patient registry with more than 5 million woman-years of contraceptive use to determine the risk of CV events.27 Overall, the risk was very low (six events per 10,000 woman-years), and it was lowest in women taking a lower-dose estrogen (20 mcg) and with levonorgestrel as the progestogen component.
Finally, Study 20 asked parents to read a prescription label and then use an oral syringe or a medicine cup to dose the liquid medication.28 Approximately 84% of parents made at least one error in their three dosing attempts. Using a syringe was far more accurate and should be recommended to parents of young patients.
Practice Guidelines
In addition to the top 20 original research studies, members of the CMA identified four guideline reports among the highest-rated POEMs. Two guidelines from the U.S. Preventive Services Task Force were highly rated. The first is an updated recommendation on colorectal cancer screening. A key message is that all approaches are effective, adding 225 to 245 life-years per 1,000 patients screened. The primary difference between strategies, as shown in a series of useful figures in the guideline, was the number of lifetime colonoscopies required, which was greatest with colonoscopy and the fecal immunochemical DNA test.29 The cost is highest for those strategies as well. Fecal immunochemical testing is the preferred stool test and is being compared with colonoscopy in several ongoing randomized trials. [Two editorials discussing colorectal cancer screening methods are available at https://www.aafp.org/afp/2017/0515/p616.html and https://www.aafp.org/afp/2017/0515/p618.html.] The second guideline serves as a reminder to ask all adults about tobacco use, advise them to stop, and offer help in terms of nicotine replacement or other pharmacotherapy to enhance their likelihood of success.30 The evidence was insufficient to make any recommendations on the use of e-cigarettes to reduce the use of traditional cigarettes.
The American College of Physicians released an evidence-based guideline on the treatment of chronic insomnia.31 The preferred initial treatment is cognitive behavior therapy focused on stimulus control, sleep restriction, sleep hygiene, and relaxation techniques. Drug therapy is somewhat effective, but there are no long-term studies, and these medications all have the potential for adverse effects. Some drugs in fairly widespread use, like diphenhydramine and trazodone, have not been studied for the treatment of chronic insomnia.
Finally, the Centers for Disease Control and Prevention (CDC) released a guideline for prescribing opioids in patients with chronic pain.32 Based largely on low-quality evidence and short-term studies, the CDC recommends using nonpharmacologic therapies first, establishing realistic goals, discussing risks and benefits with patients before initiation, using the lowest effective dose, and providing close follow-up. Referral to a pain management subspecialist is recommended when the dose exceeds 50 to 90 morphine milligram equivalents per day.
editor's note: This article was cowritten by Dr. Mark Ebell, who was a member of the U.S. Preventive Services Task Force (USPSTF) from 2012 to 2015 and currently serves as a consultant to the USPSTF. This article does not necessarily represent the views and policies of the USPSTF. Dr. Ebell is deputy editor for American Family Physician (AFP) and cofounder and editor-in-chief of Essential Evidence Plus, published by Wiley-Blackwell, Inc. The POEMs described in this article stem from work that Dr. Ebell and his colleagues have been doing for the past two decades. Medical journals occasionally publish an article summarizing the best studies in a certain field from the previous year; however, those articles are limited by being one person's idiosyncratic collection of a handful of studies. In contrast, this article by Drs. Ebell and Roland Grad is validated in two ways: (1) the source material (POEMs) was derived from a systematic review of thousands of articles using a rigorous criterion-based process, and (2) these “best of the best” summaries were rated by thousands of Canadian primary care physicians for relevance and benefits to practice.
Because of Dr. Ebell's dual roles and ties to Essential Evidence Plus, the concept for this article was independently reviewed and approved by a group of AFP's medical editors. In addition, the article underwent peer review and editing by three of AFP's medical editors. Dr. Ebell was not involved in the editorial decision-making process.—Jay Siwek, MD, Editor, American Family Physician
The authors thank Wiley-Blackwell, Inc., for giving permission to excerpt the POEMs; Drs. Allen Shaughnessy, Henry Barry, David Slawson, Nita Kulkarni, and Linda Speer for their work in selecting and writing the original POEMs; the academic family medicine fellows and faculty of the University of Missouri–Columbia, for their work as peer reviewers; Pierre Pluye, PhD, for his work in codeveloping the Information Assessment Method; and Maria Vlasak for her assistance with copyediting the POEMs for the past 23 years.
