Case Scenario
A 58-year-old nonspeaking patient with an intellectual disability was admitted to the hospital for cholecystitis. He also had a well-controlled seizure disorder, secondary parkinsonism from medications he was no longer taking, and diabetes insipidus. His surgery was uncomplicated. Because of the patient's underlying disability and need to drink a high volume of water to maintain sodium balance, his recovery proceeded slowly. Six days after surgery, his ability to swallow had partially recovered, but he was still requiring fluids and food through a nasogastric tube.
The hospitalist took the initiative to invite hospice representatives to a team meeting to discuss goals of care. He recommended a transfer to hospice care because of what he called, “The patient's suffering and risk of aspiration.” Hospice was willing to admit him based on the referral, and his family initially agreed. However, when the hospitalist was confronted with questions from the patient's primary care physician about the terminal diagnosis and evidence of suffering, it became clear that the recommendation for hospice was based on the hospitalist's misperception of the patient's quality of life and pressures to advance discharge, rather than on specific medical indications. The patient was back home within a couple of months, eating his favorite foods, and he recovered to his previous baseline function. He has returned to his day program and activities. What could the hospitalist have done better to support and expedite this outcome?
Commentary
False assumptions about patients' quality of life can affect prognosis, the treatment options that we present, and the types of referrals that we offer. In this case, the physician equated complex disability with terminal illness. This common confusion can result in premature withdrawal of life-preserving care. Disability is not a disease. Persons with physical, mental, and cognitive disabilities can and do live rich, full lives. They are often healthy, even if they need support for basic activities of daily living. If well managed, secondary conditions such as aspiration, pressure sores, and osteoporosis can be prevented or minimized. With appropriate services and accommodations, persons with disabilities can make decisions, have relationships, and contribute to their community. This outcome is more likely when they are welcomed, supported, and valued. Despite a high prevalence of chronic medical conditions, the life expectancy of persons with developmental disabilities approaches that of the general population.1
Physicians may mistakenly extrapolate high rates of significant functional decline observed in older patients after hospitalization to younger patients with complex disabilities. Younger patients with disabilities, however, are often healthier and more resilient than older patients, and their prognosis is often better after an acute illness.
This patient is recovering slowly from an acute, temporary illness. The physician's concern for aspiration, although understandable, hardly warranted transfer to hospice. Aspiration is a preventable secondary condition that can be effectively managed through diet texture, posture, careful supervision, and assistance with feeding. Falsely labeling a person with a disability as terminally ill can create a self-fulfilling prophecy, especially for those who need long-term support to thrive.2
Physicians should be careful to avoid making assumptions about patients' quality of life, especially those who rely on external assistance. They should also avoid reinforcing patient or caregiver fears and misconceptions about living with disability. For example, in one study of hospitalized able patients with serious illnesses, more than one-half of respondents believed that some health states were the same as or worse than death, including incontinence, requiring a breathing tube, relying on a feeding tube, or needing care from others all of the time.3 But many persons with developmental disabilities have required these supports since birth, yet still have meaningful lives.4 After a period of adjustment, those who live with acquired, chronic illness and disability also typically rate their own quality of life significantly higher than their physicians and caregivers do. Self-reported quality of life for persons with disabilities is not significantly different than that of the general population.5–7
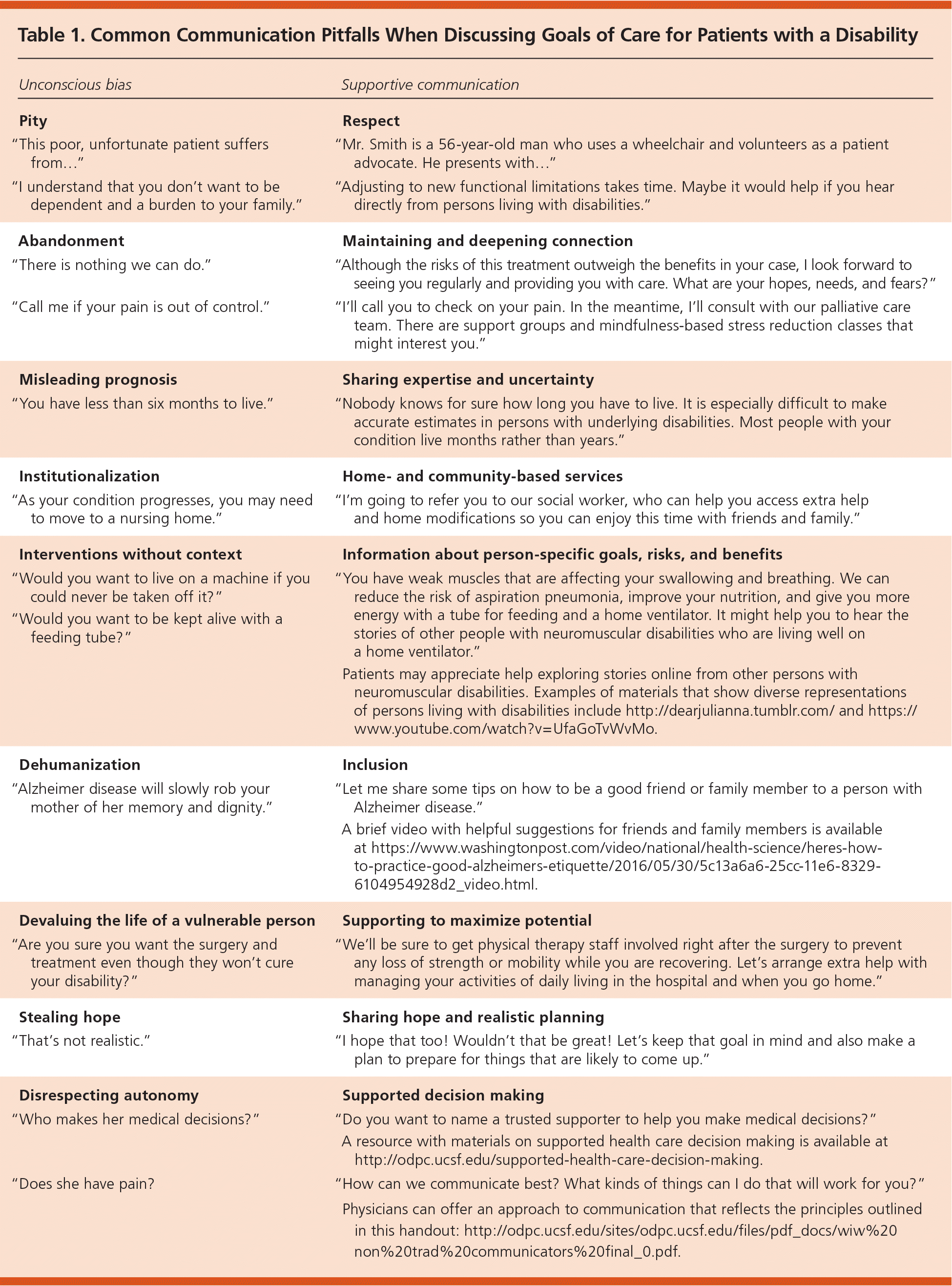
Instead of sharing decision making and respecting autonomy, physicians may unconsciously project their own attitudes onto the patients they serve through how they frame informed-consent discussions.8 Table 1 includes examples of common communication pitfalls with alternative phrasing and resources. Being aware of unconscious biases will help physicians better support their patients during stressful times.
The attitudes and beliefs of physicians can interfere with the care patients want or need.9 We can improve access by reassuring patients that no matter what choices they face, we will care and advocate for them.
Table 1. Common Communication Pitfalls When Discussing Goals of Care for Patients with a Disability
| Unconscious bias | Supportive communication |
|---|---|
| Pity | Respect |
| “This poor, unfortunate patient suffers from…” | “Mr. Smith is a 56-year-old man who uses a wheelchair and volunteers as a patient advocate. He presents with…” |
| “I understand that you don't want to be dependent and a burden to your family.” | “Adjusting to new functional limitations takes time. Maybe it would help if you hear directly from persons living with disabilities.” |
| Abandonment | Maintaining and deepening connection |
| “There is nothing we can do.” | “Although the risks of this treatment outweigh the benefits in your case, I look forward to seeing you regularly and providing you with care. What are your hopes, needs, and fears?” |
| “Call me if your pain is out of control.” | “I'll call you to check on your pain. In the meantime, I'll consult with our palliative care team. There are support groups and mindfulness-based stress reduction classes that might interest you.” |
| Misleading prognosis | Sharing expertise and uncertainty |
| “You have less than six months to live.” | “Nobody knows for sure how long you have to live. It is especially difficult to make accurate estimates in persons with underlying disabilities. Most people with your condition live months rather than years.” |
| Institutionalization | Home- and community-based services |
| “As your condition progresses, you may need to move to a nursing home.” | “I'm going to refer you to our social worker, who can help you access extra help and home modifications so you can enjoy this time with friends and family.” |
| Interventions without context | Information about person-specific goals, risks, and benefits |
| “Would you want to live on a machine if you could never be taken off it?” | “You have weak muscles that are affecting your swallowing and breathing. We can reduce the risk of aspiration pneumonia, improve your nutrition, and give you more energy with a tube for feeding and a home ventilator. It might help you to hear the stories of other people with neuromuscular disabilities who are living well on a home ventilator.” |
| “Would you want to be kept alive with a feeding tube?” | Patients may appreciate help exploring stories online from other persons with neuromuscular disabilities. Examples of materials that show diverse representations of persons living with disabilities include http://dearjulianna.tumblr.com/ and https://www.youtube.com/watch?v=UfaGoTvWvMo. |
| Dehumanization | Inclusion |
| “Alzheimer disease will slowly rob your mother of her memory and dignity.” | “Let me share some tips on how to be a good friend or family member to a person with Alzheimer disease.” |
| A brief video with helpful suggestions for friends and family members is available at https://www.washingtonpost.com/video/national/health-science/heres-how-to-practice-good-alzheimers-etiquette/2016/05/30/5c13a6a6-25cc-11e6-8329-6104954928d2_video.html. | |
| Devaluing the life of a vulnerable person | Supporting to maximize potential |
| “Are you sure you want the surgery and treatment even though they won't cure your disability?” | “We'll be sure to get physical therapy staff involved right after the surgery to prevent any loss of strength or mobility while you are recovering. Let's arrange extra help with managing your activities of daily living in the hospital and when you go home.” |
| Stealing hope | Sharing hope and realistic planning |
| “That's not realistic.” | “I hope that too! Wouldn't that be great! Let's keep that goal in mind and also make a plan to prepare for things that are likely to come up.” |
| Disrespecting autonomy | Supported decision making |
| “Who makes her medical decisions?” | “Do you want to name a trusted supporter to help you make medical decisions?” |
| A resource with materials on supported health care decision making is available at http://odpc.ucsf.edu/supported-health-care-decision-making. | |
| “Does she have pain? | “How can we communicate best? What kinds of things can I do that will work for you?” |
| Physicians can offer an approach to communication that reflects the principles outlined in this handout: http://odpc.ucsf.edu/sites/odpc.ucsf.edu/files/pdf_docs/wiw%20non%20trad%20communicators%20final_0.pdf. |

