
Am Fam Physician. 2018;97(9):603-604
Author disclosure: No relevant financial affiliations.
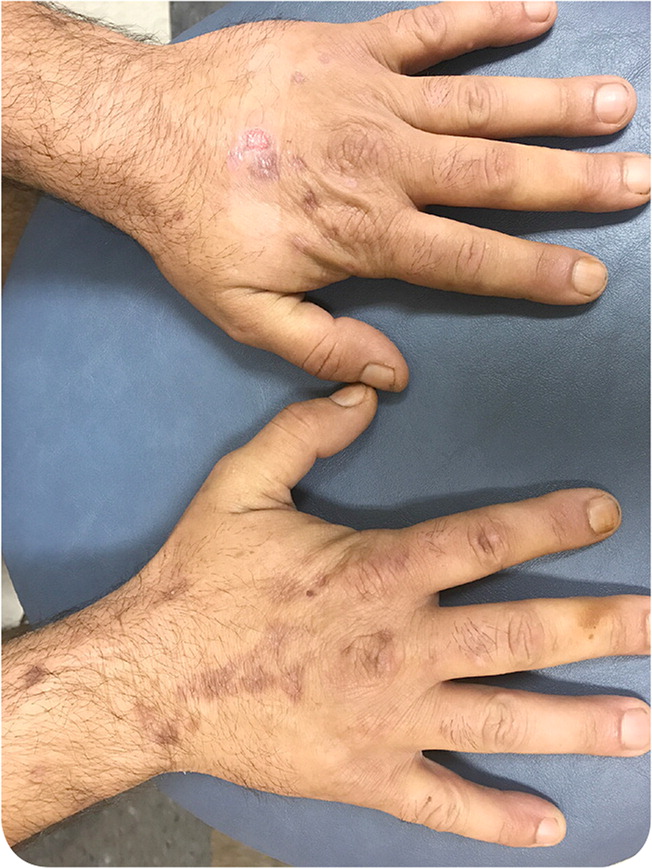
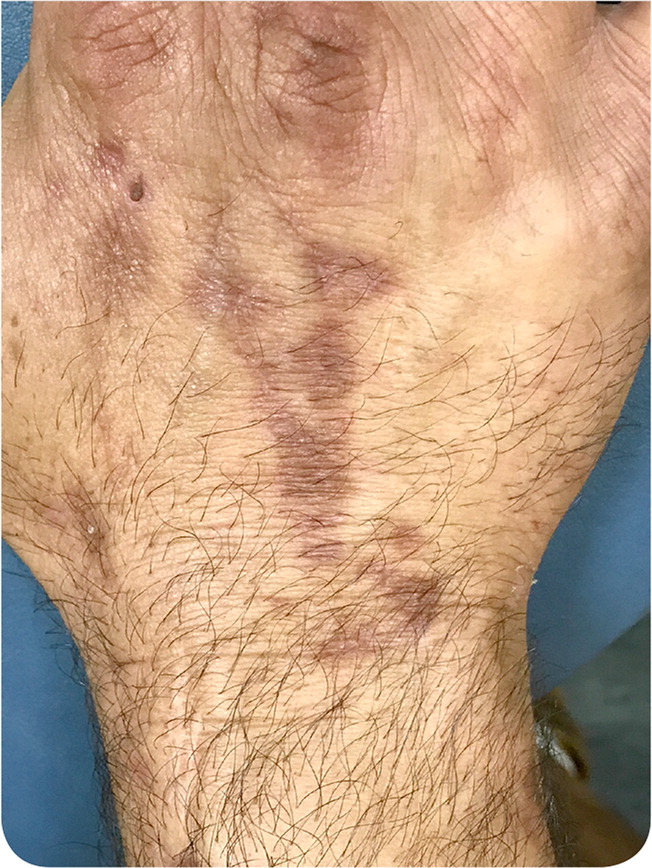
A 50-year-old man presented with skin lesions on his upper extremities (Figures 1 and 2) that developed two months earlier. He thought they may have appeared following a spider bite. The lesions were located primarily over the dorsal aspects of the hands and consisted of hyperpigmented patches with one visible erosion. The patches were painful but not pruritic.
The patient's medical history included human immunodeficiency virus (HIV) infection, type 2 diabetes mellitus, alcohol use disorder, and tobacco use disorder. He was not taking any medications, including nonsteroidal anti-inflammatory drugs.
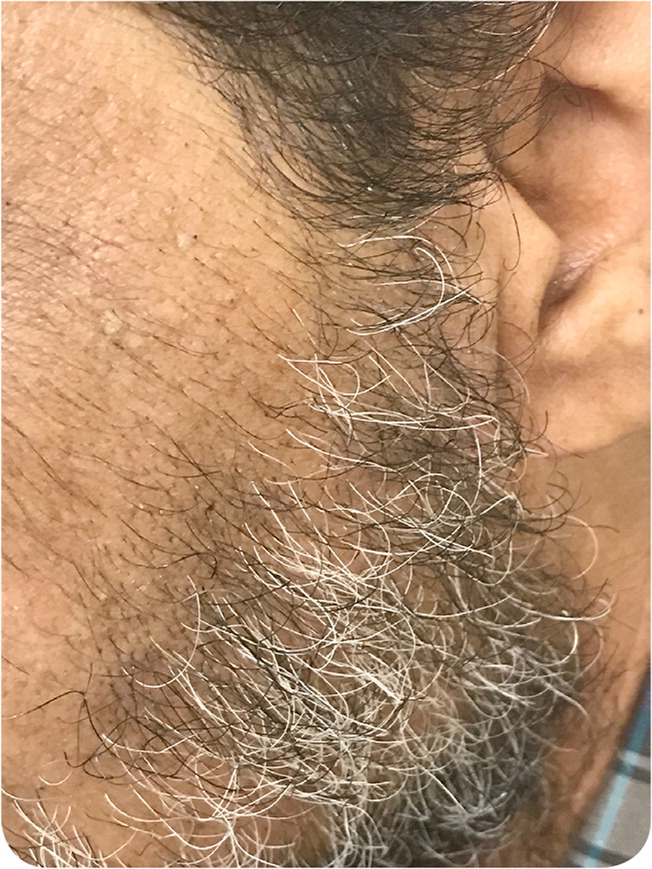
Physical examination revealed hyperpigmented patches on the malar region of the face with hypertrichosis (Figure 3). The patches were brownish and not raised.
Question
Discussion
The answer is C: porphyria cutanea tarda. Porphyria cutanea tarda is the most common type of porphyria and affects approximately one in 25,000 persons in the United States. It is a result of acquired inhibition of an enzyme (uroporphyrin decarboxylase or uroporphyrinogen decarboxylase) in the heme biosynthesis pathway of the liver.1,2 Porphyria cutanea tarda usually arises spontaneously, although accumulated iron, alcohol use, smoking, hepatitis C virus infection, excess estrogen exposure, and HIV infection are common inciting factors.
Reduced hepatic enzyme activity leads to accumulation of carboxylated porphyrinogens that are subsequently oxidized to photoactive porphyrins.3 Photodamage leads to the characteristic cutaneous features, including increased skin fragility, noninflammatory bullae and vesicles that scar, hyperpigmentation, and milia on sun-exposed areas.4 Increased fragility of the skin leads to erosions and blistering from trivial trauma, commonly on the hands.4 Hirsutism of the face and forearms is also a common finding, whereas sclerodermatous changes are less common.5
Skin biopsy is not necessary for diagnosis. Measuring total porphyrins in plasma or serum is the laboratory evaluation of choice for suspected disease; however, a spot urine sample showing porphyrins may also be used.4 Primary therapies for porphyria cutanea tarda include phlebotomy and low-dose hydroxychloroquine (Plaquenil).
Phytophotodermatitis is an ultraviolet A–induced contact dermatitis manifesting as linear- or bizarre-shaped erythematous patches. It is most commonly caused by photosensitizing compounds found in fruits, vegetables, and other plants.8 It is sometimes referred to as “lime disease” because of the rash it can cause on the hands of bartenders who handle limes.
Pseudoporphyria presents as photodistributed fragile skin and noninflammatory bullae and vesicles, which is clinically similar to porphyria cutanea tarda. However, porphyrin abnormalities will not be observed on serum and urine testing.1
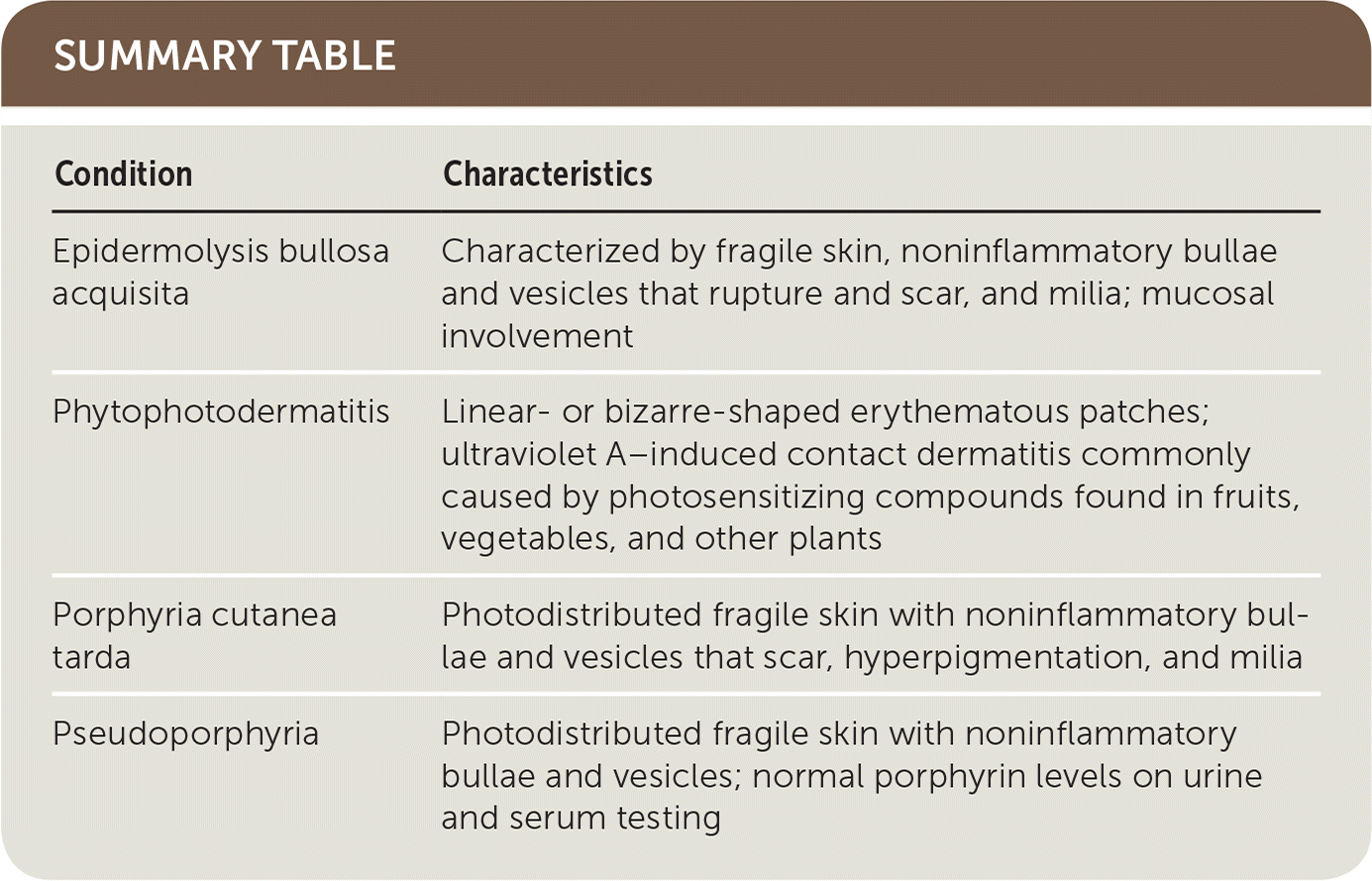
| Condition | Characteristics |
|---|---|
| Epidermolysis bullosa acquisita | Characterized by fragile skin, noninflammatory bullae and vesicles that rupture and scar, and milia; mucosal involvement |
| Phytophotodermatitis | Linear- or bizarre-shaped erythematous patches; ultraviolet A–induced contact dermatitis commonly caused by photosensitizing compounds found in fruits, vegetables, and other plants |
| Porphyria cutanea tarda | Photodistributed fragile skin with noninflammatory bullae and vesicles that scar, hyperpigmentation, and milia |
| Pseudoporphyria | Photodistributed fragile skin with noninflammatory bullae and vesicles; normal porphyrin levels on urine and serum testing |
