Family physicians spend substantial time counseling patients with psychiatric conditions, unhealthy behaviors, and medical adherence issues. Maintaining efficiency while providing counseling is a major challenge. There are several effective, structured counseling strategies developed for use in primary care settings. The transtheoretical (stages of change) model assesses patients’ motivation for change so that the physician can select the optimal counseling approach. Structured sequential strategies such as the five A’s (ask, advise, assess, assist, arrange) and FRAMES (feedback, responsibility of patient, advice to change, menu of options, empathy, self-efficacy enhancement) are effective for patients who are responsive to education about health risk behavior. For patients ambivalent about change, motivational interviewing is more likely to be successful. Capitalizing on a teachable moment may enhance the effectiveness of health behavior change counseling. The BATHE (background, affect, troubles, handling, and empathy) strategy is useful for patients with psychiatric conditions and psychosocial issues. Patients should be referred for subspecialty mental health or substance abuse treatment if they do not respond to these brief interventions.
Counseling patients on lifestyle modification and psychosocial problems is a fundamental competency for family physicians.1–4 Approximately 40% of primary care office visits are for chronic illness5 in which psychosocial factors play a major role in etiology and disease progression.6 Counseling patients about health risk behaviors and health education is a core component of 18% of all primary care office visits.5 Although counseling regarding weight management, diet, smoking, and alcohol use is an important part of clinical practice, a survey found that only between 31% and 56% of primary care physicians rated themselves as having significant expertise in counseling about these issues.4
WHAT IS NEW ON THIS TOPIC
Research based on the transtheoretical (stages of change) model suggests that it is possible to change multiple health risk behaviors concurrently.
Application of the FRAMES counseling protocol to French primary care patients found reductions in cannabis use among patients up to 18 years of age at the six-month follow-up, whereas use increased among adolescents receiving routine care.
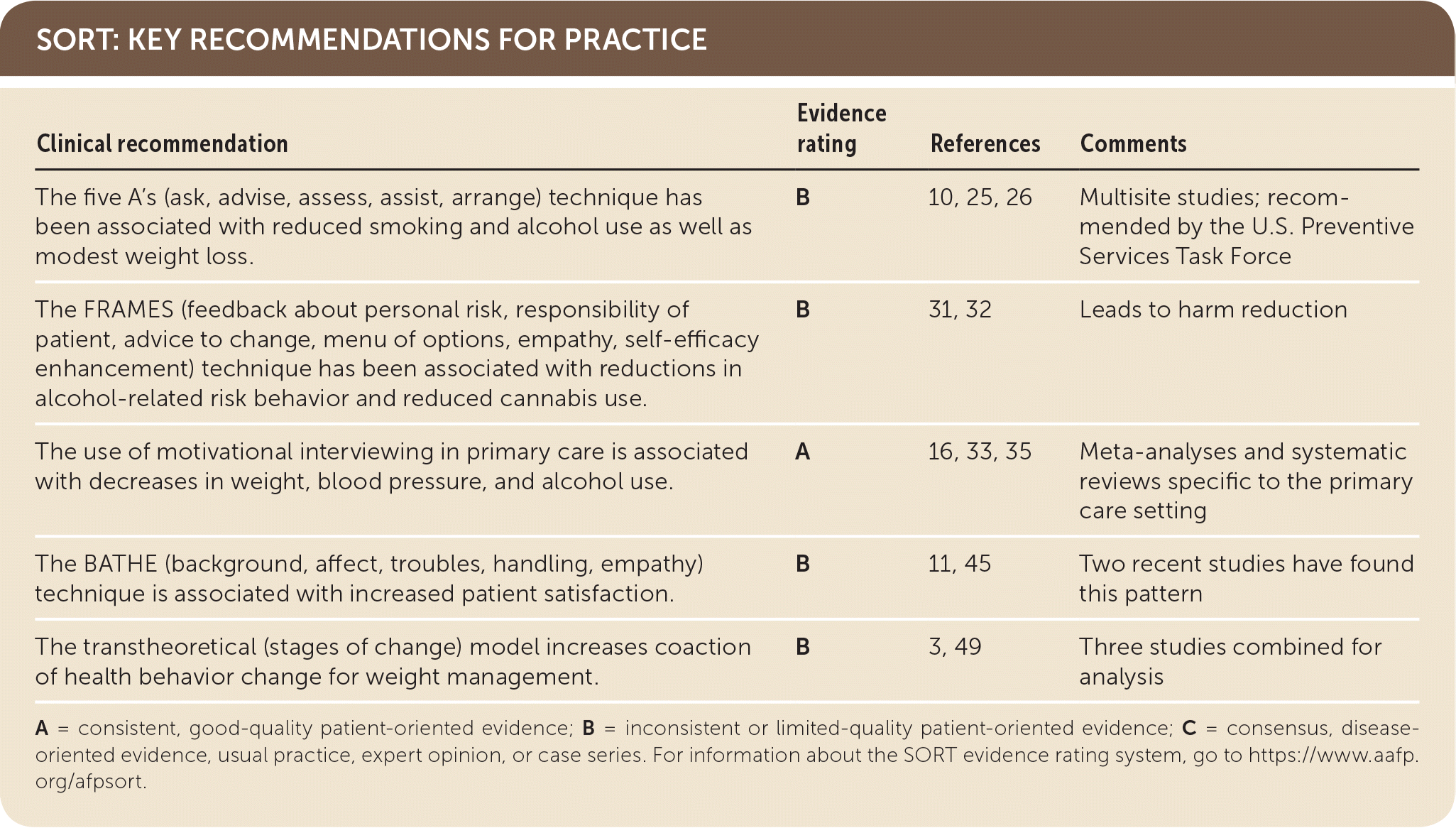
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References | Comments |
|---|---|---|---|
| The five A’s (ask, advise, assess, assist, arrange) technique has been associated with reduced smoking and alcohol use as well as modest weight loss. | B | 10, 25, 26 | Multisite studies; recommended by the U.S. Preventive Services Task Force |
| The FRAMES (feedback about personal risk, responsibility of patient, advice to change, menu of options, empathy, self-efficacy enhancement) technique has been associated with reductions in alcohol-related risk behavior and reduced cannabis use. | B | 31, 32 | Leads to harm reduction |
| The use of motivational interviewing in primary care is associated with decreases in weight, blood pressure, and alcohol use. | A | 16, 33, 35 | Meta-analyses and systematic reviews specific to the primary care setting |
| The BATHE (background, affect, troubles, handling, empathy) technique is associated with increased patient satisfaction. | B | 11, 45 | Two recent studies have found this pattern |
| The transtheoretical (stages of change) model increases coaction of health behavior change for weight management. | B | 3, 49 | Three studies combined for analysis |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
In the past decade, primary care counseling strategies have been refined,7–10 and some have been empirically evaluated.10–12 This article describes practical counseling strategies typically requiring no more than five to 10 minutes that can be integrated into a typical office visit1,3,9,13,14 (Table 13,15 ). Research and clinical guidelines suggest that smoking cessation can be effectively addressed in three minutes, problem alcohol use in five minutes, and dietary fat consumption and lipid levels in eight minutes.13 These strategies may also be adapted to multiple patient contacts. For example, the U.S. Preventive Services Task Force guidelines16 and a recent Cochrane review 17 for addressing alcohol misuse suggest that several 10- to 15-minute counseling appointments are most effective for reducing alcohol consumption.
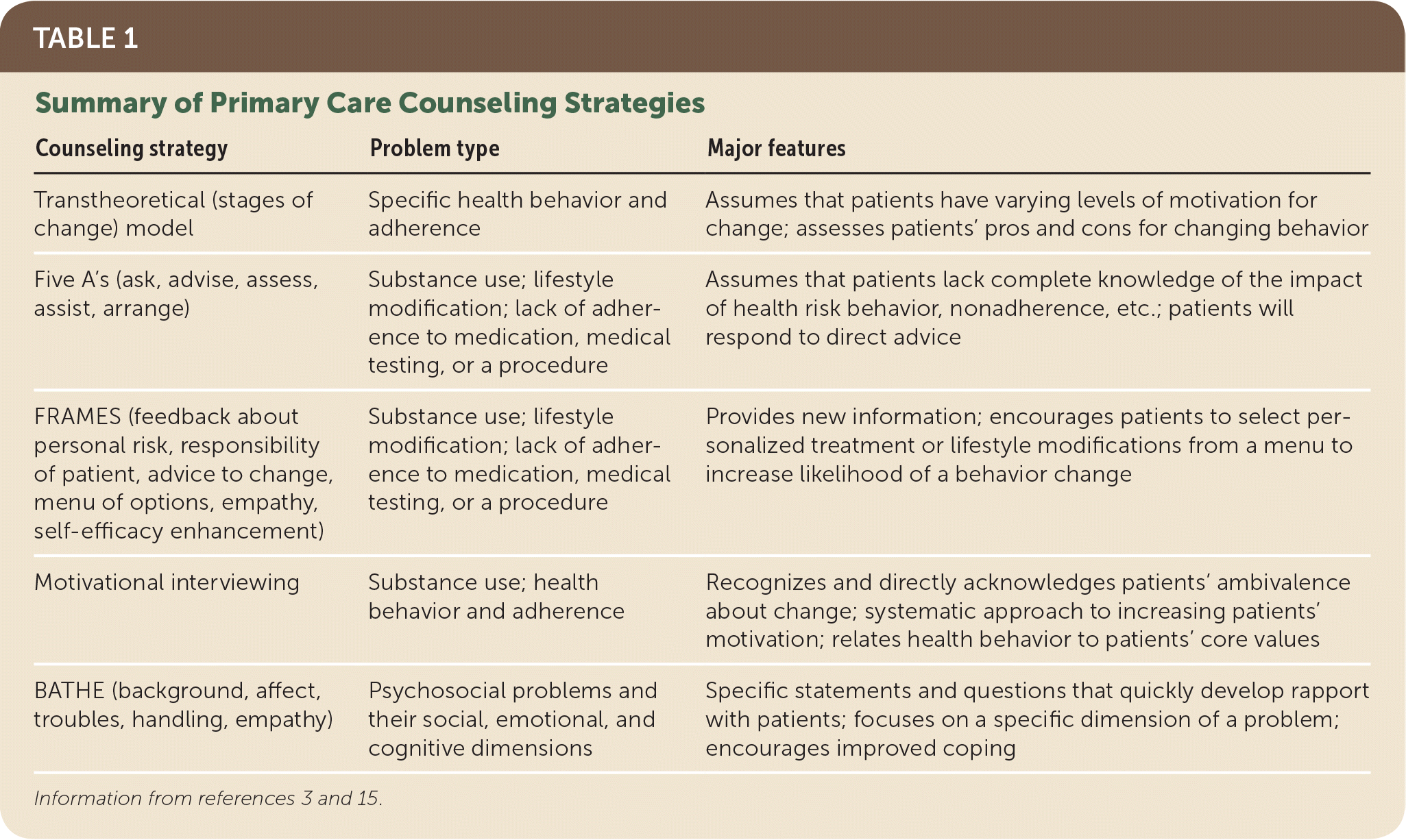
TABLE 1. Summary of Primary Care Counseling Strategies
| Counseling strategy | Problem type | Major features |
|---|---|---|
| Transtheoretical (stages of change) model | Specific health behavior and adherence | Assumes that patients have varying levels of motivation for change; assesses patients’ pros and cons for changing behavior |
| Five A’s (ask, advise, assess, assist, arrange) | Substance use; lifestyle modification; lack of adherence to medication, medical testing, or a procedure | Assumes that patients lack complete knowledge of the impact of health risk behavior, nonadherence, etc.; patients will respond to direct advice |
| FRAMES (feedback about personal risk, responsibility of patient, advice to change, menu of options, empathy, self-efficacy enhancement) | Substance use; lifestyle modification; lack of adherence to medication, medical testing, or a procedure | Provides new information; encourages patients to select personalized treatment or lifestyle modifications from a menu to increase likelihood of a behavior change |
| Motivational interviewing | Substance use; health behavior and adherence | Recognizes and directly acknowledges patients’ ambivalence about change; systematic approach to increasing patients’ motivation; relates health behavior to patients’ core values |
| BATHE (background, affect, troubles, handling, empathy) | Psychosocial problems and their social, emotional, and cognitive dimensions | Specific statements and questions that quickly develop rapport with patients; focuses on a specific dimension of a problem; encourages improved coping |
Transtheoretical (Stages of Change) Model
The stages of change model (Table 23,15,18–20 ), originally developed from studying successful smoking cessation techniques,18,19 recognizes that many patients are currently unmotivated or ambivalent about habit change. The stages of change model provides a framework for assessing the patient’s degree of commitment to change, and can guide physicians in choosing from counseling strategies such as the five A’s, FRAMES, or motivational interviewing. By asking questions assessing the patient’s motivation, and determining his or her specific stage in the change process (i.e., precontemplation, contemplation, preparation, action, maintenance), physicians can move the patient toward initiating action or support ongoing health behavior change.15,18,19
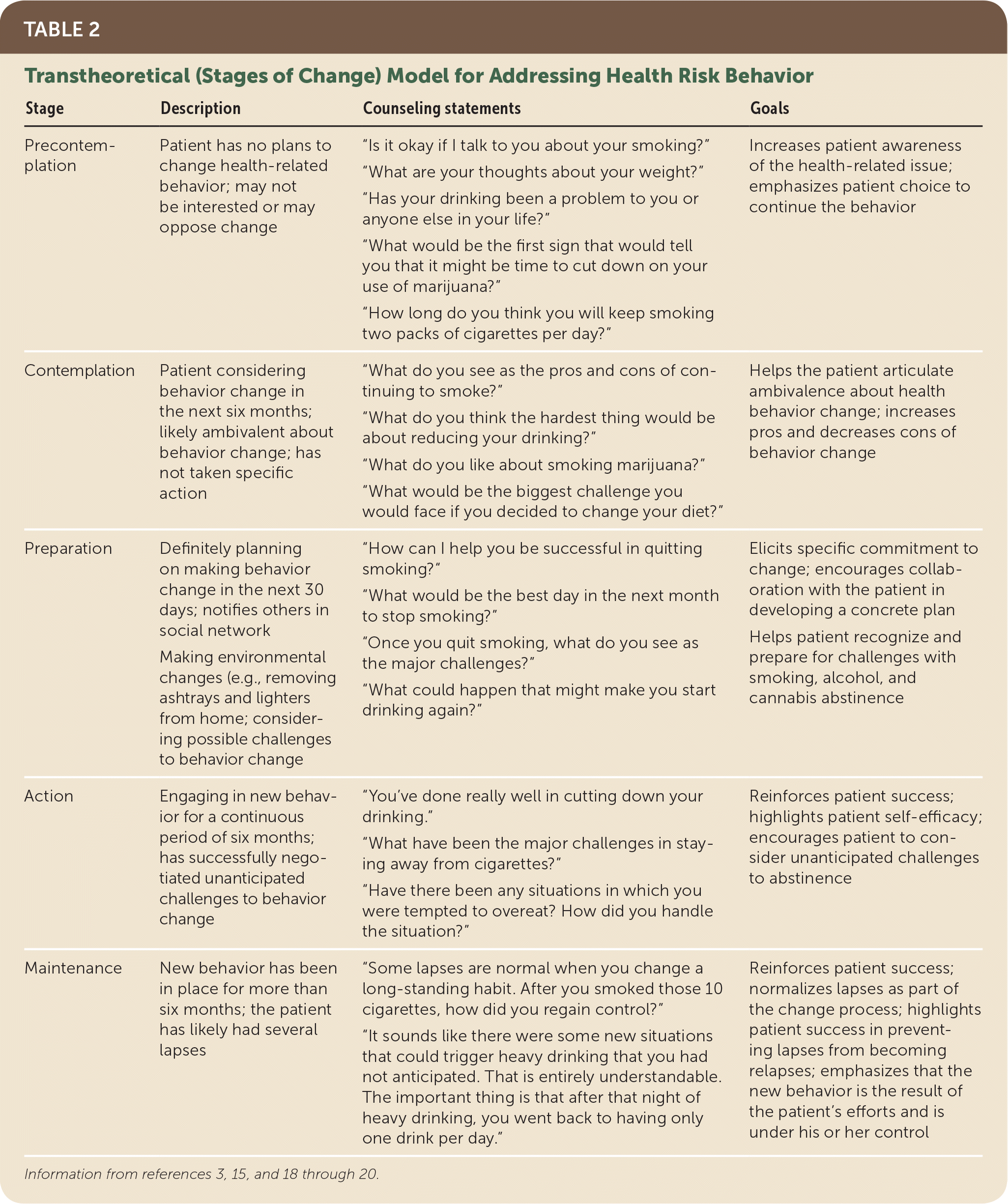
TABLE 2. Transtheoretical (Stages of Change) Model for Addressing Health Risk Behavior
| Stage | Description | Counseling statements | Goals |
|---|---|---|---|
| Precontemplation | Patient has no plans to change health-related behavior; may not be interested or may oppose change | “Is it okay if I talk to you about your smoking?” | Increases patient awareness of the health-related issue; emphasizes patient choice to continue the behavior |
| “What are your thoughts about your weight?” | |||
| “Has your drinking been a problem to you or anyone else in your life?” | |||
| “What would be the first sign that would tell you that it might be time to cut down on your use of marijuana?” | |||
| “How long do you think you will keep smoking two packs of cigarettes per day?” | |||
| Contemplation | Patient considering behavior change in the next six months; likely ambivalent about behavior change; has not taken specific action | “What do you see as the pros and cons of continuing to smoke?” | Helps the patient articulate ambivalence about health behavior change; increases pros and decreases cons of behavior change |
| “What do you think the hardest thing would be about reducing your drinking?” | |||
| “What do you like about smoking marijuana?” | |||
| “What would be the biggest challenge you would face if you decided to change your diet?” | |||
| Preparation | Definitely planning on making behavior change in the next 30 days; notifies others in social network | “What would be the best day in the next month to stop smoking?” | Elicits specific commitment to change; encourages collaboration with the patient in developing a concrete plan Helps patient recognize and prepare for challenges with smoking, alcohol, and cannabis abstinence |
| “How can I help you be successful in quitting smoking?“ | |||
| “Once you quit smoking, what do you see as the major challenges?” | |||
| Making environmental changes (e.g., removing ashtrays and lighters from home; considering possible challenges to behavior change) | |||
| “What could happen that might make you start drinking again?” | |||
| Action | Engaging in new behavior for a continuous period of six months; has successfully negotiated unanticipated challenges to behavior change | “You’ve done really well in cutting down your drinking.” | Reinforces patient success; highlights patient self-efficacy; encourages patient to consider unanticipated challenges to abstinence |
| “What have been the major challenges in staying away from cigarettes?” | |||
| “Have there been any situations in which you were tempted to overeat? How did you handle the situation?” | |||
| Maintenance | New behavior has been in place for more than six months; the patient has likely had several lapses | “Some lapses are normal when you change a long-standing habit. After you smoked those 10 cigarettes, how did you regain control?” | Reinforces patient success; normalizes lapses as part of the change process; highlights patient success in preventing lapses from becoming relapses; emphasizes that the new behavior is the result of the patient’s efforts and is under his or her control |
| “It sounds like there were some new situations that could trigger heavy drinking that you had not anticipated. That is entirely understandable. The important thing is that after that night of heavy drinking, you went back to having only one drink per day.” |
Patients in the precontemplative stage pose a particular challenge. If a patient appears unconcerned about health risks, the physician may be tempted to emphasize the consequences of a behavior such as continued smoking or excess alcohol use. However, aggressive education may increase resistance and has the unintended effect of reducing patient openness to physician input.3,15,16,18,19,21
In precontemplation, the cons of changing outweigh any perceived benefits.18 Therefore, counseling at this stage should emphasize the benefits of change. Achieving “decisional balance” involves eliciting the patient’s stated pros and cons for changing his or her behaviors. To move the patient from contemplation to action, the physician should address obstacles to change. Studies of multiple health behaviors conclude that moving through these stages involves a cross-over, with an increase in the pros and a decrease in the cons of changing behaviors.18
In the action and maintenance stages, patients contend with possible lapse and relapse. When a lapse occurs, patients are more likely to relapse to their former habit when they attribute the lapse to internal causes such as personality, genetics, or lack of willpower. Patients attributing their lapse to external factors such as peer pressure or work-related stress are less likely to relapse.20 Physicians should frame lapses and relapses as learning experiences and help patients recognize formerly unanticipated challenges as well as develop a plan for preventing future episodes.
Although the stages accurately predict health-related behaviors, the effects of specific stage-matched interventions are unclear.22,23 For example, the stages of change are useful in approaching smoking cessation counseling, with precontemplative patients responding best to a brief motivational intervention accompanied by written information.23 Patients in the preparation or action stage benefit most from a combination of focused advice, written guidance, and prescription medication when indicated.23
The Five A’s
The five A’s (ask, advise, assess, assist, arrange; Table 33,10,15,24,25 ), is a stepwise protocol for primary care physicians to efficiently assess and counsel patients about smoking cessation,3,10,15,26 alcohol intake,3,19 and weight loss.24,25 Whenever possible, advising and assessing should link the patient’s presenting problem (e.g., gastrointestinal distress, knee pain with a body mass index above 30 kg per m2) to objective, factual standards (e.g., safe vs. unsafe levels of alcohol use, recommended daily caloric intake). Patients are likely to respond more favorably to “I” statements (“I recommend…”) rather than “You” statements (“You should…”).3
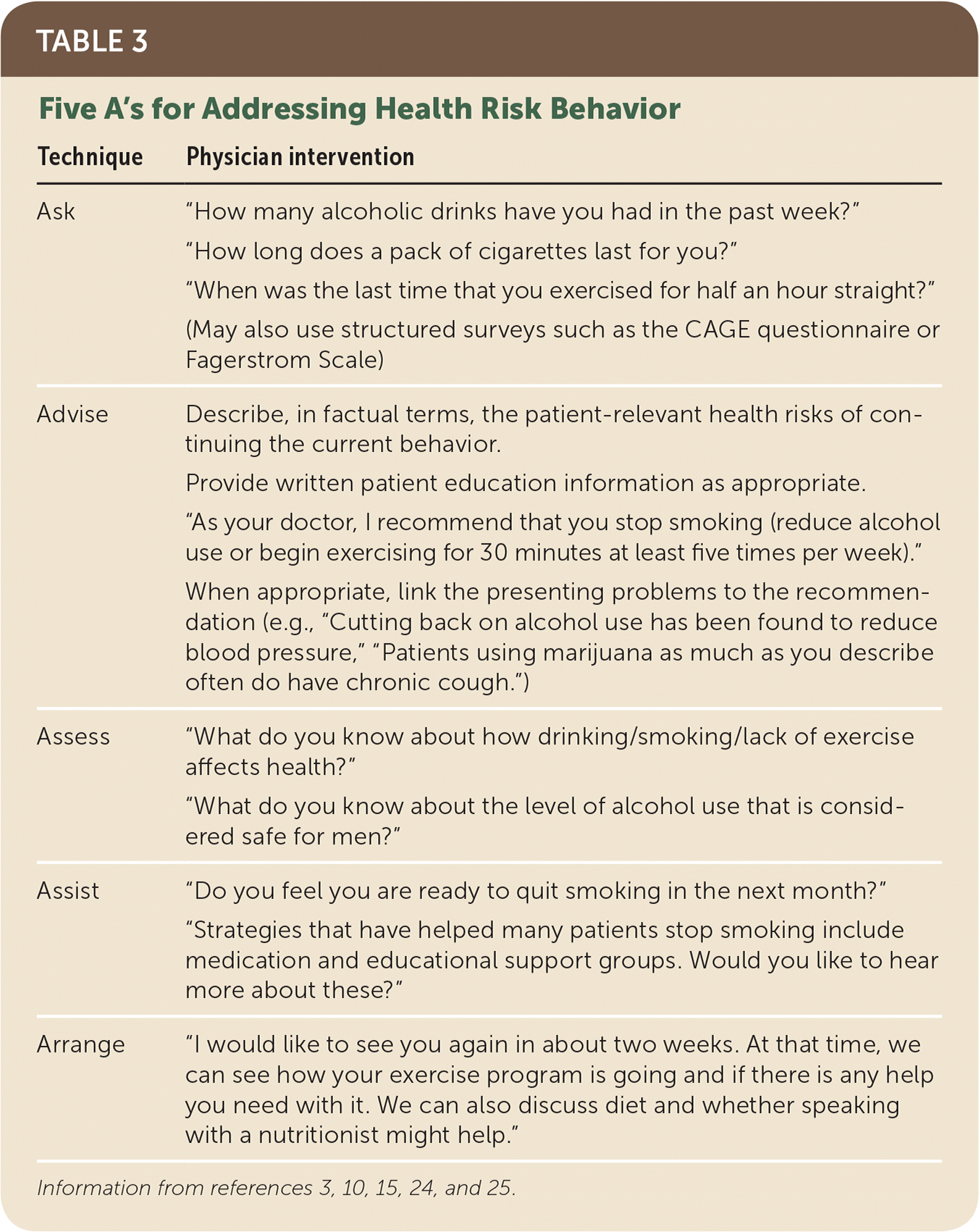
TABLE 3. Five A’s for Addressing Health Risk Behavior
| Technique | Physician intervention |
|---|---|
| Ask | “How many alcoholic drinks have you had in the past week?” |
| “How long does a pack of cigarettes last for you?” | |
| “When was the last time that you exercised for half an hour straight?” | |
| (May also use structured surveys such as the CAGE questionnaire or Fagerstrom Scale) | |
| Advise | Describe, in factual terms, the patient-relevant health risks of continuing the current behavior. |
| Provide written patient education information as appropriate. | |
| “As your doctor, I recommend that you stop smoking (reduce alcohol use or begin exercising for 30 minutes at least five times per week).” | |
| When appropriate, link the presenting problems to the recommendation (e.g., “Cutting back on alcohol use has been found to reduce blood pressure,” “Patients using marijuana as much as you describe often do have chronic cough.”) | |
| Assess | “What do you know about how drinking/smoking/lack of exercise affects health?” |
| “What do you know about the level of alcohol use that is considered safe for men?” | |
| Assist | “Do you feel you are ready to quit smoking in the next month?” |
| “Strategies that have helped many patients stop smoking include medication and educational support groups. Would you like to hear more about these?” | |
| Arrange | “I would like to see you again in about two weeks. At that time, we can see how your exercise program is going and if there is any help you need with it. We can also discuss diet and whether speaking with a nutritionist might help.” |
In one study, using some of the five A’s in a brief emergency department intervention required a median of seven minutes that included screening, describing the relationship between alcohol and the patient’s presenting problem, enhancing patient motivation, and goal setting. This physician-delivered intervention, when assessed during a six-month follow-up visit, was associated with an average of 3.3 fewer binge episodes in the previous 28 days compared with 1.5 fewer episodes for patients receiving standard care.27
Some evidence suggests that depending on the clinical context and problem, the impact of the specific A’s may vary.24,25 For example, when the five A’s impact on dietary change was assessed at the three-month follow-up, weight loss of 3.3 lb (1.5 kg) occurred only when the intervention included the “arrange” step, whereas small, statistically significant self-reported changes in fat and fiber intake occurred with the first four A’s alone.25
FRAMES
FRAMES (feedback about personal risk, responsibility of patient, advice to change, menu of options, empathy, self-efficacy enhancement) is a precursor to motivational interviewing, and was originally developed to address alcohol misuse. However, it has been applied to other health issues such as reducing stroke risk28 (Table 43,15,27,28 ). To facilitate collaboration, the physician obtains the patient’s permission before providing information. By granting permission, patients maintain control, implicitly demonstrate interest, and are less likely to experience a threat to their independence.3,15,21,29,30 How open the patient is to change will usually be evident by his or her answer to the responsibility statement that emphasizes the patient’s autonomous choice to address health risk behavior. Specific, individualized feedback is presented in a factual, nonjudgmental manner. For some patients, seeing numerical data, such as blood pressure readings or body weight, in the context of normal values, may be adequate for eliciting motivation to change.3,15,27
TABLE 4. FRAMES for Addressing Health Risk Behavior

| Technique | Physician intervention |
|---|---|
| Feedback about personal risk | Provide information in a factual manner; for example, use a CAGE questionnaire or laboratory test results to explain alcohol use. |
| Make the connection, “Do you see any connection between drinking and your blood pressure, your history of falling and breaking bones, your stomach pain and indigestion?” | |
| If yes, briefly elaborate again using facts. “There is a pretty clear association between unintentional injuries and the amount of alcohol people drink.” | |
| If no, provide information and then ask, “What do you think of that?” | |
| Responsibility of patient | “Making a change in your alcohol use is a choice that only you can make.” |
| Advice to change | Advice should be conveyed neutrally, but based on objective indicators such as the National Institute on Alcohol Abuse and Alcoholism standards for moderate drinking (one drink per day for women and two for men27). |
| “Although stopping marijuana altogether would probably be the best thing that you can do, cutting down would benefit you.” | |
| Menu of options | “Different strategies work better for different patients based on their lifestyle. Here are some strategies that have been successful for stopping smoking.” |
| Options may include medication and/or educational groups for smoking cessation or following written guidelines or attending self-help groups for dietary changes. | |
| Empathy | “You sound like you have a lot of stressors in your life. It is hard to make a major change when you’re feeling all these demands.” |
| “It sounds like you are at a point where you want to make a change and are really motivated to quit smoking and at the same time are a bit nervous about going through nicotine withdrawal.” | |
| Self-efficacy enhancement | “Two years ago, you were able to quit smoking for six months. You succeeded despite the worst part for many patients—nicotine withdrawal. That tells me that you have a lot of strength and follow-through. I genuinely believe you can be successful this time.” |
The FRAMES strategy incorporates elements of motivational interviewing21 and patient-centered care’s emphasis on understanding patients’ values and preferences.29,30 The menu of options step reflects the growing importance of shared decision making in clinical practice—particularly when there are several therapeutic options.3,15,30 Research has shown that providing choices increases patient adherence and satisfaction.29
Although abstinence remains the standard treatment for excessive alcohol use, reduced consumption has health benefits and diminishes risk of harm.31 In a randomized controlled trial, FRAMES was associated with 40% to 50% lower alcohol intake with a corresponding reduction in alcohol-related arrests and automobile crashes.31 A recent application of FRAMES to French primary care patients found reductions in cannabis use among patients up to 18 years of age at the six-month follow-up, whereas use increased among adolescents receiving routine care.32
Motivational Interviewing
Motivational interviewing has been successfully adapted to a range of behaviors including medication adherence, dietary change, and safe sex practices.33,34 Motivational interviewing was developed from the observation that substance abuse counselors who communicated empathy, understanding, and objective information were more successful in reducing patients’ substance use than those relying on confrontation.21 In the past decade, this strategy has developed further and its evidence base, particularly in primary care, has grown.33 A meta-analysis of outcomes across multiple medical conditions found that compared with usual care, motivational interviewing strategies resulted in an average of 10% to 15% added benefit in patient outcomes such as alcohol consumption, blood pressure readings, body weight, and human immunodeficiency virus viral load.33,35
Similar to the stages of change model, motivational interviewing assumes that patients are ambivalent about change21,34 and are more likely to change if they consider and explain their own reasons for new behavior.21 In the context of a supportive relationship, physicians ask Socratic-style questions that help patients articulate their own reasons and goals for addressing health risk behaviors21,34,36 (Table 53,15,21,30 ).
TABLE 5. General Motivational Interviewing Skills: Establishing Rapport and Eliciting Patient Values

| Technique | Examples of physician statements and questions | Goals |
|---|---|---|
| Open-ended question | “What brings you in today?” “How can I help you? “How do you view your drinking?” | Elicit patient’s agenda; determine key values |
| Affirmations | “You have been smoking since you were 15 years old; I applaud your determination to quit at this point in your life.” | Validate patient’s interest in changing; highlight strengths and past successes |
| Reflections | “You have become more uneasy about the amount you drink at night and don’t like the queasy feeling in the morning.” | Indicates to the patient that he or she is being heard; helpful in redirecting if the encounter goes off track |
| Summarization | “You have tried to make regular exercise a part of your life in the past, and the demands of work and family have often gotten in the way. Now, you are worried about your weight and blood pressure and are more determined to start and stick with a regular exercise routine.” | Ties together discussion and sets stage for the next step |
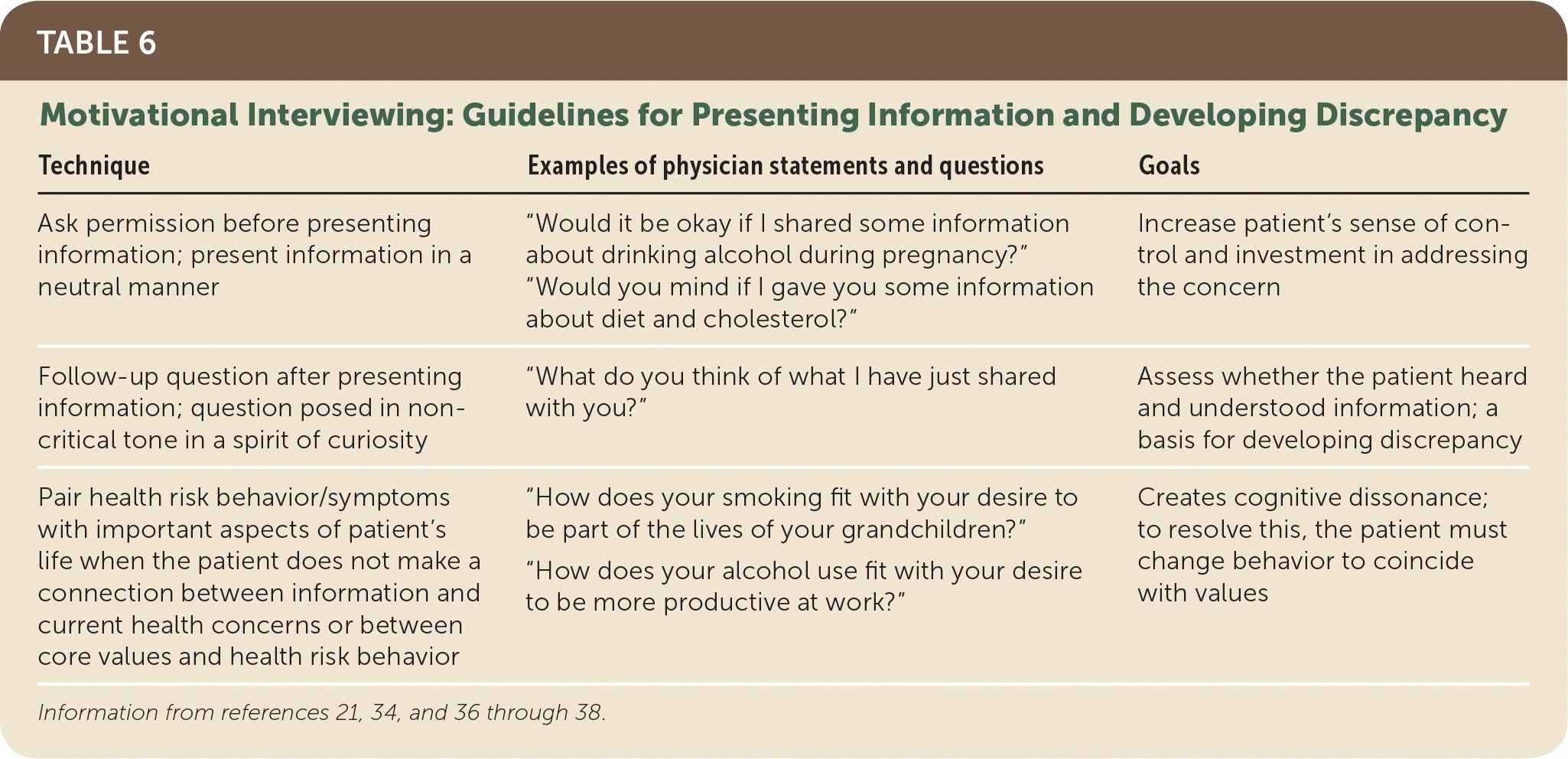
The initial stage of motivational interviewing focuses on understanding the patient’s concerns and developing rapport (Table 621,34,36–38 ). Effectiveness is optimized when physicians maintain a ratio of two reflective statements per question.38 When providing information, the physician should demonstrate a neutral, objective tone: “The amount that you reported drinking is at the 95th percentile for your age and sex, which means that you drink more than 95% of men your age in the United States.”39 In focusing the conversation, the physician emphasizes the patient’s own reasons for and against change: “After learning about your blood pressure, you are concerned about the overall effect that drinking is having on your health and that drinking beer is the way that you relax after work. Do I have that right?” The use of “and” rather than “but” is deliberate; “but” is likely to increase defensiveness.38,39
TABLE 6. Motivational Interviewing: Guidelines for Presenting Information and Developing Discrepancy
| Technique | Examples of physician statements and questions | Goals |
|---|---|---|
| Ask permission before presenting information; present information in a neutral manner | “Would it be okay if I shared some information about drinking alcohol during pregnancy?” | Increase patient’s sense of control and investment in addressing the concern |
| “Would you mind if I gave you some information about diet and cholesterol?” | ||
| Follow-up question after presenting information; question posed in noncritical tone in a spirit of curiosity | “What do you think of what I have just shared with you?” | Assess whether the patient heard and understood information; a basis for developing discrepancy |
| Pair health risk behavior/symptoms with important aspects of patient’s life when the patient does not make a connection between information and current health concerns or between core values and health risk behavior | “How does your smoking fit with your desire to be part of the lives of your grandchildren?” | Creates cognitive dissonance; to resolve this, the patient must change behavior to coincide with values |
| “How does your alcohol use fit with your desire to be more productive at work?” |
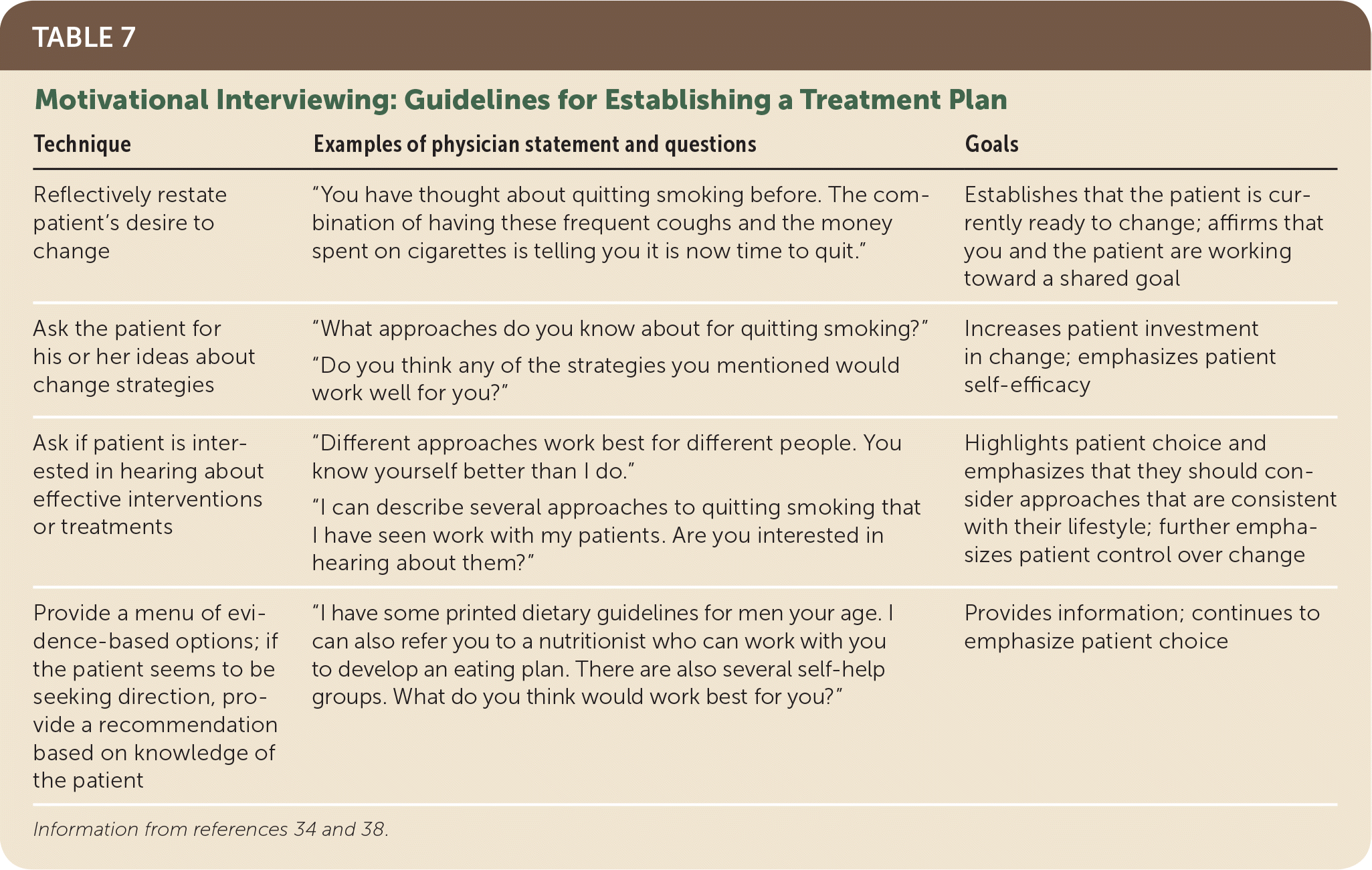
Patient values are a key component of developing an effective treatment plan (Table 734,38 ). Asking the patient about his or her ideas for habit change and continuing to ask permission before presenting options further the patient’s investment in change. This approach is also more likely to result in patient adherence. Although motivational interviewing techniques can be learned, maintaining the overall spirit of this strategy is more demanding.27 In primary care settings, benefits have been demonstrated with one to three 15- to 20-minute sessions.35 Descriptive reviews of motivational interviewing training for primary care physicians report a median of nine hours of training time40; however, basic skills have been acquired with two hours of training.41
TABLE 7. Motivational Interviewing: Guidelines for Establishing a Treatment Plan
| Technique | Examples of physician statement and questions | Goals |
|---|---|---|
| Reflectively restate patient’s desire to change | “You have thought about quitting smoking before. The combination of having these frequent coughs and the money spent on cigarettes is telling you it is now time to quit.” | Establishes that the patient is currently ready to change; affirms that you and the patient are working toward a shared goal |
| Ask the patient for his or her ideas about change strategies | “What approaches do you know about for quitting smoking?” | Increases patient investment in change; emphasizes patient self-efficacy |
| “Do you think any of the strategies you mentioned would work well for you?” | ||
| Ask if patient is interested in hearing about effective interventions or treatments | “Different approaches work best for different people. You know yourself better than I do.” | Highlights patient choice and emphasizes that they should consider approaches that are consistent with their lifestyle; further emphasizes patient control over change |
| “I can describe several approaches to quitting smoking that I have seen work with my patients. Are you interested in hearing about them?” | ||
| Provide a menu of evidence-based options; if the patient seems to be seeking direction, provide a recommendation based on knowledge of the patient | “I have some printed dietary guidelines for men your age. I can also refer you to a nutritionist who can work with you to develop an eating plan. There are also several self-help groups. What do you think would work best for you?” | Provides information; continues to emphasize patient choice |
BATHE
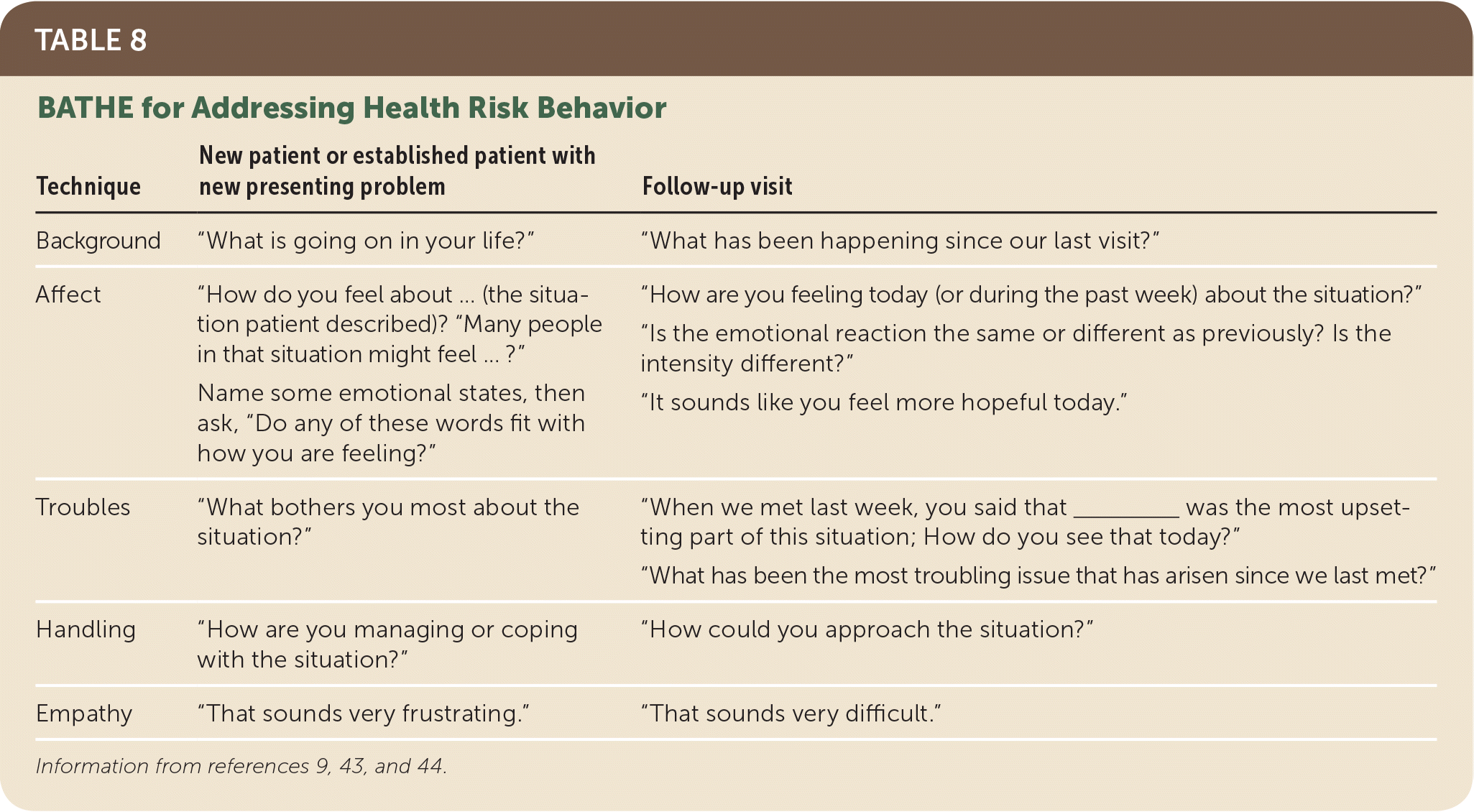
At least one-half of all mental health encounters occur in primary care,1,3,42 and patients with psychiatric conditions are twice as likely to be treated by primary care physicians than by mental health professionals.42 The BATHE (background, affect, troubles, handling, empathy) strategy is a structured set of questions and statements created specifically for the primary care setting and its inherent time constraints to address a range of psychosocial problems3,9,43 (Table 89,43,44 ). Compared with usual care, the BATHE technique has been associated with improved patient satisfaction in several medical settings.9,45
TABLE 8. BATHE for Addressing Health Risk Behavior
| Technique | New patient or established patient with new presenting problem | Follow-up visit |
|---|---|---|
| Background | “What is going on in your life?” | “What has been happening since our last visit?” |
| Affect | “How do you feel about … (the situation patient described)? “Many people in that situation might feel … ?” Name some emotional states, then ask, “Do any of these words fit with how you are feeling?” | “How are you feeling today (or during the past week) about the situation?” “Is the emotional reaction the same or different as previously? Is the intensity different?” “It sounds like you feel more hopeful today.” |
| Troubles | “What bothers you most about the situation?” | “When we met last week, you said that _______ was the most upsetting part of this situation; how do you see that today?” “What has been the most troubling issue that has arisen since we last met?” |
| Handling | “How are you managing or coping with the situation?” | “How could you approach the situation?” |
| Empathy | “That sounds very frustrating.” | “That sounds very difficult.” |
The background question deliberately encourages the patient to focus on a specified present topic or event since the most recent office visit. It is not usually productive or practical to pursue a detailed history, and physicians should generally avoid the psychotherapist’s, “Tell me more about that?” query.3,19
Affect is the next step. Nonverbal cues such as tone of voice, posture, and facial expression can be clues to emotional states that the physician can encourage the patient to consider, because some patients may have difficulty articulating their feelings.9,15
The troubles question is particularly useful with patients who are overwhelmed or are responding to a major life stressor, and it provides focus for the remaining queries. The physician should not assume that he or she knows what is most troubling to the patient.9,15 For example, if a patient’s spouse has just announced that she is filing for divorce, the key concern may not be loss of the relationship but financial worry about how to survive on a single income.
Handling is primarily an issue of coping. When there are specific actions that would render a situation less distressing, a problem focus is most helpful (e.g., learning about available treatment options for newly diagnosed cancer). However, for uncontrollable situations such as the death of a loved one, emotion-focused coping may be associated with less distress.46 In this approach, the patient is encouraged to consider activities that can help him or her get through an emotionally difficult period. An expression of empathy closes the interview.
Approach to the Patient
These counseling strategies should be implemented in a stepped care model.47 For patients who respond to direct physician advice, the five A’s and FRAMES are likely to be effective. When patient motivation is a factor, the stages of change can guide counseling. Motivational interviewing techniques for increasing patient awareness of risk and resolving ambivalence are indicated for patients who are not interested in addressing health risk behavior. For patients with psychiatric conditions and broader psychosocial issues, the BATHE technique is a useful starting point.3,15
A common dilemma is how to proceed when patients exhibit comorbid problems such as smoking and excessive alcohol use. Historically, physicians were advised to target one behavior at a time.48 Recent research suggests that this limitation may not be necessary.49 In a recent study clinicians used transtheoretical model–based counseling to address three weight-related behaviors simultaneously (e.g., reducing fat intake by less than 30% of overall calories consumed, increasing exercise to 30 minutes at least five times per week, and reducing daily food intake by 500 calories). Patients progressing to the action or maintenance stage with one behavior were twice as likely to move to the action or maintenance stage with a second behavior during a 24-month period compared with a usual care group.49
Physicians capitalizing on the teachable moment, estimated to occur in 10% of primary care office visits, may have greater counseling success.50 These moments are typically acute medical events or pregnancy that increase patients’ motivation for change.50 For example, a patient presenting with acute bronchitis may be more open to discussing smoking cessation, particularly when the physician connects the acute symptoms to cigarettes.
Patients with psychiatric conditions or psychosocial stressors will benefit from the BATHE technique, combined with psychotropic medication when appropriate.51 These patients should be closely monitored to assess their response to this initial intervention. Patients demonstrating a minimal response to brief psychosocial counseling should be referred for subspecialty mental health care.
Data Sources: Search terms included counseling and psychotherapy paired with primary health care. Some of the counseling strategies described (five A’s, FRAMES, BATHE) were entered alone. Motivational interviewing and transtheoretical (stages of change) model were paired with primary medical care. The author’s previous articles (references 3 and 15) were reviewed for recent citations. In addition to Medline, searches were run in the Agency for Health Care Research and Quality database, Cochrane Database of Systematic Reviews, U.S. Preventive Services Task Force, and the Substance Abuse and Mental Health Services Administration. Finally, to search for applications of newer counseling approaches to the primary care setting, acceptance and commitment therapy, solution focused therapy, and positive psychology were paired with primary medical care in Medline. Search dates: October 2017 through January 2018, and April, May, and September 2018.

