Clinical Question
Are lower blood pressure (BP) targets for patients with hypertension and a history of cardiovascular disease associated with decreased morbidity and mortality?
Evidence-Based Answer
Achieving a target BP of 135/85 mm Hg or less does not decrease the risk of total cardiovascular events vs. treating to a target of 140 to 160/90 to 100 mm Hg. Further, treating to the lower BP target does not improve total mortality, cardiovascular mortality, or serious adverse effects. More patients discontinue treatment because of adverse effects when treated to the lower BP target.1 (Strength of Recommendation: B, based on inconsistent or limited-quality patient-oriented evidence.)
SUMMARY TABLE: STANDARD VS. LOWER BP TARGETS IN PATIENTS WITH HYPERTENSION AND CARDIOVASCULAR DISEASE
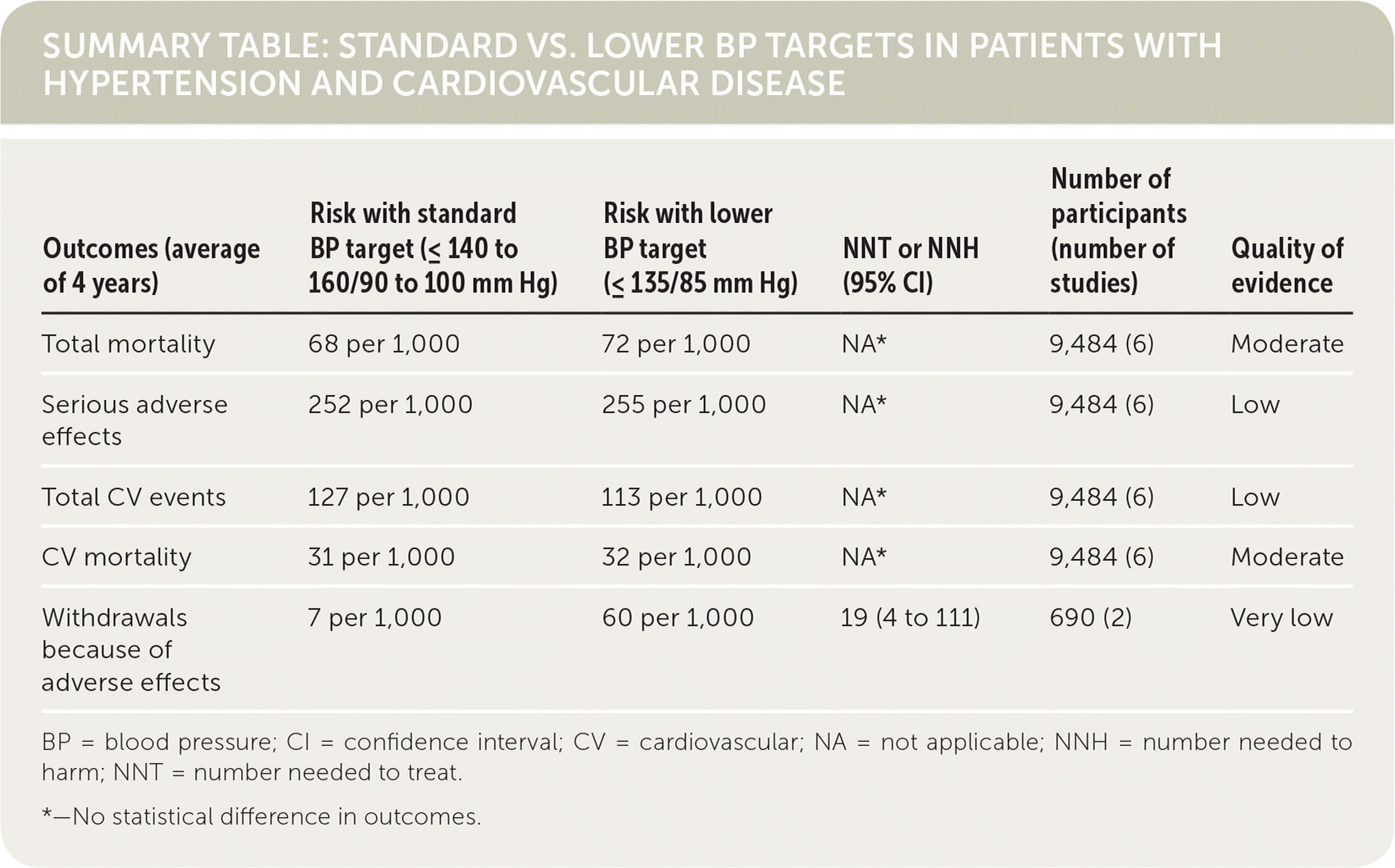
| Outcomes (average of 4 years) | Risk with standard BP target (≤ 140 to 160/90 to 100 mm Hg) | Risk with lower BP target (≤ 135/85 mm Hg) | NNT or NNH (95% CI) | Number of participants (number of studies) | Quality of evidence |
|---|---|---|---|---|---|
| Total mortality | 68 per 1,000 | 72 per 1,000 | NA* | 9,484 (6) | Moderate |
| Serious adverse effects | 252 per 1,000 | 255 per 1,000 | NA* | 9,484 (6) | Low |
| Total CV events | 127 per 1,000 | 113 per 1,000 | NA* | 9,484 (6) | Low |
| CV mortality | 31 per 1,000 | 32 per 1,000 | NA* | 9,484 (6) | Moderate |
| Withdrawals because of adverse effects | 7 per 1,000 | 60 per 1,000 | 19 (4 to 111) | 690 (2) | Very low |
BP = blood pressure; CI = confidence interval; CV = cardiovascular; NA = not applicable; NNH = number needed to harm; NNT = number needed to treat.
*—No statistical difference in outcomes.
Practice Pointers
From 2007 to 2014, the age-adjusted prevalence of hypertension was 29.6% in the United States. Of those patients with hypertension, only 75% were receiving treatment and only 51.8% had their hypertension under control.2 Between 2003 and 2013, the death rate attributable to hypertension increased by 8.2%.3 During this time, the goal of hypertension treatment was a BP of 140/90 mm Hg or less, but this Cochrane review looked at lower BP targets for patients with a history of cardiovascular disease to determine if there is added benefit with more aggressive treatment.1
This Cochrane review included six randomized controlled trials and 9,484 patients. Participants were being treated for hypertension and had a documented cardiovascular history of myocardial infarction, stroke, ischemic heart disease, peripheral vascular disease, or angina. The intervention was a lower BP target (135/85 mm Hg or less) vs. standard BP targets (140 to 160/90 to 100 mm Hg or less). Primary outcomes included total and cardiovascular mortality, serious adverse effects, and total cardiovascular events, defined as the number of participants with at least one of the following: myocardial infarction, stroke, sudden death, and hospitalization or death from congestive heart failure.1
Lower BP targets revealed no apparent difference in total mortality or cardiovascular mortality compared with standard BP targets. No differences in serious adverse effects were noted. Lower BP targets did not reduce total cardiovascular events over five years.1
Notably, more participants in the lower BP target group withdrew from the study because of adverse effects (two studies; n = 690; relative risk = 8.16; 95% confidence interval, 2.06 to 32.28), required more drugs to lower BP (2.4 vs. 1.9 drugs, on average), and achieved BP goals less often (64% vs. 75% of the time) compared with those in the standard BP target group.1
The 2017 American College of Cardiology/American Heart Association Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults recently adopted a stringent BP target (less than 130/80 mm Hg) for secondary prevention of cardiovascular events in patients with clinical cardiovascular disease.4 This Cochrane review reveals that lower BP targets in the treatment of hypertension appear to have no effect on total cardiovascular events and no change in overall and cardiovascular mortality.1 Physicians should discuss the new BP goals with patients before pursuing these targets to reduce the risk of cardiovascular events.

