Infant mortality is a key indicator for the health of a population. The United States currently ranks 26th in the world for infant mortality despite spending more than twice as much on health care.1 It lags behind economically similar countries, with little reduction in infant mortality for more than a decade. Alarmingly, the United States is the only developed country with a rising maternal mortality rate; women are more likely to die in or around childbirth now than 20 years ago.2 Regardless of community, profession, or political affiliation, this should create a sense of urgency for action and solutions.
Although not widely recognized, the top two drivers of pregnancy-related maternal death in the United States are not pregnancy specific. Cardiovascular and noncardiovascular chronic conditions (e.g., diabetes mellitus) account for 30% of maternal mortality. The leading drivers of infant mortality, congenital birth defects (20%) and preterm birth and low birth weight (18%), have remained relatively unchanged for decades and can both be directly and indirectly related to maternal health.3
For more than four decades, preconception care has been promoted as an important evidence-based part of women's health.4,5 Yet, only one in five women reports having had a preconception care visit before pregnancy.6 A traditional strategy has focused on providing preconception care to women who are planning a pregnancy at scheduled contraception visits or annual wellness examinations.
This traditional approach, however, is systematically challenged. Almost one-half of U.S. pregnancies are unintended.7 Despite robust evidence for neural tube defect prevention, only two in five women report taking folic acid before conception.8 One in four women of reproductive age in the United States has no health insurance coverage. Many women miss their postpartum visit, thus missing the opportunity for reproductive planning and the chance to be connected back to primary care and address any identified risks for the future.
Simultaneously, U.S. women of reproductive age are increasingly experiencing more health risks: more than 50% are overweight or obese, 43% have some type of chronic disease requiring frequent follow-up or medication, more women are having pregnancies later in life, and substance abuse and mental health issues are common.6–9
In 2006, the Centers for Disese Control and Prevention's Select Panel on Preconception Care published Recommendations to Improve Preconception Health and Health Care—United States.10 Recommendation 3 states that risk assessment and educational and health promotion counseling should be provided as part of primary care visits to all women of childbearing age to reduce reproductive risks and improve pregnancy outcomes. Recommendation 5 targets the care between pregnancies, specifically for women who experienced an adverse birth outcome.10 It is now 2017. Little progress toward actualizing these recommendations has been made. Providing quality preconception care is the responsibility of all primary care physicians, not just those who provide maternity care or handle a high volume of women's health.
The American Academy of Family Physicians recently published a position paper highlighting the importance of preconception care and the leading role family physicians should play in its provision.11 It provides an evidence-based summary of the key components of preconception care for men and women with suggested questions and care considerations for quick review (Tables 1 and 2).11 Family physicians are the most frequent provider of ambulatory primary care services to women 18 to 44 years of age.12,13 They also play a major role in providing these services to children and men.12 Family physicians have an outstanding opportunity to address preconception health issues in multiple settings, including when parents accompany their children to well-child visits, and during acute or chronic disease management encounters for both men and women.
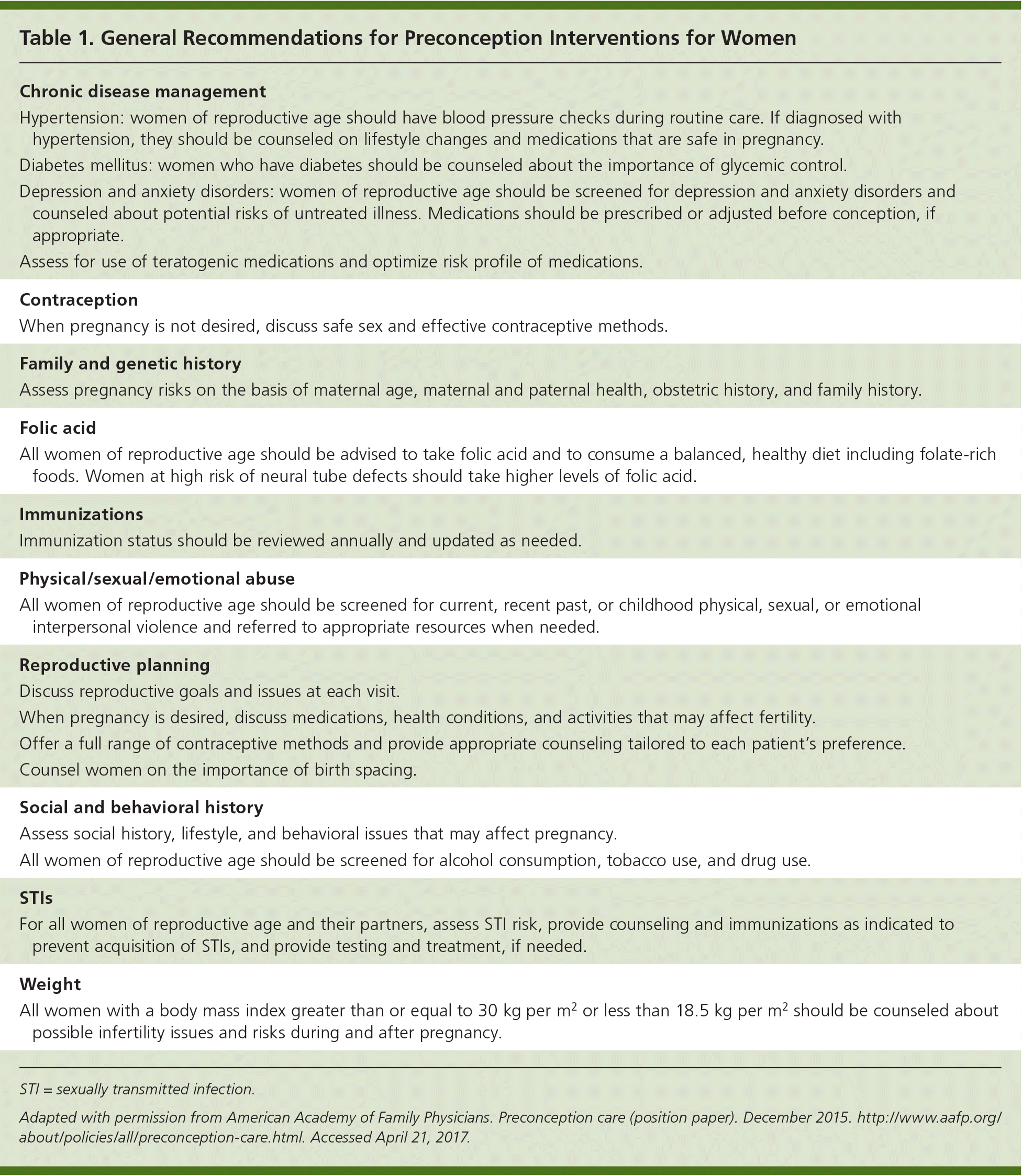
Table 1. General Recommendations for Preconception Interventions for Women
| Chronic disease management |
| Hypertension: women of reproductive age should have blood pressure checks during routine care. If diagnosed with hypertension, they should be counseled on lifestyle changes and medications that are safe in pregnancy. |
| Diabetes mellitus: women who have diabetes should be counseled about the importance of glycemic control. |
| Depression and anxiety disorders: women of reproductive age should be screened for depression and anxiety disorders and counseled about potential risks of untreated illness. Medications should be prescribed or adjusted before conception, if appropriate. |
| Assess for use of teratogenic medications and optimize risk profile of medications. |
| Contraception |
| When pregnancy is not desired, discuss safe sex and effective contraceptive methods. |
| Family and genetic history |
| Assess pregnancy risks on the basis of maternal age, maternal and paternal health, obstetric history, and family history. |
| Folic acid |
| All women of reproductive age should be advised to take folic acid and to consume a balanced, healthy diet including folate-rich foods. Women at high risk of neural tube defects should take higher levels of folic acid. |
| Immunizations |
| Immunization status should be reviewed annually and updated as needed. |
| Physical/sexual/emotional abuse |
| All women of reproductive age should be screened for current, recent past, or childhood physical, sexual, or emotional interpersonal violence and referred to appropriate resources when needed. |
| Reproductive planning |
| Discuss reproductive goals and issues at each visit. |
| When pregnancy is desired, discuss medications, health conditions, and activities that may affect fertility. |
| Offer a full range of contraceptive methods and provide appropriate counseling tailored to each patient's preference. |
| Counsel women on the importance of birth spacing. |
| Social and behavioral history |
| Assess social history, lifestyle, and behavioral issues that may affect pregnancy. |
| All women of reproductive age should be screened for alcohol consumption, tobacco use, and drug use. |
| STIs |
| For all women of reproductive age and their partners, assess STI risk, provide counseling and immunizations as indicated to prevent acquisition of STIs, and provide testing and treatment, if needed. |
| Weight |
| All women with a body mass index greater than or equal to 30 kg per m2 or less than 18.5 kg per m2 should be counseled about possible infertility issues and risks during and after pregnancy. |
STI = sexually transmitted infection.
Adapted with permission from American Academy of Family Physicians. Preconception care (position paper). December 2015. https://www.aafp.org/about/policies/all/preconception-care.html. Accessed April 21, 2017.
Table 2. General Recommendations for Preconception Interventions for Men

| Contraception |
| When a partner's pregnancy is not desired, discuss effective contraceptive methods. |
| Family and genetic history |
| Assess family history and genetic susceptibility. |
| Physical/sexual/emotional abuse |
| Beginning in adolescence, consider screening for and counseling to avoid intimate partner violence and coercive relationships, and promote respectful and consensual sexual relationships. |
| Reproductive planning |
| Male reproductive health issues should be discussed at every wellness visit. |
| Assess the patient's understanding of reproduction and his reproductive plan. |
| When a partner's pregnancy is desired, discuss medications, conditions, and activities that may affect fertility. |
| Conduct a physical examination looking for signs or conditions that may affect fertility. |
| Social and behavioral history |
| Assess social history, lifestyle risk factors (including smoking, substance abuse, and unsafe sex), and behavioral issues. |
| Assess for occupational hazards that may affect fertility. |
| STIs |
| Assess STI risk, provide counseling and immunizations as indicated to prevent acquisition of STIs, and provide testing and treatment, if needed. |
STI = sexually transmitted infection.
Adapted with permission from American Academy of Family Physicians. Preconception care (position paper). December 2015. https://www.aafp.org/about/policies/all/preconception-care.html. Accessed April 21, 2017.
Transforming the way preconception care is delivered is critical to success. Many of the components of quality preconception care are already incorporated into routine preventive care and monitored through quality improvement measures (e.g., immunizations, smoking, depression screening and counseling, weight management). However, women of reproductive age may have different chronic disease goals and/or medication recommendations depending on their future pregnancy desires. This position paper emphasizes the importance of incorporating routine identification of pregnancy intention for men and women of reproductive age to inform shared decision making around reproductive planning and risk reduction. Because reproductive choices and risks can change over time, preconception health risks should be routinely assessed during chronic disease management visits, as well as visits for acute care, and should not be limited to contraceptive, preconception, or wellness visits. Preconception care is primary care and must become a priority for primary care physicians in all settings.11

