A 40-year-old woman presented with a four-day history of sore throat, dry cough, malaise, and myalgia. She did not have red or watery eyes. One day before these symptoms began, she noted a rash on the inside of her mouth. She did not have constitutional symptoms such as fever, chills, or weight changes. She had not been exposed to sick contacts or unimmunized children.
On physical examination, she appeared well and was in no acute distress. There was mild tonsillar hypertrophy with mild erythema and no discharge. A greyish-white vesicular eruption with an erythematous background was noted on the buccal mucosa (Figure 1).
Figure 1.
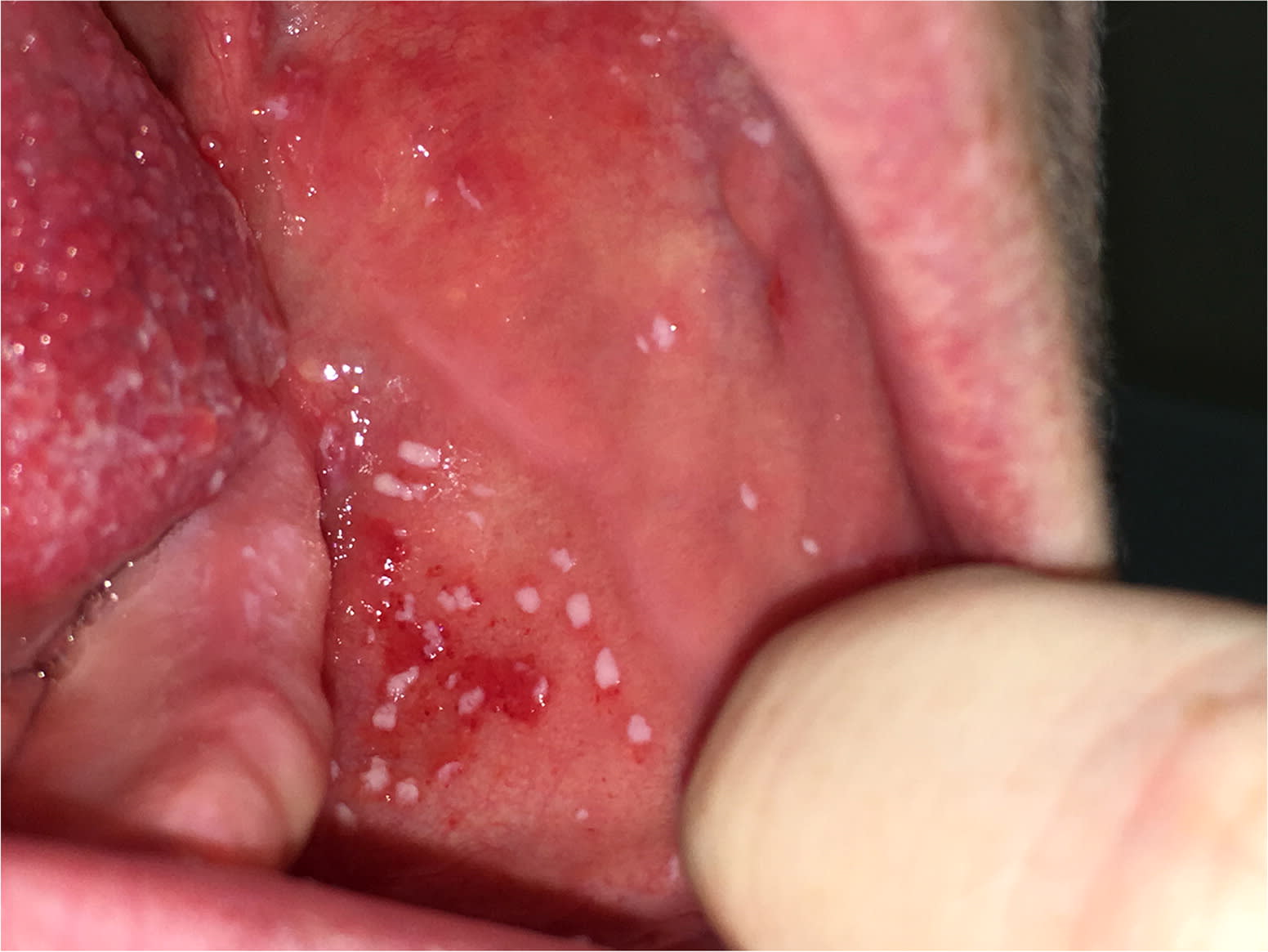
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Fordyce spots.
B. Herpetic gingivostomatitis.
C. Koplik spots.
D. Oral candidiasis.
Discussion
The answer is C: Koplik spots. Koplik spots are considered a pathognomonic sign of measles, or rubeola. Measles has an incubation period of six to 21 days. The prodrome lasts two to four days but may persist for as long as eight days. Symptoms typically include fever, malaise, and anorexia, followed by conjunctivitis, coryza, and cough. Approximately 48 hours before the onset of the measles exanthem, patients may develop an enanthem or mucosal rash that is characterized by Koplik spots. The lesions are whitish, grayish, or bluish, 1- to 3-mm elevations with an erythematous base, and are typically seen on the buccal mucosa opposite the molar teeth. The measles exanthem arises two to four days after the onset of fever and consists of an erythematous, maculopapular, blanching rash, which classically begins on the face and spreads to the neck, upper trunk, lower trunk, and extremities. Clinical improvement typically begins within 48 hours of the appearance of the rash.1,2
Confirming the diagnosis of measles requires serologic testing with virus-specific immunoglobulin G titers and viral culture. All cases of measles must be reported to state health departments. Measles was eradicated from the United States in 2000, but there are an estimated 3 to 4 million cases globally each year. In 2014, there were 667 cases of measles in the United States, most of which were acquired outside of the country.3 Treatment is supportive, including monitoring for complications. Isolation is important because the virus is highly contagious.3
Fordyce spots are benign neoplasms of the sebaceous glands. They present as isolated or scattered papules that are discrete, white to yellow, and 1 to 2 mm in size. They are particularly prominent on the vermilion border or buccal mucosa.1
Herpetic gingivostomatitis presents as multiple intraoral vesicular lesions and erosions bordered by an inflammatory, erythematous base. The lesions are typically seen on the lips, gingiva, oral palate, or tongue.1
Oral candidiasis, or thrush, can present in several ways. The pseudomembranous form is the most common and appears as white plaques on the buccal mucosa, palate, tongue, or oropharynx.1
Summary Table

| Condition | Characteristics |
|---|---|
| Fordyce spots | Discrete, white to yellow, 1- to 2-mm papules |
| Herpetic gingivostomatitis | Multiple intraoral vesicular lesions and erosions with an inflammatory, erythematous base; typically seen on the lips, gingiva, oral palate, or tongue |
| Koplik spots | Whitish, grayish, or bluish 1- to 3-mm elevations with an erythematous base; typically seen on the buccal mucosa opposite the molar teeth |
| Oral candidiasis | White plaques on the buccal mucosa, palate, tongue, or oropharynx |

