The United States has the highest incarceration rate of any nation in the world. Approximately 870 of every 100,000 U.S. citizens are currently in jails or prisons. U.S. inmates are disproportionately young males, racial and ethnic minorities, and persons of low socioeconomic status. Incarcerated persons have high rates of psychiatric conditions, communicable diseases, substance use disorders, and chronic diseases. The U.S. Preventive Services Task Force recommends that all inmates be screened for human immunodeficiency virus infection, hepatitis C, syphilis, and latent tuberculosis infection, and that sexually active female inmates be screened for gonorrhea and chlamydia. Inmates should also be screened for psychiatric conditions and substance use disorders. Therapy should be continued for all chronic conditions when indicated. Inmates should be referred to community organizations for follow-up medical care and treatment of substance use disorders before they are released from detention facilities. A systematic approach to urgent, routine, and preventive care for persons in jails and prisons creates a healthier correctional environment and a healthier community after release.
Approximately 870 of every 100,000 U.S. adult citizens are in jail or prison, which represents the highest incarceration rate in the world.1 Incarcerated persons are guaranteed a right to health care by the 1976 U.S. Supreme Court decision Estelle v. Gamble.2 Although the type and quality of health care services for incarcerated persons differ because of variations in policies, budgets, and staffing across federal, state, and local jurisdictions, such care benefits individuals, their institutional communities, and their home communities after release.
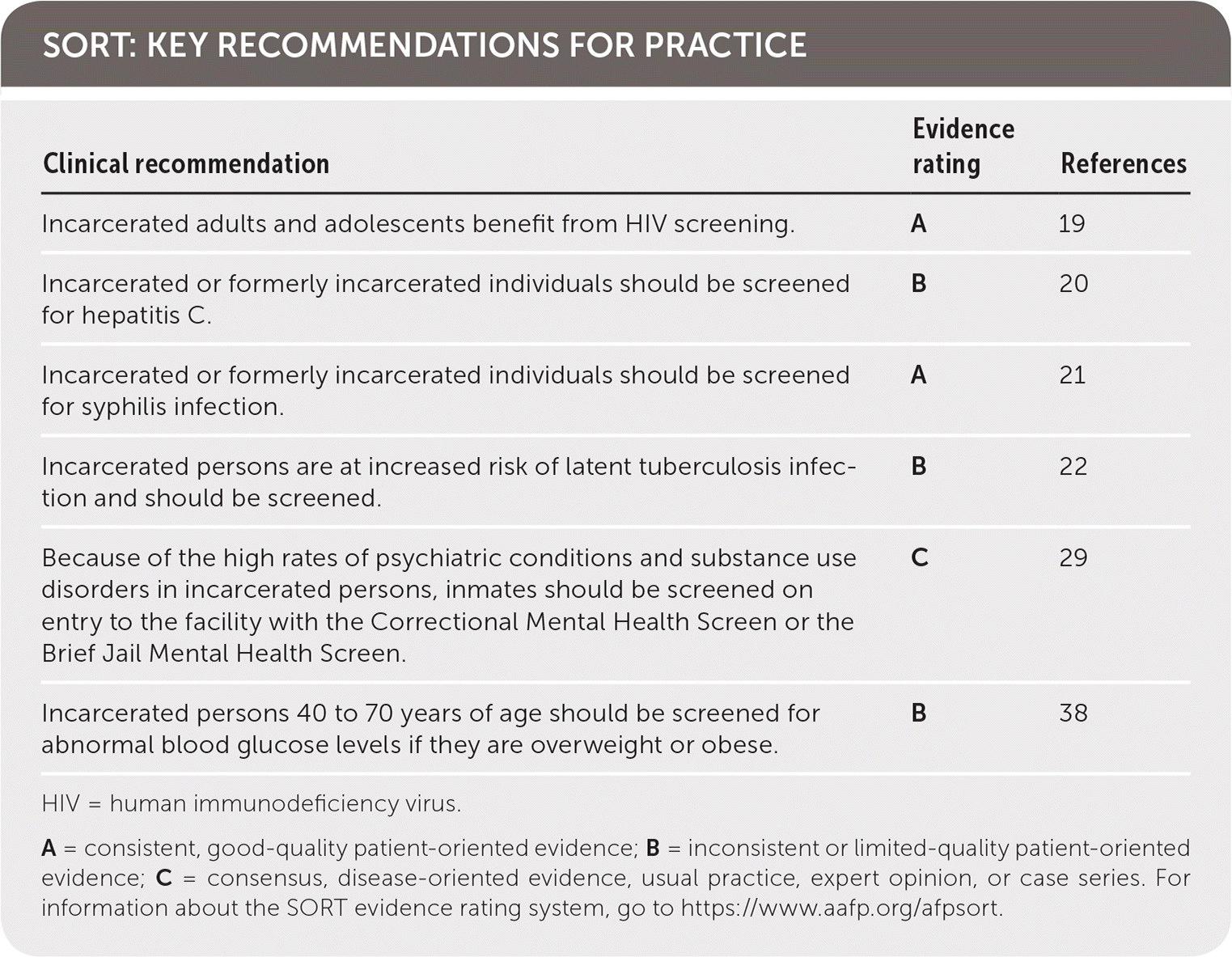
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Incarcerated adults and adolescents benefit from HIV screening. | A | 19 |
| Incarcerated or formerly incarcerated individuals should be screened for hepatitis C. | B | 20 |
| Incarcerated or formerly incarcerated individuals should be screened for syphilis infection. | A | 21 |
| Incarcerated persons are at increased risk of latent tuberculosis infection and should be screened. | B | 22 |
| Because of the high rates of psychiatric conditions and substance use disorders in incarcerated persons, inmates should be screened on entry to the facility with the Correctional Mental Health Screen or the Brief Jail Mental Health Screen. | C | 29 |
| Incarcerated persons 40 to 70 years of age should be screened for abnormal blood glucose levels if they are overweight or obese. | B | 38 |
HIV = human immunodeficiency virus.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
For the purposes of this article, the incarcerated population refers to persons held in local jails or under the jurisdiction of state or federal prisons. Jails, which are under county or municipal jurisdiction, house persons awaiting trial, sentencing, or transfer to another facility; those who have violated parole or probation; and those who have been sentenced to less than one year in custody. State and federal facilities house persons who have been sentenced to more than one year in custody. This article does not address juveniles in custody or adults in immigration detention facilities, territorial prisons, military facilities, or tribal justice facilities.
Demographics
In 2015, the U.S. correctional population included more than 2.1 million adults in jails and prisons, and 4.66 million adults supervised on probation or parole.1 The average daily population of jail inmates in 2015 was 721,300, but because of high turnover rates, there were 10.9 million admissions into jails.3 About 27% of jail inmates are held for misdemeanor offenses, and 63% have not been convicted of a crime.3 The U.S. inmate population is heavily skewed toward young males, racial and ethnic minorities, and persons of low socioeconomic status.4 Before incarceration, these persons often reside in communities with high rates of poverty, unemployment, family disruption, and racial segregation.5
As of 2015, non-Hispanic black males comprised the largest population of prisoners (37%) under state or federal jurisdiction.6 Black and Hispanic persons are incarcerated in state prisons at 5.1 and 1.4 times the rate of whites, respectively.7 Women and persons older than 55 years account for smaller but increasing percentages of the incarcerated population (7% and 11%, respectively).6 Approximately 10% of all jail, state, and federal inmates are military veterans,8 and 12% to 16% were homeless in the past or at the time of their incarceration.9,10
Initial Approach
The National Commission on Correctional Health Care and the American Correctional Association provide guidelines for the accreditation of jails, prisons, and detention centers, and processes described in this article are consistent with recommendations from these organizations. Detention facilities are not considered licensed health care entities; thus, accreditation is not mandatory. Most U.S. jails, prisons, and detention facilities are not accredited.
Intake screening should be performed for all inmates on arrival at a facility to ensure that they are healthy enough for incarceration. This process, termed a fit for confinement examination, should be done as soon as possible, particularly in a jail setting.11,12 Inmates who are not considered fit for confinement should be transferred to an emergency department for further evaluation. Intake screening usually involves a structured interview and limited examination by a health professional, but it can be completed by a trained correctional staff member. The intake health assessment is a more thorough evaluation that includes medical, dental, and mental health histories and a physical examination. It is completed by a physician, nurse practitioner, physician assistant, or specially trained nurse and should be performed within 14 days of admission to jail or within seven to 14 days of admission to prison. Intake health assessments are opportunities to perform tuberculosis and other health screenings.
Prison and jail facilities have varying levels of medical care for inmates. Clinic visits are held in prisons and some larger jails to address acute or chronic medical problems. Some facilities have continuity clinics for those with chronic illnesses. An infirmary is available in most prisons and many large jails for patients who are ill enough to require daily nursing care. Infirmary stays may be provided for recent transfers from hospitals, patients undergoing acute withdrawal symptoms, and those who cannot perform their own self-care. Some facilities have psychiatric infirmaries to house patients who are acutely homicidal or suicidal, or who are starting a new medication.
Medical Conditions in Inmates
Communicable diseases, psychiatric illness, and noncommunicable diseases are common within the U.S. prison population (Table 1).13–15
TABLE 1. Common Medical Conditions in Jail Inmates and State and Federal Prisoners

| Condition | Jail inmates (%) | State and federal prisoners (%) |
|---|---|---|
| Drug dependence or abuse13 | 63.3 | 58.5 |
| Overweight, obesity, or morbid obesity14 | 62 | 74 |
| History of mental health disorder15 | 44.3 | 36.9 |
| Hypertension14 | 26.3 | 30.2 |
| Asthma14 | 20.1 | 14.9 |
| History of infectious disease14 | 14.3 | 21 |
| Arthritis or rheumatism14 | 12.9 | 15 |
| Heart conditions14 | 10.4 | 9.8 |
| Diabetes mellitus or high blood glucose levels14 | 7.2 | 9 |
COMMUNICABLE DISEASES
The U.S. inmate population has higher rates of nearly every infectious disease compared with the general population. In 2015, the rate of human immunodeficiency virus (HIV) infection in inmates housed in state and federal facilities was 1,297 cases per 100,000 persons16; the rate among the general U.S. population was 299.5 cases per 100,000 persons.17 In 2013, the annual incidence of tuberculosis in jail inmates and federal prisoners was eight times that in the overall U.S. population.18 Nearly one-half of inmates diagnosed with tuberculosis while in custody were born outside the United States (primarily in Mexico and Central America).18 Because of the increased risk of infection in the correctional population, the U.S. Preventive Services Task Force (USPSTF) recommends that inmates be screened for HIV infection,19 hepatitis C,20 syphilis,21 and latent tuberculosis.22 It also recommends that inmates be given behavioral counseling interventions to prevent sexually transmitted infections.23 The World Health Organization recommends that condoms be distributed in prisons to decrease the transmission of HIV and other sexually transmitted infections,24 but only two states (California and Vermont) require condoms to be available to inmates.16,17,25
PSYCHIATRIC ILLNESS AND SUBSTANCE ABUSE
The number of U.S. inmates with symptoms or a diagnosis of psychiatric illness is significantly higher than in the general population; estimates vary from 37% to 60% of inmates.13,26 Psychiatric conditions increase the risk of being placed in solitary confinement,27 being assaulted while incarcerated,26 engaging in self-harming behaviors (including suicide),27 and of recidivism.28 On arrival to a correctional facility, inmates should be screened with the Correctional Mental Health Screen or the Brief Jail Mental Health Screen,29 and those who screen positive should be referred for further mental health evaluation.29 Medical records should be requested for inmates with known psychiatric diagnoses. Psychoactive medications should be continued without interruption once previous prescriptions have been verified. Many inmates report substance use disorders.30,31 They should be evaluated on admission for substance use history. Many large urban jails have standing orders for alcohol, opioid, and benzodiazepine detoxification. Medical treatment for substance use disorders, including methadone or buprenorphine, is often unavailable in correctional institutions.32,33 Substance abuse education is most commonly provided to inmates with substance use disorders or addiction problems.30,32 Because of high relapse rates, inmates with opioid use disorders should be referred to appropriate community-based medication-assisted therapy on release from correctional facilities. A recent systematic review concluded that compared with referral to community treatment for substance use disorder, extended-release naltrexone administered before release decreases opioid use in adults under criminal justice supervision. Extended-release naltrexone can be prescribed by any licensed clinician.34
CHRONIC CONDITIONS
Chronic diseases are common among inmate populations. Medical records should be requested from the inmate's primary care clinician to ensure continuity of care, and therapy should be continued for all chronic conditions. Certain chronic conditions may be exacerbated by excess calories and sodium in prison diets, lack of physical activity, and psychological stress associated with incarceration.35–37 Physicians should screen for obesity and diabetes mellitus in accordance with USPSTF recommendations for the general population.38 Preventive medications, including statins and aspirin, should also be provided based on USPSTF recommendations.
Special Needs of Incarcerated Females
The female jail population is the fastest growing correctional population, increasing by 18% between 2010 and 2014.39 Female inmates have a higher prevalence of chronic medical conditions, psychiatric conditions, and substance use disorders compared with male inmates.40 Incarcerated women have disproportionate rates of chlamydia and gonorrhea compared with incarcerated males and the general population, and females in juvenile correctional facilities have the highest rates.41 The USPSTF recommends that all sexually active incarcerated women be screened for gonorrhea and chlamydia using nucleic acid amplification testing.42 Incarcerated women also have higher rates of cervical cancer than women in the general population.43,44 Most have experienced childhood physical or sexual abuse, which is strongly linked to substance use disorders later in life,45,46 as well as increased risk of physical and sexual victimization by other inmates or staff.47,48
Addressing the reproductive health needs of incarcerated women is an essential component of health care delivery in adult and juvenile correctional settings. On average, 6% to 10% of incarcerated women are pregnant, with the highest rates in local jails.49 Incarcerated women are at risk of poor maternal and infant health outcomes because of the high rate of comorbid medical conditions in this population. Incarcerated women are also at high risk of unintended pregnancy; in one study, more than 80% of incarcerated women reported that they had had an unintended pregnancy.49 All female inmates should undergo a reproductive health evaluation and be provided with any indicated contraceptive and/or preconception health services (Figure 1).50–52 Preventive health services specific to women include screening for gonorrhea and chlamydia,42 cervical cancer,53 and breast cancer.54 These services should be provided based on USPSTF guidelines, which are endorsed by the American Academy of Family Physicians.55 In a jail setting, Papanicolaou testing and mammography should be ordered only if results will be obtained before release.
FIGURE 1
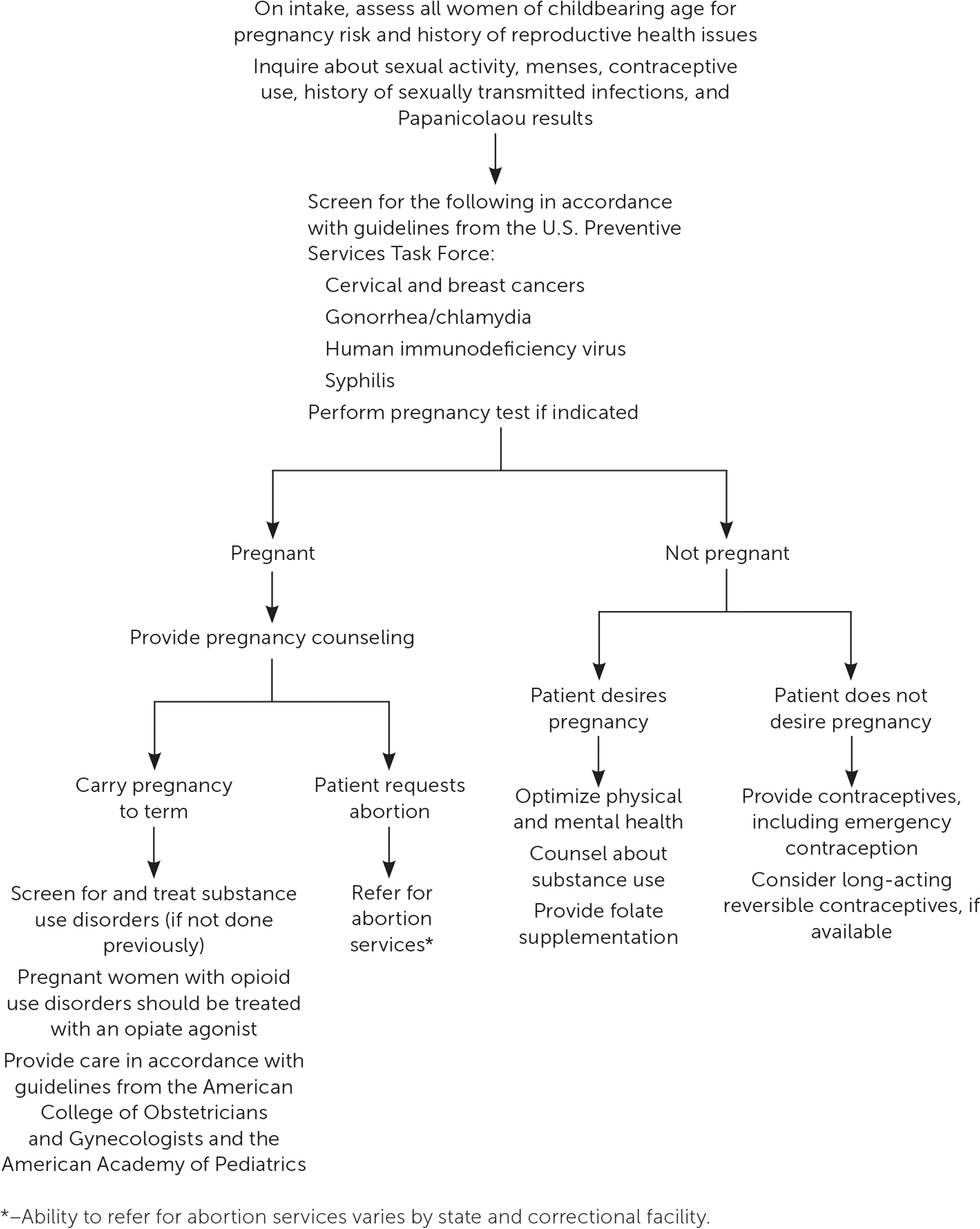
Reproductive health assessment for female correctional inmates.
Information from references 50 through 52.
Reentry to the Community
Persons recently released from incarceration have high levels of poverty, unemployment, and homelessness.56 Former inmates with medical or psychiatric conditions or substance use disorders face distinct challenges in finding housing and employment, reconnecting with family members, abstaining from substance use, and avoiding a return to prison.57 The American Correctional Association recommends that health professionals encourage continuity of care from admission to facility transfer or discharge.58 Discharge planning for inmates with serious health needs should include providing linkages between the facility and community-based organizations, assisting with scheduling appointments, and arranging medications for the patient at release.12 Despite these recommendations, most inmates are discharged from correctional facilities without a supply of medications or referrals to primary care, mental health services, or substance abuse treatment.59–61 Lack of care coordination directly affects the health of former inmates. In the two weeks following release, former inmates are 129 times more likely to die of a drug overdose and 12 times more likely to die of any cause than members of the general public.56
Many local reentry programs have been established. The Transitions Clinic Network, a primary care–based complex care management program serving formerly incarcerated persons with chronic health problems, has been well studied.62,63 Transitions clinics, which are embedded into preexisting community health centers, offer primary care services from clinicians who have experience working with corrections populations and case management from community health workers with a personal history of incarceration.63 Transitions clinics are currently located in 11 states and Puerto Rico. A 2012 study demonstrated that chronically ill persons leaving correctional facilities will engage with primary care via these clinics when they are provided access, which leads to a decrease in emergency department utilization.62 Other studies have shown excellent six-month retention rates for patients with HIV infection, but lower rates among patients with hypertension, diabetes, and opioid use disorders.64
Model for Provision of Care: An Opportunity for Family Physicians
A consistent approach is recommended for providing health services that address urgent, chronic, and infectious conditions in incarcerated persons. An ideal model for delivering health services in a correctional facility includes:
- Intake services that screen for physical and behavioral health conditions, as well as common infectious diseases
- Interprofessional health services that include acute and chronic care, behavioral and substance abuse care, dental care, and social services
- Reentry services that optimize continuity of care, patient self-management, and connecting patients with health services in their community.
The care of incarcerated populations requires judicious use of limited resources and creative collaborations. Table 2 lists evidence-based resources that can assist physicians in providing high-quality care for incarcerated individuals and their communities.
TABLE 2. Evidence-Based Correctional Health Care Resources for Physicians
| Resource | Website | |
| American Academy of Family Physicians | ||
| Incarceration and Health: A Family Medicine Perspective | https://www.aafp.org/about/policies/all/incarcerationandhealth.html | |
| American College of Correctional Physicians | http://accpmed.org/links.php | |
| American College of Obstetricians and Gynecologists | ||
| Health Care for Pregnant and Postpartum Incarcerated Women and Adolescent Females | https://www.acog.org/Clinical-Guidance-and-Publications/Committee-Opinions/Committee-on-Health-Care-for-Underserved-Women/Health-Care-for-Pregnant-and-Postpartum-Incarcerated-Women-and-Adolescent-Females | |
| Reproductive Health Care for Incarcerated Women and Adolescent Females | https://www.acog.org/Clinical-Guidance-and-Publications/Committee-Opinions/Committee-on-Health-Care-for-Underserved-Women/Reproductive-Health-Care-for-Incarcerated-Women-and-Adolescent-Females | |
| American Correctional Association | http://www.aca.org | |
| Center for Prisoner Health and Human Rights | http://www.prisonerhealth.org/ | |
| Centers for Disease Control and Prevention | ||
| Correctional Health (includes links to state resources) | https://www.cdc.gov/correctionalhealth/ | |
| Federal Bureau of Prisons Health Management Resources (includes guidelines for management of 35 conditions) | https://www.bop.gov/resources/health_care_mngmt.jsp | |
| National Commission on Correctional Health Care | https://ncchc.org | |
| Guide to Developing and Revising Alcohol and Opioid Detoxification Protocols | https://www.ncchc.org/filebin/Resources/Detoxification-Protocols-2015.pdf | |
| Managing Opiate Withdrawal: The WOWs Method (opioid withdrawal scale and management recommendations) | https://www.ncchc.org/filebin/CorrectCare/30-3-WOWS.pdf | |
| Substance Abuse and Mental Health Services Administration | ||
| Guidelines for Successful Transition of People with Mental or Substance Use Disorders from Jail and Prison: Implementation Guide | https://knowledge.samhsa.gov/resources/transition-people-mental-substance-use-disorders-jail-prison | |
| Medications for Opioid Use Disorder (reviews pharmacotherapy for opioid use disorder and provides resources for clinicians and patients) | https://store.samhsa.gov/product/tip-63-medications-opioid-use-disorder-%E2%80%93-full-document-including-executive-summary-parts-1-5 | |
| World Health Organization | ||
| Health in Prisons: A WHO Guide to the Essentials in Prison Health | http://www.euro.who.int/__data/assets/pdf_file/0009/99018/E90174.pdf | |
Data Sources: The following data sources were searched in the preparation of this manuscript: the Cochrane database, Agency for Healthcare Research and Quality evidence reports, the Bureau of Justice Statistics website, the U.S. Preventive Services Task Force, and PubMed. The search terms included care of inmates and prisoners. The initial search took place on April 15, 2017. Additional PubMed searches were done in July and August 2017 and August 2018.

