The American Academy of Family Physicians (AAFP) reviews each recommendation statement issued by the U.S. Preventive Services Task Force (USPSTF), including the evidence reviews on which they are based, and makes an independent determination about whether to endorse the recommendation or to develop its own.1 The AAFP often endorses USPSTF recommendations; however, on occasion the AAFP has a different interpretation of the complex clinical data or its application to the practice of family medicine.2,3 This occurred with the USPSTF's recent recommendation on prostate cancer screening.
The USPSTF changed its position from recommending against routine prostate-specific antigen (PSA)–based screening (D recommendation)4 to concluding that for men 55 to 69 years of age, the decision to undergo periodic PSA-based screening should be individualized (C recommendation).5 The USPSTF now recommends that men have an opportunity to discuss the potential benefits and harms of screening with their physician and to incorporate their preferences in the decision.5 The language of this recommendation implies that all men 55 to 69 years of age should be offered shared decision making regarding PSA-based prostate cancer screening, even though there is little evidence that routinely doing so improves patient-oriented outcomes.
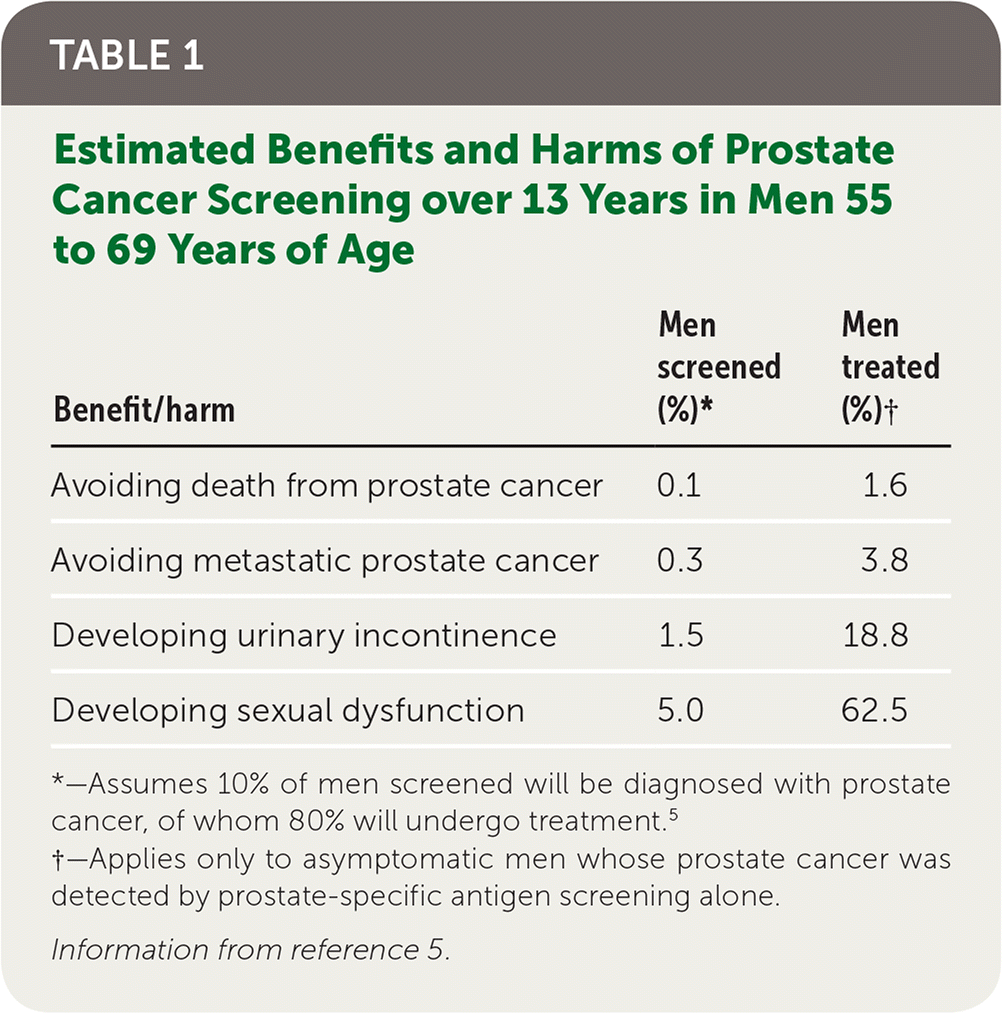
Based primarily on the single randomized controlled trial that demonstrated benefit from prostate cancer screening, the USPSTF estimates that of 1,000 men 55 to 69 years of age screened over 13 years, 100 will be diagnosed with prostate cancer, 80 will undergo treatment, and 1.3 deaths from prostate cancer and three cases of metastatic prostate cancer will be avoided.5 Table 1 shows estimated outcomes from screening average-risk men.5 Few men diagnosed with and treated for prostate cancer will experience a mortality benefit, and an estimated 20% to 50% of those treated will never become symptomatic, even without treatment.6 This high rate of overdiagnosis from prostate cancer screening exposes many men to harms without any potential benefit.
TABLE 1. Estimated Benefits and Harms of Prostate Cancer Screening over 13 Years in Men 55 to 69 Years of Age
| Benefit/harm | Men screened (%)* | Men treated (%)† |
|---|---|---|
| Avoiding death from prostate cancer | 0.1 | 1.6 |
| Avoiding metastatic prostate cancer | 0.3 | 3.8 |
| Developing urinary incontinence | 1.5 | 18.8 |
| Developing sexual dysfunction | 5.0 | 62.5 |
*—Assumes 10% of men screened will be diagnosed with prostate cancer, of whom 80% will undergo treatment.5
†—Applies only to asymptomatic men whose prostate cancer was detected by prostate-specific antigen screening alone.
Information from reference 5.
The AAFP finds that the net benefit of population screening for prostate cancer is small at best, and it does not recommend routinely discussing PSA-based screening if the patient does not request it. Providing all eligible men with shared decision making, regardless of approach,7 requires time and diverts focus from other preventive services that are more likely to improve health outcomes. However, the AAFP recognizes the importance of providing patient-centered care, incorporating patient values in decision making, and respecting patient choice. For that reason, the AAFP supports providing PSA-based screening to men 55 to 69 years of age who express a clear preference for the test after having an opportunity to participate in shared decision making.
The AAFP recommends the following:
- The AAFP does not recommend routine PSA-based screening for prostate cancer. For men 55 to 69 years of age who are considering periodic prostate cancer screening, physicians should discuss the risks and benefits and engage in shared decision making that enables an informed choice. (Grade C recommendation.)8
- The AAFP recommends against screening for prostate cancer in men 70 years and older. (Grade D recomemndation.)8
The full AAFP recommendation statement provides more background and detail, but some key items are described in Table 2.8–11
TABLE 2. AAFP Recommendations for Men Who Elect to Have Prostate Cancer Screening

| Screening method | PSA testing only; no evidence to support digital rectal examination or any other screening methods9 |
| Screening interval | Repeat PSA screening required10; beneficial screening intervals in the single effective trial typically occurred every two to four years11 |
| Men 70 years and older | No benefit to PSA screening in this population |
| Men younger than 55 years | Inadequate data to determine whether this population would benefit from screening |
| Black men and men with a family history of prostate cancer | Inadequate data to determine whether the outcomes of screening in these higher risk men are different from those in average-risk men; however, higher risk men may have different perceptions of the risks and benefits involved |
AAFP = American Academy of Family Physicians; PSA = prostate-specific antigen.
Clinical preventive service recommendations are based on populations but are applied to individuals. Even with good evidence of a significant net benefit for a population, some individuals will have no benefit, and others will be harmed. In the case of prostate cancer screening, the AAFP believes that the net benefit does not justify routine screening or routinely offering shared decision making. However, an individual may desire screening, and he will make a more informed decision following shared decision making with a trusted physician who incorporates the patient's values and respects the patient's decision. The AAFP prostate cancer screening recommendations are based on family medicine values that emphasize patient choice, use of the best available evidence, and the personal patient-physician relationship.
Editor's Note: Dr. Stevermer and Dr. Fink are chair and vice chair, respectively, of the AAFP Commission on Health of the Public and Science's Subcommittee on Clinical Preventive Services.
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the Uniformed Services University of the Health Sciences or the Department of Defense.

