Conduct disorder is a psychiatric syndrome that most commonly occurs in childhood and adolescence. It is characterized by symptoms of aggression toward people or animals, destruction of property, deceitfulness or theft, and serious violations of rules. Risk factors include male sex, maternal smoking during pregnancy, poverty in childhood, exposure to physical or sexual abuse or domestic violence, and parental substance use disorders or criminal behavior. At least three symptoms should have been present in the past 12 months, with at least one present in the past six months to diagnose conduct disorder. Interventions consist of treating comorbid conditions such as attention-deficit/hyperactivity disorder; supporting clear, direct, and positive communication within the family; and encouraging the family and youth to connect with community resources. There are several evidence-based psychosocial interventions that a psychologist or therapist may implement as part of long-term treatment. Currently, no medications have been approved by the U.S. Food and Drug Administration to treat conduct disorder. Treatment with psychostimulants is highly recommended for patients who have both attention-deficit/hyperactivity disorder and conduct problems. There is some evidence to support the treatment of conduct disorder and aggression with risperidone, but health care professionals should weigh the medication's potential benefits against its adverse metabolic effects.
Conduct disorder is a psychiatric syndrome that most commonly occurs during childhood and adolescence. Conduct disorder is characterized by repetitive, persistent violations of both the rights of others and age-appropriate societal norms. The Diagnostic and Statistical Manual of Mental Disorders, 5th ed. (DSM-5), outlines 15 possible criteria for conduct disorder in the categories of aggression toward people or animals, destruction of property, deceitfulness or theft, and serious violations of rules (Table 1).1 The estimated lifetime prevalence of conduct disorder in the United States is 9.5%, with a lifetime prevalence of 12% for males and 7.1% for females.2
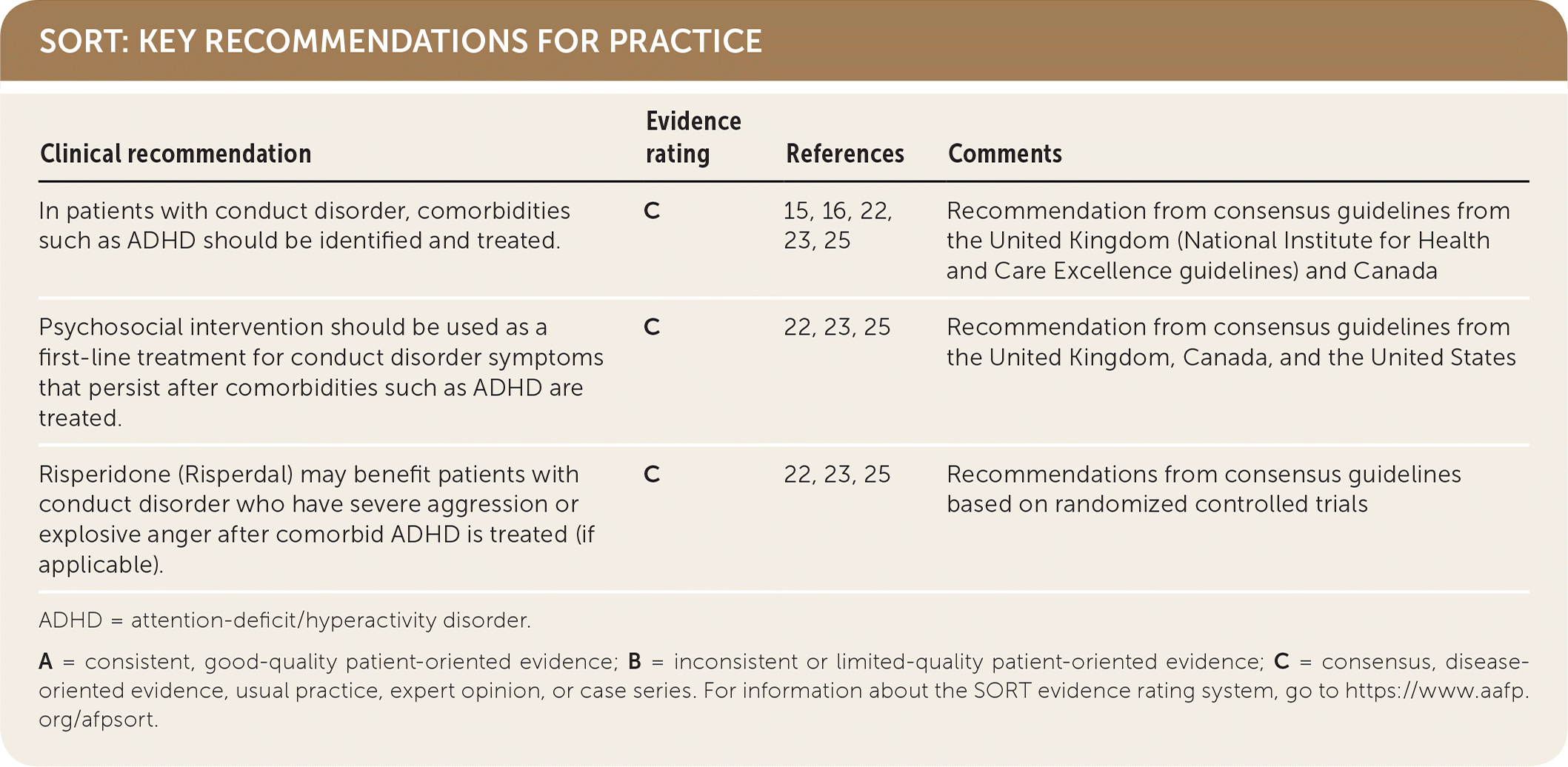
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
| In patients with conduct disorder, comorbidities such as ADHD should be identified and treated. | C | 15, 16, 22, 23, 25 | Recommendation from consensus guidelines from the United Kingdom (National Institute for Health and Care Excellence guidelines) and Canada |
| Psychosocial intervention should be used as a first-line treatment for conduct disorder symptoms that persist after comorbidities such as ADHD are treated. | C | 22, 23, 25 | Recommendation from consensus guidelines from the United Kingdom, Canada, and the United States |
| Risperidone (Risperdal) may benefit patients with conduct disorder who have severe aggression or explosive anger after comorbid ADHD is treated (if applicable). | C | 22, 23, 25 | Recommendations from consensus guidelines based on randomized controlled trials |
ADHD = attention-deficit/hyperactivity disorder.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
TABLE 1. DSM-5 Diagnostic Criteria for Conduct Disorder

|
DSM = Diagnostic and Statistical Manual of Mental Disorders.
Reprinted with permission from the American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th ed. Washington, DC: American Psychiatric Association; 2013:469–471.
Risk Factors
Risk factors for developing conduct disorder include male sex, maternal smoking during pregnancy, living in poverty in childhood, and parental conditions such as substance use disorders and criminal behavior. Additional risk factors are exposure to physical or sexual abuse in childhood, or to domestic violence between parents. Family instability, specifically changes in parent or guardian figures, is a risk factor, as are lower cognitive ability and association with peers who use substances, are truant from school, or engage in criminal activity.3,4 Additionally, children who experience harsh discipline, have parents with a cruel or rejecting attitude,4 have poor health, and who are not brought to visit other people who have children are at a higher risk for developing conduct disorder.5
Clinical Presentation
For a formal diagnosis, the DSM-5 specifies that at least three of 15 criteria should have been present in the past 12 months, with at least one criterion present in the past six months.1 Several rating scales can be used to screen for conduct disorder, including the Child Behavior Checklist, the Disruptive Behavior Disorders Rating Scale, and the National Institute for Children's Health Quality Vanderbilt Assessment Scales. The Vanderbilt Assessment Scales (parent and teacher versions) are used primarily to assess for attention-deficit/hyperactivity disorder (ADHD) and are commonly used in primary care. The Vanderbilt scales are available on several websites, such as www.nichq.org/resource/nichq-vanderbilt-assessment-scales. The Vanderbilt scales also include screening questions for disorders such as conduct disorder and oppositional defiant disorder (ODD). There are few data about the validity of the Vanderbilt scales in diagnosing conduct disorder, with one study finding that the Vanderbilt Parent Rating Scale had only a 67% sensitivity.6 Whether or not a rating scale is used, the diagnosis of conduct disorder is dependent on history. Physical findings during the visit and laboratory testing do not contribute to the diagnosis, although evidence of injuries may prompt a revelation of pertinent information, such as fighting.
Illustrative Cases
The following cases illustrate ways that conduct disorder may present in a family medicine setting. Such cases should prompt the health care professional to ask additional follow-up questions (Table 2).7
TABLE 2. Interview Questions to Assess for Conduct Disorder

| Have you ever skipped school? If so, how often? Under what circumstances? Have you been suspended or expelled from school? If so, what were the situations around that? |
| Have you ever gotten into any physical fights at school? If so, how many/how often? What led up to those fights? Have you gotten into physical fights in your neighborhood, or other places? |
| Have you gotten in trouble with the police? If so, were you arrested? Have there been any charges filed against you? If so, for what? Have you had other interactions with the police that did not lead to an arrest? If so, what happened? Have you engaged in any stealing? |
| Have you been in situations where you destroyed property? If so, what were the circumstances? Have you experimented with fire, or set any fires? If so, what was the situation? |
| Do you use alcohol? Do you use drugs? If so, how often? How much? |
| Are you sexually active? |
| Have there been times when you stayed out very late without permission? Have you stayed out all night? Have there been times when you have run away from home? |
Note: In assessing the answers to these questions, the family physician should prioritize safety. If the youth indicates that he or she is in imminent danger of harming others or of being harmed (e.g., by fire setting, fighting, or running away from home), the family physician should immediately involve parents and help them establish a safety plan, which would at a minimum involve increased monitoring at home and could even involve inpatient psychiatric hospitalization. If the youth answers yes to ANY of the above questions, the family physician should try to engage the youth around possible reasons to change behavior, discuss the concern with parents, and encourage ongoing communication within the family and with other health professionals. Not all of the above questions may be age-appropriate. The physician should choose which questions to ask based on age and context.
Adapted with permission from Searight HR, Rottnek F, Abby SL. Conduct disorder: diagnosis and treatment in primary care. Am Fam Physician. 2001;63(8):1583.
CASE 1
A seven-year-old boy presents for a well-child visit. He walks around the office, occasionally picking up objects or opening drawers, as his mother describes his recent suspension from school for pushing other children. The boy threatened to stab another child, stole items from classmates' lunches, and is suspected of stealing money from the teacher's purse. He once left the school premises without permission, prompting a call to police. At home, he often fights with siblings and has thrown rocks at other children. He seems to barely pay attention to the telling of his history and does not contradict any of his mother's statements. His mother reports feeling overwhelmed because of his behaviors and mentions that his father is incarcerated. She states that her relatives are taking turns coming to the home and are trying to help her control his behaviors.
CASE 2
A 14-year-old girl presents at the end of the summer for a required school physical. She becomes irritated as her mother tearfully relates that her daughter has been smoking tobacco and marijuana cigarettes and has left home overnight on several occasions. The girl describes school as “boring and stupid” and reports that she has skipped school on several occasions to go hang out at a lake. This summer she was arrested for shoplifting clothes and jewelry and was also charged with marijuana possession. As her mother mentions that her daughter received probation, the girl retorts that if her mother had money to buy clothes she would not have to steal them. The girl adds that her mother is jealous because she has friends, but her mother spends her time alone.
Differential Diagnosis and Comorbidity
The differential diagnosis of conduct disorder includes screening for other disorders in which aggression or disruptive behaviors may be present (Table 3),1 such as ODD, ADHD, mood disorders, and adjustment disorders. In terms of comorbidities, conduct disorder is often associated with ADHD, ODD, and substance use disorders. Approximately 16% to 20% of youth with conduct disorder have comorbid ADHD.8 More than one-half of patients who receive a diagnosis of conduct disorder have never received a previous diagnosis of ODD9; however, approximately 60% of patients with conduct disorder concurrently meet full criteria for ODD.10 In youth, the combination of conduct disorder and ADHD may indicate a greater likelihood of tobacco and alcohol use than conduct disorder alone.11
TABLE 3. Differential Diagnosis of Conduct Disorder

| Diagnosis | Features |
|---|---|
| Oppositional defiant disorder | There is a pattern of opposition and defiance to adults, but no pattern of violation of the rights of others, aggression, property destruction, or deceitfulness or theft. |
| Intermittent explosive disorder | Although there may be aggression, it is impulsive rather than planned or predatory. |
| Attention-deficit/hyperactivity disorder | There may be aggression, but it is impulsive, and there may be intrusiveness and hyperactivity, but there is no pattern of violation of the rights of others. |
| Disruptive mood dysregulation disorder | There may be aggression as part of temper outbursts, but unlike conduct disorder, the primary pattern is of irritability and temper outbursts, whether or not aggression is involved, rather than violation of the rights of others. |
| Major depressive disorder or persistent depressive disorder | The primary symptom is typically depressed mood, and there may be changes in sleep, appetite, and energy level, as well as suicidal ideation. These disorders do not involve aggression, property destruction, or deceitfulness or theft. |
| Bipolar disorders (bipolar I, bipolar II, unspecified bipolar disorder) | In addition to grandiosity there may be periods of impulsivity, but this occurs as part of a manic episode rather than a persistent pattern. |
| Adjustment disorders (with depressed mood, with disturbance of conduct, with mixed disturbance of emotions and conduct) | There may be irritability and disruptive behaviors, but these occur in response to a stressor and typically resolve within six months of elimination of the stressor. |
| Substance use disorders | There may be disruptive behaviors in the context of intoxication or withdrawal, but the disruptive behaviors should resolve in the absence of these conditions. |
| Posttraumatic stress disorder | The primary symptom is typically reexperiencing trauma in the form of nightmares or intrusive memories. There are efforts to avoid reminders of the trauma. There may be irritability and outbursts. Unlike conduct disorder, there is no pattern of violation of the rights of others, property destruction, or deceitfulness or theft. |
Information from reference 1.
Antisocial personality disorder develops in 45% to 70% of adolescents with conduct disorder.12 A relationship exists between the number of conduct disorder symptoms and an increased risk of most psychiatric disorders, including depression and anxiety.12 The combination of early onset alcohol abuse and conduct disorder is associated with the highest risk of personality disorders, particularly antisocial/borderline comorbidity, and predicts violent crime and drug use.13 Conduct disorder is also associated with failure to complete high school, drug use, and criminal behavior.14
In adults, conduct disorder is associated with other psychiatric disorders, and a history of conduct disorder alone has an increased risk of developing an alcohol use disorder (78% in men, 65% in women) or drug use disorder (48% in men, 46% in women).12
Interventions
Treatment for conduct disorder is multifaceted and involves treatment of comorbidities, family support, psychosocial interventions, and pharmacotherapy for some patients (Table 4).7 ADHD is a common comorbidity that must be addressed because it can adversely impact outcomes.15,16 Although the family physician may be the initial point of contact for the family, it is helpful to refer the patient immediately to a psychologist for psychosocial interventions and to a psychiatrist for treatment of psychiatric comorbidities.
TABLE 4. Practical Interventions for the Treatment of Patients with Conduct Disorder

| Advise parents to treat their own physical and mental health issues, if applicable. |
| Assess severity and refer to a subspecialist for treatment as needed. |
| Demonstrate listening and communicating skills to parents and youth in clear, direct ways. |
| Emphasize parental monitoring of the youth's activities (e.g., where the youth is, who he/she is with). Encourage enforcement of curfews. |
| Encourage parents and youth to discuss rewards for appropriate behavior and consequences for misbehavior (such as staying out after curfew). Rewards and consequences should be discussed ahead of time, ideally in a session with a health care professional who can facilitate communication. |
| Encourage parents to coordinate with school personnel, including school social workers, around any concerns in the school setting. All professionals involved in treating the youth should coordinate care to ensure that all are aware of comorbidities, concerns, and approaches to treatment. |
| Encourage structuring of the youth's time and activities, including after school time, to minimize times when he or she is not monitored by a responsible adult such as a teacher, coach, or parent. |
| Ensure that comorbidities such as ADHD, substance use, and mood or anxiety disorders are treated. |
| If the youth has his or her own phone and social media account, encourage the parents and youth to review texts and social media posts together, with discussion about how the messages affect all parties involved. |
| Provide the parents and youth with options for healthy activities, such as sports teams, school clubs, church activities, community groups such as Scouts, and mentoring organizations such as Big Brothers Big Sisters of America. |
| Recommend that parents and youth establish a daily routine of engaging in play or an enjoyable activity together (e.g., playing a board game, playing catch, watching an appropriate television program). |
ADHD = attention-deficit/hyperactivity disorder.
Adapted with permission from Searight HR, Rottnek F, Abby SL. Conduct disorder: diagnosis and treatment in primary care. Am Fam Physician. 2001;63(8):1584.
FAMILY SUPPORT
The physician should emphasize the benefits of overall stress reduction in the home,17 warmth in parental interactions with the child, and avoidance of harsh discipline.18 The physician should also encourage the family to seek support from organizations such as the National Alliance on Mental Illness (www.nami.org), Big Brothers Big Sisters of America (www.bbbsa.com), and school or church groups that offer positive interactions and model appropriate behavior. Participation in high school sports can reduce the association between conduct disorder and adult antisocial behavior and could be considered an intervention to reduce the symptoms of conduct disorder.19 Parents should be empathic and modulate their own emotional expression in communication with their children who have been diagnosed with conduct disorder.20 The reasons for interventions such as attending appointments and establishing limits such as a curfew should be clearly explained. Parents should also be encouraged to treat their own mental health concerns.
PSYCHOSOCIAL INTERVENTIONS
The most recent U.S. expert guidelines were published in 1997,21 but clinical guidelines for antisocial behavior and conduct disorders were released in 2013 in the United Kingdom22 and in 2015 in Canada.23 Both the National Institute for Health and Care Excellence (NICE) and the Canadian guidelines recommend psychosocial interventions as first-line interventions for conduct disorder that persists after comorbidities such as ADHD are treated, as does a third set of guidelines, commonly known as the CERT (Center for Education and Research on Mental Health Therapeutics) guidelines.24 Evidence-based psychosocial treatment methods for disruptive behavior disorders, including conduct disorder, have been compiled in a booklet by the U.S. Department of Health and Human Services, Substance Abuse and Mental Health Services Administration (available at https://store.samhsa.gov/system/files/ebpspromisingpractices-idbd.pdf).25
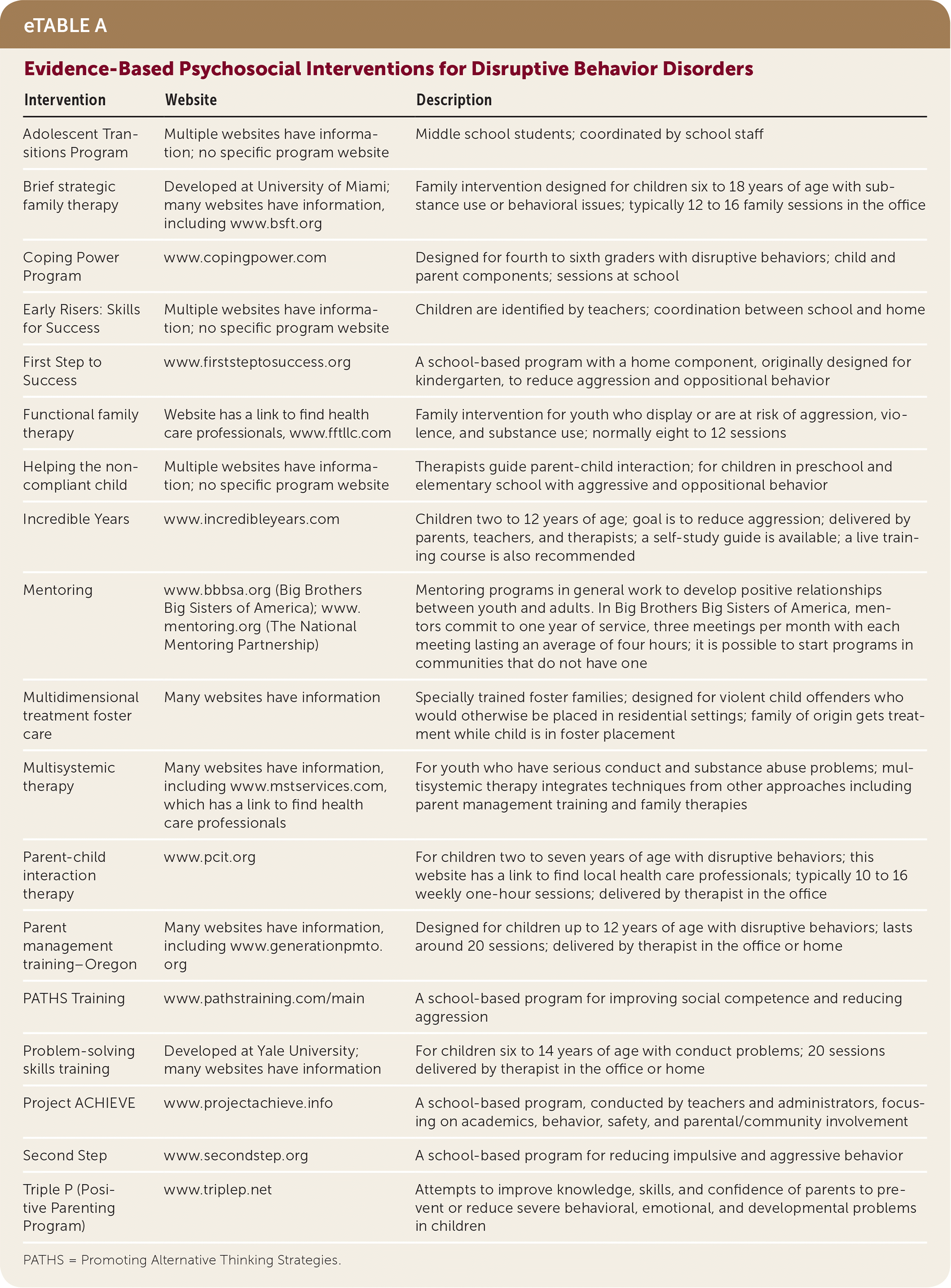
Most of these psychosocial treatment methods were developed at universities and are marketed toward systems such as school districts or health care systems, which often finance training through grants. The treatments take years to implement and therefore may not be accessible to most physicians. There are websites that provide links for finding local health care professionals who use these methods (eTable A). The physician may need to network with local psychologists and ask them if they treat conduct disorder, or collaborate with schools and determine whether they have a formal approach for treating conduct disorder.
eTABLE A Evidence-Based Psychosocial Interventions for Disruptive Behavior Disorders
| Intervention | Website | Description |
|---|---|---|
| Adolescent Transitions Program | Multiple websites have information; no specific program website | Middle school students; coordinated by school staff |
| Brief strategic family therapy | Developed at University of Miami; many websites have information, including www.bsft.org | Family intervention designed for children six to 18 years of age with substance use or behavioral issues; typically 12 to 16 family sessions in the office |
| Coping Power Program | www.copingpower.com | Designed for fourth to sixth graders with disruptive behaviors; child and parent components; sessions at school |
| Early Risers: Skills for Success | Multiple websites have information; no specific program website | Children are identified by teachers; coordination between school and home |
| First Step to Success | www.firststeptosuccess.org | A school-based program with a home component, originally designed for kindergarten, to reduce aggression and oppositional behavior |
| Functional family therapy | Website has a link to find health care professionals, www.fftllc.com | Family intervention for youth who display or are at risk of aggression, violence, and substance use; normally eight to 12 sessions |
| Helping the non-compliant child | Multiple websites have information; no specific program website | Therapists guide parent-child interaction; for children in preschool and elementary school with aggressive and oppositional behavior |
| Incredible Years | www.incredibleyears.com | Children two to 12 years of age; goal is to reduce aggression; delivered by parents, teachers, and therapists; a self-study guide is available; a live training course is also recommended |
| Mentoring | www.bbbsa.org (Big Brothers Big Sisters of America); www.mentoring.org (The National Mentoring Partnership) | Mentoring programs in general work to develop positive relationships between youth and adults. In Big Brothers Big Sisters of America, mentors commit to one year of service, three meetings per month with each meeting lasting an average of four hours; it is possible to start programs in communities that do not have one |
| Multidimensional treatment foster care | Many websites have information | Specially trained foster families; designed for violent child offenders who would otherwise be placed in residential settings; family of origin gets treatment while child is in foster placement |
| Multisystemic therapy | Many websites have information, including www.mstservices.com, which has a link to find health care professionals | For youth who have serious conduct and substance abuse problems; multisystemic therapy integrates techniques from other approaches including parent management training and family therapies |
| Parent-child interaction therapy | www.pcit.org | For children two to seven years of age with disruptive behaviors; this website has a link to find local health care professionals; typically 10 to 16 weekly one-hour sessions; delivered by therapist in the office |
| Parent management training–Oregon | Many websites have information, including www.generationpmto.org | Designed for children up to 12 years of age with disruptive behaviors; lasts around 20 sessions; delivered by therapist in the office or home |
| PATHS Training | www.pathstraining.com/main | A school-based program for improving social competence and reducing aggression |
| Problem-solving skills training | Developed at Yale University; many websites have information | For children six to 14 years of age with conduct problems; 20 sessions delivered by therapist in the office or home |
| Project ACHIEVE | www.projectachieve.info | A school-based program, conducted by teachers and administrators, focusing on academics, behavior, safety, and parental/community involvement |
| Second Step | www.secondstep.org | A school-based program for reducing impulsive and aggressive behavior |
| Triple P (Positive Parenting Program) | www.triplep.net | Attempts to improve knowledge, skills, and confidence of parents to prevent or reduce severe behavioral, emotional, and developmental problems in children |
PATHS = Promoting Alternative Thinking Strategies.
PHARMACOTHERAPY
No medications have been approved by the U.S. Food and Drug Administration (FDA) for the treatment of conduct disorder. The NICE guideline specifies “Do not offer pharmacological interventions for the routine management of behavioral problems in children and young people with ODD or conduct disorder.”22 This guideline recommends pharmacologic treatment only if indicated for concurrent ADHD, and recommends considering risperidone (Risperdal) as a short-term treatment for severe aggression or explosive anger after comorbid ADHD is treated (if applicable).22
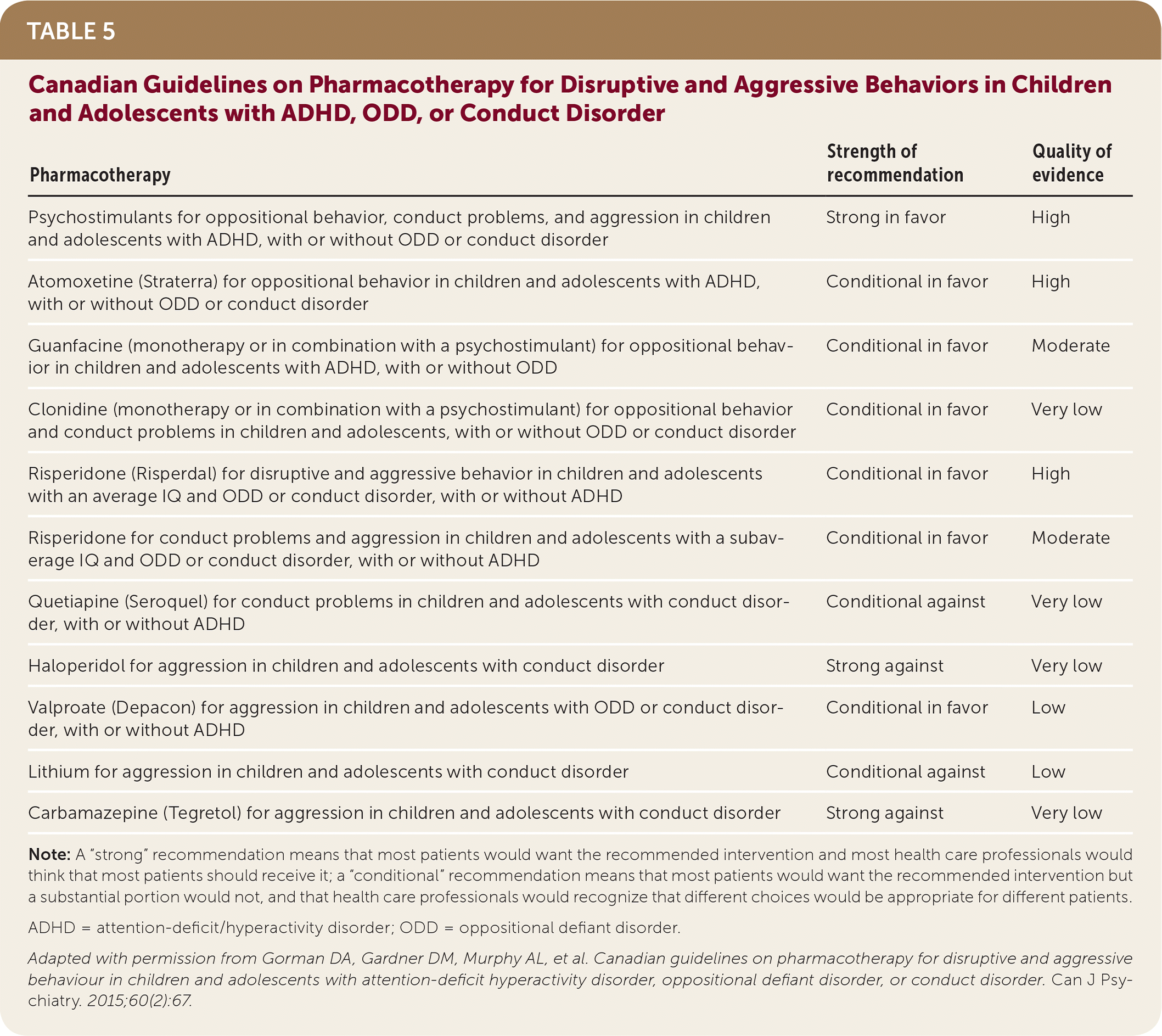
The Canadian guidelines provide a more detailed discussion of pharmacotherapy. They strongly recommend psychostimulants such as methylphenidate preparations or amphetamines for the treatment of oppositional behavior, conduct problems, and aggression in children and adolescents who have ADHD, with or without ODD or conduct disorder. No other medications receive a “strong” recommendation in the Canadian guidelines (Table 5).23 Atomoxetine (Strattera), guanfacine, and clonidine all receive conditional recommendations in favor of their use.23
TABLE 5. Canadian Guidelines on Pharmacotherapy for Disruptive and Aggressive Behaviors in Children and Adolescents with ADHD, ODD, or Conduct Disorder
| Pharmacotherapy | Strength of recommendation | Quality of evidence |
|---|---|---|
| Psychostimulants for oppositional behavior, conduct problems, and aggression in children and adolescents with ADHD, with or without ODD or conduct disorder | Strong in favor | High |
| Atomoxetine (Straterra) for oppositional behavior in children and adolescents with ADHD, with or without ODD or conduct disorder | Conditional in favor | High |
| Guanfacine (monotherapy or in combination with a psychostimulant) for oppositional behavior in children and adolescents with ADHD, with or without ODD | Conditional in favor | Moderate |
| Clonidine (monotherapy or in combination with a psychostimulant) for oppositional behavior and conduct problems in children and adolescents, with or without ODD or conduct disorder | Conditional in favor | Very low |
| Risperidone (Risperdal) for disruptive and aggressive behavior in children and adolescents with an average IQ and ODD or conduct disorder, with or without ADHD | Conditional in favor | High |
| Risperidone for conduct problems and aggression in children and adolescents with a subaverage IQ and ODD or conduct disorder, with or without ADHD | Conditional in favor | Moderate |
| Quetiapine (Seroquel) for conduct problems in children and adolescents with conduct disorder, with or without ADHD | Conditional against | Very low |
| Haloperidol for aggression in children and adolescents with conduct disorder | Strong against | Very low |
| Valproate (Depacon) for aggression in children and adolescents with ODD or conduct disorder, with or without ADHD | Conditional in favor | Low |
| Lithium for aggression in children and adolescents with conduct disorder | Conditional against | Low |
| Carbamazepine (Tegretol) for aggression in children and adolescents with conduct disorder | Strong against | Very low |
Note: A “strong” recommendation means that most patients would want the recommended intervention and most health care professionals would think that most patients should receive it; a “conditional” recommendation means that most patients would want the recommended intervention but a substantial portion would not, and that health care professionals would recognize that different choices would be appropriate for different patients.
ADHD = attention-deficit/hyperactivity disorder; ODD = oppositional defiant disorder.
Adapted with permission from Gorman DA, Gardner DM, Murphy AL, et al. Canadian guidelines on pharmacotherapy for disruptive and aggressive behaviour in children and adolescents with attention-deficit hyperactivity disorder, oppositional defiant disorder, or conduct disorder. Can J Psychiatry. 2015;60(2):67.
Risperidone carries a conditional recommendation to treat disruptive and aggressive behavior in patients with an average IQ and ODD or conduct disorder, with or without concomitant ADHD. Risperidone also carries a conditional recommendation to treat patients with a below average IQ.
In eight randomized controlled trials (RCTs) of risperidone for the treatment of conduct disorder, aggression, or disruptive behavior disorders,26–33 the mean dosages ranged from less than 1 mg to up to 2.9 mg per day. This coincides with the range of general target dosages used to treat children and adolescents who have schizophrenia, bipolar mania, or irritability associated with autistic disorder, which are the FDA-approved indications for risperidone in youth. In these studies, improvements were seen in areas such as aggressive/destructive behavior, irritability, lethargy, and hyperactivity. Risperidone has an adverse effect profile that includes weight gain, dyslipidemia, hyperglycemia, diabetes mellitus, extrapyramidal symptoms, tardive dyskinesia, hyperprolactinemia, and increased risk of suicidal ideation. The physician prescribing risperidone should track parameters such as weight, blood pressure, blood glucose, lipid profile, and A1C, and the risk and benefit ratio must be discussed.
The only other medication that carries a conditional favorable recommendation is valproate.23 In the two randomized, placebo-controlled trials of divalproex (Depakote), the sodium analogue of valproate, for the treatment of conduct disorder, ODD, or ADHD and aggression, the mean blood levels were 82 mcg per mL and 68 mcg per mL,34,35 which are consistent with acceptable levels when divalproex or valproate is used to treat bipolar disorder. Patients showed improvement in impulse control, depression, and aggressive behavior. Valproate can produce adverse effects such as hepatotoxicity, pancreatitis, thrombocytopenia, increased risk of suicidal ideation, and fetal risks, including neural tube defects and a lower IQ. Blood levels of the medication should be monitored, and liver function tests, blood counts, and coagulation tests should be performed.
Resolution of Cases
CASE 1
This patient displays symptoms of ADHD. The family physician should obtain rating scales such as the Vanderbilt to assess for ADHD and should treat the patient with a stimulant. There could be coordination with the patient's school about whether they use an evidence-based psychosocial approach for aggression. The mother is getting help from relatives and they could work collectively with health care professionals to establish and enforce limits at home.
CASE 2
The mother in this case has symptoms of depression and should be encouraged to seek treatment. The patient could be educated about substance use and engaged around why she might want to stop. Perhaps her legal charges could be expunged if she were to complete a treatment program. The mother and daughter should be referred for a family therapy intervention that focuses on parenting skills and communication. If the patient can swim (which is assumed because she goes to a lake), she might also be encouraged to join a community activity such as a swim team.
This article updates a previous article on this topic by Searight, et al.7
Data Sources: A PubMed search was completed using the key terms conduct disorder and conduct disorder clinical trial. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. Also searched were the Agency for Healthcare Research and Quality Evidence Reports, the Cochrane Database of Systematic Reviews, Clinical Evidence, evidence-based guidelines from the National Guideline Clearinghouse, Institute for Clinical Systems Improvement, and U.S. Preventive Services Task Force. Search dates: December 2017, January 2018, and August 2018.
The author thanks Anne Walling, MD, for her assistance with the manuscript.

