A 41-year-old refugee from Africa presented with seven months of recurrent painful oral ulcers. The ulcers were present prior to his arrival in the United States. The ulcers initially responded to oral corticosteroids but recurred one month after treatment. Associated symptoms included erythema, bleeding, dysphagia, odynophagia, anorexia, abdominal pain, and rectal bleeding. He had no fever or night sweats. He was treated for conjunctivitis and a nonpainful penile ulcer two weeks before presentation. His medical history was significant for hepatitis B with cirrhosis, treated syphilis, latent tuberculosis, Candida esophagitis, schistosomiasis, and rectal bleeding.
The patient was afebrile on physical examination. He had erythema and ulcers that involved the lips, tongue, and oropharynx with tender and friable mucosa (Figure 1). Immunofluorescence with enzyme-linked immunoreceptor assay was positive for desmoglein 1 and 3 antibodies.
FIGURE 1
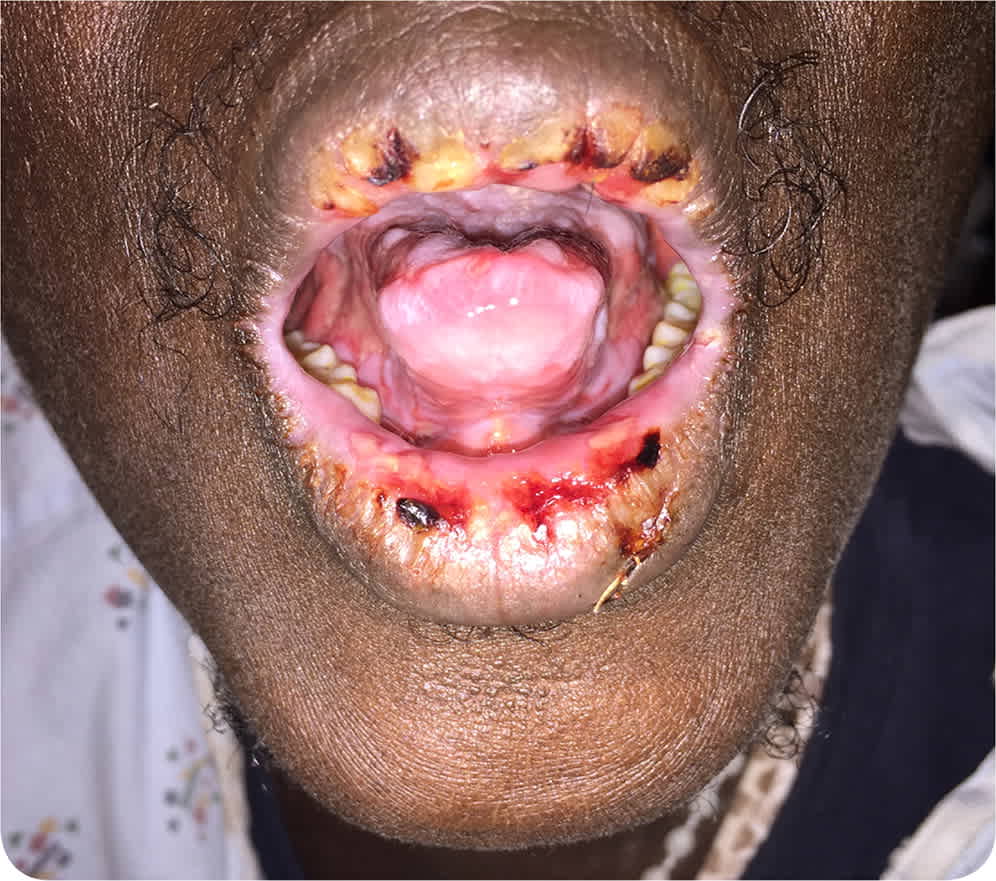
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Behçet disease.
B. Erythema multiforme.
C. Pemphigus vulgaris.
D. Recurrent aphthous stomatitis.
Discussion
The answer is C: pemphigus vulgaris. This rare and life-threatening blistering disease is caused by circulating autoantibodies against desmosomes. This results in cell-cell detachment (acantholysis) and development of intraepithelial blisters.1,2 The incidence of pemphigus vulgaris is approximately 0.1 to 0.5 per 1 million persons per year, with a higher incidence in individuals of Indian, Malaysian, Chinese, Japanese, Middle Eastern, or Jewish descent.3 It affects men and women equally, with an average age of onset between the fourth and sixth decades of life.3
Oral mucosal erosion is the most common initial manifestation of pemphigus vulgaris, occuring in 80% of patients with the disease. It can also involve the eyes and genital area, causing conjunctivitis and genital ulcers.3 Diagnosis is confirmed with direct immunofluorescence microscopy demonstrating autoantibodies against desmoglein 1 and 3. Serum can also be tested for circulating autoantibodies against the same antigens.1 Corticosteroids and immunosuppressants, such as azathioprine (Imuran) or cyclophosphamide, are used for initial treatment.4 Intravenous immune globulin has been shown to be an effective alternative therapy. Triggers include emotional stress, use of medications containing thiol or phenol, exposure to spicy or hot foods or beverages, and sunburns. Coexisting herpetic infections may trigger pemphigus in genetically susceptible individuals.2,4
Behçet disease is a multiorgan inflammatory disorder that manifests as recurrent oral and genital ulcers with cutaneous and ocular involvements. The etiology is unclear. Recurrent aphthous stomatitis occurs in 97% to 100% of patients with Behçet disease, and urogenital lesions occur in more than 70% of patients.5
Erythema multiforme is an acute, immune-mediated skin and mucosal disorder that is triggered by hypersensitivity to various drugs and infections.1 Target lesions appear on the palms, soles, and extensor surfaces of the extremities. Multiple large oral and mucosal ulcers may occur in severe cases.1
Recurrent aphthous stomatitis is a common condition presenting as recurrent small, tender, shallow, round ulcers with well-defined borders. The base of the ulcers is generally yellow to gray with surrounding erythema.6 The ulcers vary from 8 mm to more than 1 cm in diameter.5 Smaller lesions generally heal within 10 to 14 days without scarring. Larger ulcers can persist for up to six weeks and heal with scarring.6
SUMMARY TABLE
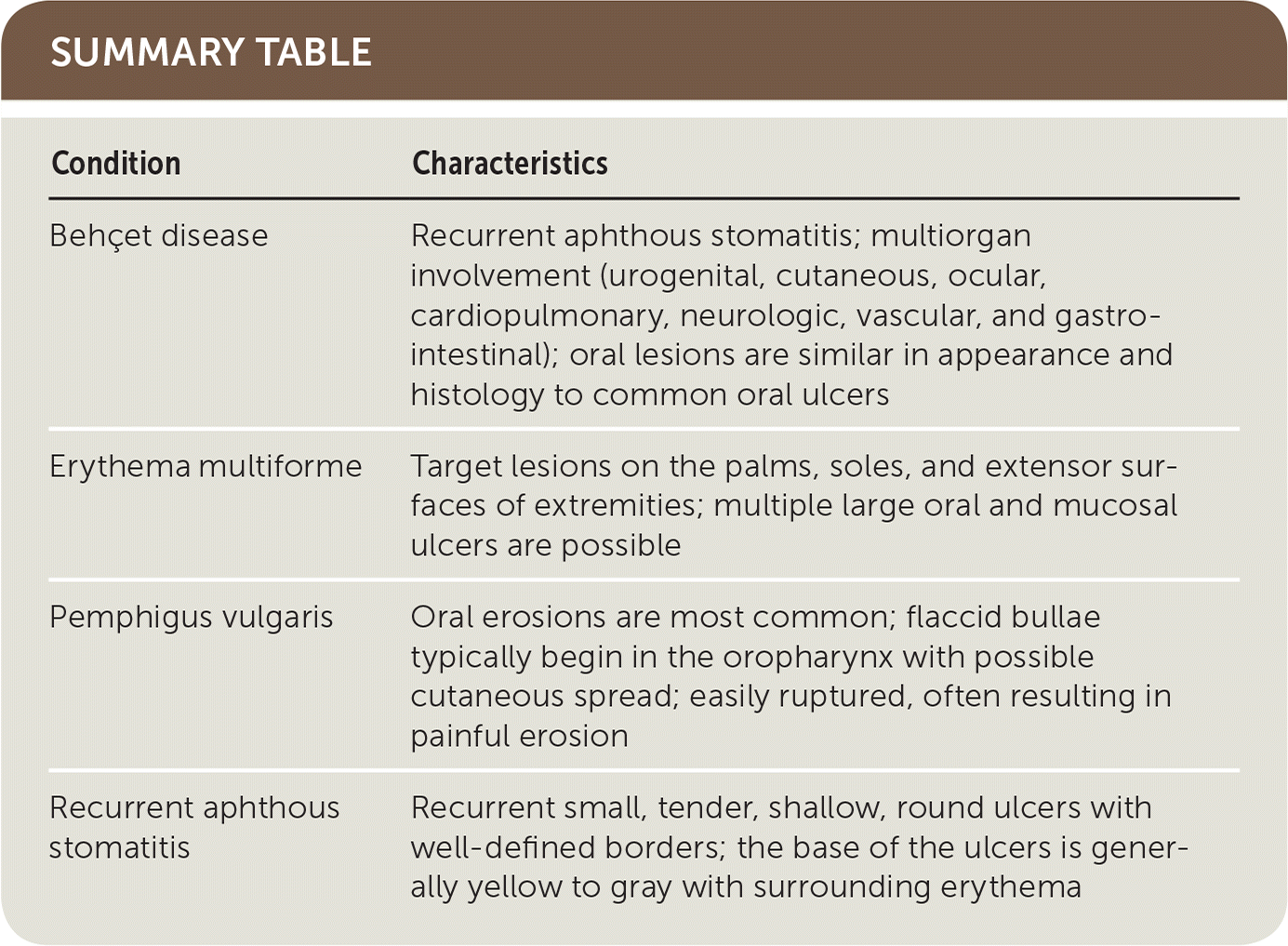
| Condition | Characteristics |
|---|---|
| Behçet disease | Recurrent aphthous stomatitis; multiorgan involvement (urogenital, cutaneous, ocular, cardiopulmonary, neurologic, vascular, and gastrointestinal); oral lesions are similar in appearance and histology to common oral ulcers |
| Erythema multiforme | Target lesions on the palms, soles, and extensor surfaces of extremities; multiple large oral and mucosal ulcers are possible |
| Pemphigus vulgaris | Oral erosions are most common; flaccid bullae typically begin in the oropharynx with possible cutaneous spread; easily ruptured, often resulting in painful erosion |
| Recurrent aphthous stomatitis | Recurrent small, tender, shallow, round ulcers with well-defined borders; the base of the ulcers is generally yellow to gray with surrounding erythema |
The authors thank Dr. Gary N. Elsasser for his guidance on the writing of the manuscript.

