
Am Fam Physician. 2018;98(11):643-644
Author disclosure: No relevant financial affiliations.
Clinical Question
Can improved diet, increased physical activity, or both prevent or delay the development of type 2 diabetes mellitus in high-risk patients?
Evidence-Based Answer
There is moderate-quality evidence that in patients with impaired glucose tolerance (IGT) defined by an abnormal 75-g two-hour glucose tolerance test, implementing changes in diet and adding physical activity together can prevent or delay the development of type 2 diabetes (absolute risk reduction [ARR] = 11%; 95% confidence interval [CI], 9.3% to 12.8%; number needed to treat = 9; 95% CI, 8 to 11). This review found no evidence that either diet or physical activity alone affects the incidence of type 2 diabetes in high-risk patients. Most of the included studies used IGT to define persons at high risk of diabetes; evidence is lacking about the effectiveness of diet and exercise in patients with prediabetes defined by other criteria, including elevated fasting blood glucose or elevated A1C levels.1 (Strength of Recommendation: B, based on inconsistent or limited-quality patient-oriented evidence.)
Practice Pointers
Prediabetes is commonly used to describe persons with intermediate hyperglycemia defined by impaired fasting glucose (IFG), IGT, or elevated A1C values lower than those that are diagnostic for diabetes. Persons with prediabetes have a higher risk of developing diabetes than those with normal blood glucose levels. The annual incidence of new diabetes in this population depends on the test used. In a given year, 4% to 6% of those with IGT will develop diabetes. Similarly, 6% to 9% of those with IFG, and 15% to 19% of those with both IGT and IFG will progress to diabetes.2 There is a continuous association between an increasing A1C level and diabetes incidence; the five-year risk for patients with an A1C level between 5.5% and 6.0% is 9% to 25%, whereas the five-year risk for those with an A1C level greater than 6.0% to 6.5% is 25% to 50%.3 Persons who have prediabetes are encouraged to modify their diet and increase physical activity to prevent progression to type 2 diabetes.4 However, it is unclear if those interventions are effective.
This Cochrane review included 12 randomized controlled trials comprising 5,238 individuals with prediabetes. The trials compared diet, physical activity, or both with standard treatment or no treatment.1 Standard treatment included recommendations, advice, or education about how to increase physical activity and reduce calories. The interventions were varied and included structured classes or individual instruction and support to increase activity and decrease calories for modest weight loss. The included trials followed patients for two to six years (mean duration = 3.6 years). Eleven studies used diet plus exercise vs. standard treatment or no treatment, one study compared a diet-only intervention with a physical-activity–only intervention or to standard treatment, and two compared physical activity only to standard treatment. Nine of the trials used IGT to define prediabetes, and three used IFG instead of or in addition to IGT to define the population. None of the studies used A1C levels.
Participants included men and women 45 to 63 years of age from Asia, Scandinavia, the United Kingdom, and the United States. Studies were excluded if they compared diet or physical activity interventions with a pharmacologic intervention, or if the diet component consisted of a single food or supplement change.
In addition to the incidence of type 2 diabetes, the primary outcomes studied were all-cause mortality and serious adverse events. Studies that reported all-cause or cardiovascular mortality found no clinical or statistical differences, albeit with very-low-quality evidence. No serious adverse events were noted in the standard treatment or intervention groups, and patient-oriented outcomes such as blindness, renal failure, and quality of life were not reported.
This review lacks specific data about what constituted the changes in diet and physical activity. The National Institute of Diabetes and Digestive and Kidney Diseases recommends 5% to 10% weight loss through portion control and the “plate method,” and 150 combined minutes of moderate aerobic exercise and two sessions of resistance training per week.5
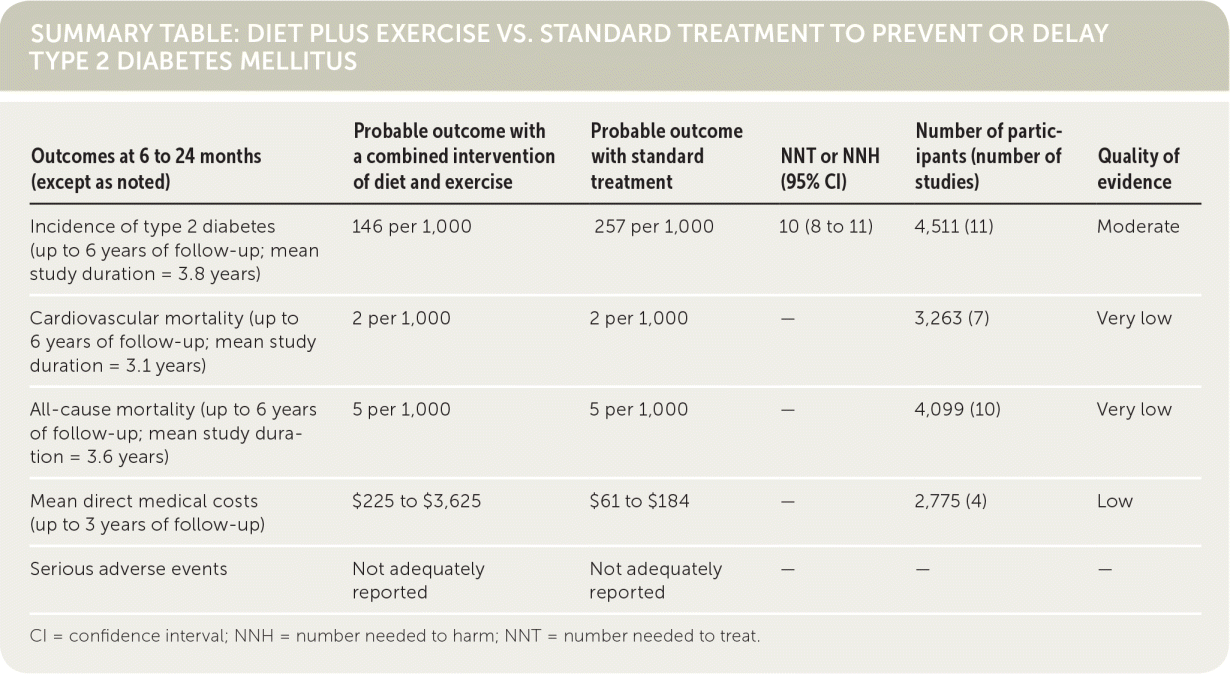
| Outcomes at 6 to 24 months (except as noted) | Probable outcome with a combined intervention of diet and exercise | Probable outcome with standard treatment | NNT or NNH (95% CI) | Number of participants (number of studies) | Quality of evidence |
|---|---|---|---|---|---|
| Incidence of type 2 diabetes (up to 6 years of follow-up; mean study duration = 3.8 years) | 146 per 1,000 | 257 per 1,000 | 10 (8 to 11) | 4,511 (11) | Moderate |
| Cardiovascular mortality (up to 6 years of follow-up; mean study duration = 3.1 years) | 2 per 1,000 | 2 per 1,000 | — | 3,263 (7) | Very low |
| All-cause mortality (up to 6 years of follow-up; mean study duration = 3.6 years) | 5 per 1,000 | 5 per 1,000 | — | 4,099 (10) | Very low |
| Mean direct medical costs (up to 3 years of follow-up) | $225 to $3,625 | $61 to $184 | — | 2,775 (4) Low | |
| Serious adverse events | Not adequately reported | Not adequately reported | — | — | — |
Editor's Note: The numbers needed to treat reported in this Cochrane for Clinicians were calculated by the author based on raw data provided in the original Cochrane review.
The practice recommendations in this activity are available at http://www.cochrane.org/CD003054.
