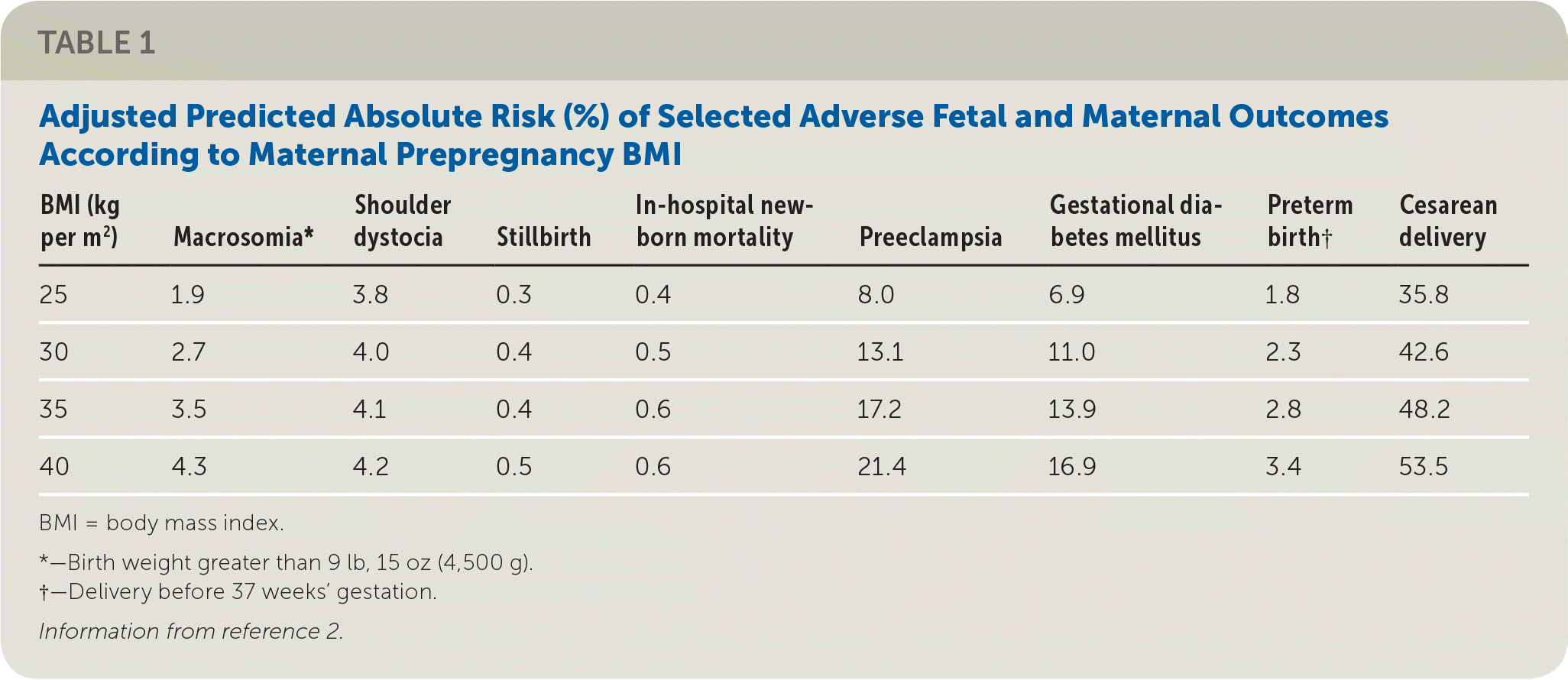
As obesity becomes more common, it is important for all maternity care clinicians to understand the risks and associated management of obesity in pregnancy. According to the National Health and Nutrition Examination Survey, 33.4% of women 20 to 34 years of age are obese (body mass index [BMI] of 30 kg per m2 or greater), and 58.4% are overweight (BMI of 25 kg per m2 or greater).1 Elevated prepregnancy weight increases the absolute risk of many adverse fetal and maternal outcomes (Table 12 ). Obesity during pregnancy also increases the odds of spontaneous and recurrent miscarriages, suboptimal ultrasound screening for fetal anomalies, congenital heart and neural tube defects, wound infections, maternal thromboembolic and anesthesia complications, depression, breastfeeding problems, and many other adverse outcomes.3 Mechanisms for these outcomes, the understanding of which is evolving, include changes in maternal hormone levels, altered gene expression, and fetal epigenetic modification.4
TABLE 1. Adjusted Predicted Absolute Risk (%) of Selected Adverse Fetal and Maternal Outcomes According to Maternal Prepregnancy BMI
| BMI (kg per m2) | Macrosomia* | Shoulder dystocia | Stillbirth | In-hospital newborn mortality | Preeclampsia | Gestational diabetes mellitus | Preterm birth† | Cesarean delivery |
|---|---|---|---|---|---|---|---|---|
| 25 | 1.9 | 3.8 | 0.3 | 0.4 | 8.0 | 6.9 | 1.8 | 35.8 |
| 30 | 2.7 | 4.0 | 0.4 | 0.5 | 13.1 | 11.0 | 2.3 | 42.6 |
| 35 | 3.5 | 4.1 | 0.4 | 0.6 | 17.2 | 13.9 | 2.8 | 48.2 |
| 40 | 4.3 | 4.2 | 0.5 | 0.6 | 21.4 | 16.9 | 3.4 | 53.5 |
BMI = body mass index.
*—Birth weight greater than 9 lb, 15 oz (4,500 g).
†—Delivery before 37 weeks' gestation.
Information from reference 2.
Interventions to Reduce Obesity in Pregnancy
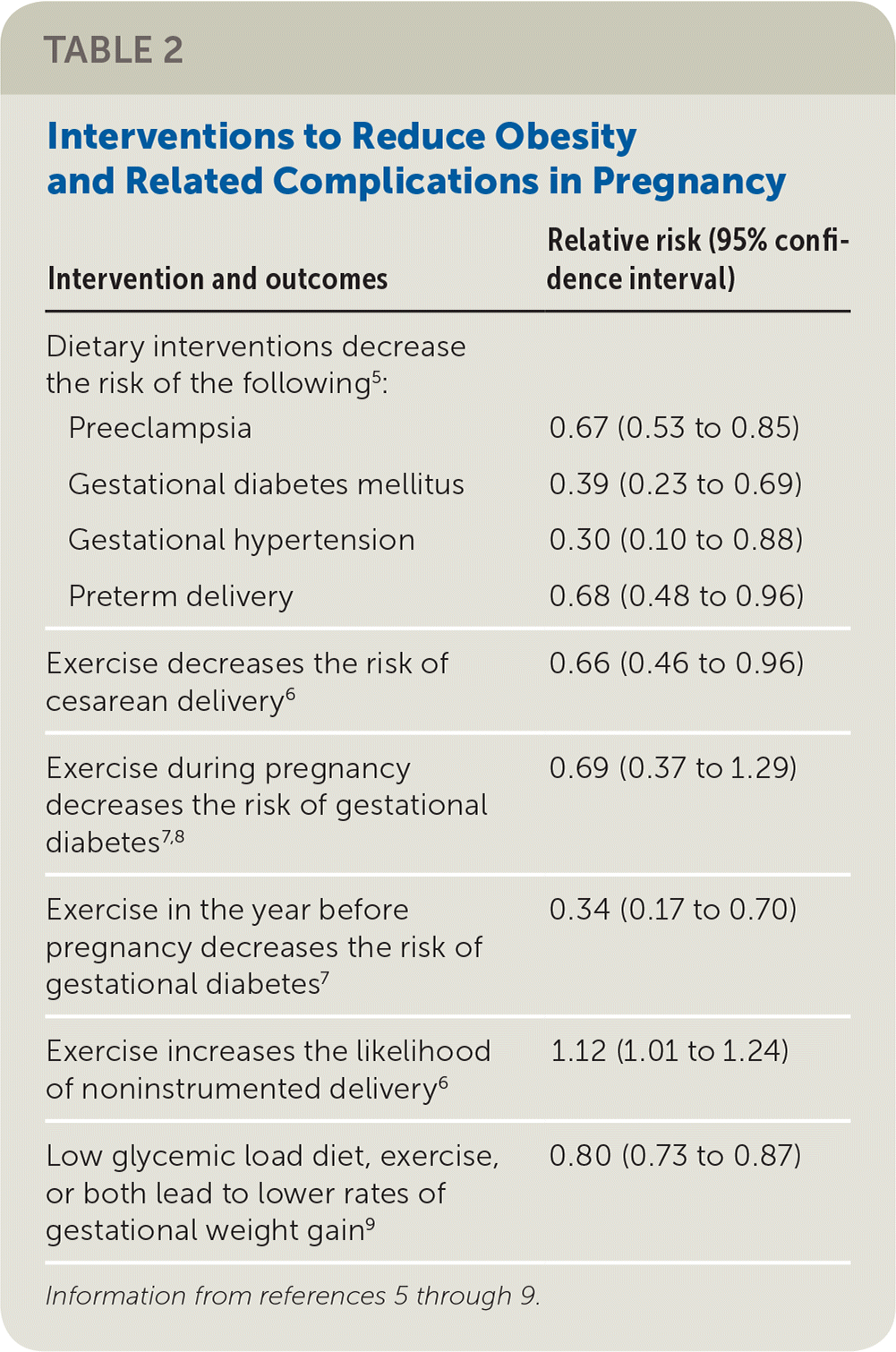
Weight loss before pregnancy is the most effective way to reduce maternal and fetal risks. Preconception counseling for overweight women should address the significant health risks associated with increased weight during pregnancy. Table 2 outlines interventions with limited data showing a reduction in the risk of complications from obesity in pregnancy.5–9
TABLE 2. Interventions to Reduce Obesity and Related Complications in Pregnancy
| Intervention and outcomes | Relative risk (95% confidence interval) | |
|---|---|---|
| Dietary interventions decrease the risk of the following5: | ||
| Preeclampsia | 0.67 (0.53 to 0.85) | |
| Gestational diabetes mellitus | 0.39 (0.23 to 0.69) | |
| Gestational hypertension | 0.30 (0.10 to 0.88) | |
| Preterm delivery | 0.68 (0.48 to 0.96) | |
| Exercise decreases the risk of cesarean delivery 6 | 0.66 (0.46 to 0.96) | |
| Exercise during pregnancy decreases the risk of gestational diabetes7,8 | 0.69 (0.37 to 1.29) | |
| Exercise in the year before pregnancy decreases the risk of gestational diabetes7 | 0.34 (0.17 to 0.70) | |
| Exercise increases the likelihood of noninstrumented delivery6 | 1.12 (1.01 to 1.24) | |
| Low glycemic load diet, exercise, or both lead to lower rates of gestational weight gain9 | 0.80 (0.73 to 0.87) | |
Guidance on optimal weight gain during pregnancy remains controversial. Since 2009, the Institute of Medicine has recommended a weight gain of 11 to 20 lb (4.95 to 9 kg) for women who are obese and 15 to 25 lb (6.8 to 11.25 kg) for women who are overweight.10 Based on meta-analyses noting an increased risk of infants being small for gestational age in women with inadequate weight gain during pregnancy, recent recommendations instruct women who are over-weight or obese to comply with the Institute of Medicine guidelines for gestational weight gain.4 However, more than one-half of women who are overweight or obese gain more than the recommended amount during pregnancy.7 Healthy diet and exercise are the mainstays of weight management. Clinicians can offer nutritional counseling or enlist help from a dietitian or behavioral health counselor to set up individual diet recommendations. Although there is no clearly superior diet for pregnant patients who are obese, two commonly recommended diets are a low glycemic load diet and a Mediterranean diet. Tools such as food diaries and pedometers may also help patients achieve successful weight management. Physicians should encourage a gradual increase in physical activity up to a goal of 30 minutes of moderate-intensity exercise daily.7
Bariatric surgery may be an option for patients who are planning to have children in the future. Infants born after surgery have better outcomes than siblings born before weight loss.7 However, patients are advised to avoid pregnancy for 12 to 18 months after bariatric surgery to reduce postoperative complications and to reduce fetal exposure to the rapid weight loss period. After bariatric surgery, patients should be evaluated for nutritional deficiencies and given routine supplementation with folate, iron, and vitamin B12 as needed.11
Obesity Management During Pregnancy and the Peripartum Period
In light of the increased risks for patients with BMIs greater than 30 kg per m2, physicians may consider additional testing beyond early glucose screening, such as measuring baseline 24-hour urine protein, creatinine, and transaminase levels, and performing questionnaire screening for obstructive sleep apnea. Detailed anatomy ultrasonography (administered at approximately 18 to 22 weeks' estimated gestational age for patients with BMIs greater than 35 kg per m2) and fetal echocardiography (for patients with BMIs greater than 40 kg per m2) may also be prudent, given the increased risk of cardiac anomalies in patients who are obese.
Because of the increased difficulty of administering regional and general anesthesia in pregnant patients who are obese, physicians should consider anesthesia consultation before admission for labor if the patient has obstructive sleep apnea or poorly controlled diabetes mellitus or hypertension, or if a difficult airway is anticipated. However, no specific ancillary preoperative tests are indicated. During the postpartum period, oxygen saturation should be closely monitored in women with obstructive sleep apnea, and narcotics should be used with caution to avoid respiratory depression.
For patients who are interested in a vaginal birth after cesarean, physicians must recognize that the success rate for trial of labor after cesarean is inversely related to body weight and, therefore, should consider the use of a vaginal birth after cesarean calculator when counseling patients who are overweight. An online calculator is available at https://mfmu.bsc.gwu.edu/PublicBSC/MFMU/VGBirthCalc/vagbirth.html.
Compounding the increased rates of cesarean deliveries and unsuccessful trials of labor after cesarean in women who are obese is a fourfold increased risk of thromboembolism and wound infections in these patients. The American College of Chest Physicians and the Royal College of Obstetricians and Gynaecologists have published guidelines to help clinicians estimate the risk of thrombosis and determine a risk-based approach to thromboprophylaxis in those who are obese.12,13
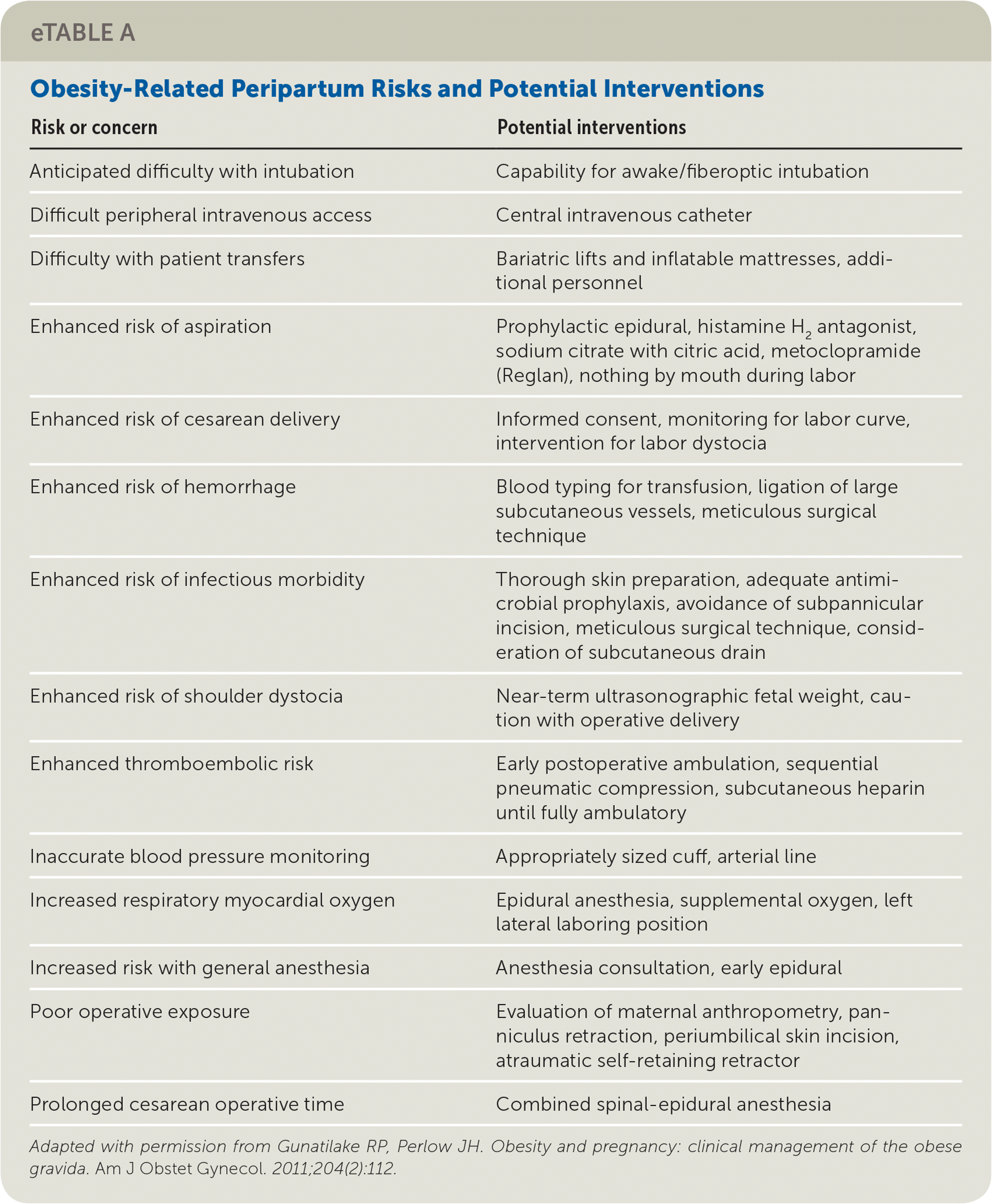
An overview of potential interventions to reduce peripartum risks for overweight and obese pregnant patients is shown in eTable A.
eTABLE A Obesity-Related Peripartum Risks and Potential Interventions
| Risk or concern | Potential interventions |
|---|---|
| Anticipated difficulty with intubation | Capability for awake/fiberoptic intubation |
| Difficult peripheral intravenous access | Central intravenous catheter |
| Difficulty with patient transfers | Bariatric lifts and inflatable mattresses, additional personnel |
| Enhanced risk of aspiration | Prophylactic epidural, histamine H2 antagonist, sodium citrate with citric acid, metoclopramide (Reglan), nothing by mouth during labor |
| Enhanced risk of cesarean delivery | Informed consent, monitoring for labor curve, intervention for labor dystocia |
| Enhanced risk of hemorrhage | Blood typing for transfusion, ligation of large subcutaneous vessels, meticulous surgical technique |
| Enhanced risk of infectious morbidity | Thorough skin preparation, adequate antimicrobial prophylaxis, avoidance of subpannicular incision, meticulous surgical technique, consideration of subcutaneous drain |
| Enhanced risk of shoulder dystocia | Near-term ultrasonographic fetal weight, caution with operative delivery |
| Enhanced thromboembolic risk | Early postoperative ambulation, sequential pneumatic compression, subcutaneous heparin until fully ambulatory |
| Inaccurate blood pressure monitoring | Appropriately sized cuff, arterial line |
| Increased respiratory myocardial oxygen | Epidural anesthesia, supplemental oxygen, left lateral laboring position |
| Increased risk with general anesthesia | Anesthesia consultation, early epidural |
| Poor operative exposure | Evaluation of maternal anthropometry, panniculus retraction, periumbilical skin incision, atraumatic self-retaining retractor |
| Prolonged cesarean operative time | Combined spinal-epidural anesthesia |
Adapted with permission from Gunatilake RP, Perlow JH. Obesity and pregnancy: clinical management of the obese gravida. Am J Obstet Gynecol. 2011;204(2):112.
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the U.S. Air Force Medical Department or the U.S. Air Force at large.

