Clinical Question
What is the most accurate way to estimate cardiovascular risk?
Evidence Summary
The primary prevention of cardiovascular disease (CVD) depends on accurate estimation of cardiovascular risk. However, a recent systematic review identified 363 prediction models.1
Although the Framingham risk score has long been recommended, the diversification of the U.S. population has led clinicians and researchers to express concern that the score, which is based on a predominantly white, middle-class Massachusetts population, may no longer be representative of the U.S. population in general. Additionally, the Framingham risk score is designed to estimate coronary heart disease alone and does not predict other significant atherosclerotic outcomes, such as stroke.2
The 2013 American College of Cardiology/American Heart Association (ACC/AHA) Pooled Cohort Risk (PCR) equations (http://my.americanheart.org/cvriskcalculator) were developed from five large cohorts: the Framingham Heart Study, Framingham Offspring Study, Atherosclerosis Risk in Communities Study, Cardiovascular Health Study, and Coronary Artery Risk Development in Young Adults Study.3 The PCR equations are based on hard atherosclerotic events (defined as nonfatal myocardial infarction, coronary heart disease death, or stroke) and are the only risk assessment tool that was developed using a significant percentage of black patients.
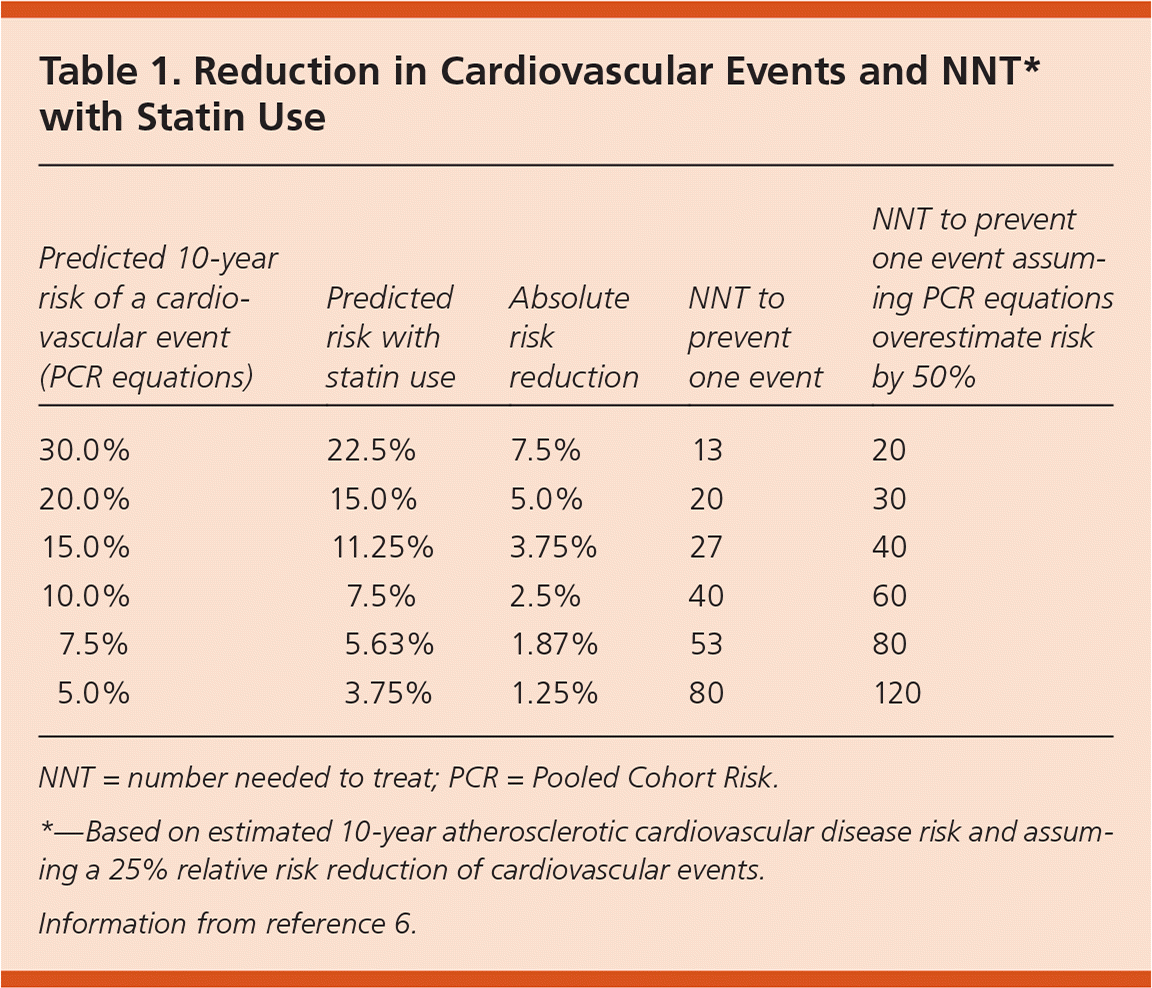
The associated ACC/AHA practice guideline recommends initiation of statin therapy for primary prevention of CVD in patients with a predicted 10-year risk of 7.5% or more, and consideration of statin therapy in patients with a predicted 10-year risk between 5% and 7.5%.4 Of note, the Veterans Affairs and U.S. Department of Defense dyslipidemia treatment guideline recommends a similar approach, but it uses thresholds of 12% and 6% for initiation and consideration of statin therapy, respectively.5 Assuming that statins reduce the risk of an event by approximately 25%, the absolute risk reduction and number needed to treat to prevent one event are shown in Table 1.6
Table 1. Reduction in Cardiovascular Events and NNT* with Statin Use
| Predicted 10-year risk of a cardiovascular event (PCR equations) | Predicted risk with statin use | Absolute risk reduction | NNT to prevent one event | NNT to prevent one event assuming PCR equations overestimate risk by 50% |
|---|---|---|---|---|
| 30.0% | 22.5% | 7.5% | 13 | 20 |
| 20.0% | 15.0% | 5.0% | 20 | 30 |
| 15.0% | 11.25% | 3.75% | 27 | 40 |
| 10.0% | 7.5% | 2.5% | 40 | 60 |
| 7.5% | 5.63% | 1.87% | 53 | 80 |
| 5.0% | 3.75% | 1.25% | 80 | 120 |
NNT = number needed to treat; PCR = Pooled Cohort Risk.
*—Based on estimated 10-year atherosclerotic cardiovascular disease risk and assuming a 25% relative risk reduction of cardiovascular events.
Information from reference 6.
One concern about the new ACC/AHA guideline is that it greatly increases the percentage of patients for whom statins are indicated compared with previous guidelines. One validation study used data from the National Health and Nutrition Examination Survey (NHANES) to compare the number of persons for whom statin therapy would be recommended based on the ACC/AHA PCR equations vs. the guideline from the National Cholesterol Education Program's Third Adult Treatment Panel. When extrapolated to a population of 115.4 million adults in the United States between 40 and 75 years of age, nearly 50% of patients would be candidates for statin therapy based on the new guideline. Among adults 60 to 75 years of age, the percentage of those eligible for statin therapy would increase from 30% to 87% in men and from 21% to 54% in women.7
Predicted 10-year CVD risk using the PCR equations was compared with observed event rates in three large-scale primary prevention cohorts: the Women's Health Study, Physicians' Health Study, and Women's Health Initiative Observational Study. In each cohort, the ACC/AHA risk prediction algorithm overestimated observed risk by 75% to 150%. A similar overestimation of CVD risk, although not of the same magnitude, was seen in two other external validation cohorts.8 Another study followed a large insured population of adults 40 to 75 years of age without diabetes mellitus. The PCR equations again substantially overestimated actual five-year risk of CVD in both sexes, across multiple socioeconomic strata, and in multiple racial/ethnic subgroups. In the group with a predicted five-year CVD risk of 5% or more, the observed risk was 1.85.9
A recent analysis using NHANES data compared observed all-cause and CVD mortality, as reported in the National Center for Health Statistics National Death index, with predicted CVD risk using PCR equations. In patients without CVD at baseline, CVD risk estimated by PCR equations was significantly associated with all-cause and CVD-specific mortality. However, a direct comparison of observed vs. predicted risk was not presented.10
The PCR equations systematically overestimate 10-year CVD risk, which is in part responsible for the guideline deeming substantially more individuals eligible for statin therapy when compared with previous guidelines. Although the difference between predicted and observed risk varies depending on the subpopulation analyzed, the equations' discrimination (ability to differentiate between individuals with and without disease) is good.11 Importantly, the estimation of cardiovascular risk is just that—an estimate. It is unlikely that data on CVD outcomes with statin therapy, directed by a risk prediction score, will be available in the near future. Family physicians who understand the use and limitations of the ACC/AHA PCR equations will be in the best position to direct a comprehensive discussion about an individual's overall cardiovascular risk and strategies to decrease that risk.
Applying the Evidence
A 67-year-old African American man presents as a new patient for evaluation of hypertension, for which he has been prescribed amlodipine (Norvasc) and chlorthalidone. He does not smoke and has no history of diabetes. His blood pressure is 132/78 mg per dL, total cholesterol is 216 mg per dL (5.59 mmol per L), and high-density lipoprotein cholesterol is 48 mg per dL (1.24 mmol per L). Based on the ACC/AHA PCR equations (http://my.americanheart.org/cvriskcalculator), what is his predicted 10-year atherosclerotic cardiovascular disease risk? What do you recommend to this patient?
Answer: His risk is calculated at 18.7%. After a discussion of risks, benefits, and alternatives, he accepts your recommendation to initiate moderate- to high-intensity statin therapy and continued therapeutic lifestyle change.

