The adult well-male examination should provide evidence-based guidance toward the promotion of optimal health and well-being. The medical history should focus on tobacco and alcohol use, risk of human immunodeficiency virus and other sexually transmitted infections, and diet and exercise habits. The physical examination should include blood pressure screening, and height and weight measurements to calculate body mass index. Lipid screening is performed in men 40 to 75 years of age; there is insufficient evidence for screening younger men. One-time screening ultrasonography for detection of abdominal aortic aneurysm is recommended in men 65 to 75 years of age who have ever smoked. Screening for prostate cancer using prostate-specific antigen testing in men 55 to 69 years of age should be individualized using shared decision making. Screening for colorectal cancer should begin at 50 years of age for average-risk men and continue until at least 75 years of age. Screening options include fecal immunochemical testing, colonoscopy, or computed tomography colonography. Lung cancer screening using low-dose computed tomography is recommended in men 55 to 80 years of age who have at least a 30-pack-year smoking history and currently smoke or have quit within the past 15 years. Immunizations should be updated according to guidelines from the Advisory Committee on Immunization Practices.
The goals of the adult well-male examination are to provide evidence-based guidance toward the promotion of optimal health and well-being, to screen for and potentially prevent premature morbidity and mortality from chronic diseases, and to provide age-appropriate cancer screening and immunizations. Most primary care guidelines come from the U.S. Preventive Services Task Force (USPSTF) and have been adopted by the American Academy of Family Physicians (AAFP).1,2 Some subspecialty guidelines offer additional guidance but may have conflicting recommendations. Currently, there is no accepted guideline for frequency of adult well-male examinations, although many private health insurance plans and Medicare recommend annual examinations.
WHAT IS NEW ON THIS TOPIC
The life expectancy of U.S. men in 2015 was 76.3 years, a slight decrease from previous averages and five years lower than that of women.
The U.S. Preventive Services Task Force found insufficient evidence to recommend for or against lipid screening in any risk group younger than 40 years.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
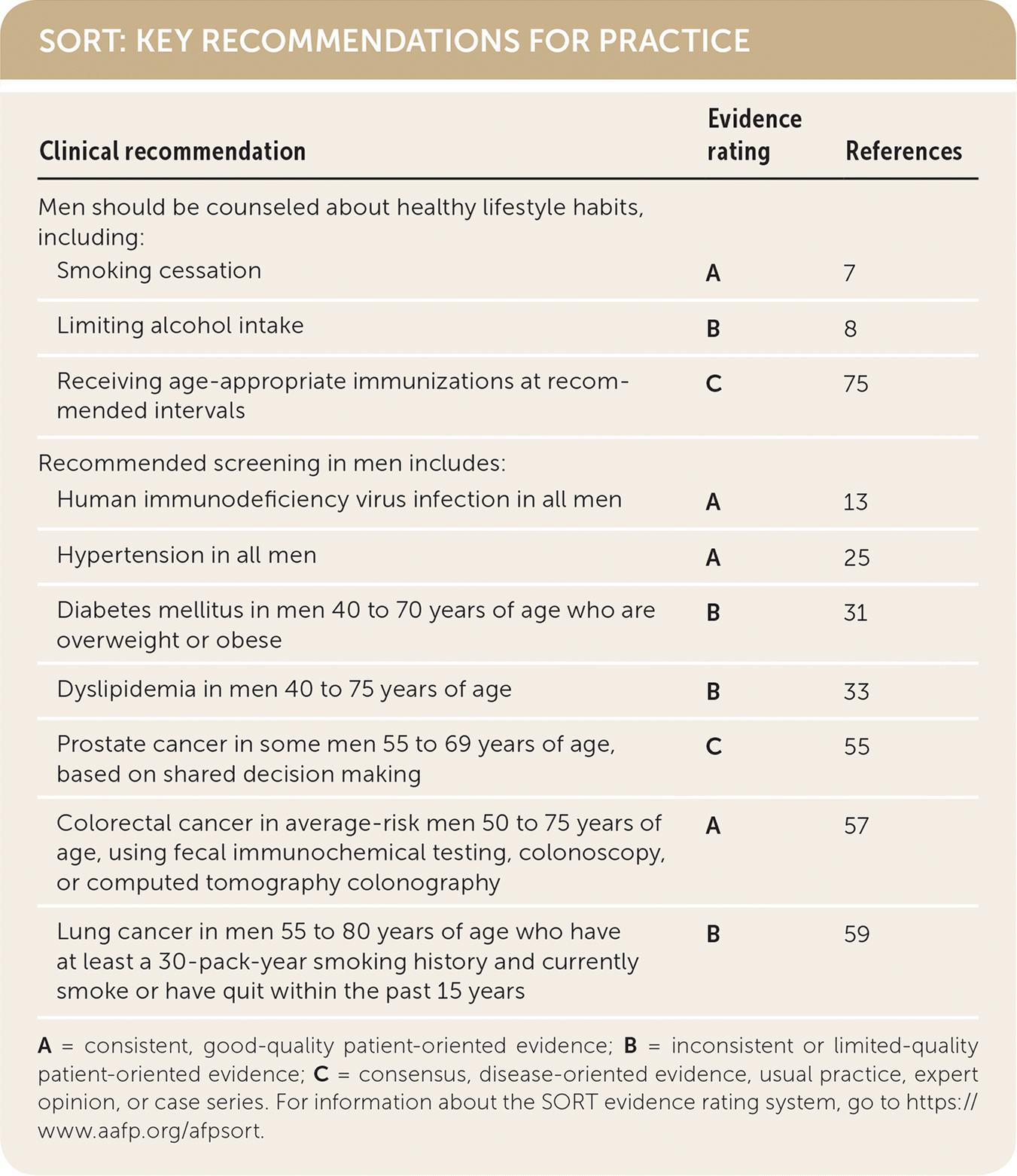
| Clinical recommendation | Evidence rating | References | |
|---|---|---|---|
| Men should be counseled about healthy lifestyle habits, including: | |||
| Smoking cessation | A | 7 | |
| Limiting alcohol intake | B | 8 | |
| Receiving age-appropriate immunizations at recommended intervals | C | 75 | |
| Recommended screening in men includes: | |||
| Human immunodeficiency virus infection in all men | A | 13 | |
| Hypertension in all men | A | 25 | |
| Diabetes mellitus in men 40 to 70 years of age who are overweight or obese | B | 31 | |
| Dyslipidemia in men 40 to 75 years of age | B | 33 | |
| Prostate cancer in some men 55 to 69 years of age, based on shared decision making | C | 55 | |
| Colorectal cancer in average-risk men 50 to 75 years of age, using fecal immunochemical testing, colonoscopy, or computed tomography colonography | A | 57 | |
| Lung cancer in men 55 to 80 years of age who have at least a 30-pack-year smoking history and currently smoke or have quit within the past 15 years | B | 59 | |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
In 2007, men 15 to 65 years of age were significantly less likely than women to seek preventive care services from a primary care physician (15% vs. 44% of total visits, respectively).3 In 2000, one in three men reported not having a primary care physician, compared with one in five women.4 No data are available on the impact of the Patient Protection and Affordable Care Act. The life expectancy of U.S. men in 2015 was 76.3 years, a slight decrease from previous averages and five years lower than that of women.5 Table 1 includes Centers for Disease Control and Prevention statistics related to men’s health and well-being.6
TABLE 1. Statistics on Men’s Health and Well-Being

| 56% of men ≥ 18 years meet the federal physical activity guidelines for aerobic activity through leisure-time aerobic activity* |
| 34% of men ≥ 20 years are obese† |
| 33% of men ≥ 20 years have hypertension and/or take antihypertensive medication† |
| 32% of men ≥ 18 years have had five or more alcoholic drinks in one day at least once in the past year* |
| 18% of men ≥ 18 years currently smoke cigarettes* |
| 12% of men < 65 years do not have health insurance* |
| 12% of men ≥ 18 years rate their overall health as fair or poor‡ |
*—2016 data.
†—2011 to 2014 data.
‡—2015 data.
Information from reference 6.
History
For the evaluation of men, the patient history should be comprised of medical and surgical histories, current medications, and allergies. Family history relevant to the risk of chronic diseases and cancer should also be included. Social history should focus on lifestyle risks that contribute to premature morbidity and mortality, including substance use, risk of human immunodeficiency virus and other sexually transmitted infections (STIs), and diet and exercise habits. Evaluation of men with Medicare should also include gait stability, their ability to achieve activities of daily living, and depression screening.
Screening for Lifestyle and Mental Health Risks
TABLE 2. Screening Guidelines for Lifestyle and Mental Health Risks in Men
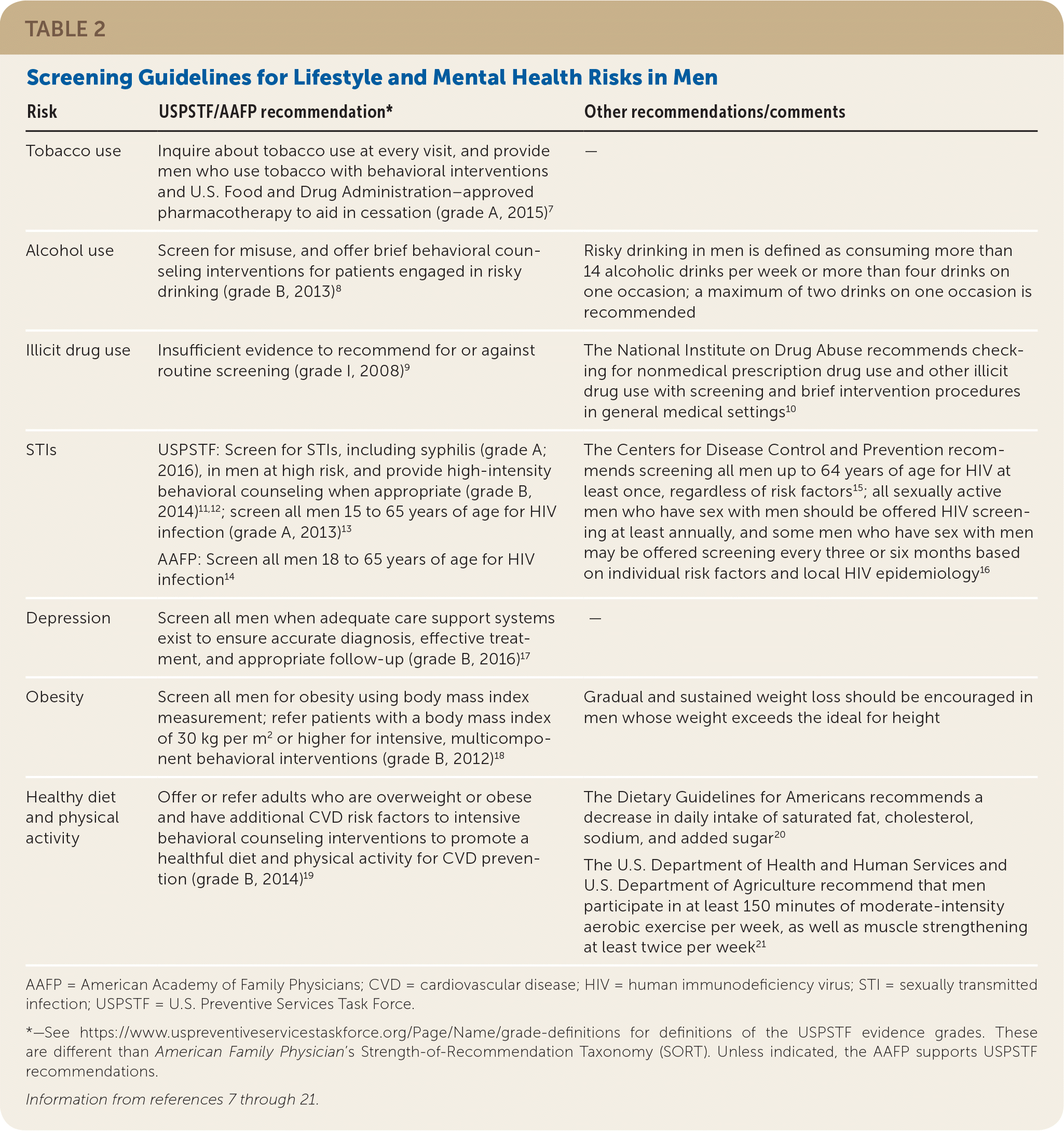
| Risk | USPSTF/AAFP recommendation* | Other recommendations/comments |
|---|---|---|
| Tobacco use | Inquire about tobacco use at every visit, and provide men who use tobacco with behavioral interventions and U.S. Food and Drug Administration–approved pharmacotherapy to aid in cessation (grade A, 2015)7 | — |
| Alcohol use | Screen for misuse, and offer brief behavioral counseling interventions for patients engaged in risky drinking (grade B, 2013)8 | Risky drinking in men is defined as consuming more than 14 alcoholic drinks per week or more than four drinks on one occasion; a maximum of two drinks on one occasion is recommended |
| Illicit drug use | Insufficient evidence to recommend for or against routine screening (grade I, 2008)9 | The National Institute on Drug Abuse recommends checking for nonmedical prescription drug use and other illicit drug use with screening and brief intervention procedures in general medical settings10 |
| STIs | USPSTF: Screen for STIs, including syphilis (grade A; 2016), in men at high risk, and provide high-intensity behavioral counseling when appropriate (grade B, 2014)11,12; screen all men 15 to 65 years of age for HIV infection (grade A, 2013)13 | The Centers for Disease Control and Prevention recommends screening all men up to 64 years of age for HIV at least once, regardless of risk factors15 ; all sexually active men who have sex with men should be offered HIV screening at least annually, and some men who have sex with men may be offered screening every three or six months based on individual risk factors and local HIV epidemiology16 |
| AAFP: Screen all men 18 to 65 years of age for HIV infection14 | ||
| Depression | Screen all men when adequate care support systems exist to ensure accurate diagnosis, effective treatment, and appropriate follow-up (grade B, 2016)17 | — |
| Obesity | Screen all men for obesity using body mass index measurement; refer patients with a body mass index of 30 kg per m2 or higher for intensive, multicomponent behavioral interventions (grade B, 2012)18 | Gradual and sustained weight loss should be encouraged in men whose weight exceeds the ideal for height |
| Healthy diet and physical activity | Offer or refer adults who are overweight or obese and have additional CVD risk factors to intensive behavioral counseling interventions to promote a healthful diet and physical activity for CVD prevention (grade B, 2014)19 | The Dietary Guidelines for Americans recommends a decrease in daily intake of saturated fat, cholesterol, sodium, and added sugar20 |
| The U.S. Department of Health and Human Services and U.S. Department of Agriculture recommend that men participate in at least 150 minutes of moderate-intensity aerobic exercise per week, as well as muscle strengthening at least twice per week21 |
AAFP = American Academy of Family Physicians; CVD = cardiovascular disease; HIV = human immunodeficiency virus; STI = sexually transmitted infection; USPSTF = U.S. Preventive Services Task Force.
*—See https://www.uspreventiveservicestaskforce.org/Page/Name/grade-definitions for definitions of the USPSTF evidence grades. These are different than American Family Physician’s Strength-of-Recommendation Taxonomy (SORT). Unless indicated, the AAFP supports USPSTF recommendations.
TOBACCO AND SUBSTANCE USE
Men should be asked about tobacco and alcohol use at every visit.7,8 The USPSTF found insufficient evidence to recommend for or against screening for illicit drug use9; however, the National Institute on Drug Abuse recommends screening for nonmedical prescription drug use and other illicit drug use.10 Clinicians can use recommended counseling approaches such as the five A’s (ask, advise, assess, assist, and arrange), the CAGE questionnaire, or motivational interviewing.8,22
SEXUALLY TRANSMITTED INFECTIONS
Men with risk factors, including men with multiple sex partners, men who engage in unprotected sex, and men who have sex with men, should be screened for STIs.11,12,23 There is good evidence of increased yield from routine screening for human immunodeficiency virus infection in persons who report no individual risk factors but are seen in high-risk or high-prevalence clinical settings, including STI clinics, correctional facilities, homeless shelters, tuberculosis clinics, clinics serving men who have sex with men, and adolescent health clinics that have a high prevalence of STIs. However, all men should be offered screening.13
One study concluded that counseling patients about the use of condoms is likely to benefit some patients at STI clinics and minimize the risk of infection transmission, although it is unlikely to benefit men who have sex with men.24 The cost-effectiveness of implementing behavioral counseling in STI programs is unclear, but feasibility would be improved if behavioral counseling were implemented in the context of other prevention efforts.
DEPRESSION
Men should be screened for depression using the two-item Patient Health Questionnaire (PHQ; http://www.commonwealthfund.org/usr_doc/PHQ2.pdf). If results of the PHQ-2 are positive, the patient should be further evaluated using the PHQ-9 (https://www.phqscreeners.com/sites/g/files/g10049256/f/201412/PHQ-9_English.pdf).17
Screening for Chronic Conditions
TABLE 3. Screening Guidelines for Chronic Conditions in Men
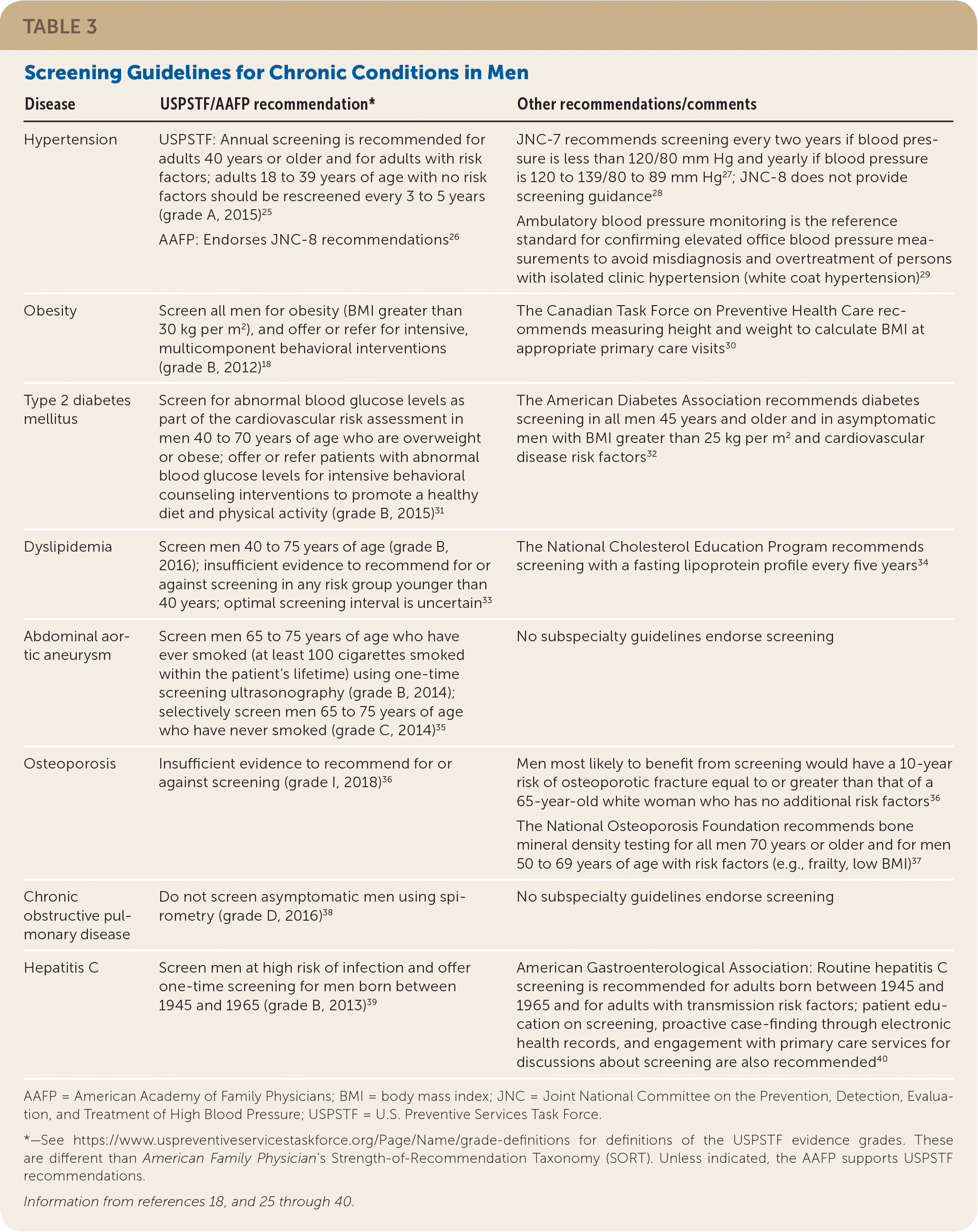
| Disease | USPSTF/AAFP recommendation* | Other recommendations/comments |
|---|---|---|
| Hypertension | USPSTF: Annual screening is recommended for adults 40 years or older and for adults with risk factors; adults 18 to 39 years of age with no risk factors should be rescreened every 3 to 5 years (grade A, 2015)25 | JNC-7 recommends screening every two years if blood pressure is less than 120/80 mm Hg and yearly if blood pressure is 120 to 139/80 to 89 mm Hg27; JNC-8 does not provide screening guidance28 |
| AAFP: Endorses JNC-8 recommendations26 | Ambulatory blood pressure monitoring is the reference standard for confirming elevated office blood pressure measurements to avoid misdiagnosis and overtreatment of persons with isolated clinic hypertension (white coat hypertension)29 | |
| Obesity | Screen all men for obesity (BMI greater than 30 kg per m2), and offer or refer for intensive, multicomponent behavioral interventions (grade B, 2012)18 | The Canadian Task Force on Preventive Health Care recommends measuring height and weight to calculate BMI at appropriate primary care visits30 |
| Type 2 diabetes mellitus | Screen for abnormal blood glucose levels as part of the cardiovascular risk assessment in men 40 to 70 years of age who are overweight or obese; offer or refer patients with abnormal blood glucose levels for intensive behavioral counseling interventions to promote a healthy diet and physical activity (grade B, 2015)31 | The American Diabetes Association recommends diabetes screening in all men 45 years and older and in asymptomatic men with BMI greater than 25 kg per m2 and cardiovascular disease risk factors32 |
| Dyslipidemia | Screen men 40 to 75 years of age (grade B, 2016); insufficient evidence to recommend for or against screening in any risk group younger than 40 years; optimal screening interval is uncertain33 | The National Cholesterol Education Program recommends screening with a fasting lipoprotein profile every five years34 |
| Abdominal aortic aneurysm | Screen men 65 to 75 years of age who have ever smoked (at least 100 cigarettes smoked within the patient’s lifetime) using one-time screening ultrasonography (grade B, 2014); selectively screen men 65 to 75 years of age who have never smoked (grade C, 2014)35 | No subspecialty guidelines endorse screening |
| Osteoporosis | Insufficient evidence to recommend for or against screening (grade I, 2018)36 | Men most likely to benefit from screening would have a 10-year risk of osteoporotic fracture equal to or greater than that of a 65-year-old white woman who has no additional risk factors36 |
| The National Osteoporosis Foundation recommends bone mineral density testing for all men 70 years or older and for men 50 to 69 years of age with risk factors (e.g., frailty, low BMI)37 | ||
| Chronic obstructive pulmonary disease | Do not screen asymptomatic men using spirometry (grade D, 2016)38 | No subspecialty guidelines endorse screening |
| Hepatitis C | Screen men at high risk of infection and offer one-time screening for men born between 1945 and 1965 (grade B, 2013)39 | American Gastroenterological Association: Routine hepatitis C screening is recommended for adults born between 1945 and 1965 and for adults with transmission risk factors; patient education on screening, proactive case-finding through electronic health records, and engagement with primary care services for discussions about screening are also recommended40 |
AAFP = American Academy of Family Physicians; BMI = body mass index; JNC = Joint National Committee on the Prevention, Detection, Evaluation, and Treatment of High Blood Pressure; USPSTF = U.S. Preventive Services Task Force.
*—See https://www.uspreventiveservicestaskforce.org/Page/Name/grade-definitions for definitions of the USPSTF evidence grades. These are different than American Family Physician’s Strength-of-Recommendation Taxonomy (SORT). Unless indicated, the AAFP supports USPSTF recommendations.
CARDIOVASCULAR RISK
Components of the adult well-male examination include blood pressure screening and height and weight measurements to calculate body mass index (BMI).18,25
Hypertension. Men should be screened for high blood pressure.25 When treatment decisions are being made, blood pressure should be considered with global risk of cardiovascular disease (CVD); smoking status; presence of diabetes mellitus, dyslipidemia, or obesity; physical activity level; age; and sex.25 Hypertension (defined as a systolic blood pressure of 140 mm Hg or higher or a diastolic blood pressure of 90 mm Hg or higher by the Eighth Report of the Joint National Committee on the Prevention, Detection, Evaluation, and Treatment of High Blood Pressure [JNC-8]) can be diagnosed after two or more elevated readings are obtained on at least two visits over a period of one to several weeks.28 Recent guidelines recommend a cutoff for stage 1 hypertension of 130 to 139 mm Hg systolic or 80 to 89 mm Hg diastolic 41; however, the AAFP continues to support the cutoff recommended by the JNC-8.26,42
Evidence supports ambulatory blood pressure monitoring as the reference standard for confirming elevated office blood pressure measurements to avoid misdiagnosis and overtreatment of persons with isolated clinic hypertension (white coat hypertension).29 The ASCVD (Atherosclerotic Cardiovascular Disease) Risk Estimator (available at http://tools.acc.org/ASCVD-Risk-Estimator-Plus/#!/calculate/estimate/) can be used to determine the 10-year risk of cardiovascular events or stroke in men 40 to 79 years of age.
Obesity. Height and weight measurements should be obtained at every visit to calculate BMI.18 An abdominal (waist) circumference greater than 40 inches is associated with an increased risk of type 2 diabetes, dyslipidemia, hypertension, and CVD in men with a BMI of 25 to 35 kg per m2.43 In persons with a BMI of 35 kg per m2 or greater, determination of waist circumference has limited additional value in the prediction of CVD risk.43 In Asian and black men, waist circumference and other measures such as waist-to-height ratio may be better indicators of CVD risk than BMI because BMI does not adequately account for differences in visceral fat distribution.43
Diabetes. Among men 20 years and older, more than 15 million have diabetes and approximately 44.5 million have prediabetes.44 Diabetes is considered a CVD risk equivalent because diabetes-related comorbidity with other risk factors leads to a higher risk of CVD within 10 years.31 The American Diabetes Association defines diabetes as an A1C level of 6.5% or higher; fasting plasma glucose concentration of 126 mg per dL (7.0 mmol per L) or greater; plasma glucose concentration of 200 mg per dL (11.1 mmol per L) or greater two hours after a 75-g oral glucose load; and a random plasma glucose concentration of 200 mg per dL or greater in a patient with classic symptoms of hyperglycemia or hyperglycemic crisis (e.g., polyuria, polydipsia, polyphagia).32
Dyslipidemia. The USPSTF recommends lipid screening in men 40 to 75 years of age; a risk calculator is then used to determine the need for treatment.33 The optimal interval for screening is uncertain.33 Notably, the USPSTF found insufficient evidence to recommend for or against screening in any risk group younger than 40 years.33
Risk factors for CVD include elevated low-density lipoprotein cholesterol, history of CVD or noncoronary atherosclerosis, diabetes, smoking, hypertension, obesity, and family history of CVD before 50 years of age in male relatives or before 60 years of age in female relatives.33,34
Fasting lipoprotein profile is the preferred screening test for dyslipidemia.33,34 For nonfasting samples, total cholesterol and high-density lipoprotein cholesterol measurements are recommended and are sufficient for calculating 10-year cardiovascular risk using most calculators.45,46
Abdominal Aortic Aneurysm. The USPSTF recommends one-time screening ultrasonography for detection of abdominal aortic aneurysm in men 65 to 75 years of age who have ever smoked.35 Randomized trials show that the benefits of screening and surgical repair in this high-risk group outweigh potential harms.35 The pooled prevalence of abdominal aortic aneurysm is 4.4%.47 The mortality rate after dissection and rupture approaches 80% for men who reach the hospital and 50% for men who undergo emergent surgical repair.48 Smoking is the risk factor most strongly associated with abdominal aortic aneurysm (odds ratio = 5.07) and accounts for 75% of all aneurysms 4 cm or greater.49 Other risk factors include hypertension, dyslipidemia, family history, and atherosclerosis. A meta-analysis determined that a well-functioning screening program would reduce abdominal aortic aneurysm–related mortality by at least 45%; the number needed to screen to prevent one rupture is 238.50
OSTEOPOROSIS
The USPSTF found insufficient evidence to recommend for or against screening men for osteoporosis, given that the relative benefits and harms of therapy for osteoporosis in men have not been determined.36 Although evidence for screening is lacking, men most likely to benefit from screening would have a 10-year risk of osteoporotic fracture equal to or greater than that of a 65-year-old white woman with no additional risk factors.36 For men, major risk factors include increasing age, white race, and family history. The National Osteoporosis Foundation recommends bone mineral density testing for all men 70 years or older and men 50 to 69 years of age with risk factors (e.g., frailty, low BMI).37 The USPSTF found insufficient evidence to recommend for or against calcium and vitamin D supplementation to prevent fractures.51
CHRONIC OBSTRUCTIVE PULMONARY DISEASE
The USPSTF recommends against screening adults for chronic obstructive pulmonary disease (COPD) using spirometry.38 Men with COPD, including those with mild or moderate illness, benefit from smoking cessation and annual influenza vaccination. Moderate evidence suggests that influenza vaccination reduces COPD exacerbations.38
HEPATITIS C
Screening for hepatitis C should be offered to men at high risk of infection. Adults born between 1945 and 1965 should be offered one-time screening.39
Cancer Screening
TABLE 4. Cancer Screening Guidelines for Men
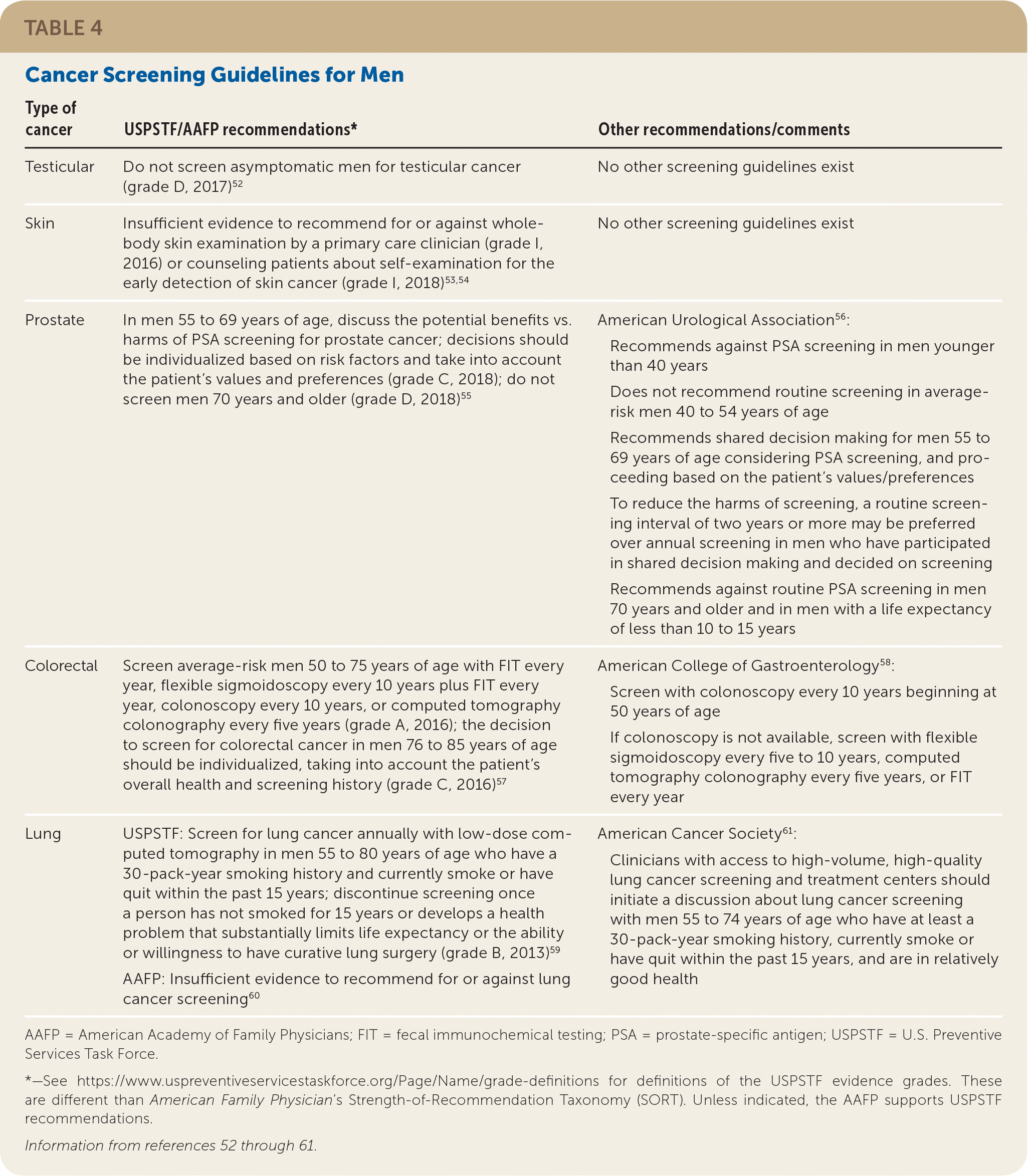
| Type of cancer | USPSTF/AAFP recommendations* | Other recommendations/comments |
|---|---|---|
| Testicular | Do not screen asymptomatic men for testicular cancer (grade D, 2017)52 | No other screening guidelines exist |
| Skin | Insufficient evidence to recommend for or against whole-body skin examination by a primary care clinician (grade I, 2016) or counseling patients about self-examination for the early detection of skin cancer (grade I, 2018)53,54 | No other screening guidelines exist |
| Prostate | In men 55 to 69 years of age, discuss the potential benefits vs. harms of PSA screening for prostate cancer; decisions should be individualized based on risk factors and take into account the patient’s values and preferences (grade C, 2018); do not screen men 70 years and older (grade D, 2018)55 | American Urological Association56:
|
| Colorectal | Screen average-risk men 50 to 75 years of age with FIT every year, flexible sigmoidoscopy every 10 years plus FIT every year, colonoscopy every 10 years, or computed tomography colonography every five years (grade A, 2016); the decision to screen for colorectal cancer in men 76 to 85 years of age should be individualized, taking into account the patient’s overall health and screening history (grade C, 2016)57 | American College of Gastroenterology58:
|
| Lung | USPSTF: Screen for lung cancer annually with low-dose computed tomography in men 55 to 80 years of age who have a 30-pack-year smoking history and currently smoke or have quit within the past 15 years; discontinue screening once a person has not smoked for 15 years or develops a health problem that substantially limits life expectancy or the ability or willingness to have curative lung surgery (grade B, 2013)59 AAFP: Insufficient evidence to recommend for or against lung cancer screening60 | American Cancer Society61:
|
AAFP = American Academy of Family Physicians; FIT = fecal immunochemical testing; PSA = prostate-specific antigen; USPSTF = U.S. Preventive Services Task Force.
*—See https://www.uspreventiveservicestaskforce.org/Page/Name/grade-definitions for definitions of the USPSTF evidence grades. These are different than American Family Physician’s Strength-of-Recommendation Taxonomy (SORT). Unless indicated, the AAFP supports USPSTF recommendations.
TESTICULAR CANCER
The USPSTF recommends against screening asymptomatic men for testicular cancer. Because the incidence of testicular cancer is very low and treatment is often effective even in advanced stages, the benefits of earlier detection are minimal and likely outweighed by the harms of false-positive results and unnecessary workup for benign conditions.52
SKIN CANCER
The USPSTF concludes that there is insufficient evidence to assess the benefits vs. harms of a whole-body skin examination performed by a primary care clinician for the early detection of skin cancer in men. It concludes that there is also insufficient evidence to assess the benefits vs. harms of counseling patients about performing self-examinations.53,54
PROSTATE CANCER
Screening for prostate cancer in primary care is controversial because it is widely believed that screening has resulted in overdiagnosis and overtreatment of clinically insignificant cancers. An editorial on prostate cancer screening was published in American Family Physician (available at https://www.aafp.org/afp/2018/1015/p478.html).
Previous USPSTF recommendations argued against screening for prostate cancer with prostate-specific antigen testing because of possible harms, based on data from the European Randomized Study of Screening for Prostate Cancer and the Prostate, Lung, Colorectal, and Ovarian Cancer Screening Trial.62 Current USPSTF and AAFP guidelines align with American Urological Association guidelines in recommending a discussion of benefits vs. risks of screening for men 55 to 69 years of age and using a shared decision-making approach; screening decisions should be individualized based on risk factors (i.e., family history, black race) and take into account the patient’s values and preferences.55,56,63 The USPSTF and AAFP recommend against prostate-specific antigen screening for prostate cancer in men 70 years and older.55,56
Although not recommended by the USPSTF, expert opinion from the American Urological Association and data from an uncontrolled trial suggest that prostate cancer screening should combine the digital rectal examination and prostate-specific antigen test, which improves detection compared with either test alone (positive predictive value = 18% and 45%, respectively).56,64
COLORECTAL CANCER
Screening for colorectal cancer should begin at 50 years of age for average-risk men and continue until at least 75 years of age.57 Colonoscopy is increasingly becoming the test of choice for colorectal cancer screening in primary care, yet there are no randomized controlled trials comparing colonoscopy, flexible sigmoidoscopy, and fecal occult blood testing (FOBT) with a definable outcome of cancer-specific or all-cause mortality.57,65,66 Fecal immunochemical testing has greater sensitivity and specificity compared with guaiac-based FOBT.67 Fecal DNA testing has not proved more accurate than FOBT or fecal immunochemical testing and has more false-positive results than FOBT (16% vs. 5%).68 Computed tomography colonography may result in harms from low-dose ionizing radiation exposure or identification of extracolonic findings.69
LUNG CANCER
Lung cancer is the third most common cancer and the leading cause of preventable cancer-related death in the United States.70 Smoking is the most important risk factor for lung cancer, accounting for approximately 85% of cases.71 The USPSTF recommends annual screening for lung cancer with low-dose computed tomography in adults 55 to 80 years of age who have at least a 30-pack-year smoking history and currently smoke or have quit within the past 15 years,59,72 whereas the AAFP concludes that the evidence is insufficient to recommend for or against screening.60 Physicians should be aware of the high rate of false-positives with low-dose computed tomography screening; more than one-half of patients require additional testing and tracking, of which only 1.5% receive a lung cancer diagnosis.73 Screening should be discontinued once a patient has not smoked for 15 years or if a patient develops a health problem that substantially limits life expectancy or the ability or willingness to have curative lung surgery.59
Immunizations
The Advisory Committee on Immunization Practices (ACIP) strongly encourages annual influenza vaccination for all adults, with the high-dose preparation recommended for those older than 65 years. ACIP recommends a single tetanus toxoid, reduced diphtheria toxoid, and acellular pertussis (Tdap) vaccination, regardless of when the last tetanus and diphtheria toxoids (Td) booster was given.74
A vaccine series does not need to be restarted, even if a long period has passed between doses, although immunity may need to be verified via serologic testing.74 Full ACIP vaccine recommendations are available at https://www.cdc.gov/vaccines/schedules/hcp/imz/adult.html.
This article updates a previous article on this topic by Heidelbaugh and Tortorello.75
Data Sources: I performed a bibliographic search of select men’s health topics highlighting USPSTF guidelines, the Cochrane Database of Systematic Reviews, Essential Evidence Plus, the American Urological Association, the Agency for Healthcare Research and Quality, DynaMed, and the National Guideline Clearinghouse database. I searched Medline using the terms men’s health, guidelines, evidence-based, hypertension, hyperlipidemia, obesity, diabetes mellitus, abdominal aortic aneurysm, osteoporosis, prostate cancer, colorectal cancer, lung cancer, testicular cancer, skin cancer, sexually transmitted diseases/infections, and immunizations. Original research studies cited within these guidelines were reviewed. Search dates: September through November 2017.

