A 54-year-old woman presented with painful lesions on her upper and lower extremities that developed a few weeks earlier. The rash did not improve after two courses of antibiotics. She had a fever and severe generalized pain. Her medical history was unremarkable.
Physical examination revealed an erythematous rash with vesicles and papules (Figure 1). Her temperature was 101°F (38°C). She was admitted for intravenous antibiotic treatment, pain control, and infectious disease consultation. Initial laboratory results showed anemia, thrombocytopenia, elevated erythrocyte sedimentation rate, and elevated C-reactive protein level.
FIGURE 1.
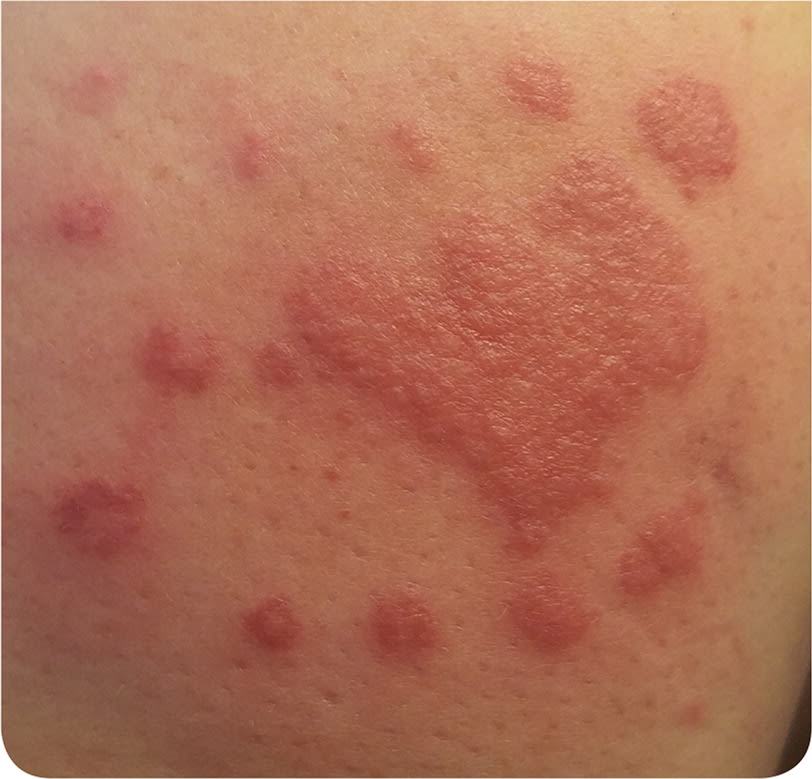
Question
Based on the patient's history, physical examination, and laboratory findings, which one of the following is the most likely diagnosis?
A. Contact dermatitis.
B. Drug eruption rash.
C. Erythema multiforme.
D. Erythema nodosum.
E. Sweet syndrome.
Discussion
The answer is E: Sweet syndrome. Sweet syndrome, or acute febrile neutrophilic dermatitis, is characterized by painful papules, nodules, or plaques caused by an accumulation of neutrophils in the dermis.1 Multiple tender, erythematous lesions develop on the skin or mucosa, most commonly on the face, neck, and upper and lower extremities.1 There are three forms of Sweet syndrome: classic, malignancy associated, and drug induced.2,3 Diagnosis includes major and minor criteria. Major criteria are the rapid onset of painful erythematous plaques and nodules, and typical histopathology of dense neutrophil infiltration without leukocytoclastic vasculitis.4 Minor criteria include fever higher than 100.4°F (38°C), erythrocyte sedimentation rate greater than 20 mm per hour, white blood cell count greater than 8,000 per mm3 (8 × 109 per L), neutrophils greater than 70%, and an elevated C-reactive protein level.4
Sweet syndrome is often diagnosed in patients who have a history of upper respiratory tract infection, recent immunization, gastrointestinal infection, hematologic or solid neoplasia, or inflammatory disorder, or in women who are pregnant.1,4 Sweet syndrome responds to treatment with a corticosteroid or potassium iodide.1,4 In this patient, a bone marrow biopsy confirmed acute myeloid leukemia. About 20% of Sweet syndrome cases occur in patients with cancer.2,3 A punch biopsy was consistent with the cutaneous infiltrate of chronic myelogenous leukemia.
Contact dermatitis is a delayed cutaneous reaction to an irritant. It is characterized by vesicles, edema, redness, and pruritus.1
A drug eruption is a diffuse maculopapular or papulosquamous rash or hives that generally spare the face. Common causative medications are penicillin, carbamazepine (Tegretol), and allopurinol.1
Erythema multiforme is a cutaneous reaction to antigenic stimuli such as drugs or an infection. It may be idiopathic. It is characterized by target lesions, which are maculopapular with central clearing and a discrete ring of erythema. The lesions are symmetric, involving palms, soles, and the dorsum of hands and feet.1
Erythema nodosum is an acute inflammatory and immunologic reaction of subcutaneous fat to drugs, infection, or inflammatory diseases. It is characterized by pink or dusty-red, firm nodules with blurred edges, most commonly on pretibial surfaces.1
SUMMARY TABLE
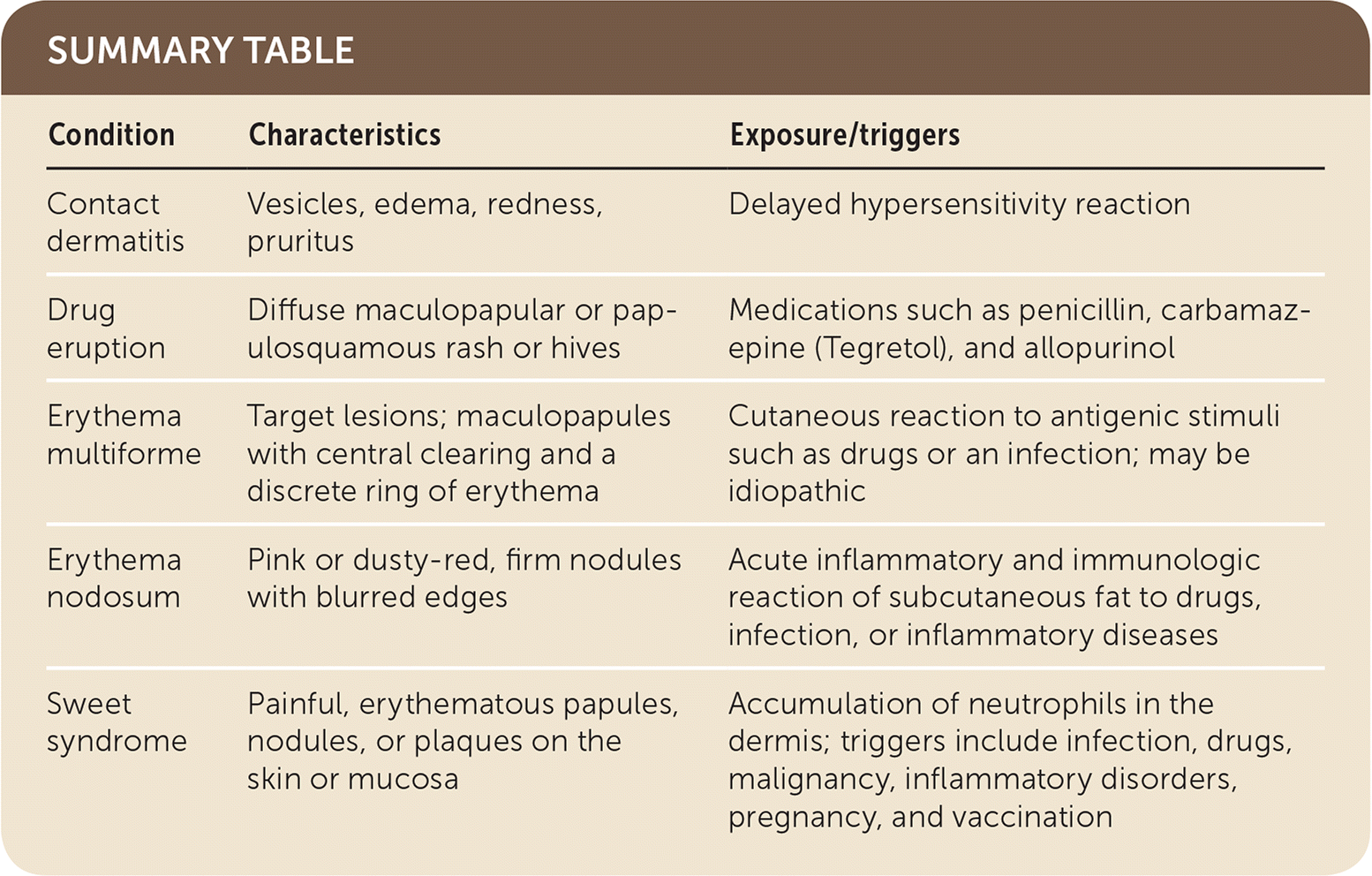
| Condition | Characteristics | Exposure/triggers |
|---|---|---|
| Contact dermatitis | Vesicles, edema, redness, pruritus | Delayed hypersensitivity reaction |
| Drug eruption | Diffuse maculopapular or papulosquamous rash or hives | Medications such as penicillin, carbamazepine (Tegretol), and allopurinol |
| Erythema multiforme | Target lesions; maculopapules with central clearing and a discrete ring of erythema | Cutaneous reaction to antigenic stimuli such as drugs or an infection; may be idiopathic |
| Erythema nodosum | Pink or dusty-red, firm nodules with blurred edges | Acute inflammatory and immunologic reaction of subcutaneous fat to drugs, infection, or inflammatory diseases |
| Sweet syndrome | Painful, erythematous papules, nodules, or plaques on the skin or mucosa | Accumulation of neutrophils in the dermis; triggers include infection, drugs, malignancy, inflammatory disorders, pregnancy, and vaccination |

