
Am Fam Physician. 2018;98(11):660G-660H
AFP uses the Strength-of-Recommendation Taxonomy (SORT),1 to label key recommendations in clinical review articles. In general, only key recommendations are given a Strength-of-Recommendation grade. Grades are assigned on the basis of the quality and consistency of available evidence. Table 1 shows the three grades recognized.
An alternative way to understand the significance of a strength-of-recommendation grade is through the algorithm generally followed by authors and editors in assigning grades based on a body of evidence (Figure 1). While this algorithm provides a general guideline, authors and editors may adjust the strength of recommendation based on the benefits, harms, and costs of the intervention being recommended.

| Strength of recommendation | Basis for recommendation |
|---|---|
| A | Consistent, good-quality patient-oriented evidence* |
| B | Inconsistent or limited-quality patient-oriented evidence* |
| C | Consensus, disease-oriented evidence,** usual practice, expert opinion, or case series for studies of diagnosis, treatment, prevention, or screening |
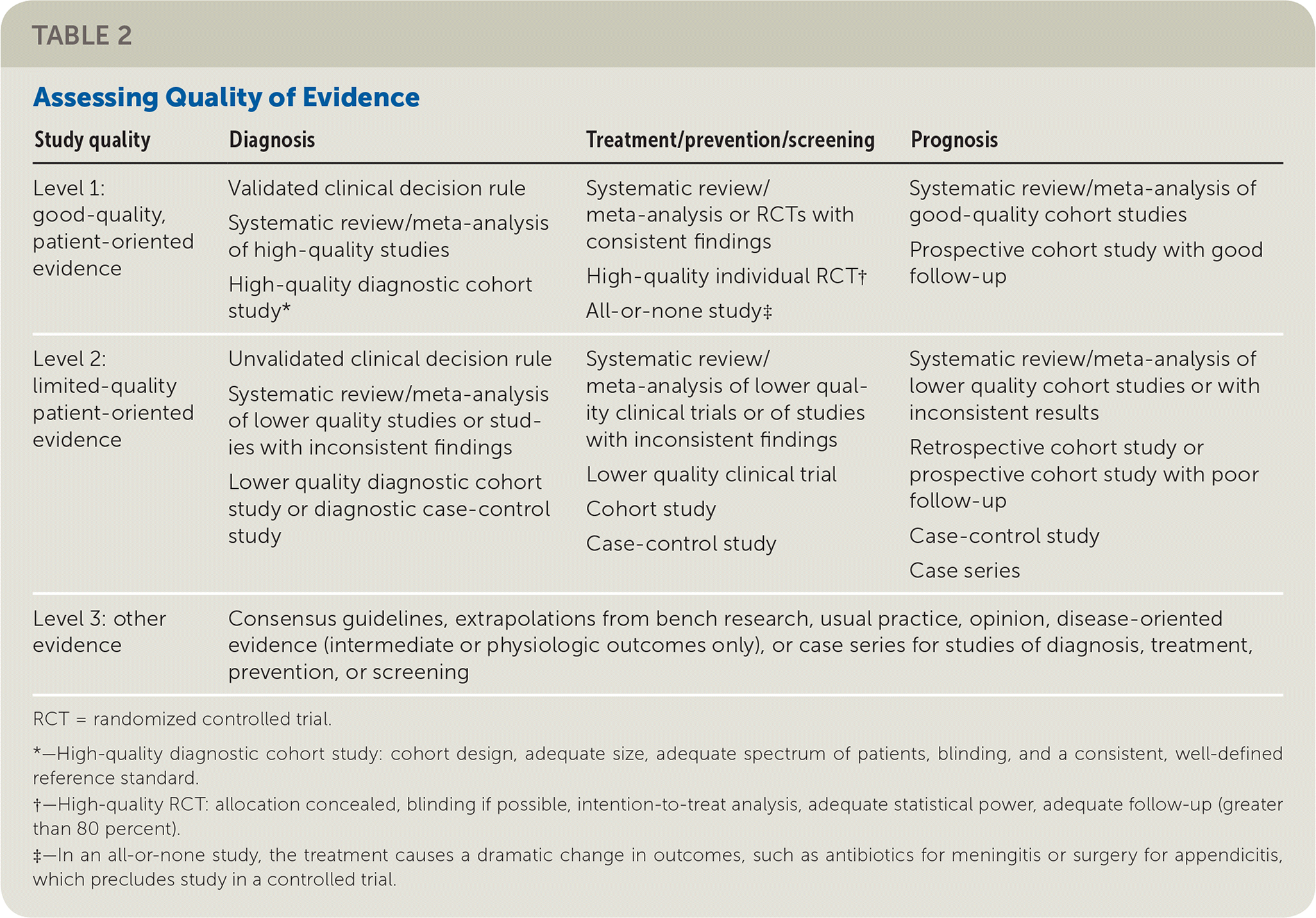
| Study quality | Diagnosis | Treatment/prevention/screening | Prognosis |
|---|---|---|---|
| Level 1: good-quality, patient-oriented evidence | Validated clinical decision rule Systematic review/meta-analysis of high-quality studies High-quality diagnostic cohort study* | Systematic review/meta-analysis or RCTs with consistent findings High-quality individual RCT† All-or-none study‡ | Systematic review/meta-analysis of good-quality cohort studies Prospective cohort study with good follow-up |
| Level 2: limited-quality patient-oriented evidence | Unvalidated clinical decision rule Systematic review/meta-analysis of lower quality studies or studies with inconsistent findings Lower quality diagnostic cohort study or diagnostic case-control study | Systematic review/meta-analysis of lower quality clinical trials or of studies with inconsistent findings Lower quality clinical trial Cohort study Case-control study | Systematic review/meta-analysis of lower quality cohort studies or with inconsistent results Retrospective cohort study or prospective cohort study with poor follow-up Case-control study Case series |
| Level 3: other evidence | Consensus guidelines, extrapolations from bench research, usual practice, opinion, disease-oriented evidence (intermediate or physiologic outcomes only), or case series for studies of diagnosis, treatment, prevention, or screening | ||

| Consistent | Most studies found similar or at least coherent conclusions (coherence means that differences are explainable). or If high-quality and up-to-date systematic reviews or meta-analyses exist, they support the recommendation. |
| Inconsistent | Considerable variation among study findings and lack of coherence or If high-quality and up-to-date systematic reviews or meta-analyses exist, they do not find consistent evidence in favor of the recommendation. |
