Braces and splints can immobilize and protect joints, reduce pain, decrease swelling, and facilitate healing of acute injuries. They are also used for injury prevention and chronic pain reduction, and to alter the function of a joint. The medial unloading (valgus) knee brace is an option for patients with medial knee osteoarthritis, but evidence of long-term benefit is limited. The patellar stabilizing brace helps maintain proper patellar alignment but has mixed results in treating patellofemoral pain syndrome. The patellar tendon strap is effective in treating pain from patellar tendinopathy. The knee immobilizing splint is used after surgery to prevent reinjury and for acute or presurgical management of quadriceps rupture, patellar tendon rupture, medial collateral ligament rupture, patellar fracture or dislocation, and other acute traumatic knee injuries. Use of a functional ankle brace is more effective than immobilization or a compression wrap in terms of functional outcomes after an acute ankle sprain and prevention of future ankle sprains. The thumb spica splint is effective for the treatment of thumb carpometacarpal osteoarthritis and de Quervain tenosynovitis, and may be used for patients with suspected scaphoid fractures. A wrist splint has short-term effectiveness in treating symptoms of carpal tunnel syndrome but may not be more effective than other conservative therapies.
Family physicians often treat musculoskeletal conditions for which bracing or splinting can be useful (Table 1).1 In 2015, U.S. spending on orthopedic braces, casting supplies, and splints was estimated at $1.2 billion, and these expenses are expected to increase as insurance companies cover less of these products.2
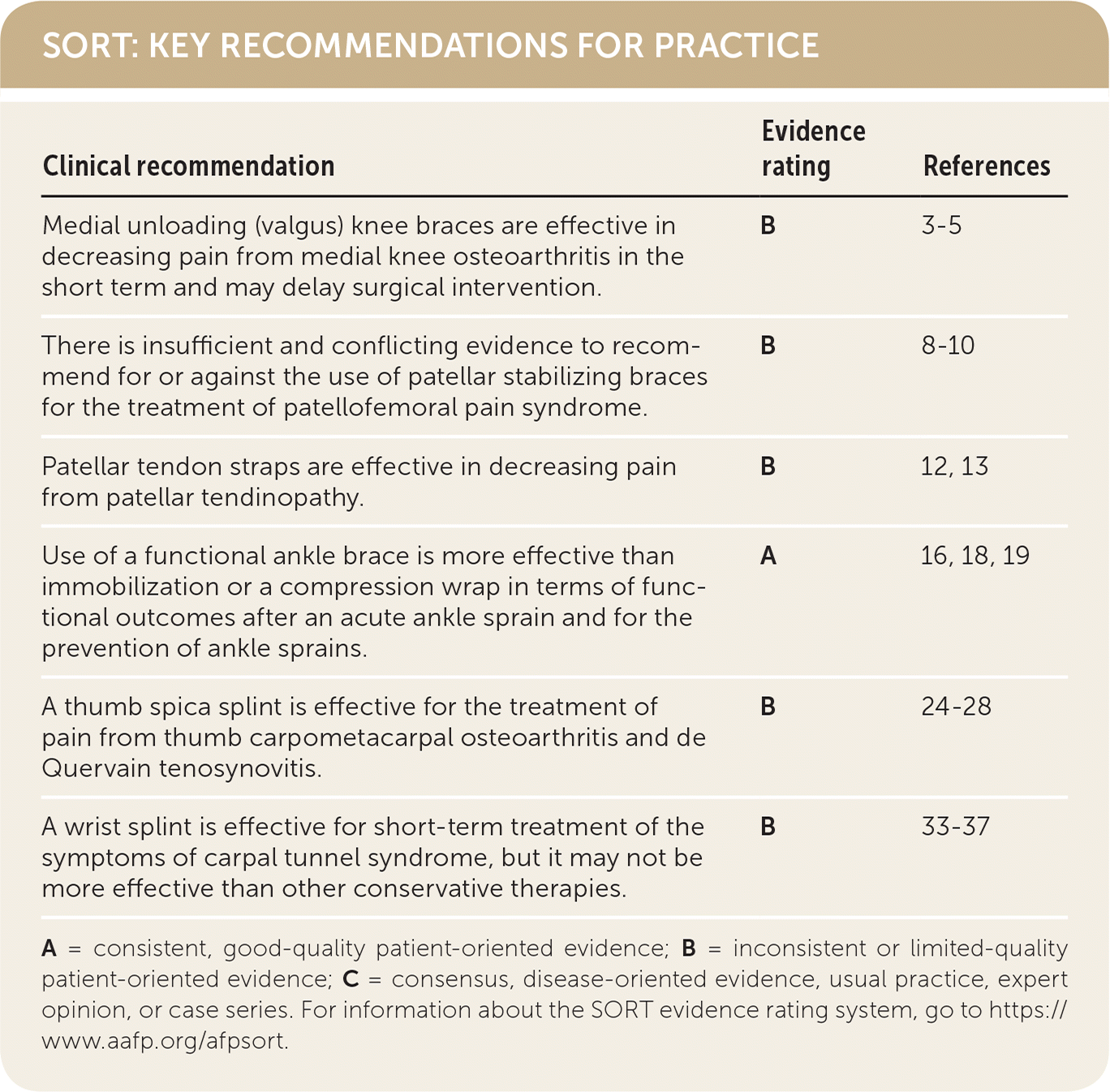
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Medial unloading (valgus) knee braces are effective in decreasing pain from medial knee osteoarthritis in the short term and may delay surgical intervention. | B | 3–5 |
| There is insufficient and conflicting evidence to recommend for or against the use of patellar stabilizing braces for the treatment of patellofemoral pain syndrome. | B | 8–10 |
| Patellar tendon straps are effective in decreasing pain from patellar tendinopathy. | B | 12, 13 |
| Use of a functional ankle brace is more effective than immobilization or a compression wrap in terms of functional outcomes after an acute ankle sprain and for the prevention of ankle sprains. | A | 16, 18, 19 |
| A thumb spica splint is effective for the treatment of pain from thumb carpometacarpal osteoarthritis and de Quervain tenosynovitis. | B | 24–28 |
| A wrist splint is effective for short-term treatment of the symptoms of carpal tunnel syndrome, but it may not be more effective than other conservative therapies. | B | 33–37 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
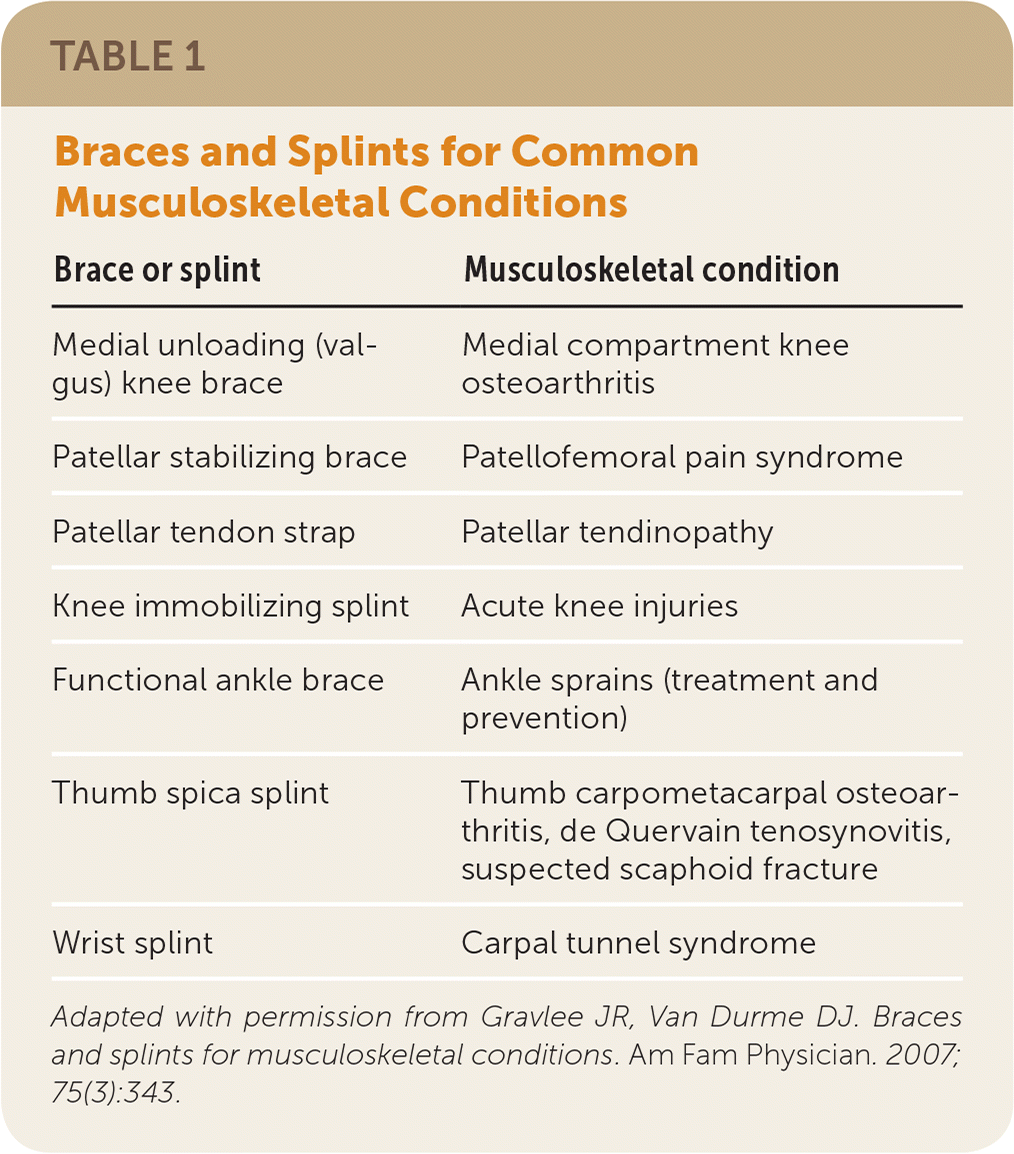
TABLE 1. Braces and Splints for Common Musculoskeletal Conditions
| Brace or splint | Musculoskeletal condition |
|---|---|
| Medial unloading (valgus) knee brace | Medial compartment knee osteoarthritis |
| Patellar stabilizing brace | Patellofemoral pain syndrome |
| Patellar tendon strap | Patellar tendinopathy |
| Knee immobilizing splint | Acute knee injuries |
| Functional ankle brace | Ankle sprains (treatment and prevention) |
| Thumb spica splint | Thumb carpometacarpal osteoarthritis, de Quervain tenosynovitis, suspected scaphoid fracture |
| Wrist splint | Carpal tunnel syndrome |
Adapted with permission from Gravlee JR, Van Durme DJ. Braces and splints for musculoskeletal conditions. Am Fam Physician. 2007;75(3):343.
Braces and splints can immobilize and protect joints, reduce pain, decrease swelling, and facilitate healing of acute injuries. They are also used for injury prevention and chronic pain reduction, and to alter the function of a joint. It is important for the family physician to choose the appropriate brace or splint for the patient's condition, and to determine the correct size, fit, and duration of use. Selection of an inappropriate brace or splint may lead to delayed healing or further injury. Unnecessarily prolonged use can lead to joint stiffness and muscle weakness, which may increase the risk of injury. Even when used correctly, braces and splints should not replace an adequate rehabilitation program.
Knee Braces
Knee braces are used to improve joint function in medial knee osteoarthritis (OA), stabilize patellofemoral articulation in patellofemoral pain syndrome (PFPS), assist with treatment of patellar tendinopathy, and immobilize the knee after an acute injury.
MEDIAL UNLOADING (VALGUS) KNEE BRACE
The medial unloading (valgus) knee brace (Figure 11 ) is an option for treating pain from medial compartment OA and varus malalignment of the knee. The brace applies an external valgus force on the knee, reducing the load on the medial compartment. The use of medial unloading knee braces has greater benefit in decreasing pain and improving knee function compared with conservative treatment alone.3 An eight-year prospective study showed that wearing this type of brace for six months can halve the chance of knee arthroplasty compared with three months of use, and patients who wore the brace for two years were less likely to require surgery at eight years' follow-up.4 However, another prospective study examining the effectiveness of medial unloading knee braces at 2.7 years and 11.2 years showed short-term but not long-term benefits, with use decreasing significantly over time.5 A Cochrane review comparing various knee braces, foot orthotics, and conservative therapies for the treatment of medial compartment OA concluded that the optimal choice for orthosis is unclear, and that long-term data on their effectiveness are lacking.6
FIGURE 1
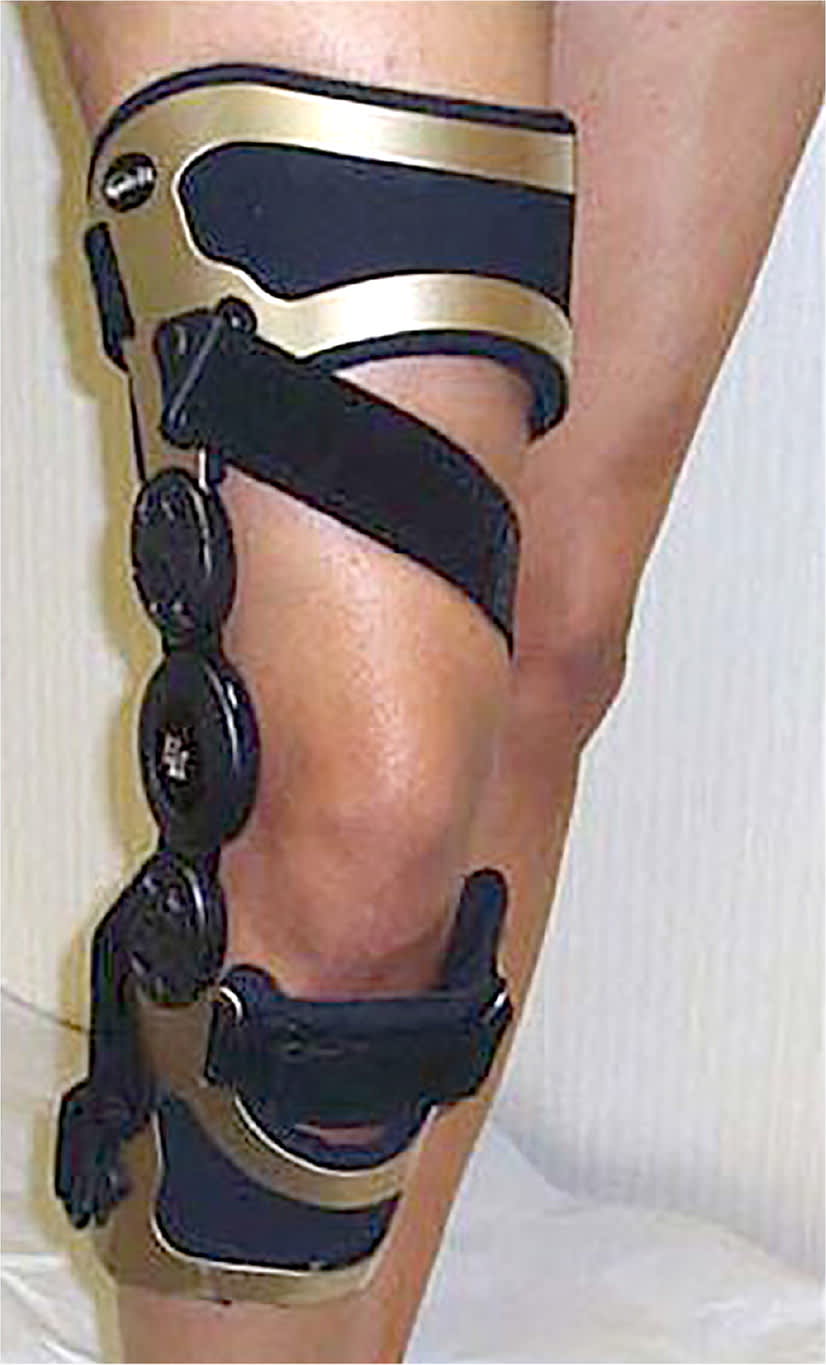
Medial unloading (valgus) knee brace for medial knee osteoarthritis.
Adapted with permission from Gravlee JR, Van Durme DJ. Braces and splints for musculoskeletal conditions. Am Fam Physician. 2007;75(3):344.
PATELLAR STABILIZING BRACE
PFPS is a common cause of anterior knee pain in younger patients. The etiology of PFPS is multi-factorial, and patellar malalignment and instability are thought to have major roles. Patellar stabilizing braces are commonly used to maintain proper patellar alignment in patients with patellar instability, patellar tracking abnormalities, and PFPS.7 These braces are made of an elastic material with additional straps or a buttress to provide patellar support (Figure 2). Despite the biomechanical effectiveness of these braces, two systematic reviews found insufficient evidence to support their long-term use for the treatment of PFPS vs. exercise therapy alone.8,9 Another systematic review found a small benefit for treating PFPS with patellar stabilizing braces.10
FIGURE 2

Patellar stabilizing brace for patellofemoral pain syndrome.
PATELLAR TENDON STRAP
Patellar tendinopathy is a painful chronic condition resulting from repetitive stress. This condition is common in physically active persons and is relatively easy to diagnose in patients presenting with pain, swelling, and tendon thickening localized to any portion of the patellar tendon. Patellar tendon straps (Figure 3) are placed across the midportion of the tendon to reduce tensile stress.11 They have been shown to reduce pain and positively alter biomechanical alignment during physical activity.12 A randomized controlled trial (RCT) found patellar tendon straps to be as effective as patellar taping in improving pain from patellar tendinopathy.13
FIGURE 3
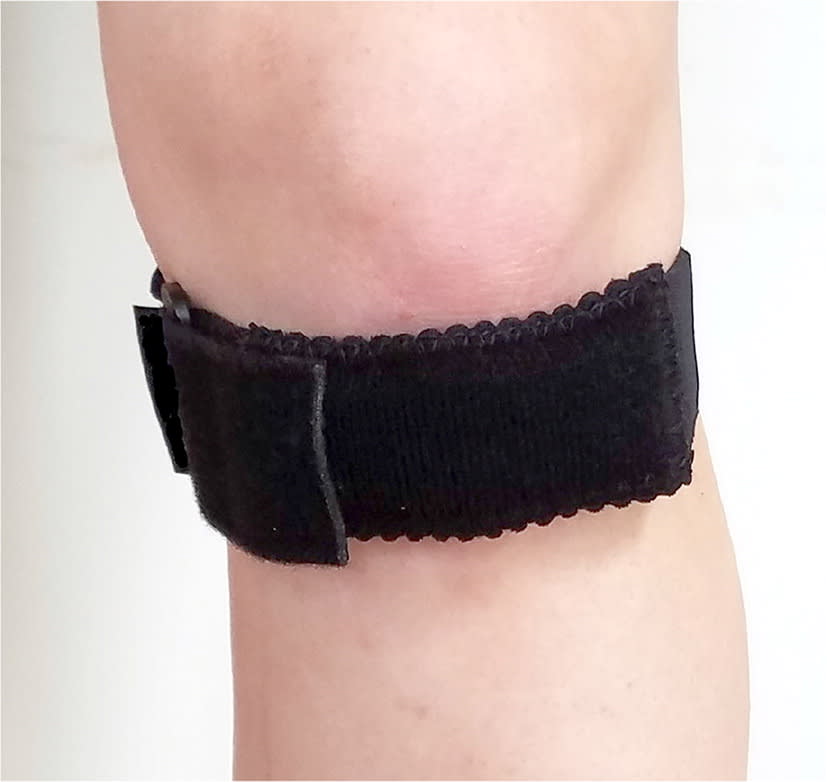
Patellar tendon strap for patellar tendinopathy.
KNEE IMMOBILIZING SPLINT
Knee immobilizing splints (Figure 4) are often used after surgery to help prevent unwanted movement that could reinjure the leg or harm the healing area. They can also be used to stabilize the knee joint and cushion it from impact. Indications for knee immobilizing splints include the acute or presurgical management of quadriceps rupture, patellar tendon rupture, medial collateral ligament rupture, patellar fracture or dislocation, and other acute traumatic knee injuries.1
FIGURE 4
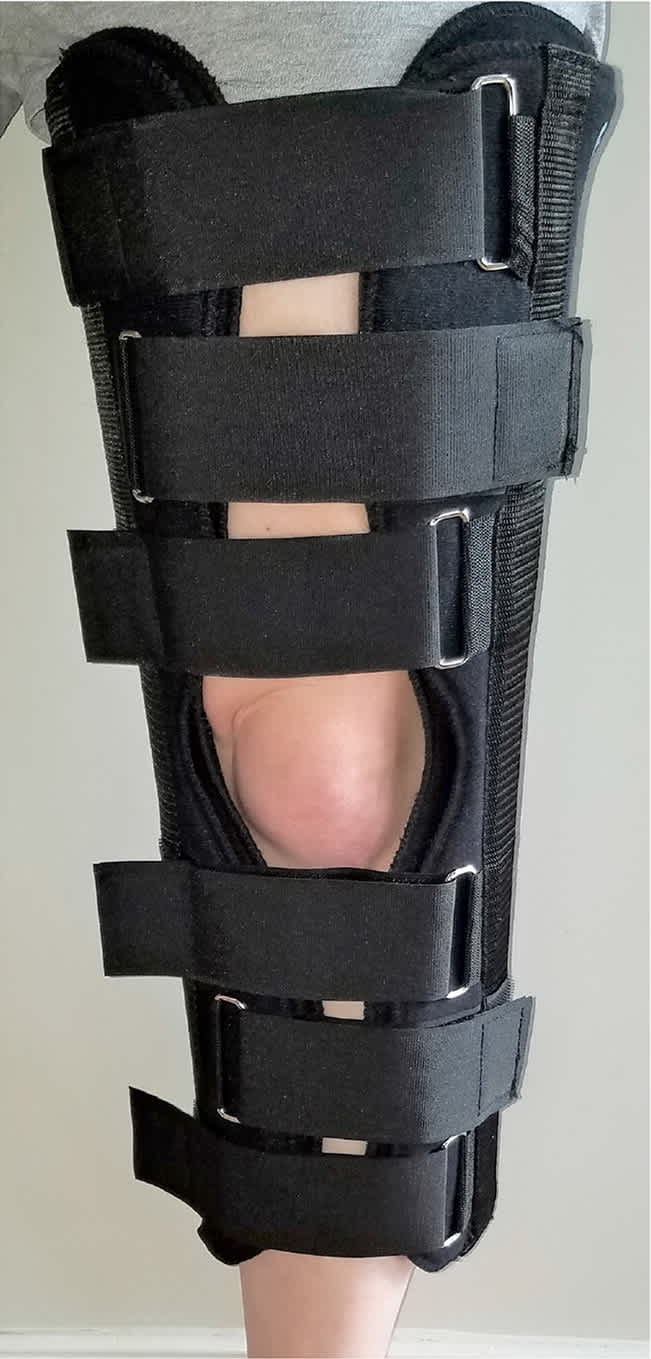
Knee immobilizing splint for acute knee injuries.
Ankle Braces
Ankle sprains are the most common acute sports-related injury, comprising about one-fourth of these injuries.14,15 Because early mobilization after an ankle sprain leads to better outcomes, braces that immobilize the ankle are not recommended.16 Functional ankle braces provide compression and allow for mobility during physical activity while protecting against inversion and eversion of the joint. Functional ankle braces with the best evidence of effectiveness for the prevention and treatment of ankle sprains include the soft lace-up ankle brace (Figure 5) and semirigid air stirrup brace (Figure 6). Many lace-up ankle braces also have straps to provide additional support. The semirigid air stirrup brace has thermoplastic lateral stirrups lined with foam, gel, or air compartments along the medial and lateral malleoli.
FIGURE 5

Soft lace-up ankle brace for acute ankle sprains.
FIGURE 6
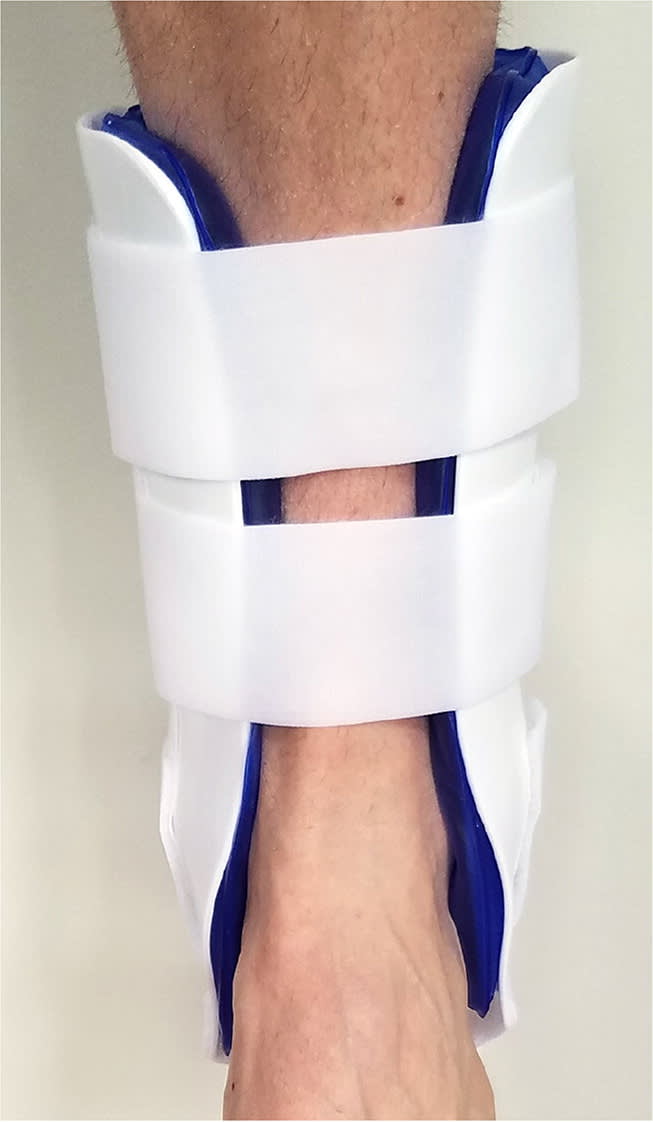
Semirigid air stirrup brace for acute ankle sprains.
One RCT showed that the use of a semirigid air stirrup brace for 12 months was superior to an eight-week neuromuscular training program for the prevention of recurrent ankle sprains.17 In another RCT, the air stirrup brace outperformed an elastic compression wrap in terms of functional outcomes up to one month after acute lateral ankle sprains.18 This is consistent with findings of a Cochrane review, which concluded that air stirrup braces and lace-up ankle braces are more effective than elastic compression wraps in reducing the time to return to physical activity.19 Other studies found no significant differences between various types of braces for the prevention of inversion ankle sprains.20 Although ankle taping can be effective for preventing ankle sprains, braces may be more practical, consistent, and cost-effective.20,21 There is insufficient evidence to determine how long an ankle brace should be worn to prevent reinjury after an acute ankle sprain.1
Thumb Spica Splints
The thumb spica splint immobilizes the thumb by crisscrossing layers of material around it. Thumb spica splints are used for a multitude of thumb and wrist injuries and disorders, and are available in three common forms: thermoplastic (custom-fitted), prefabricated (Figure 7A), and fiberglass (Figure 7B). A trial of conservative management for thumb carpometacarpal OA concluded that prefabricated thumb spica splints are generally more comfortable, less expensive, and as effective as thermoplastic splints.22
FIGURE 7
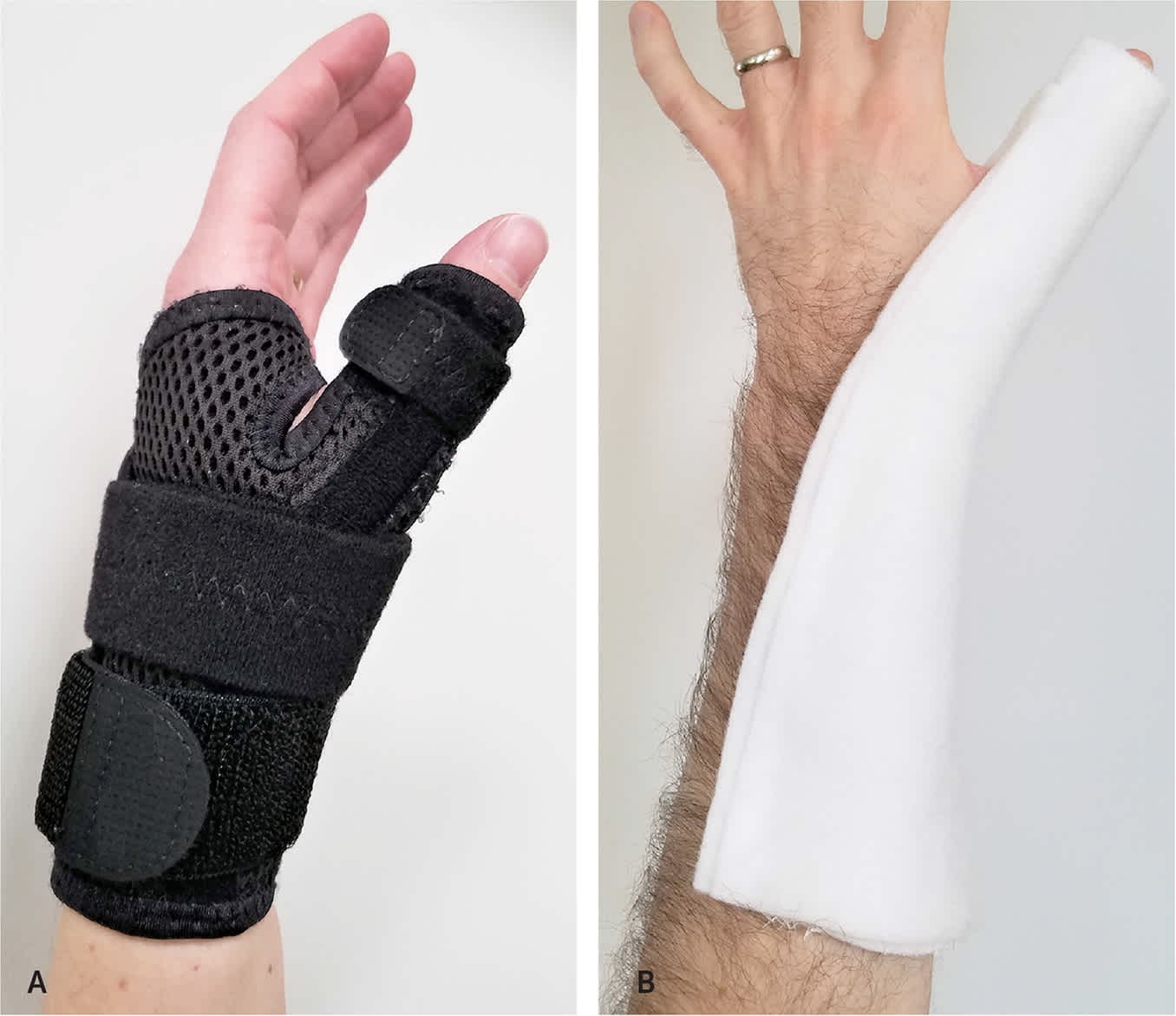
Thumb spica splints. (A) Prefabricated. (B) Fiberglass.
THUMB CARPOMETACARPAL OA
One of the most common forms of OA involves the thumb carpometacarpal joint, with an overall prevalence of 15%.23 Management is challenging because of the unique joint anatomy and its disabling features when symptomatic. Most data supporting thumb spica splinting for OA are based on case reports and observational studies. However, two systematic reviews evaluating the use of splints for thumb carpometacarpal OA showed that they improved pain scores, particularly in the long term (longer than three months, up to seven years).24,25 A seven-year prospective study showed that 70% of patients awaiting surgery for thumb carpometacarpal OA were able to postpone or avoid surgery after conservative treatment with joint protection and splinting.26
DE QUERVAIN TENOSYNOVITIS
The etiology of de Quervain tenosynovitis is unknown, but it has been attributed to overuse or repetitive movements of the wrist or thumb. This condition is typically self-limiting, and the prognosis is generally good. Evidence in support of splinting is mostly observational. RCTs evaluating the effectiveness of splinting in conjunction with glucocorticoid injections have shown some benefit.27 A retrospective study comparing splinting plus nonsteroidal anti-inflammatory drugs, splinting plus glucocorticoid injections, and injections alone for patients with de Quervain tenosynovitis found that 88% of patients with mild symptoms improved with splinting; however, once symptoms progressed to moderate or severe, the success rate of splinting plus anti-inflammatory drugs dropped to 32%.28
SCAPHOID FRACTURES
Scaphoid fractures are one of the most common wrist injuries, accounting for up to 70% of all carpal bone fractures.29 The diagnosis should be considered in patients with radial wrist pain resulting from a fall on an outstretched hand, even if initial radiographic findings are normal. Immobilization with a thumb spica splint is the mainstay of treatment for nondisplaced fractures. Although permanent casting is ultimately performed in most cases, splinting is not circumferential and offers some benefit in the immediate postinjury period, when swelling may progress.
Wrist Splints
Carpal tunnel syndrome results from a compressive force to the median nerve at the wrist and has a prevalence of 5% to 16%.30 Wrist splints (Figure 8) are one of the simplest and safest means to treat mild to moderate carpal tunnel syndrome. These splints immobilize the wrist and decrease pain and numbness by decreasing carpal tunnel pressure. However, the optimal wrist position is debatable, with limited evidence favoring the neutral position.31,32
FIGURE 8

Wrist splint for carpal tunnel syndrome.
One RCT of 120 patients showed that wrist splints resulted in symptomatic and functional improvement in carpal tunnel syndrome over three months.33 Similarly, three systematic reviews provided evidence of short-term effectiveness, but one of these found surgical intervention to be superior to splinting in the long term.34–36 Another systematic review concluded that there is limited evidence that wearing a splint at night is superior to no treatment, but that there is insufficient evidence to recommend wrist splinting over other nonsurgical interventions.37
This article updates previous articles on this topic by Gravlee and Van Durme,1 and by Paluska and McKeag.38
Data Sources: Searches were completed primarily in PubMed using the key terms medial knee osteoarthritis, medial unloading brace, patellofemoral pain syndrome, patellar tendinopathy, ankle sprain, brace, de Quervain tenosynovitis, thumb osteoarthritis, and carpal tunnel syndrome. The Cochrane Database of Systematic Reviews, Database of Abstracts of Reviews and Effects, and BMJ Clinical Evidence were also searched. Search results included meta-analyses, systematic reviews, randomized controlled trials, and other trials/reviews. Search dates: October 2017 to July 2018.
The authors thank Wayne Berry, MD, for writing assistance, and Gretchen Sprouse, MD, for assistance with the figures and tables.

