Clinical Question
What is the best approach to evaluate patients with suspected pulmonary embolism (PE) in the outpatient primary care setting?
Evidence Summary
Acute PE accounts for one out of 400 to 1,500 adult presentations to the emergency department,1 with a 30-day mortality rate of 5.4%.2 Chronic thromboembolic pulmonary hypertension further adds to morbidity in 4.8% of patients who survive PE.3 However, PE has a highly variable presentation.
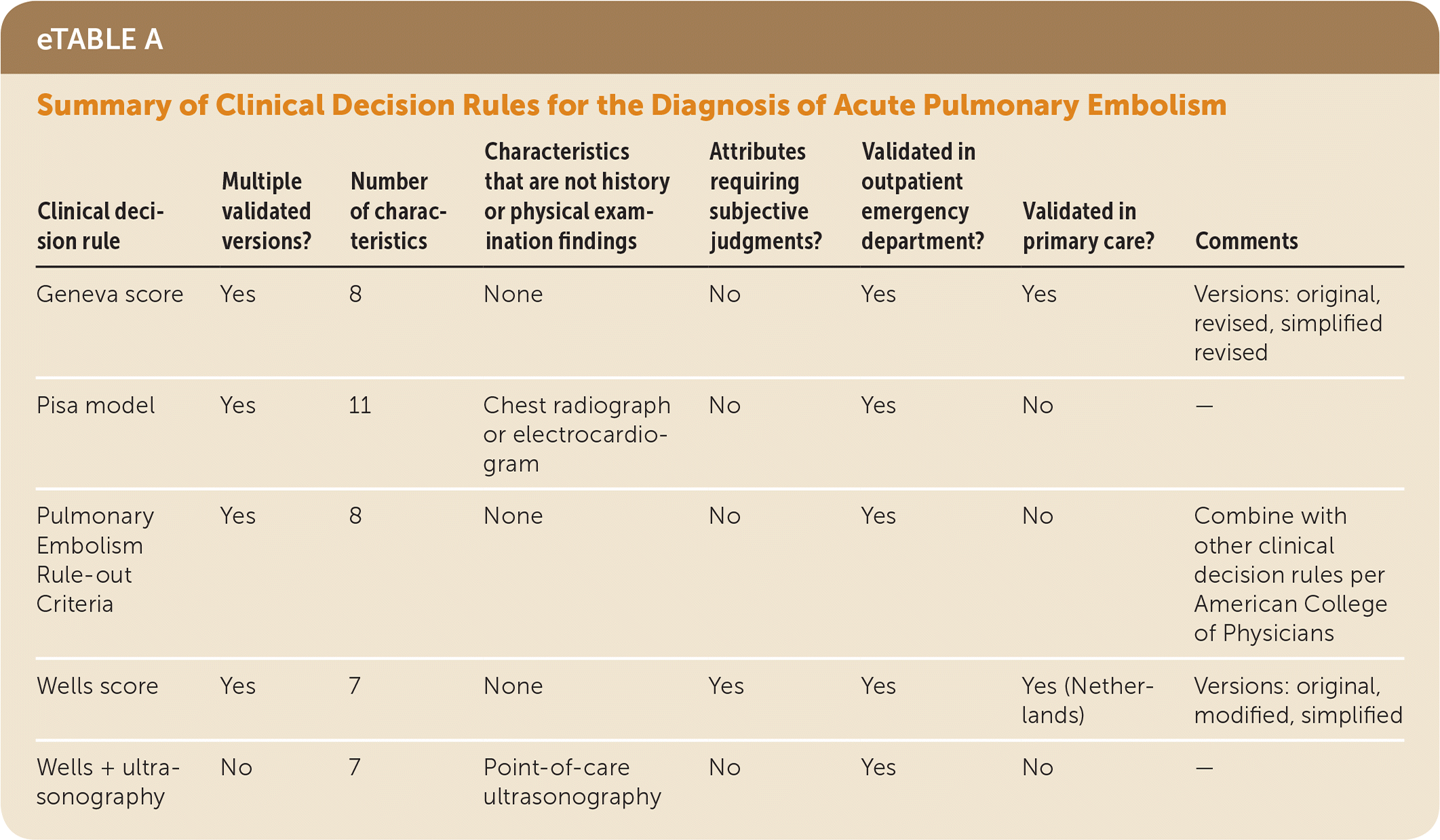
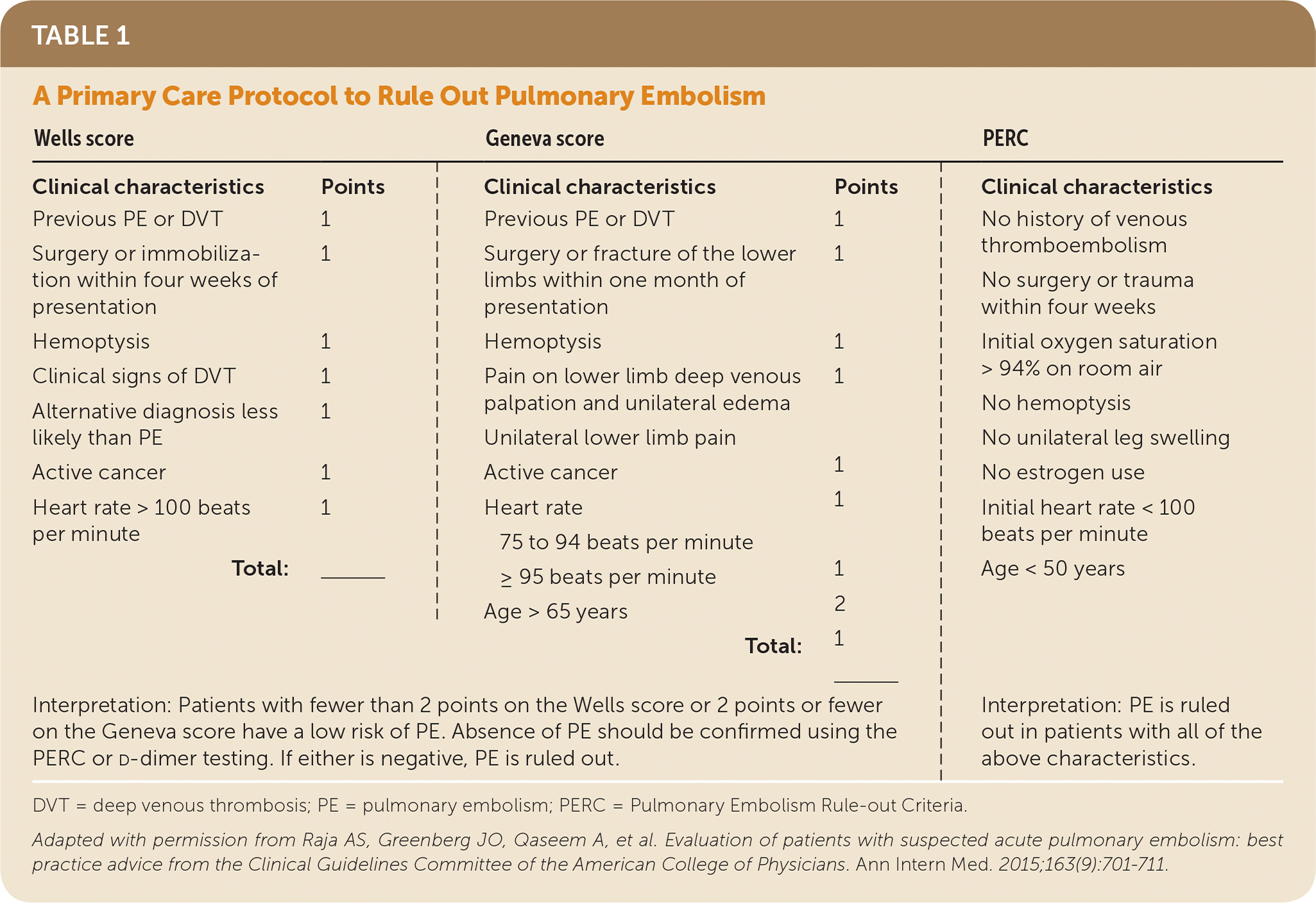
Many clinical decision rules exist to estimate the patient's risk level based on certain clinical characteristics and subsequently guide the evaluation of suspected PE. These include the Wells score, Geneva score, Pisa model, and Pulmonary Embolism Rule-out Criteria (PERC). Each of the rules has advantages and disadvantages (eTable A). A primary care protocol that uses three of these rules to rule out PE is presented in Table 1.4
eTABLE A Summary of Clinical Decision Rules for the Diagnosis of Acute Pulmonary Embolism
| Clinical decision rule | Multiple validated versions? | Number of characteristics | Characteristics that are not history or physical examination findings | Attributes requiring subjective judgments? | Validated in outpatient emergency department? | Validated in primary care? | Comments |
|---|---|---|---|---|---|---|---|
| Geneva score | Yes | 8 | None | No | Yes | Yes | Versions: original, revised, simplified revised |
| Pisa model | Yes | 11 | Chest radiograph or electrocardiogram | No | Yes | No | — |
| Pulmonary Embolism Rule-out Criteria | Yes | 8 | None | No | Yes | No | Combine with other clinical decision rules per American College of Physicians |
| Wells score | Yes | 7 | None | Yes | Yes | Yes (Netherlands) | Versions: original, modified, simplified |
| Wells + ultrasonography | No | 7 | Point-of-care ultrasonography | No | Yes | No | — |
TABLE 1. A Primary Care Protocol to Rule Out Pulmonary Embolism
| Wells score | Geneva score | PERC | ||
|---|---|---|---|---|
| Clinical characteristics | Points | Clinical characteristics | Points | Clinical characteristics |
| Previous PE or DVT | 1 | Previous PE or DVT | 1 | No history of venous thromboembolism |
| Surgery or immobilization within four weeks of presentation | 1 | Surgery or fracture of the lower limbs within one month of presentation | 1 | No surgery or trauma within four weeks |
| Hemoptysis | 1 | Hemoptysis | 1 | Initial oxygen saturation > 94% on room air |
| Clinical signs of DVT | 1 | Pain on lower limb deep venous palpation and unilateral edema | 1 | No hemoptysis |
| Alternative diagnosis less likely than PE | 1 | Unilateral lower limb pain | 1 | No unilateral leg swelling |
| Active cancer | 1 | Active cancer | 1 | No estrogen use |
| Heart rate > 100 beats per minute | 1 | Heart rate | Initial heart rate < 100 beats per minute | |
| Total: | ______ | 75 to 94 beats per minute | 1 | |
| ≥ 95 beats per minute | 2 | Age < 50 years | ||
| Age > 65 years | 1 | |||
| Total: | ______ | |||
| Interpretation: Patients with fewer than 2 points on the Wells score or 2 points or fewer on the Geneva score have a low risk of PE. Absence of PE should be confirmed using the PERC or | Interpretation: PE is ruled out in patients with all of the above characteristics. | |||
DVT = deep venous thrombosis; PE = pulmonary embolism; PERC = Pulmonary Embolism Rule-out Criteria.
Adapted with permission from Raja AS, Greenberg JO, Qaseem A, et al. Evaluation of patients with suspected acute pulmonary embolism: best practice advice from the Clinical Guidelines Committee of the American College of Physicians. Ann Intern Med. 2015;163(9):701–711.
The Wells score consists of seven characteristics based on the history and physical examination, forgoing the need for additional testing.5 However, the Wells score incorporates a subjective judgment: an estimate of the probability of PE and whether it is more or less likely than an alternative diagnosis. Each characteristic is assigned a point value, and the cumulative score places patients into risk categories that guide further testing.6 There are several versions of the Wells score. The original, modified, and simplified versions are most commonly used, and each assigns different point values for the characteristics and have two or three risk categories.5,7 A recent study examining the use of point-of-care ultrasonography of the lung and lower extremities in 446 emergency department patients found that it improved the accuracy of the Wells score compared with the Wells score alone.8
The Geneva score consists of eight objective characteristics, eliminating the physician's subjective judgment. Like the Wells score, each characteristic is assigned a point value, and the cumulative score stratifies patients into different risk categories. There are several versions of the Geneva score (the original, revised, and simplified revised), adjusting point values and risk categories to alter performance.
The PERC consists of eight characteristics. In a study of 61,322 patients in an urban emergency department, those with none of the characteristics had a less than 1% likelihood of PE.9 The Pisa model consists of 11 characteristics but requires an electrocardiogram or a chest radiograph, depending on the version.10,11
All of these clinical decision rules were originally validated in an emergency department and/or tertiary care referral center. Differences in the prevalence of PE may limit their use (or alter their interpretation) in a primary care setting. Only the Wells and Geneva scores have been studied specifically in primary care, making them the preferred clinical decision rules in this setting.
With multiple versions of a clinical decision rule, it is important to correlate the point values with the correct version of risk strata to properly assess a patient's likelihood of PE.
A study comparing different versions of the Geneva and Wells scores in a prospective cohort of inpatients and outpatients found that all versions were similar in performance.12 A meta-analysis of 12 studies including 3,613 inpatients and outpatients from emergency departments concluded that the original Wells score was more accurate and effective than the revised Geneva score.13 A Dutch study of 662 patients is the only validation study in the primary care setting. The study found that although the Wells and Geneva scores had similar discrimination as measured by the area under the receiver operating characteristic curve, the Wells score classified fewer patients with PE into the low-risk category (1.98% difference between the simplified Wells score and the simplified revised Geneva score).14 When used as a clinical decision rule to assess pretest probability, this characteristic is most important.
The American College of Physicians Best Practice Advice recommends a clinical decision rule be used first to estimate pretest probability for acute PE. If the pretest probability is low and the PERC rule score is 0, then it is reasonable to forgo other testing, including checking d-dimer.4
Applying the Evidence
A 49-year-old man presents to your office with increasing shortness of breath that began two days ago. He has a productive cough but no hemoptysis. He does not have a history of deep venous thrombosis or PE episodes, recent surgeries, fractures or prolonged periods of immobilization, or cancer. He has a 30-pack-year smoking history but has never had pulmonary function testing. He has no sick contacts and does not have fever, chills, or other signs or symptoms suggesting pneumonia. On examination, he has no lower extremity swelling or pain, Homans sign is negative, and his pulse is 92 beats per minute. His pulse oxygen level is 97% on room air.
He receives 0 points on the simplified Wells score; therefore, PE is a less likely diagnosis than chronic obstructive pulmonary disease. He receives 1 point on the simplified revised Geneva score. Based on these scores, the patient has a low pretest probability of PE. The PERC rules out PE. It would be reasonable to forgo any further testing for PE.4

