The well-child visit allows for comprehensive assessment of a child and the opportunity for further evaluation if abnormalities are detected. A complete history during the well-child visit includes information about birth history; prior screenings; diet; sleep; dental care; and medical, surgical, family, and social histories. A head-to-toe examination should be performed, including a review of growth. Immunizations should be reviewed and updated as appropriate. Screening for postpartum depression in mothers of infants up to six months of age is recommended. Based on expert opinion, the American Academy of Pediatrics recommends developmental surveillance at each visit, with formal developmental screening at nine, 18, and 30 months and autism-specific screening at 18 and 24 months; the U.S. Preventive Services Task Force found insufficient evidence to make a recommendation. Well-child visits provide the opportunity to answer parents' or caregivers' questions and to provide age-appropriate guidance. Car seats should remain rear facing until two years of age or until the height or weight limit for the seat is reached. Fluoride use, limiting or avoiding juice, and weaning to a cup by 12 months of age may improve dental health. A one-time vision screening between three and five years of age is recommended by the U.S. Preventive Services Task Force to detect amblyopia. The American Academy of Pediatrics guideline based on expert opinion recommends that screen time be avoided, with the exception of video chatting, in children younger than 18 months and limited to one hour per day for children two to five years of age. Cessation of breastfeeding before six months and transition to solid foods before six months are associated with childhood obesity. Juice and sugar-sweetened beverages should be avoided before one year of age and provided only in limited quantities for children older than one year.
Well-child visits for infants and young children (up to five years) provide opportunities for physicians to screen for medical problems (including psychosocial concerns), to provide anticipatory guidance, and to promote good health. The visits also allow the family physician to establish a relationship with the parents or caregivers. This article reviews the U.S. Preventive Services Task Force (USPSTF) and the American Academy of Pediatrics (AAP) guidelines for screenings and recommendations for infants and young children. Family physicians should prioritize interventions with the strongest evidence for patient-oriented outcomes, such as immunizations, postpartum depression screening, and vision screening.
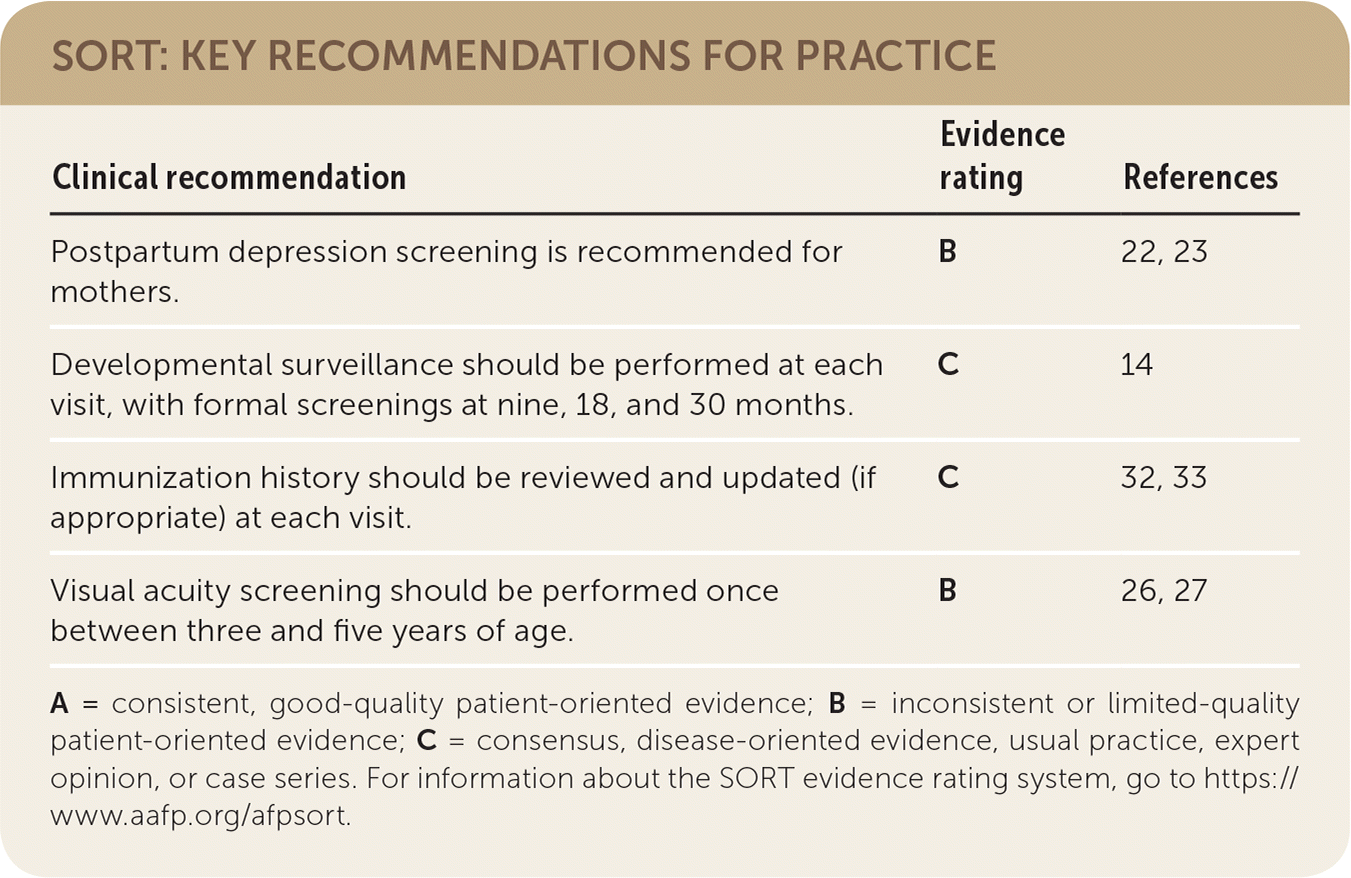
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Postpartum depression screening is recommended for mothers. | B | 22, 23 |
| Developmental surveillance should be performed at each visit, with formal screenings at nine, 18, and 30 months. | C | 14 |
| Immunization history should be reviewed and updated (if appropriate) at each visit. | C | 32, 33 |
| Visual acuity screening should be performed once between three and five years of age. | B | 26, 27 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Clinical Examination
HISTORY
The history should include a brief review of birth history; prematurity can be associated with complex medical conditions.1 Evaluate breastfed infants for any feeding problems,2 and assess formula-fed infants for type and quantity of iron-fortified formula being given.3 For children eating solid foods, feeding history should include everything the child eats and drinks. Sleep, urination, defecation, nutrition, dental care, and child safety should be reviewed. Medical, surgical, family, and social histories should be reviewed and updated. For newborns, review the results of all newborn screening tests (Table 14–7 ) and schedule follow-up visits as necessary.2
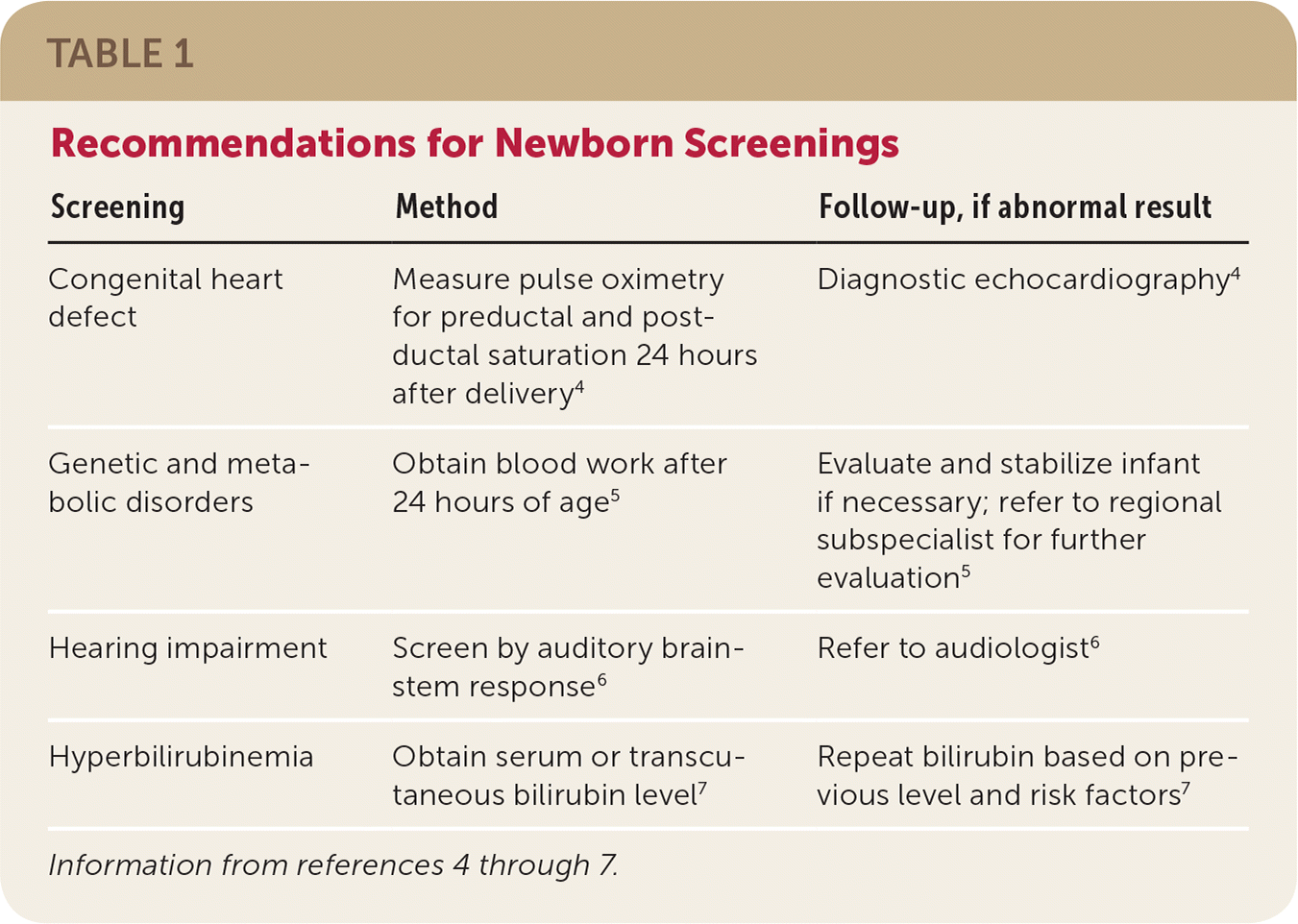
TABLE 1. Recommendations for Newborn Screenings
| Screening | Method | Follow-up, if abnormal result |
|---|---|---|
| Congenital heart defect | Measure pulse oximetry for preductal and postductal saturation 24 hours after delivery4 | Diagnostic echocardiography4 |
| Genetic and metabolic disorders | Obtain blood work after 24 hours of age5 | Evaluate and stabilize infant if necessary; refer to regional subspecialist for further evaluation5 |
| Hearing impairment | Screen by auditory brain-stem response6 | Refer to audiologist6 |
| Hyperbilirubinemia | Obtain serum or transcutaneous bilirubin level7 | Repeat bilirubin based on previous level and risk factors7 |
PHYSICAL EXAMINATION
A comprehensive head-to-toe examination should be completed at each well-child visit. Interval growth should be reviewed by using appropriate age, sex, and gestational age growth charts for height, weight, head circumference, and body mass index if 24 months or older. The Centers for Disease Control and Prevention (CDC)-recommended growth charts are available. Percentiles and observations of changes along the chart's curve should be assessed at every visit. Include assessment of parent/caregiver-child interactions and potential signs of abuse such as bruises on uncommonly injured areas, burns, human bite marks, bruises on nonmobile infants, or multiple injuries at different healing stages.8
Screenings
The USPSTF and AAP screening recommendations are outlined in Table 2.3,9–27 A summary of AAP recommendations is available. The American Academy of Family Physicians (AAFP) generally adheres to USPSTF recommendations.28
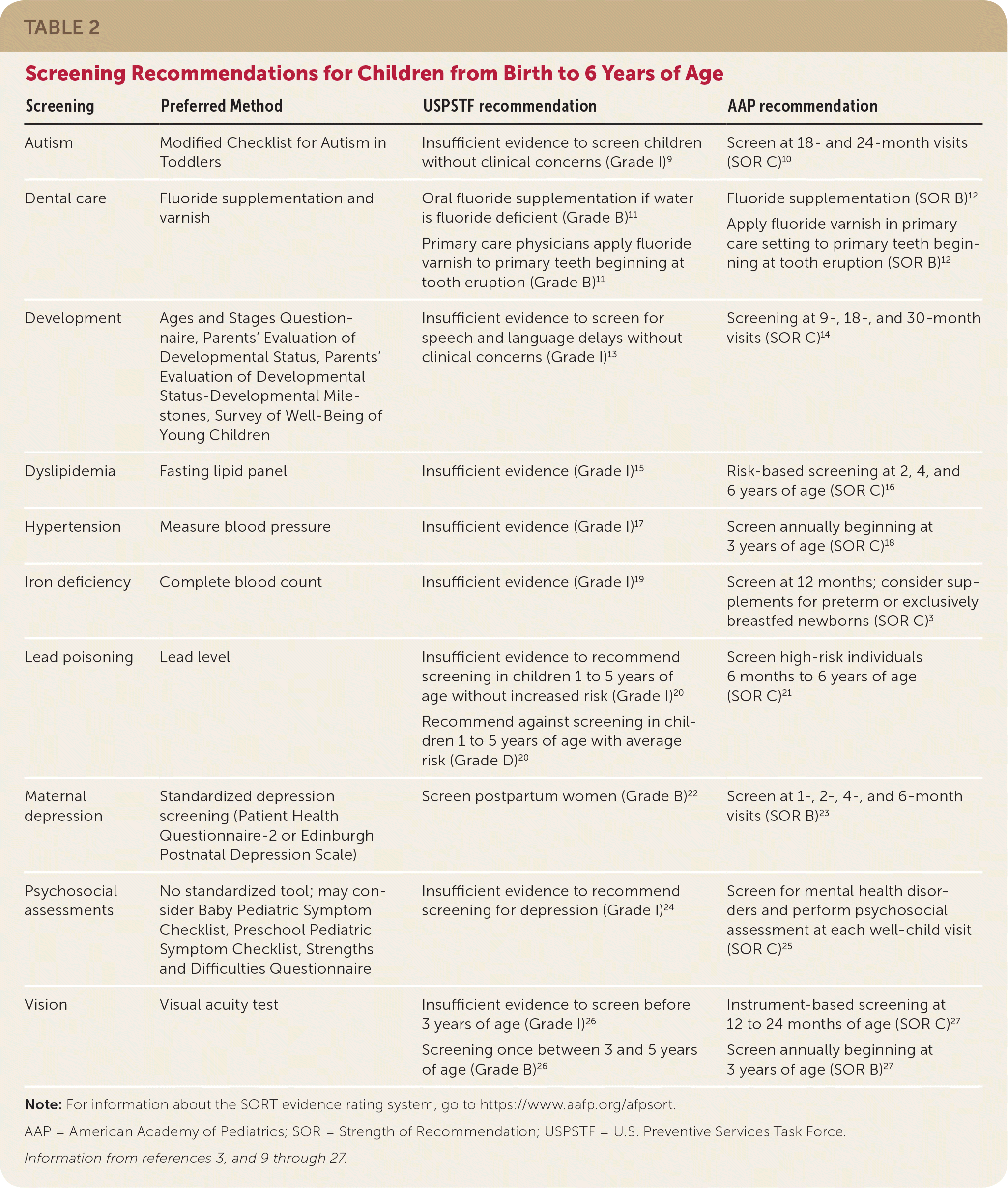
TABLE 2. Screening Recommendations for Children from Birth to 6 Years of Age
| Screening | Preferred Method | USPSTF recommendation | AAP recommendation |
|---|---|---|---|
| Autism | Modified Checklist for Autism in Toddlers | Insufficient evidence to screen children without clinical concerns (Grade I)9 | Screen at 18- and 24-month visits (SOR C)10 |
| Dental care | Fluoride supplementation and varnish | Oral fluoride supplementation if water is fluoride deficient (Grade B)11 Primary care physicians apply fluoride varnish to primary teeth beginning at tooth eruption (Grade B)11 | Fluoride supplementation (SOR B)12 Apply fluoride varnish in primary care setting to primary teeth beginning at tooth eruption (SOR B)12 |
| Development | Ages and Stages Questionnaire, Parents' Evaluation of Developmental Status, Parents' Evaluation of Developmental Status-Developmental Milestones, Survey of Well-Being of Young Children | Insufficient evidence to screen for speech and language delays without clinical concerns (Grade I)13 | Screening at 9-, 18-, and 30-month visits (SOR C)14 |
| Dyslipidemia | Fasting lipid panel | Insufficient evidence (Grade I)15 | Risk-based screening at 2, 4, and 6 years of age (SOR C)16 |
| Hypertension | Measure blood pressure | Insufficient evidence (Grade I)17 | Screen annually beginning at 3 years of age (SOR C)18 |
| Iron deficiency | Complete blood count | Insufficient evidence (Grade I)19 | Screen at 12 months; consider supplements for preterm or exclusively breastfed newborns (SOR C)3 |
| Lead poisoning | Lead level | Insufficient evidence to recommend screening in children 1 to 5 years of age without increased risk (Grade I)20 Recommend against screening in children 1 to 5 years of age with average risk (Grade D)20 | Screen high-risk individuals 6 months to 6 years of age (SOR C)21 |
| Maternal depression | Standardized depression screening (Patient Health Questionnaire-2 or Edinburgh Postnatal Depression Scale) | Screen postpartum women (Grade B)22 | Screen at 1-, 2-, 4-, and 6-month visits (SOR B)23 |
| Psychosocial assessments | No standardized tool; may consider Baby Pediatric Symptom Checklist, Preschool Pediatric Symptom Checklist, Strengths and Difficulties Questionnaire | Insufficient evidence to recommend screening for depression (Grade I)24 | Screen for mental health disorders and perform psychosocial assessment at each well-child visit (SOR C)25 |
| Vision | Visual acuity test | Insufficient evidence to screen before 3 years of age (Grade I)26 Screening once between 3 and 5 years of age (Grade B)26 | Instrument-based screening at 12 to 24 months of age (SOR C)27 Screen annually beginning at 3 years of age (SOR B)27 |
Note: For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
AAP = American Academy of Pediatrics; SOR = Strength of Recommendation; USPSTF = U.S. Preventive Services Task Force.
MATERNAL DEPRESSION
Prevalence of postpartum depression is around 12%,22 and its presence can impair infant development. The USPSTF and AAP recommend using the Edinburgh Postnatal Depression Scale or the Patient Health Questionnaire-2 to screen for maternal depression. The USPSTF does not specify a screening schedule; however, based on expert opinion, the AAP recommends screening mothers at the one-, two-, four-, and six-month well-child visits, with further evaluation for positive results.23 There are no recommendations to screen other caregivers if the mother is not present at the well-child visit.
PSYCHOSOCIAL
With nearly one-half of children in the United States living at or near the poverty level, assessing home safety, food security, and access to safe drinking water can improve awareness of psychosocial problems, with referrals to appropriate agencies for those with positive results.29 The prevalence of mental health disorders (i.e., primarily anxiety, depression, behavioral disorders, attention-deficit/hyperactivity disorder) in preschool-aged children is around 6%.30 Risk factors for these disorders include having a lower socioeconomic status, being a member of an ethnic minority, and having a non–English-speaking parent or primary caregiver.25 The USPSTF found insufficient evidence regarding screening for depression in children up to 11 years of age.24 Based on expert opinion, the AAP recommends that physicians consider screening, although screening in young children has not been validated or standardized.25
DEVELOPMENT AND SURVEILLANCE
Based on expert opinion, the AAP recommends early identification of developmental delays14 and autism10; however, the USPSTF found insufficient evidence to recommend formal developmental screening13 or autism-specific screening9 if the parents/caregivers or physician have no concerns. If physicians choose to screen, developmental surveillance of language, communication, gross and fine movements, social/emotional development, and cognitive/problem-solving skills should occur at each visit by eliciting parental or caregiver concerns, obtaining interval developmental history, and observing the child. Any area of concern should be evaluated with a formal developmental screening tool, such as Ages and Stages Questionnaire, Parents' Evaluation of Developmental Status, Parents' Evaluation of Developmental Status-Developmental Milestones, or Survey of Well-Being of Young Children. These tools are available. If results are abnormal, consider intervention or referral to early intervention services. The AAP recommends completing the previously mentioned formal screening tools at nine-, 18-, and 30-month well-child visits.14
The AAP also recommends autism-specific screening at 18 and 24 months.10 The USPSTF recommends using the two-step Modified Checklist for Autism in Toddlers (M-CHAT) screening tool if a physician chooses to screen a patient for autism.10 The M-CHAT can be incorporated into the electronic medical record, with the possibility of the parent or caregiver completing the questionnaire through the patient portal before the office visit.
IRON DEFICIENCY
Multiple reports have associated iron deficiency with impaired neurodevelopment. Therefore, it is essential to ensure adequate iron intake. Based on expert opinion, the AAP recommends supplements for preterm infants beginning at one month of age and exclusively breastfed term infants at six months of age.3 The USPSTF found insufficient evidence to recommend screening for iron deficiency in infants.19 Based on expert opinion, the AAP recommends measuring a child's hemoglobin level at 12 months of age.3
LEAD
Lead poisoning and elevated lead blood levels are prevalent in young children. The AAP and CDC recommend a targeted screening approach. The AAP recommends screening for serum lead levels between six months and six years in high-risk children; high-risk children are identified by location-specific risk recommendations, enrollment in Medicaid, being foreign born, or personal screening.21 The USPSTF does not recommend screening for lead poisoning in children at average risk who are asymptomatic.20
VISION
The USPSTF recommends at least one vision screening to detect amblyopia between three and five years of age. Testing options include visual acuity, ocular alignment test, stereoacuity test, photoscreening, and autorefractors. The USPSTF found insufficient evidence to recommend screening before three years of age.26 The AAP, American Academy of Ophthalmology, and the American Academy of Pediatric Ophthalmology and Strabismus recommend the use of an instrument-based screening (photoscreening or autorefractors) between 12 months and three years of age and annual visual acuity screening beginning at four years of age.31
IMMUNIZATIONS
The AAFP recommends that all children be immunized.32 Recommended vaccination schedules, endorsed by the AAP, the AAFP, and the Advisory Committee on Immunization Practices, are found at https://www.cdc.gov/vaccines/schedules/hcp/child-adolescent.html. Immunizations are usually administered at the two-, four-, six-, 12-, and 15- to 18-month well-child visits; the four- to six-year well-child visit; and annually during influenza season. Additional vaccinations may be necessary based on medical history.33 Immunization history should be reviewed at each wellness visit.
Anticipatory Guidance
SAFETY
Injuries remain the leading cause of death among children,34 and the AAP has made several recommendations to decrease the risk of injuries.35–42 Appropriate use of child restraints minimizes morbidity and mortality associated with motor vehicle collisions. Infants need a rear-facing car safety seat until two years of age or until they reach the height or weight limit for the specific car seat. Children should then switch to a forward-facing car seat for as long as the seat allows, usually 65 to 80 lb (30 to 36 kg).35 Children should never be unsupervised around cars, driveways, and streets. Young children should wear bicycle helmets while riding tricycles or bicycles.37
Having functioning smoke detectors and an escape plan decreases the risk of fire- and smoke-related deaths.36 Water heaters should be set to a maximum of 120°F (49°C) to prevent scald burns.37 Infants and young children should be watched closely around any body of water, including water in bathtubs and toilets, to prevent drowning. Swimming pools and spas should be completely fenced with a self-closing, self-latching gate.38
Infants should not be left alone on any high surface, and stairs should be secured by gates.43 Infant walkers should be discouraged because they provide no benefit and they increase falls down stairs, even if stair gates are installed.39 Window locks, screens, or limited-opening windows decrease injury and death from falling.40 Parents or caregivers should also anchor furniture to a wall to prevent heavy pieces from toppling over. Firearms should be kept unloaded and locked.41
Young children should be closely supervised at all times. Small objects are a choking hazard, especially for children younger than three years. Latex balloons, round objects, and food can cause life-threatening airway obstruction.42 Long strings and cords can strangle children.37
DENTAL CARE
Infants should never have a bottle in bed, and babies should be weaned to a cup by 12 months of age.44 Juices should be avoided in infants younger than 12 months.45 Fluoride use inhibits tooth demineralization and bacterial enzymes and also enhances remineralization.11 The AAP and USPSTF recommend fluoride supplementation and the application of fluoride varnish for teeth if the water supply is insufficient.11,12 Begin brushing teeth at tooth eruption with parents or caregivers supervising brushing until mastery. Children should visit a dentist regularly, and an assessment of dental health should occur at well-child visits.44
SCREEN TIME
Hands-on exploration of their environment is essential to development in children younger than two years. Video chatting is acceptable for children younger than 18 months; otherwise digital media should be avoided. Parents and caregivers may use educational programs and applications with children 18 to 24 months of age. If screen time is used for children two to five years of age, the AAP recommends a maximum of one hour per day that occurs at least one hour before bedtime. Longer usage can cause sleep problems and increases the risk of obesity and social-emotional delays.46
SLEEP
To decrease the risk of sudden infant death syndrome (SIDS), the AAP recommends that infants sleep on their backs on a firm mattress for the first year of life with no blankets or other soft objects in the crib.45 Breastfeeding, pacifier use, and room sharing without bed sharing protect against SIDS; infant exposure to tobacco, alcohol, drugs, and sleeping in bed with parents or caregivers increases the risk of SIDS.47
DIET AND ACTIVITY
The USPSTF, AAFP, and AAP all recommend breastfeeding until at least six months of age and ideally for the first 12 months.48 Vitamin D 400 IU supplementation for the first year of life in exclusively breastfed infants is recommended to prevent vitamin D deficiency and rickets.49 Based on expert opinion, the AAP recommends the introduction of certain foods at specific ages. Early transition to solid foods before six months is associated with higher consumption of fatty and sugary foods50 and an increased risk of atopic disease.51 Delayed transition to cow's milk until 12 months of age decreases the incidence of iron deficiency.52 Introduction of highly allergenic foods, such as peanut-based foods and eggs, before one year decreases the likelihood that a child will develop food allergies.53
With approximately 17% of children being obese, many strategies for obesity prevention have been proposed.54 The USPSTF does not have a recommendation for screening or interventions to prevent obesity in children younger than six years.54 The AAP has made several recommendations based on expert opinion to prevent obesity. Cessation of breastfeeding before six months and introduction of solid foods before six months are associated with childhood obesity and are not recommended.55 Drinking juice should be avoided before one year of age, and, if given to older children, only 100% fruit juice should be provided in limited quantities: 4 ounces per day from one to three years of age and 4 to 6 ounces per day from four to six years of age. Intake of other sugar-sweetened beverages should be discouraged to help prevent obesity.45 The AAFP and AAP recommend that children participate in at least 60 minutes of active free play per day.55,56
Data Sources: Literature search was performed using the USPSTF published recommendations and the AAP Periodicity table. PubMed searches were completed using the key terms pediatric, obesity prevention, and allergy prevention with search limits of infant younger than 23 months or pediatric younger than 18 years. The searches included systematic reviews, randomized controlled trials, clinical trials, and position statements. Essential Evidence Plus was also reviewed. Search dates: May through October 2017.

