Food security is defined as access by all persons at all times to enough food for an active, healthy life. Limited availability of nutritionally adequate and safe food or the inability to acquire these foods in socially acceptable ways is called food insecurity (FI).1
Prior to the Great Recession (2007 to 2009), the rate of FI was 11.1%; FI peaked at 14.9% in 2011 before declining to 12.3% (almost 16 million American households) in 2016.2 FI occurs most often in households with income near or below the federal poverty line or with a person living alone, in households containing children, or in households headed by a black or Hispanic person or single parent. In addition, the prevalence of FI is higher among those living in principal cities of metropolitan areas (14.2%) or in rural areas (15.0%), with the highest prevalence occurring in the South (13.5%), followed by the Midwest (12.2%), the West (11.5%), and the Northeast (10.8%).2
The interaction between FI and chronic disease is cyclical. FI results in constrained dietary options and compensatory strategies, as well as competing demands for limited resources (e.g., postponement of needed health care). Changes in health status and stress from FI can result in development and progression of chronic diseases, causing further competing demands that exacerbate FI.3 Obesity is associated with FI, especially in women and in persons with diabetes mellitus, hypertension, dyslipidemia, or depression.4–10 Adults with very low food security have a higher 10-year risk of cardiovascular events than those with traditional risk factors.11 In children and adolescents, FI increases the risks of hypertension, asthma, obesity, poor nutrition, infection, anemia, untreated dental caries, poorly developed social-emotional skills (in young children), poor academic achievement, and behavioral problems (in adolescent males).12
Physicians can improve the health of patients who experience FI by following the SEARCH (screen, educate, adjust, recognize, connect, help) mnemonic13 and by using the resources outlined in Table 1.
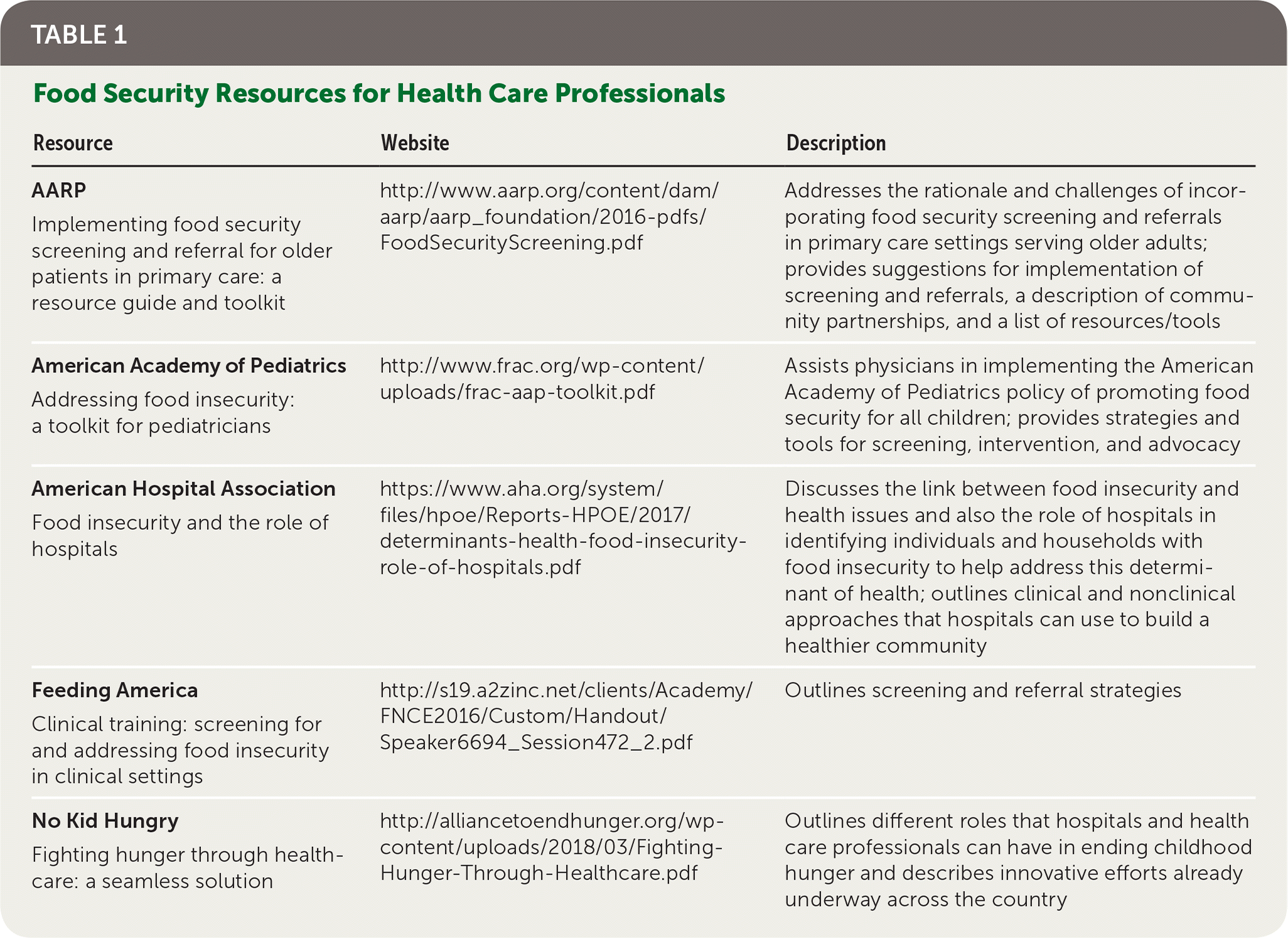
TABLE 1. Food Security Resources for Health Care Professionals
| Resource | Website | Description |
|---|---|---|
| AARP Implementing food security screening and referral for older patients in primary care: a resource guide and toolkit | http://www.aarp.org/content/dam/aarp/aarp_foundation/2016-pdfs/FoodSecurityScreening.pdf | Addresses the rationale and challenges of incorporating food security screening and referrals in primary care settings serving older adults; provides suggestions for implementation of screening and referrals, a description of community partnerships, and a list of resources/tools |
| American Academy of Pediatrics Addressing food insecurity: a toolkit for pediatricians | http://www.frac.org/wp-content/uploads/frac-aap-toolkit.pdf | Assists physicians in implementing the American Academy of Pediatrics policy of promoting food security for all children; provides strategies and tools for screening, intervention, and advocacy |
| American Hospital Association Food insecurity and the role of hospitals | https://www.aha.org/system/files/hpoe/Reports-HPOE/2017/determinants-health-food-insecurity-role-of-hospitals.pdf | Discusses the link between food insecurity and health issues and also the role of hospitals in identifying individuals and households with food insecurity to help address this determinant of health; outlines clinical and nonclinical approaches that hospitals can use to build a healthier community |
| Feeding America Clinical training: screening for and addressing food insecurity in clinical settings | http://s19.a2zinc.net/clients/Academy/FNCE2016/Custom/Handout/Speaker6694_Session472_2.pdf | Outlines screening and referral strategies |
| No Kid Hungry Fighting hunger through health-care: a seamless solution | http://alliancetoendhunger.org/wp-content/uploads/2018/03/Fighting-Hunger-Through-Healthcare.pdf | Outlines different roles that hospitals and health care professionals can have in ending childhood hunger and describes innovative efforts already underway across the country |
Screen
Screen all patients for FI, especially in practices that serve at-risk populations, and document findings in the electronic health record. Although the preferred screening tool for FI is an 18-item survey, two questions have been identified that can quickly assess for FI.14,15 An affirmative response (“often true” or “sometimes true” vs. “never true”) to either of the following statements can identify FI with 97% sensitivity and 83% specificity: (1) Within the past 12 months we worried whether our food would run out before we got money to buy more, and (2) Within the past 12 months the food we bought just didn't last, and we didn't have money to get more.15 Screening could be completed during the intake process so that physicians can focus their time on helping patients who screen positive.16
Educate
Educate patients at risk of FI about appropriate coping strategies. Although some individuals with limited resources manage without major disruptions to food intake, many eat less or eat less healthy foods to get by. Physicians can help patients avoid other unhealthy coping strategies such as prioritizing food quantity over quality; stretching or diluting food and beverages; avoiding medical care or filling prescriptions; eating one large, highly satiating meal per day; choosing a small variety of low-cost or fast foods; fasting or skipping meals; and overeating when food is available. Some individuals may go to the emergency department to obtain food or may commit a petty crime to get a jail meal.13
Educate patients with diabetes who are at increased risk of hypoglycemia to coordinate hypoglycemic medications (e.g., sulfonylureas, prandial insulin) with meals rather than time of day. Patients should avoid taking these medications if they are not going to eat a meal, no matter the reason. Educate patients with hypertension or heart disease about sodium restriction because sodium levels may be higher in prepackaged donated food or low-cost fast food.
Adjust
Adjust the patient's medication if it should be taken with food. Prescribe medications that minimize the likelihood of hypoglycemia for patients with FI who have diabetes.13 Hypoglycemia may occur more often toward the end of the month because of the lack of financial resources to buy food.17
A physician or registered dietitian nutritionist can help patients adjust meal plans and timing of meals to reduce negative interactions between the patient's diet and prescribed medications for chronic conditions.18 Prescribe medications that are effective and affordable and that promote optimal adherence.
Recognize
Recognize that FI is typically recurrent but is usually not chronic. Patients should be screened at each visit to ensure appropriate evaluation and management of intermittent or recurrent FI.
Connect
Connect patients with assistance programs and encourage patients with FI to use food banks. See eTable A for more information on available programs.
eTABLE A Food Assistance Programs
| Program | Website | Description |
|---|---|---|
| Child and Adult Care Food Program | http://www.fns.usda.gov/cacfp/cacfp-contacts | Provides aid for nutritious meals and snacks for children who attend day care or after-school care or who reside in homeless shelters and for adults who are chronically impaired or disabled and who attend an adult day care; usually administered by the state education agency |
| Expanded Food and Nutrition Education Program | https://nifa.usda.gov/program/expanded-food-and-nutrition-education-program-efnep | Helps families and youth with limited resources acquire the knowledge, behavioral skills, and attitudes necessary to maintain nutritionally sound diets and to enhance personal development (e.g., education on basic nutrition, food preparation, and resource management) |
| Food Distribution Programs: governmental, volunteer, and emergency assistance | http://www.fns.usda.gov/fdd | Supports the nutrition safety net through commodity distribution and other nutritional assistance to low-income families, older adults, emergency feeding programs, and American Indian reservations; patients are referred to local food banks/pantries, faith-based groups, and other agencies/organizations where supplemental food is distributed (local food banks can be found at http://www.feedingamerica.org) |
| Meals on Wheels America Foundation | http://www.mealsonwheelsamerica.org | Provides meal delivery to older adults; programs are organized by local groups, including communities, churches, charitable organizations, and citizens; the local Area Agency on Aging may be a helpful resource when locating a local program |
| National School Lunch Program and School Breakfast Program | http://www.fns.usda.gov/cnd/lunch/default.htm http://www.fns.usda.gov/sbp/school-breakfast-program-sbp | Provides low-cost or free lunch and breakfast (consistent with the Dietary Guidelines for Americans) to students enrolled in public schools, nonprofit private schools, and residential child care centers; provides snacks served in after-school educational and enrichment programs; patients are referred to local schools to enroll (information about eligibility is available at http://www.fns.usda.gov/school-meals/income-eligibility-guidelines) |
| Senior Farmers' Market Nutrition Program | http://www.fns.usda.gov/wic/seniorFMNP/SFMNPmenu.htm | Provides low-income older adults with coupons that can be exchanged for eligible fresh foods at farmers markets, roadside stands, and community-supported agriculture programs (information on eligibility is available at https://www.fns.usda.gov/sfmnp/sfmnp-income-guidelines) |
| Special Supplemental Nutrition Program for Women, Infants, and Children and Women, Infants, and Children Farmers' Market Nutrition Program | http://www.fns.usda.gov/wic http://www.fns.usda.gov/wic/FMNP/FMNPfaqs.htm | Provides supplemental foods, nutrition education and counseling, and access to health services to low-income pregnant and postpartum women and to infants and children up to five years of age who are found to be at nutritional risk; the farmers market program provides coupons that can be exchanged for eligible fresh, nutritious foods (information on eligibility is available at https://www.fns.usda.gov/wic/wic-how-apply) |
| Summer Food Service Program | https://www.fns.usda.gov/sfsp/summer-food-service-program | Provides nutritious breakfasts, lunches, and snacks to children during long school breaks when they do not have access to school lunch or breakfast; patients are referred to local summer programs; schools or the local food bank may also have information about available programs (information on eligibility is available at https://www.fns.usda.gov/school-meals/income-eligibility-guidelines) |
| Supplemental Nutrition Assistance Program (formerly Food Stamp Program) | http://www.fns.usda.gov/snap | Enables low-income families to buy eligible nutritious food at authorized stores and farmers markets using coupons and electronic benefits transfer cards |
Adapted with permission from Holben DH, Myles W. Food insecurity in the United States: its effect on our patients. Am Fam Physician. 2004;69(5):1060.
Help
Help other health care professionals recognize that poor health and FI often exacerbate one another. Addressing FI during medical education enables faculty and trainees to understand the role of FI in population health and to propose solutions.19 Physicians should advocate for food security resources in clinics, hospitals, and communities (Table 1).

