
Am Fam Physician. 2018;97(4):271-272
Author disclosure: No relevant financial affiliations.
A 25-year-old man presented with malaise, fatigue, headache, and redness in his left eye. He was treated with oseltamivir (Tamiflu) for presumed influenza. The next day, his headaches became worse, and he developed blurry vision and eye pain with discharge. He went to the emergency department, where he was found to have dyspnea and hypotension. He had worsening hypoxic respiratory failure, and was intubated and admitted to the intensive care unit. His medical history was significant for intravenous heroin use.
On physical examination, his left eye was opaque, with scleral redness and edema. There was a prominent gray ring on the perimeter of the iris with purulent drainage (Figure 1). A retinal examination was not possible because of the hazy discoloration. Janeway lesions were noted on both hands. Because of lethargy, a lumbar puncture was performed. Cultures from blood, cerebral spinal fluid, urine, and sputum all showed methicillin-sensitive Staphylococcus aureus. A transesophageal echocardiogram revealed multiple mobile echogenicities on the mitral valve and severe mitral regurgitation.
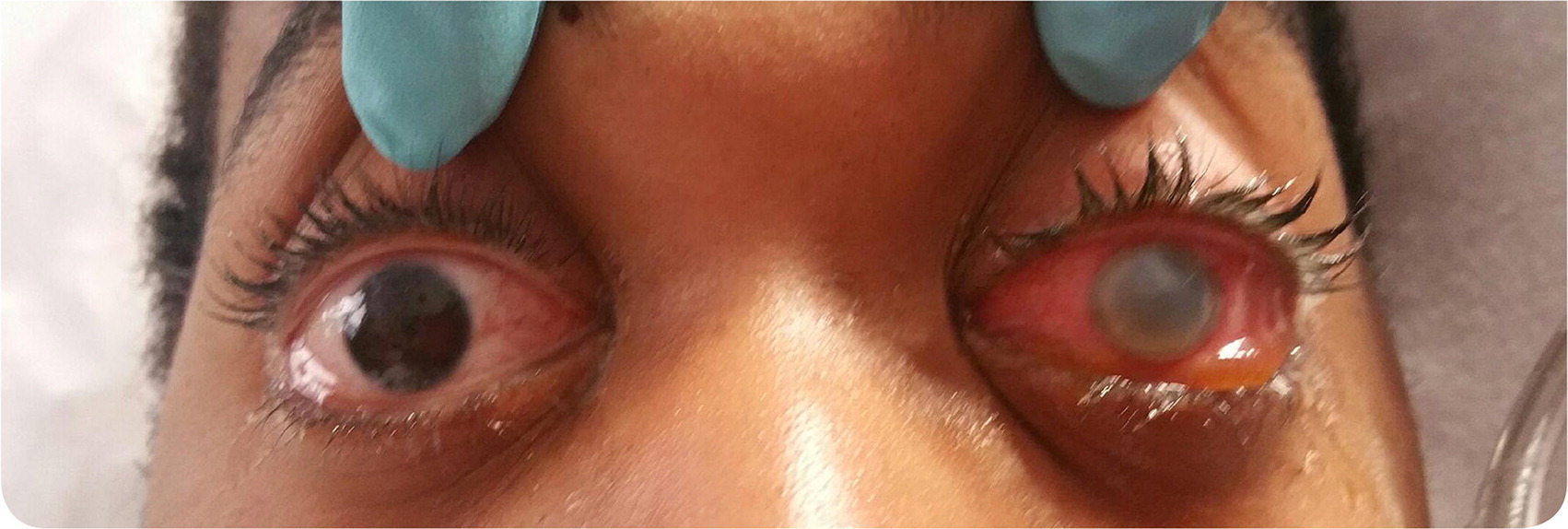
Question
Discussion
The answer is D: intravitreal ceftazidime and vancomycin. This patient presented with the clinical features of bacterial endocarditis with complication of endogenous endophthalmitis. Bacterial endocarditis initially should be treated empirically with intravenous vancomycin and an aminoglycoside or a third-generation cephalosporin, but the use of intravenous antibiotics alone is insufficient for endogenous endophthalmitis. To salvage ocular function, concurrent therapy with intravitreal antibiotics is recommended, often with an emergent vitrectomy. The decision to use intravitreal antibiotics or vitrectomy depends on the patient's vision at the time of diagnosis and overall hemodynamic condition.1
The clinical signs of endogenous endophthalmitis are eyelid edema, conjunctival injection, circumcorneal congestion, pain, photophobia, and the presence of floaters.2 Patients often have hypopyon or leukocytic exudate in the anterior chamber of the eye. Because of the nonspecific symptoms, diagnosing early presentations of endogenous endophthalmitis can be challenging. It is misdiagnosed as conjunctivitis, acute glaucoma, or other ocular conditions in 16% to 63% of cases.3 Systemic antibiotics are used to treat the source of infection, with two to four weeks of therapy required to ensure eradication of the infection and prevent reinfection of the eye.3
Although this patient's left eye was affected, the right eye is most often involved because of the direct blood flow from the right brachiocephalic artery to the right carotid artery.1 The most common eye complications from bacterial endocarditis are retinal hemorrhage (Roth spots) and conjunctival hemorrhages.4 However, more invasive bacterial infection could lead to endogenous endophthalmitis, which is a medical emergency.3 Blindness may occur from damage caused by septic emboli entering the posterior segment vasculature and disseminating the organism into the surrounding tissues with subsequent microbial proliferation and inflammatory reactions.2 An ophthalmoscopic examination should be performed as soon as hypopyon is noted in the eye.
Gram-positive bacteria cause 75% of endogenous endophthalmitis cases—25% from S. aureus and 32% from streptococcus. Endogenous endophthalmitis caused by streptococcus in adults is usually related to endocarditis.3,5 The primary organism identified for this patient's infective endocarditis was S. aureus, which accounts for 20% to 30% of bacterial endocarditis cases, most commonly from intravenous drug use.4
There are several other causes of red eye that should be considered in the differential diagnosis. Acute retinal necrosis causes a red eye with periorbital pain. Patients report blurry or hazy vision, with floaters and decreased color vision. Fungal endophthalmitis also causes a red eye with photophobia and vision loss. Patients may report floaters and scotoma but may be asymptomatic. Intermediate uveitis presents as a red eye and decreased visual acuity, blurry vision, and floaters. Interstitial keratitis presents as an orange-red discoloration of the cornea with increased tearing, pain, and decreased visual acuity.
