Measurement of vitamin D levels and supplementation with oral vitamin D have become commonplace, although clinical trials have not demonstrated health benefits. The usefulness of serum 25-hydroxyvitamin D levels to assess adequate exposure to vitamin D is hampered by variations in measurement technique and precision. Serum levels less than 12 ng per mL reflect inadequate vitamin D intake for bone health. Levels greater than 20 ng per mL are adequate for 97.5% of the population. Routine vitamin D supplementation does not prolong life, decrease the incidence of cancer or cardiovascular disease, or decrease fracture rates. Screening asymptomatic individuals for vitamin D deficiency and treating those considered to be deficient do not reduce the risk of cancer, type 2 diabetes mellitus, or death in community-dwelling adults, or fractures in persons not at high risk of fractures. Randomized controlled trials of vitamin D supplementation in the treatment of depression, fatigue, osteoarthritis, and chronic pain show no benefit, even in persons with low levels at baseline.
Measurement of vitamin D levels and supplementation with oral vitamin D have become commonplace in clinical practice.1,2 In 2014, vitamin D levels were the fifth most common laboratory test ordered for Medicare patients, with a total cost of $323 million.1 Although vitamin D was first identified as a vitamin, it is now considered a prohormone and is unique to other nutrients because it can be synthesized in the skin through exposure to sunlight. Although vitamin D deficiency has been labeled a worldwide problem,3 estimates of disease burden are based on specific laboratory values,4 rather than on health problems that can be reliably attributed to low vitamin D levels or that have been shown to respond to vitamin D supplementation.
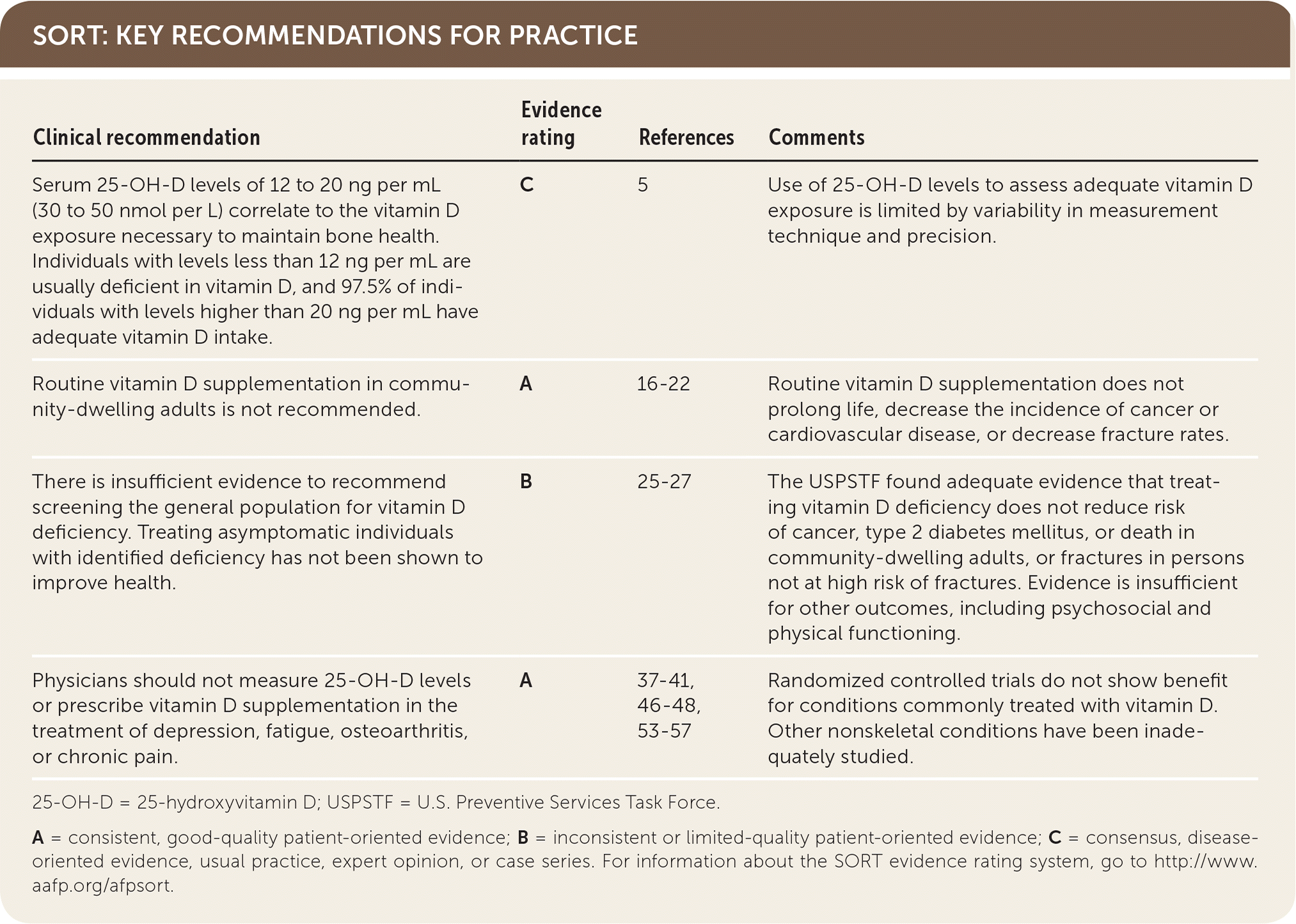
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
| Serum 25-OH-D levels of 12 to 20 ng per mL (30 to 50 nmol per L) correlate to the vitamin D exposure necessary to maintain bone health. Individuals with levels less than 12 ng per mL are usually deficient in vitamin D, and 97.5% of individuals with levels higher than 20 ng per mL have adequate vitamin D intake. | C | 5 | Use of 25-OH-D levels to assess adequate vitamin D exposure is limited by variability in measurement technique and precision. |
| Routine vitamin D supplementation in community-dwelling adults is not recommended. | A | 16–22 | Routine vitamin D supplementation does not prolong life, decrease the incidence of cancer or cardiovascular disease, or decrease fracture rates. |
| There is insufficient evidence to recommend screening the general population for vitamin D deficiency. Treating asymptomatic individuals with identified deficiency has not been shown to improve health. | B | 25–27 | The USPSTF found adequate evidence that treating vitamin D deficiency does not reduce risk of cancer, type 2 diabetes mellitus, or death in community-dwelling adults, or fractures in persons not at high risk of fractures. Evidence is insufficient for other outcomes, including psychosocial and physical functioning. |
| Physicians should not measure 25-OH-D levels or prescribe vitamin D supplementation in the treatment of depression, fatigue, osteoarthritis, or chronic pain. | A | 37–41, 46–48, 53–57 | Randomized controlled trials do not show benefit for conditions commonly treated with vitamin D. Other nonskeletal conditions have been inadequately studied. |
25-OH-D = 25-hydroxyvitamin D; USPSTF = U.S. Preventive Services Task Force.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to http://www.aafp.org/afpsort.
BEST PRACTICES IN ENDOCRINOLOGY

| Recommendation | Sponsoring organization |
|---|---|
| Do not perform population-based screening for 25-OH-D deficiency. | American Society for Clinical Pathology |
| Do not routinely measure 1,25-dihydroxyvitamin D unless the patient has hypercalcemia or decreased kidney function. | Endocrine Society/American Association of Clinical Endocrinologists |
25-OH-D = 25-hydroxyvitamin D.
Source: For more information on the Choosing Wisely Campaign, see http://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see http://www.aafp.org/afp/recommendations/search.htm.
The role vitamin D deficiency plays in the development of rickets and osteomalacia is established.5 Osteomalacia is a relatively rare condition characterized by replacement of resorbed bone with unmineralized osteoid. It has various causes, including prolonged severe vitamin D deficiency; improvement over weeks to months is typically dramatic with vitamin D repletion.6,7 It is standard of care to ensure adequate exposure to vitamin D and calcium in patients with osteoporosis,8 although trials of pharmacologic treatment of osteoporosis to prevent fracture have not evaluated the independent contribution of vitamin D.9–12
The management of skeletal diseases that may be related to vitamin D is beyond the scope of this review, which evaluates the broader impact of vitamin D on the health of persons without overt skeletal disease.
How Is Vitamin D Deficiency Defined?
The National Academy of Medicine (formerly the Institute of Medicine) considers a serum 25-hydroxyvitamin D (25-OH-D) level of 12 to 20 ng per mL (30 to 50 nmol per L) as the normal range for adequate exposure to vitamin D to maintain bone health. Individuals with levels less than 12 ng per mL will usually be deficient, and 97.5% of individuals with a serum level higher than 20 ng per mL have adequate vitamin D exposure.
EVIDENCE SUMMARY
Each laboratory independently establishes its own normal range for serum 25-OH-D levels. Commonly used cutoffs for deficiency or insufficiency are not based on the distribution of results across a healthy population, but rather on the correlation with physiologic parameters such as parathyroid hormone levels.
The National Academy of Medicine publishes a Dietary Reference Intakes report for an array of nutrients, including vitamin D.5 The report includes estimated average requirement, recommended dietary allowance, and tolerable upper intake level. The need for any biologic nutrient varies from person to person, generally in a normal distribution across the population. The recommended dietary allowance for vitamin D reflects the intake necessary to maintain bone health for those with the highest biologic need. Thus, the recommended dietary allowances of 600 IU per day for persons one to 70 years of age and 800 IU per day for persons older than 70 years are the allowances needed for those with the greatest biologic need, not the minimum or average needed across the population, which has been widely misinterpreted (Figure 1).13 The estimated average requirement is 400 IU per day. The estimated average requirement and the recommended dietary allowance both assume minimal to no sun exposure. Sufficient sun exposure to produce a light-pink skin hue (one minimal erythema dose) is equivalent to 20,000 IU of oral vitamin D.14
FIGURE 1.
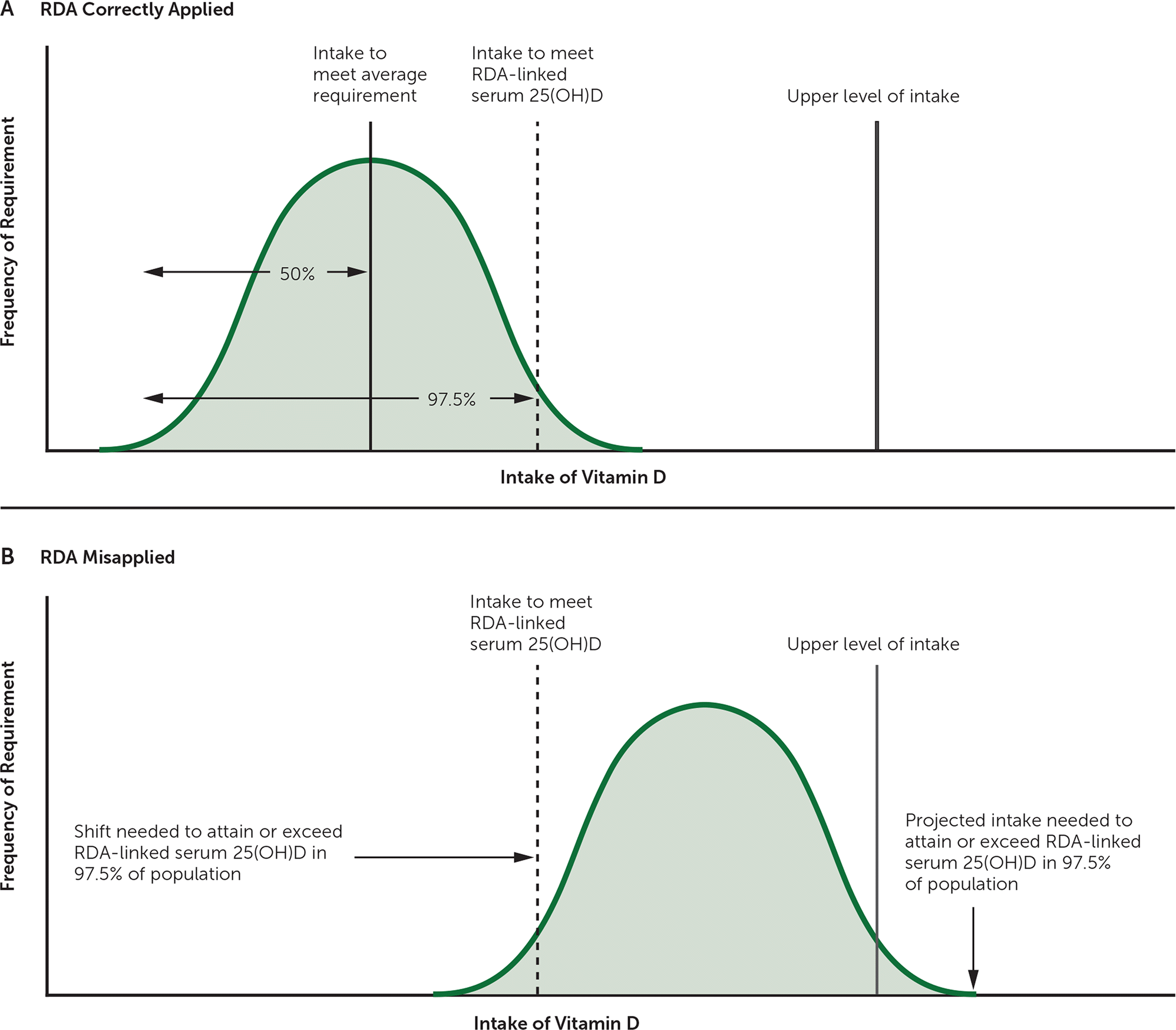
Distribution of vitamin D intake requirements in a healthy population (panel A) and the upward shift in distribution required to attain the RDA-linked serum 25(OH)D concentration in 97.5% of the population (panel B).
25(OH)D = 25-hydroxyvitamin D, RDA = recommended dietary allowance.
Reprinted with permission from Manson JE, Brannon PM, Rosen CJ, Taylor CL. Vitamin D deficiency—is there really a pandemic? N Engl J Med. 2016;375(19):1819.
Serum 25-OH-D concentrations may be useful as an indicator of adequacy of vitamin D exposure from all sources. The National Academy of Medicine concluded that serum 25-OH-D levels of 12 to 20 ng per mL correlate to the vitamin D exposure necessary to maintain bone health.5 Persons with levels less than 12 ng per mL are at significant risk of bone disease, and 97.5% of persons with levels higher than 20 ng per mL have adequate vitamin D for bone health.5 For an individual, a specific value in the normal range may not reflect sufficiency. For example, a value of 12 ng per mL will reflect adequate vitamin D for those with low biologic need, but it may be inadequate for those with a high biologic need.
These values are not universally accepted. For instance, the 2011 Endocrine Society guideline defines vitamin D insufficiency as a level between 21 and 29 ng per mL (52 to 72 nmol per L), citing early biochemical studies showing increased calcium absorption and decreased parathyroid hormone levels up to a threshold of 30 ng per mL (75 nmol per L).14
Using serum 25-OH-D levels to identify those with inadequate vitamin D is hampered by variations in measurement technique and precision. The Vitamin D Standardization Program specifies that an acceptable variance in assay precision is 10%, although this level of precision is not uniform across laboratories. In practice, this level of precision means that if the test value from an assay is 30 ng per mL, clinicians can be 95% certain that the true value is between 24 and 36 ng per mL (60 to 90 nmol per L).15
Does Routine Supplementation with Vitamin D in the Adult Population Result in Improved Health?
Clinical trials have not demonstrated health benefits of routine vitamin D supplementation in community-dwelling adults. Potential harms of excessive vitamin D include nephrolithiasis, soft tissue calcification, and renal and cardiovascular damage.
EVIDENCE SUMMARY
The U.S. Preventive Services Task Force (USPSTF) has addressed the use of vitamin D for prevention of cardiovascular disease, cancer, falls, and fractures. In 2014, the USPSTF concluded that the current evidence is insufficient to assess the balance of benefits and harms of using vitamin D with or without calcium for the prevention of cardiovascular disease, cancer, or all-cause mortality.16 In 2013 and again in a 2017 draft recommendation, the USPSTF considered the evidence adequate to recommend against daily supplementation with 400 IU or less of vitamin D3 and 1,000 mg or less of calcium for the primary prevention of fractures in noninstitutionalized postmenopausal women.17 Evidence was insufficient to determine benefits and harms of higher doses. In 2017, the USPSTF provisionally recommended against vitamin D supplementation to prevent falls in community-dwelling adults 65 years or older, based on recent trials that found no protective effects or potential harms.18–20
An umbrella review identified 87 meta-analyses of randomized controlled trials of vitamin D supplementation.21 Most of the meta-analyses including skeletal and nonskeletal benefits did not examine patient-oriented outcomes, and the number of trials evaluating each specific nonskeletal outcome identified was small. There was no beneficial effect on mortality, falls, or fractures. A meta-analysis adjusting for cumulative sample sizes demonstrated no evidence that vitamin D prevents ischemic heart disease, cerebrovascular disease, or cancer, and a futility analysis indicated that although trials are ongoing, they are unlikely to influence the outcome because of the size and consistency of the existing trials.22 Similarly, a systematic review found a shortage of large-scale and long-term randomized clinical trials supporting preventive or therapeutic benefits of vitamin D for chronic nonskeletal disorders.23
Short-term trials have not shown harms of vitamin D supplementation at doses consistent with the recommended dietary allowance,17,24 although the harms of long-term supplementation are unknown.5 The National Academy of Medicine considers a 25-OH-D level of 50 ng per mL (125 nmol per L) as reflective of the safe upper tolerable intake. Hypercalcemia and hypercalciuria are the hallmarks of excess vitamin D exposure and can eventually lead to nephrolithiasis, soft tissue calcification, and renal and cardiovascular damage. Vitamin D intoxication produces nonspecific symptoms that may include anorexia, weight loss, polyuria, and heart arrhythmias.5
Do Screening Asymptomatic Individuals for Vitamin D Deficiency and Supplementing Those Identified as Deficient Improve Health?
There is insufficient evidence to recommend screening the general population for vitamin D deficiency. Treating asymptomatic individuals with identified deficiency has not been shown to improve health.
EVIDENCE SUMMARY
The USPSTF and the American Academy of Family Physicians have concluded that the current evidence is insufficient to assess the balance of benefits and harms of screening for vitamin D deficiency in asymptomatic adults.25,26 The USPSTF found adequate evidence that treating vitamin D deficiency does not reduce the risk of cancer, type 2 diabetes mellitus, or death in community-dwelling adults, or the risk of fractures in persons not at high risk of fractures. The USPSTF found inadequate evidence regarding the benefits of treatment on other outcomes, including psychosocial and physical functioning. A recent randomized controlled trial including 230 postmenopausal women younger than 75 years with 25-OH-D levels between 14 and 27 ng per mL (35 to 67 nmol per L) compared vitamin D3 supplementation (800 IU daily or 50,000 IU twice per month) with placebo. Although increased calcium absorption occurred only in the high-dose group, the effect was small and did not translate into beneficial effects on bone mineral density, muscle function, muscle mass, or falls.27
Are There Specific Symptoms or Nonskeletal Disease States for Which Vitamin D Measurement and Supplementation Improve Health?
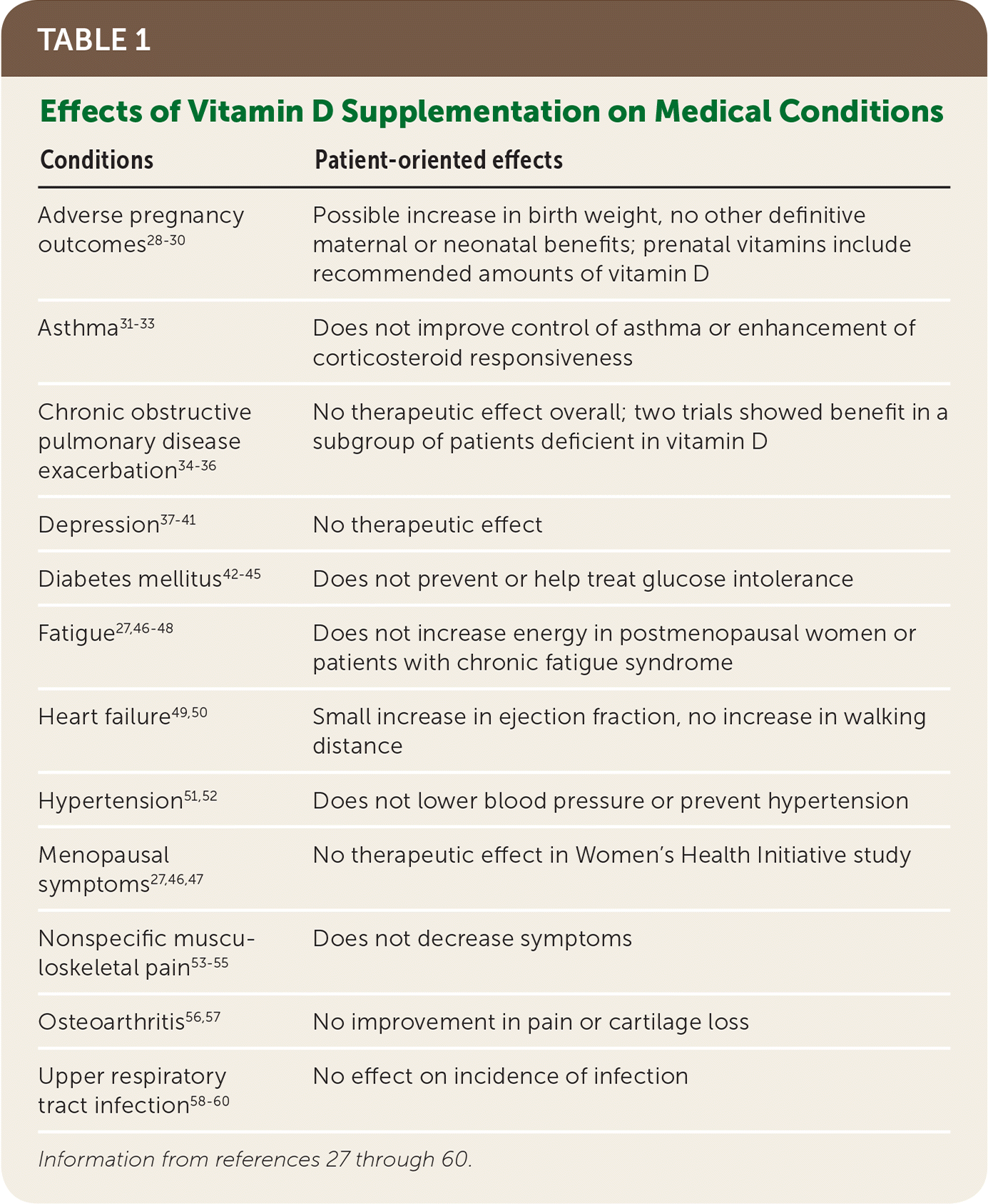
Therapeutic benefits for chronic nonskeletal disorders have not been established. A variety of nonskeletal disease states have been associated with vitamin D levels, but clinical trials generally do not support health benefits of supplementation. Evidence is mixed for some conditions, and larger trials will be required to draw definitive conclusions. Table 1 summarizes the effects of vitamin D supplementation on certain medical conditions.27–60
TABLE 1. Effects of Vitamin D Supplementation on Medical Conditions
| Conditions | Patient-oriented effects |
|---|---|
| Adverse pregnancy outcomes28–30 | Possible increase in birth weight, no other definitive maternal or neonatal benefits; prenatal vitamins include recommended amounts of vitamin D |
| Asthma31–33 | Does not improve control of asthma or enhancement of corticosteroid responsiveness |
| Chronic obstructive pulmonary disease exacerbation34–36 | No therapeutic effect overall; two trials showed benefit in a subgroup of patients deficient in vitamin D |
| Depression37–41 | No therapeutic effect |
| Diabetes mellitus42–45 | Does not prevent or help treat glucose intolerance |
| Fatigue27,46–48 | Does not increase energy in postmenopausal women or patients with chronic fatigue syndrome |
| Heart failure49,50 | Small increase in ejection fraction, no increase in walking distance |
| Hypertension51,52 | Does not lower blood pressure or prevent hypertension |
| Menopausal symptoms27,46,47 | No therapeutic effect in Women's Health Initiative study |
| Nonspecific musculoskeletal pain53–55 | Does not decrease symptoms |
| Osteoarthritis56,57 | No improvement in pain or cartilage loss |
| Upper respiratory tract infection58–60 | No effect on incidence of infection |
EVIDENCE SUMMARY
Fatigue or Depression. A study of Women's Health Initiative trial participants showed that vitamin D deficiency was not associated with an increased rate of menopausal symptoms at baseline,46 and daily supplementation with 400 IU of vitamin D plus 1,000 mg of calcium did not improve energy, sleep, or mood over six years of follow-up.47 A randomized trial of high-dose supplementation (100,000 IU every two months) in patients with chronic fatigue syndrome showed no benefit.48 Because of a cross-sectional association between low vitamin D and depressed mood, vitamin D measurements are often ordered and supplements prescribed as part of the management of depression.46 However, vitamin D levels are not prospectively related to depression, implying the association is due to confounding.37,38,47 Randomized trials and meta-analyses have not demonstrated that vitamin D supplementation has a therapeutic effect on depression.39–41
Chronic Pain or Osteoarthritis. Two large, multiyear randomized trials showed no improvement in pain or cartilage loss in patients with osteoarthritis taking vitamin D supplements.56,57 Women in the supplementation arm of the Women's Health Initiative trial had no improvement in joint symptoms compared with placebo.53 A randomized controlled trial in Norway found that vitamin D supplementation did not improve nonspecific musculoskeletal pain or headache compared with placebo, despite increases in serum 25-OH-D levels.54 A 2015 Cochrane review concluded that vitamin D is ineffective as a treatment for chronic painful conditions.55
Glycemic Control in Prediabetes or Diabetes. There is sufficient evidence that vitamin D is ineffective as an adjunct for glycemic control. Supplementation has not been shown to improve glycemic control in patients with type 2 diabetes.42,43 In one five-year trial, supplementation did not reduce progression of prediabetes to diabetes.44 A randomized trial of supplementation in pregnant women did not show a decrease in rates of gestational diabetes.45
Respiratory Conditions. Although a Cochrane review of trials involving children and adults with asthma suggested that vitamin D supplementation may reduce exacerbations and hospitalizations,61 the largest trial in adults using inhaled corticosteroids found no benefit.31,32 Supplementation in pregnant women did not reduce wheezing in their children.33 Studies of vitamin D supplementation in patients with chronic obstructive pulmonary disease are conflicting. In randomized trials, supplementation did not improve symptoms of chronic obstructive pulmonary disease and did not reduce exacerbations in those with baseline 25-OH-D levels greater than 20 ng per mL.34 In two studies, supplementation in subgroups of patients with 25-OH-D levels less than 20 ng per mL decreased moderate to severe exacerbations.35,36 Multiple randomized controlled trials showed that vitamin D supplementation does not meaningfully affect the incidence of upper respiratory tract infection.58–60
Editor's Note: Dr. LeFevre served as a member, vice chair, and chair of the USPSTF from 2005 to 2015, and coauthored its recommendation statements relating to vitamin D screening and supplementation.
This article updates a previous article on this topic by Bordelon, et al.62
Data Sources: Medline was searched covering the years 2012 to 2016. The first search was for all randomized clinical trials of vitamin D and returned 573 citations. The second search was for meta-analyses and systematic reviews of vitamin D and returned 183 citations. Results were reviewed in abstract form, and selected relevant full-text articles were also reviewed. An evidence summary, generated from Essential Evidence, that included relevant POEMs, Cochrane reviews, diagnostic test data, and a custom PubMed search for the best available evidence was also reviewed. Additional reviews included all relevant USPSTF recommendations and evidence reports, a summary of the Vitamin D: Moving Toward Evidence-based Decision Making in Primary Care conference (December 2 to 3, 2014; Office of Dietary Supplements, National Institutes of Health), and the National Academy of Medicine report Dietary Reference Intakes: Calcium, Vitamin D. Search date: May 2016.

