Am Fam Physician. 2017;96(3):189-190
Author disclosure: No relevant financial affiliations.
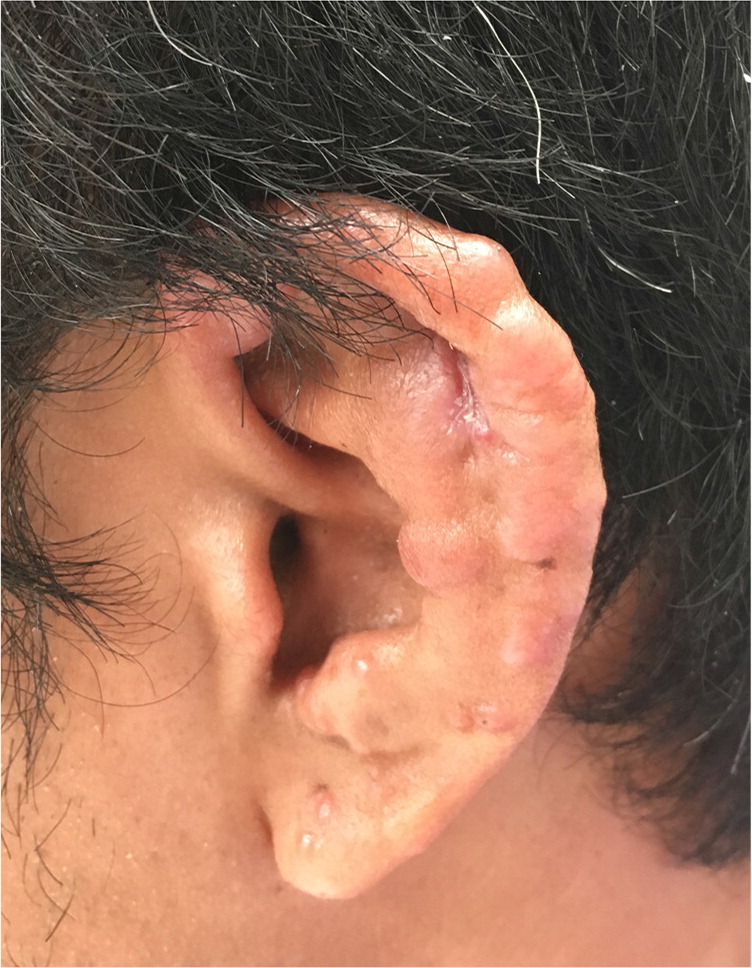
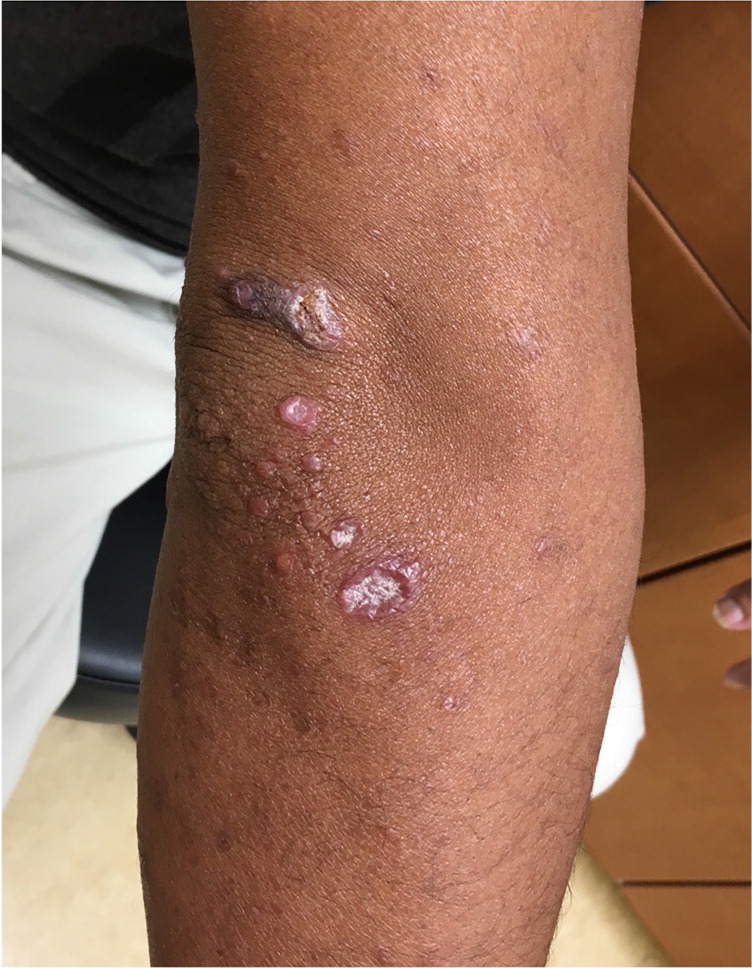
A 26-year-old man presented with a rash on much of his body that had steadily spread over one year. The rash covered his limbs, including his palms and soles, and his ears (Figures 1 and 2). He did not have associated pain, pruritus, or limb paresthesia. He did not have fevers, chills, night sweats, or weight loss. He was originally from the Marshall Islands and moved to Oklahoma within the six months before presentation. His vaccinations were up to date.
The physical examination revealed painless nodular lesions on his pinnae, arms, legs, hands, and feet. There were no lesions on his trunk or back. He had macular spots on his soles and palms. There were ulcerated nodules on his left wrist, elbows, and ankles.
Question
Discussion
The answer is C: Hansen disease (leprosy). The nodular painless rash on the limbs and, more specifically, the pinnae of the ear is suggestive of Hansen disease. Hansen disease is caused by Mycobacterium leprae infection and affects the skin and peripheral nerves. It is not as highly contagious as previously thought—about 95% of those who are exposed do not develop the disease.1,2 Hansen disease is rare, and most new cases in the United States are among immigrants. It is more common in males.2,3
Hansen disease should be suspected in a patient with hypopigmented patches or red skin nodules. These lesions are typically painless. Lumps or swelling of the earlobes and face is common. Patients may present with paresthesia or numbness in the hands and feet. Late findings are peripheral nerve damage leading to claw fingers, footdrop, or facial paralysis; glaucoma and blindness; and erectile dysfunction. Clinical, histologic, and immunologic manifestations of Hansen disease present along a spectrum. In the United States, the Ridley-Jopling system is most commonly used to classify the disease state.2–4
The National Hansen's Disease (Leprosy) Clinical Center assists physicians in the diagnosis and treatment of Hansen disease.4 Treatment consists of multiple drug regimens with dapsone, rifampin, and clofazimine for up to 24 months depending on disease classification and severity. Early treatment can decrease the risk of neuropathy and ophthalmologic complications.3,4
Annular psoriasis is a common skin condition associated with well-demarcated, erythematous, annular lesions, typically with a silver scale. These lesions tend to be on extensor surfaces and the scalp. Lesions are pruritic and can have periods of worsening and remission.
Cutaneous leishmaniasis is caused by the Leishmania parasite, which is transmitted through sandfly bites. The skin lesions are found only on areas of exposed skin. They begin as a papule and can progress to a plaque or nodule and finally to an ulcerated lesion over weeks to months. The lesions can be pruritic and are prone to secondary bacterial infections.5
Keloids are an excessive, fibrous reaction to tissue injury. They are more common in persons younger than 30 years, those with a family history of keloid formation, and those with darker skin tones.6 Keloids will extend past the original borders of the injury. Keloids can be painless or tender, and are occasionally pruritic.

| Condition | History | Characteristics |
|---|---|---|
| Annular psoriasis | Chronic with periods of worsening and remission | Well-demarcated, erythematous, annular, pruritic lesions with silvery scales on extensor surfaces and the scalp |
| Cutaneous leishmaniasis | Insect bite | Pruritic papule on exposed skin that progresses to an ulcerated lesion |
| Hansen disease (leprosy) | Chronic progression; contact with infected individual or armadillo | Nodular lesions on limbs, hands, feet, and ears; swelling of the face and earlobes; painless; can progress to neuropathy |
| Keloids | Skin trauma or scarring | Extends past the borders of the original injury; can be painless or painful |