When I was diagnosed with stage IV terminal lung cancer, my primary care doctor gave me the news. His compassion created a pathway of healing that has sustained me for more than seven years.
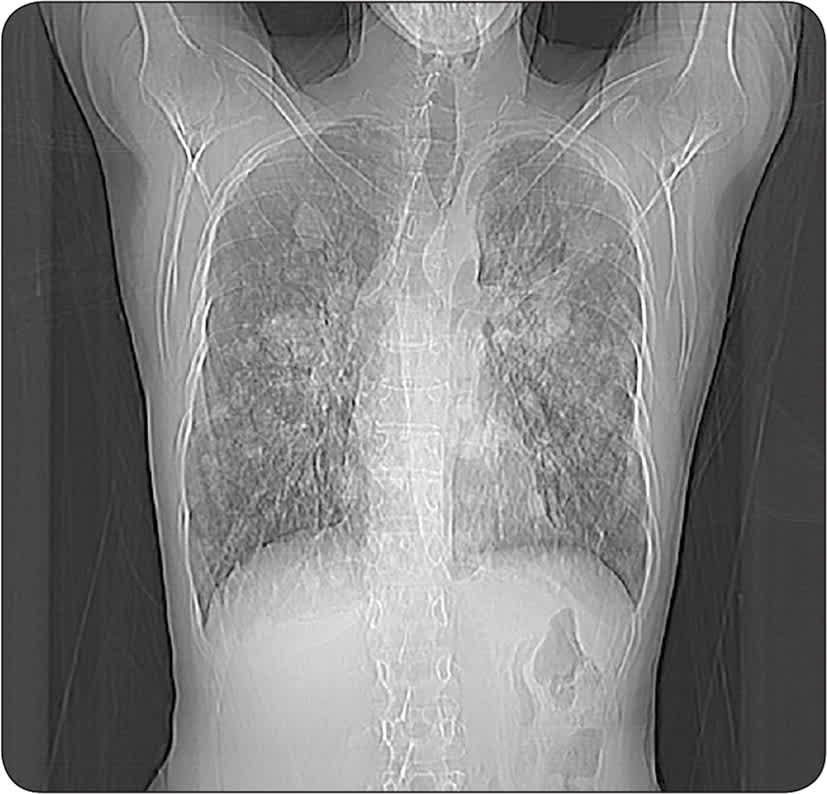
Shortly after my diagnosis, I had a set of scans. One concern was the condition of my lung: had it sufficiently re-expanded so that I could safely fly to see loved ones? When I turned to my oncologist, she said I had to wait eight days for the scan results. The surgeon also had protocols that prevented him from sharing information with me. Frantic, more about my trapped lung than the cancer, I turned to my primary care physician. Without hesitation he said over the phone, “Let's open your scan right now.” Not only was I safe to fly, my tumors were smaller after targeted therapy.
Soon afterward, my oncologist called to say, “Your primary care doctor should not have given you that information, and I am going to speak to him.” Her anger triggered a stress response in me—hardly a situation conducive to optimal well-being. I was worried that my doctor was in trouble for helping me. But, when I saw him later and apologized for causing him hardship, he asked warmly, “How could you have caused me hardship?”
After having problems with several oncologists, I asked my primary care physician to assume my cancer treatment. Although the cancer center asserted that only oncologists can prescribe targeted therapy, my doctor took the matter to the chief of medicine, and he was allowed to treat my cancer. Because of his courage, I am thriving. Primary care doctors can take a holistic view of treatment, and this in itself is life-changing and life-saving. —N.W.
Commentary
N.W.'s story highlights what has changed within the practice of medicine, as well as what has remained the same.
First, the changes. Access to technology and data now allows physicians in an ambulatory office miles from the hospital to receive, in real time, images and radiologic interpretations. To avoid confusion, misunderstanding, or miscommunication of information, it is important to have protocols and expectations for sharing data among physicians and between physicians and their patients.
Another core evolution of primary care relates to chronic disease. Thirty years ago, metastatic non–small cell lung cancer was managed as an acute illness by a subspecialist within the walls of a hospital. Today, with the advent of tyrosine kinase inhibitors, metastatic non–small cell lung cancer can be managed as a chronic illness in a small subset of patients. Medical treatments and modalities are advancing rapidly. Over the next several decades it may very well become appropriate for new complex chronic illnesses to be comanaged with primary care physicians. With support, this can become a source of professional satisfaction for physicians and a value to the health care system overall.
So, what has remained unchanged? The patient-physician relationship! I decided to manage my patient's treatment because of our long-standing relationship, my knowledge of her as a person, and our mutual sense of trust. That is part of being a primary care physician. I took this step only after weighing all other options and having extensive conversations with the patient and her former oncologist. Technology and the nature of illness will change over time. The value of our relationship with patients will always remain the same.

