Protracted exposure to radon decay products is the leading environmental cause of cancer mortality in the United States.1,2 Family physicians play a key role in informing their patients about the health risks posed by radon exposure and in recommending proactive actions to reduce radon exposure.
How Does Radon Enter a Home?
Radon, with a radioactive half-life of 3.8 days, is a tasteless, colorless, and odorless radioactive noble gas formed from the radioactive decay of radium, a globally occurring natural component of soil and bedrock. Radon naturally occurs outdoors, but it is generally found at higher concentrations indoors because most houses are not built to be radon resistant. Building ventilation and stack effects cause lower air pressure in a house as compared with the air pressure in the soil around the foundation and basement slab. This pressure differential draws radon into the house through floor-wall joints, cracks in the foundation, and other openings in the building's substructure. Radon released from well water and building materials (e.g., concrete) also represents a potential secondary source of radon in a house.
Elevated residential radon concentrations are found in all types of houses in every U.S. state, regardless of the age of the home or the socioeconomic status of the neighborhood. Therefore, the U.S. Environmental Protection Agency (EPA) recommends that all houses be tested for radon and that action be taken to reduce radon concentrations that are equal to or exceed the EPA's radon action level of 4 pCi per L (150 Bq per m3).3 The EPA also suggests lowering the radon concentrations to less than 4 pCi per L to further reduce lung cancer risk because there is no safe level of radon.3
Radon testing is inexpensive ($15 to $25) and can easily be completed using do-it-yourself radon test kits, which are available at most hardware stores or by calling 800-SOS-RADON (800-767-7236). If elevated radon concentrations are detected, radon mitigation costs generally range from $800 to $1,500 and are eligible health savings account or flexible spending account expenses.
Additional information about radon testing and mitigation is provided in the EPA's Citizen's Guide to Radon3 and other EPA publications (https://www.epa.gov/radon). In collaboration with the EPA, the Conference of Radiation Control Program Directors (a nonprofit organization) also recently released a new Radon Guide for Health Care Providers2 that provides clinicians with guidance to help their patients reduce exposure to radon (http://canceriowa.org/BreathingEasier.aspx).
What Is the Evidence of Radon's Carcinogenicity?
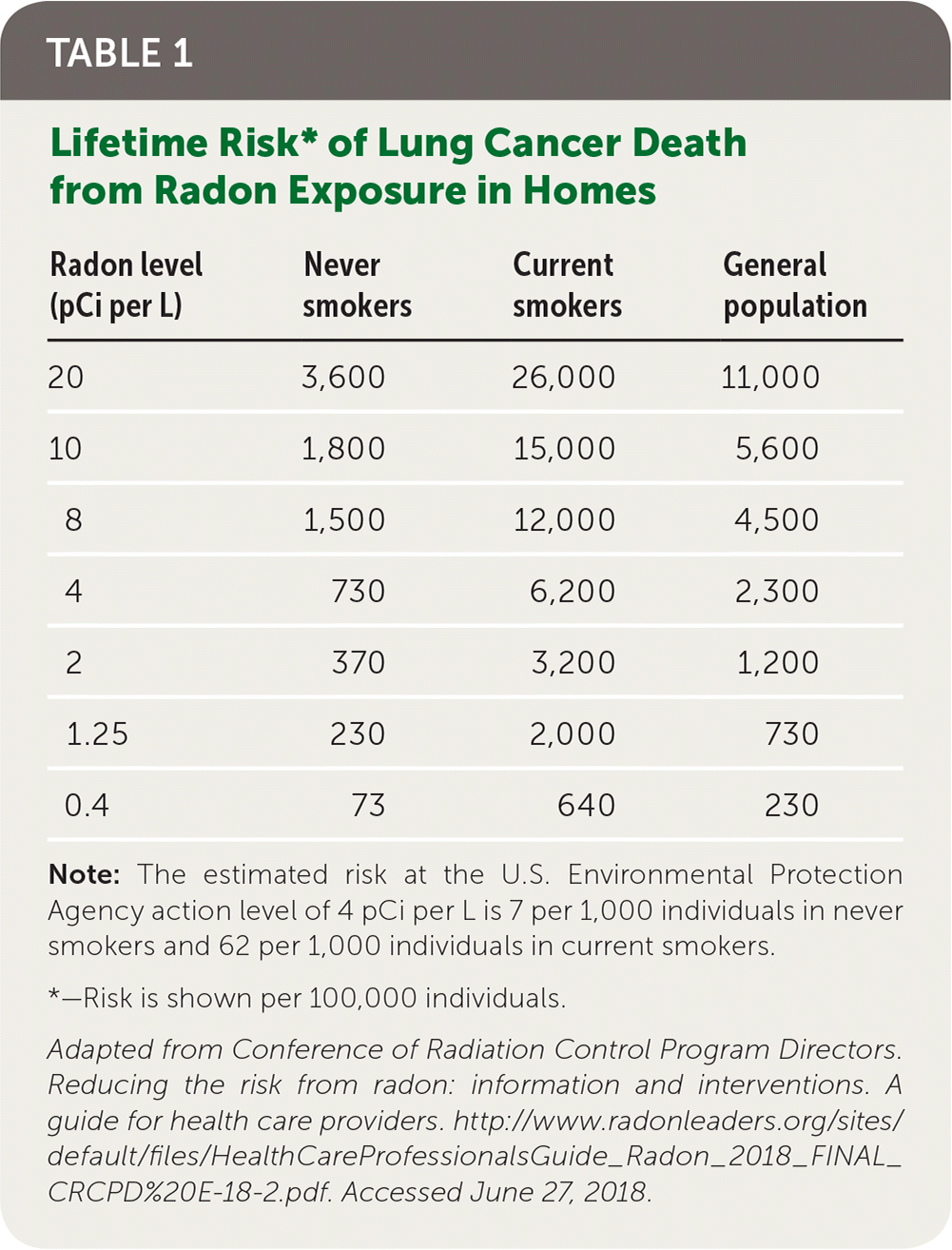
Overwhelming evidence of radon's carcinogenicity comes from 11 large epidemiologic studies of underground miners exposed to radon and from the 1999 National Research Council's pooled analysis of those studies.4,5 In addition, pooled analyses of residential radon studies performed in China, Europe, and North America have also demonstrated that protracted exposure to radon (and radon decay products), even below the EPA's action level, significantly increases lung cancer risk.6–8 The National Research Council's lung cancer risk projections to the general public from protracted radon exposure closely agree with the risk estimates reported from these three pooled analyses.1,2,5 Based on the National Research Council's findings from the pooled underground miner studies4 and further supported by the findings of the residential radon case-control studies,6–8 the EPA estimates that 21,000 people die from radon-induced lung cancer each year in the United States, which represents about 13% of annual U.S. lung cancer deaths.9 If treated as an individual disease category, radon-induced lung cancer would rank among the top 10 causes of cancer mortality.2 The combined health effects of radon and tobacco exposure are synergistic rather than additive, so reducing either of the exposures substantially reduces lung cancer risk.2,5 Table 1 presents the lifetime risk of lung cancer death from radon exposure in homes based on smoking status and radon level.2
TABLE 1 Lifetime Risk* of Lung Cancer Death from Radon Exposure in Homes
| Radon level (pCi per L) | Never smokers | Current smokers | General population |
|---|---|---|---|
| 20 | 3,600 | 26,000 | 11,000 |
| 10 | 1,800 | 15,000 | 5,600 |
| 8 | 1,500 | 12,000 | 4,500 |
| 4 | 730 | 6,200 | 2,300 |
| 2 | 370 | 3,200 | 1,200 |
| 1.25 | 230 | 2,000 | 730 |
| 0.4 | 73 | 640 | 230 |
Note: The estimated risk at the U.S. Environmental Protection Agency action level of 4 pCi per L is 7 per 1,000 individuals in never smokers and 62 per 1,000 individuals in current smokers.
*—Risk is shown per 100,000 individuals.
Adapted from Conference of Radiation Control Program Directors. Reducing the risk from radon: information and interventions. A guide for health care providers. http://www.radonleaders.org/sites/default/files/HealthCareProfessionalsGuide_Radon_2018_FINAL_CRCPD%20E-18-2.pdf. Accessed June 27, 2018.
How Does Radon Induce Lung Cancer?
Radon decays into a series of solid radioactive products that can be inhaled and then deposited onto the pulmonary epithelium. Two of the alpha-emitting decay products, polonium-214 and polonium-218, deliver the majority of the radiogenic dose to the lungs and have been identified as the primary cause of radon-induced lung cancer.2–5 These decay products cause single- and double-strand DNA breaks as well as indirect genotoxic and nongenotoxic effects on cells, which can lead to malignancy.2,4,5
Does Radon Present a Substantial Risk to Individuals Who Have Never Smoked?
In the United States, up to 20% of lung cancer deaths each year occur in individuals who have never smoked, which translates to about 30,000 Americans in 2017.10 Protracted radon exposure is considered the leading cause of lung cancer in this population.1–5
Is a History of High Radon Exposure An Eligible Criterion for Low-Dose CT Screening?
The U.S. Preventive Services Task Force states that the benefit of low-dose computed tomography (CT) screening varies because individuals who are at higher risk of developing lung cancer because of smoking history and other risk factors, such as high radon exposure, are more likely to benefit than individuals who have no risk factors.11 Furthermore, the National Comprehensive Cancer Network guidelines recommend low-dose CT screening beginning at 50 years of age for individuals with at least a 20 pack-year smoking history and documented high radon exposure.12 Interviews to assess eligibility for low-dose CT screening present an opportunity to educate patients about the risks posed by smoking and radon exposure, even if the individual is not eligible for low-dose CT screening. It is important to note that the American Academy of Family Physicians concludes that the evidence is insufficient to recommend for or against screening for lung cancer with low-dose CT in persons at high risk based on age and smoking history.13

