Urine drug testing is an essential component of monitoring patients who are receiving long-term opioid therapy, and it has been suggested for patients receiving long-term benzodiazepine or stimulant therapy. Family physicians should be familiar with the characteristics and capabilities of screening and confirmatory drug tests. Immunoassays are used for initial screening and can give false-positive and false-negative results. All results are considered presumptive until confirmatory testing is performed. False-positive results have significant implications for a patient's pain treatment plan, and false-negative results can be a missed opportunity to detect misuse. Urine drug testing is an essential component of monitoring patients who are receiving long-term opioid therapy, and it has been suggested for patients receiving long-term benzodiazepine or stimulant therapy. Family physicians should be familiar with the characteristics and capabilities of screening and confirmatory drug tests. Immunoassays are qualitative tests used for initial screening of urine samples. They can give false-positive and false-negative results, so all results are considered presumptive until confirmatory testing is performed. Immunoassays for opioids may not detect commonly prescribed semisynthetic and synthetic opioids such as methadone and fentanyl; similarly, immunoassays for benzodiazepines may not detect alprazolam or clonazepam. Immunoassays can cross-react with other medications and give false-positive results, which have important implications for a patient's pain treatment plan. False-negative results can cause missed opportunities to detect misuse. Urine samples can be adulterated with other substances to mask positive results on urine drug testing. Family physicians must be familiar with these substances, the methods to detect them, and their effects on urine drug testing.
Urine drug testing is an important part of managing long-term opioid therapy. With the recent increase in deaths caused by opioid overdoses, several federal and state regulations have been enacted that recommend or require urine drug testing in patients receiving long-term opioid therapy. Similar guidance has been suggested for patients receiving long-term benzodiazepine or stimulant therapy. The purpose of urine drug testing is to monitor compliance with prescribed therapy and detect the use of nonprescribed and illicit substances, especially heroin and nonprescribed opioids and benzodiazepines, all of which can increase the risk of a fatal overdose.1,2 Weak evidence suggests that random urine drug testing decreases the use of illicit drugs in patients receiving long-term opioid therapy.3
WHAT IS NEW ON THIS TOPIC
Several federal and state regulations have been enacted that recommend or require urine drug testing in patients receiving long-term opioid therapy. Similar guidance may apply to patients receiving long-term benzodiazepine or stimulant therapy.
Ingestion of food containing poppy seeds will not cause a positive urine drug test result. Similarly, passive inhalation of marijuana smoke is unlikely to cause a positive tetrahydrocannabinol urine test result.
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Urine drug testing can be used to monitor compliance with prescribed therapy and detect the use of nonprescribed and illicit substances, especially opioids, benzodiazepines, and heroin. | C | 1 |
| Immunoassays are subject to false-positive and false-negative results. All positive and any unexpected negative results must be verified by confirmatory testing. | C | 9 |
| Casual dietary ingestion of poppy seeds does not cause a positive result for opioids on urine drug testing. | C | 22 |
| Casual exposure to cannabis smoke does not cause a positive result on urine drug testing. | C | 23 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
A positive urine drug test result has significant implications for a patient's pain treatment plan, as well as his or her personal and professional life. Many controlled substance treatment agreements specify that pain medications will be tapered off or stopped if a test result is positive. Some state regulatory agencies require consultation with a pain management subspecialist if misuse is suspected4; therefore, it is imperative that family physicians know how to order urine drug tests and interpret results.
Family physicians cannot rely on urine drug testing alone to determine adherence to therapy, nor can testing reliably detect intermittent use of nonprescribed substances. Because there are no typical behaviors that predict misuse or diversion, monitoring of patients receiving long-term opioid therapy should include a focused history using validated tools (e.g., Opioid Risk Tool, Addiction Behaviors Checklist, Pain Medication Questionnaire), physical examination, and use of prescription drug monitoring programs. Before ordering a urine drug test, the physician must note when the patient last took a prescription medication (to determine the likelihood of a positive test result), whether any other medications were taken concurrently (that might cross-react with the assay), and whether any nonprescribed or illicit substances were used (in the event of an unexpected positive result). The physician must also be aware of which substances are most commonly misused in the community.
Frequency of Testing
Guidelines from the American Pain Society5 and the Centers for Disease Control and Prevention1 on the use of long-term opioid therapy for chronic noncancer pain recommend periodic urine drug testing for adherence to treatment, but the frequency is left to the individual physician. More frequent testing is required for patients at high risk of misuse and those with aberrant behaviors.1 Table 1 lists suggested frequencies for urine drug testing based on individual risk factors.6
TABLE 1. Recommended Frequency for Urine Drug Testing

| Level of misuse risk | Frequency |
|---|---|
| Low (no risk factors) | Every 6 to 12 months |
| Moderate | Every 3 to 6 months |
| High (mental health disorder, substance use disorder, prior opioid misuse, aberrant behavior*) or opioid dosage > 120 morphine milligram equivalents | Every 1 to 3 months |
*—Aberrant behavior includes but is not limited to lost prescriptions, multiple requests for early refills, opioid prescriptions from multiple physicians, unauthorized dose escalation, and apparent intoxication.
Adapted with permission from Washington State Agency Medical Directors' Group. Interagency guideline on prescribing opioids for pain. 3rd ed. June 2015. http://www.agencymeddirectors.wa.gov/files/2015amdgopioidguideline.pdf. Accessed August 18, 2018.
Choosing the Correct Test
Urine, serum, saliva, sweat, and hair can be tested for the presence of drugs. However, urine testing is most common because of ease of collection, adequate sensitivity and specificity to detect commonly used drugs, and a longer window of detection than serum.7 Urine drug concentrations do not reflect serum concentrations; rather, they are a function of how rapidly a person metabolizes and eliminates the drug and its metabolites, as well as hydration status. Urine drug testing can be performed in the office as a point-of-care test, or the sample can be sent to a reference laboratory for testing. Testing may be performed for reasons other than monitoring opioid therapy,8 such as drug rehabilitation, employment requirements (e.g., for occupations that require special transportation licensing), military or sports participation, or legal situations. Properly performed urine drug testing involves two steps: an initial screening test followed by confirmatory testing for substances with positive screening results. Confirmatory testing is also needed in situations with an unexpected negative result as a means of distinguishing a false negative from a true negative.9
The initial screening test is usually an immunoassay, a qualitative test that screens for the five major drug classes targeted by federal workplace testing programs: opioids, cannabinoids, cocaine, amphetamines, and phencyclidine. Immunoassays can be performed at the point of care, provide rapid results, and are relatively inexpensive. Positive and unexpected negative samples are then sent to a reference laboratory for confirmatory testing. Immunoassays can also be sent to a reference laboratory with instructions to run confirmatory tests.
Specific immunoassays must be ordered for different substances; therefore, physicians should be familiar with the test used in their office and at the reference laboratory they routinely use. The typical immunoassay can detect only nonsynthetic opioids (morphine and codeine). The immunoassays used for workplace testing programs are useful for detecting illicit substances such as cannabis or cocaine, but they do not reliably detect synthetic or semisynthetic opioids (e.g., methadone, buprenorphine, oxycodone, oxymorphone, fentanyl) or help distinguish between various opioids. Therefore, many laboratories require a specific order to test for semisynthetic and synthetic opioids and other drugs such as carisoprodol (Soma). Immunoassays that test for the presence of other common prescription drugs, such as benzodiazepines, are also available. Many benzodiazepine immunoassays reliably detect nordiazepam (metabolite of diazepam [Valium]), oxazepam, and temazepam (Restoril), but not alprazolam (Xanax), lorazepam (Ativan), or clonazepam (Klonopin).10 Hence, a positive screening result must always be followed with confirmatory testing. Furthermore, if benzodiazepine use is suspected, the sample must be sent for additional testing despite a negative initial screening result.
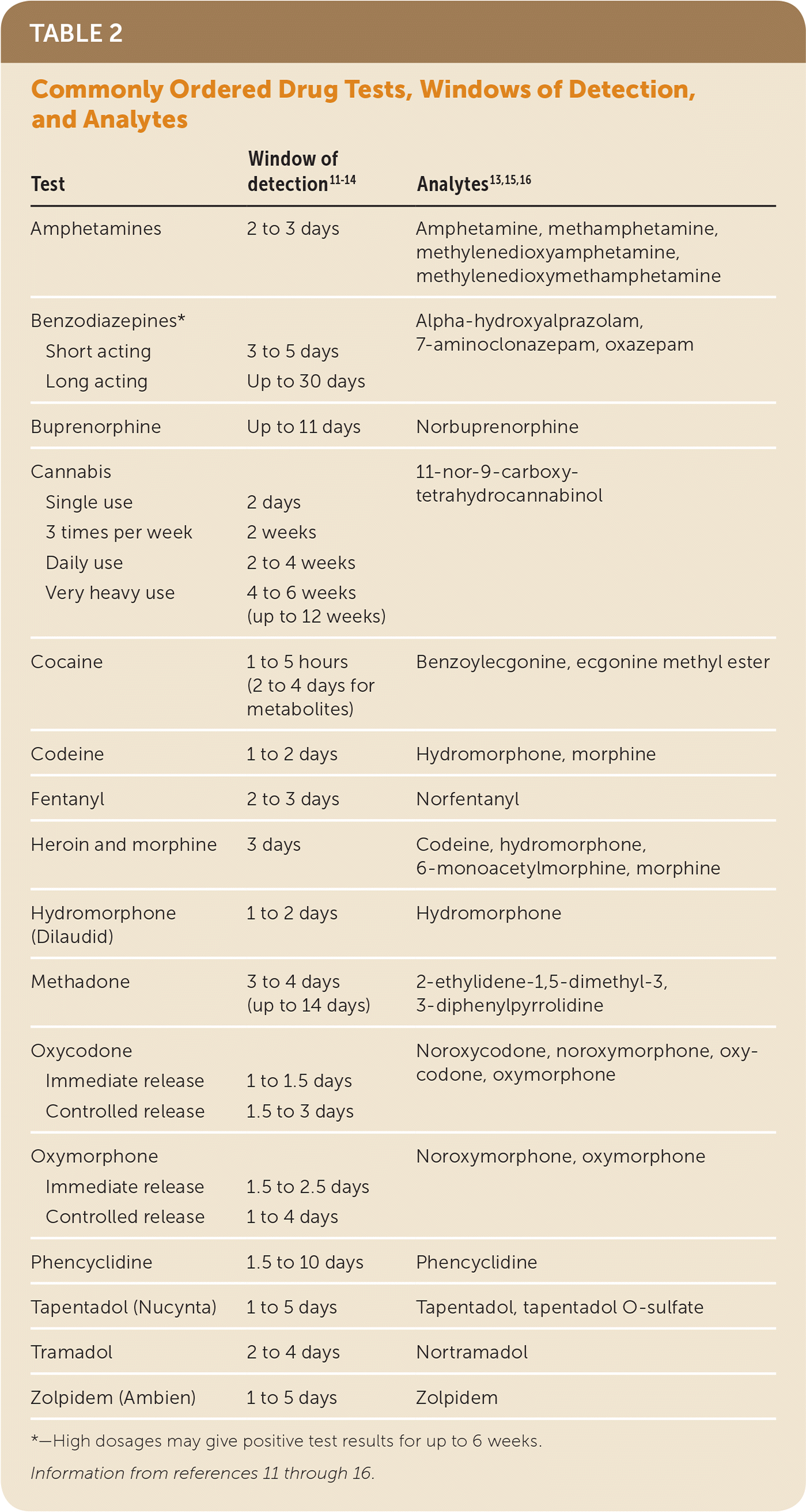
Most confirmatory tests use gas or high-performance liquid chromatography to separate various drugs, and mass spectrometry to detect them. These methods have a much lower threshold for detection and are able to accurately distinguish individual drugs and metabolites. Because of cost constraints, it is not practical to test each sample for every possible drug. The physician should be aware of which tests to order if nonadherence or substance misuse is suspected. The initial test should include the prescribed drug, amphetamines, opioids, cocaine, benzodiazepines, oxycodone, barbiturates, methadone, fentanyl, and marijuana.6 Table 2 lists commonly ordered tests, the principal drug analytes they detect, and their windows of detection.11–16
TABLE 2. Commonly Ordered Drug Tests, Windows of Detection, and Analytes
| Test | Window of detection11–14 | Analytes13,15,16 |
|---|---|---|
| Amphetamines | 2 to 3 days | Amphetamine, methamphetamine, methylenedioxyamphetamine, methylenedioxymethamphetamine |
| Benzodiazepines* | Alpha-hydroxyalprazolam, 7-aminoclonazepam, oxazepam | |
| Short acting | 3 to 5 days | |
| Long acting | Up to 30 days | |
| Buprenorphine | Up to 11 days | Norbuprenorphine |
| Cannabis | 11-nor-9-carboxy-tetrahydrocannabinol | |
| Single use | 2 days | |
| 3 times per week | 2 weeks | |
| Daily use | 2 to 4 weeks | |
| Very heavy use | 4 to 6 weeks (up to 12 weeks) | |
| Cocaine | 1 to 5 hours (2 to 4 days for metabolites) | Benzoylecgonine, ecgonine methyl ester |
| Codeine | 1 to 2 days | Hydromorphone, morphine |
| Fentanyl | 2 to 3 days | Norfentanyl |
| Heroin and morphine | 3 days | Codeine, hydromorphone, 6-monoacetylmorphine, morphine |
| Hydromorphone (Dilaudid) | 1 to 2 days | Hydromorphone |
| Methadone | 3 to 4 days (up to 14 days) | 2-ethylidene-1,5-dimethyl-3,3-diphenylpyrrolidine |
| Oxycodone | Noroxycodone, noroxymorphone, oxycodone, oxymorphone | |
| Immediate release | 1 to 1.5 days | |
| Controlled release | 1.5 to 3 days | |
| Oxymorphone | Noroxymorphone, oxymorphone | |
| Immediate release | 1.5 to 2.5 days | |
| Controlled release | 1 to 4 days | |
| Phencyclidine | 1.5 to 10 days | Phencyclidine |
| Tapentadol (Nucynta) | 1 to 5 days | Tapentadol, tapentadol O-sulfate |
| Tramadol | 2 to 4 days | Nortramadol |
| Zolpidem (Ambien) | 1 to 5 days | Zolpidem |
*—High dosages may give positive test results for up to 6 weeks.
Recently, several synthetic cannabinoids (e.g., spice), cathinones (e.g., bath salts), and hallucinogens (25I-NBOMe or N-bomb) have been sold as “legal stimulants” as a way to avoid regulatory controls.17,18 The manufacturers vary the chemical composition of these drugs, and most commercial urine drug tests are not able to detect them. If the patient's symptoms suggest ingestion of these drugs, urine and blood samples should be sent to laboratories that are capable of detecting them.
Interpreting Test Results
Many drugs are rapidly metabolized into active or inactive metabolites. Drug testing is dependent on detecting these metabolites. Opioids and benzodiazepines include multiple drugs with overlapping metabolic pathways, which can make interpretation of screening results difficult (eFigure A and eFigure B). Thus, the presence of morphine in a sample could indicate morphine, codeine, or heroin use, or any combination of these. Similarly, the presence of hydromorphone (Dilaudid) could indicate hydromorphone, hydrocodone, or morphine use.
eFIGURE A
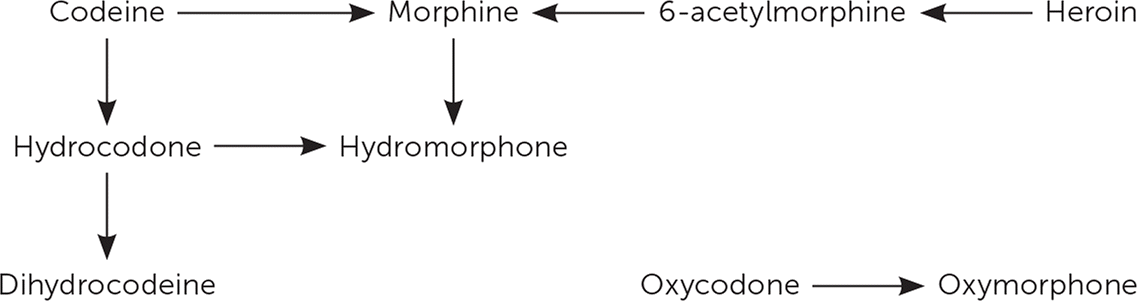
Metabolic pathways of opioids.
Information from:
Reisfield GM, Chronister CW, Goldberger BA, Bertholf RL. Unexpected urine drug testing results in a hospice patient on high-dose morphine therapy. Clin Chem. 2009;55(10):1766.
Reisfield GM, Salazar E, Bertholf RL. Rational use and interpretation of urine drug testing in chronic opioid therapy. Ann Clin Lab Sci. 2007;37(4):310.
eFIGURE B
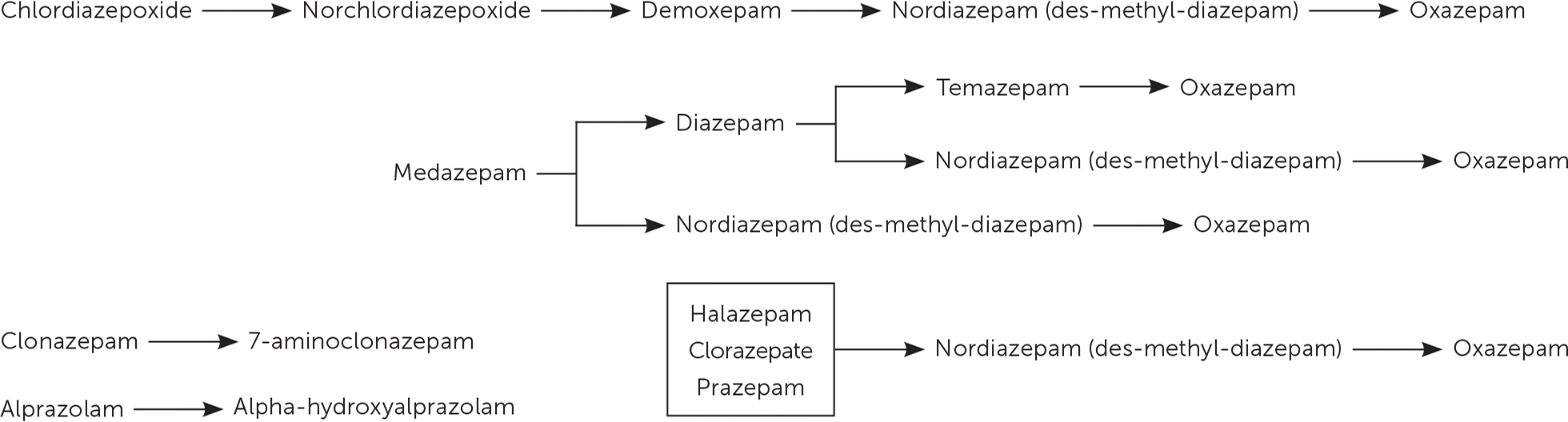
Metabolic pathways of benzodiazepines.
Information from Valentine JL, Middleton R, Sparks C. Identification of urinary benzodiazepines and their metabolites: comparison of automated HPLC and GC-MS after immunoassay screening of clinical specimens. J Anal Toxicol. 1996;20(6):419.
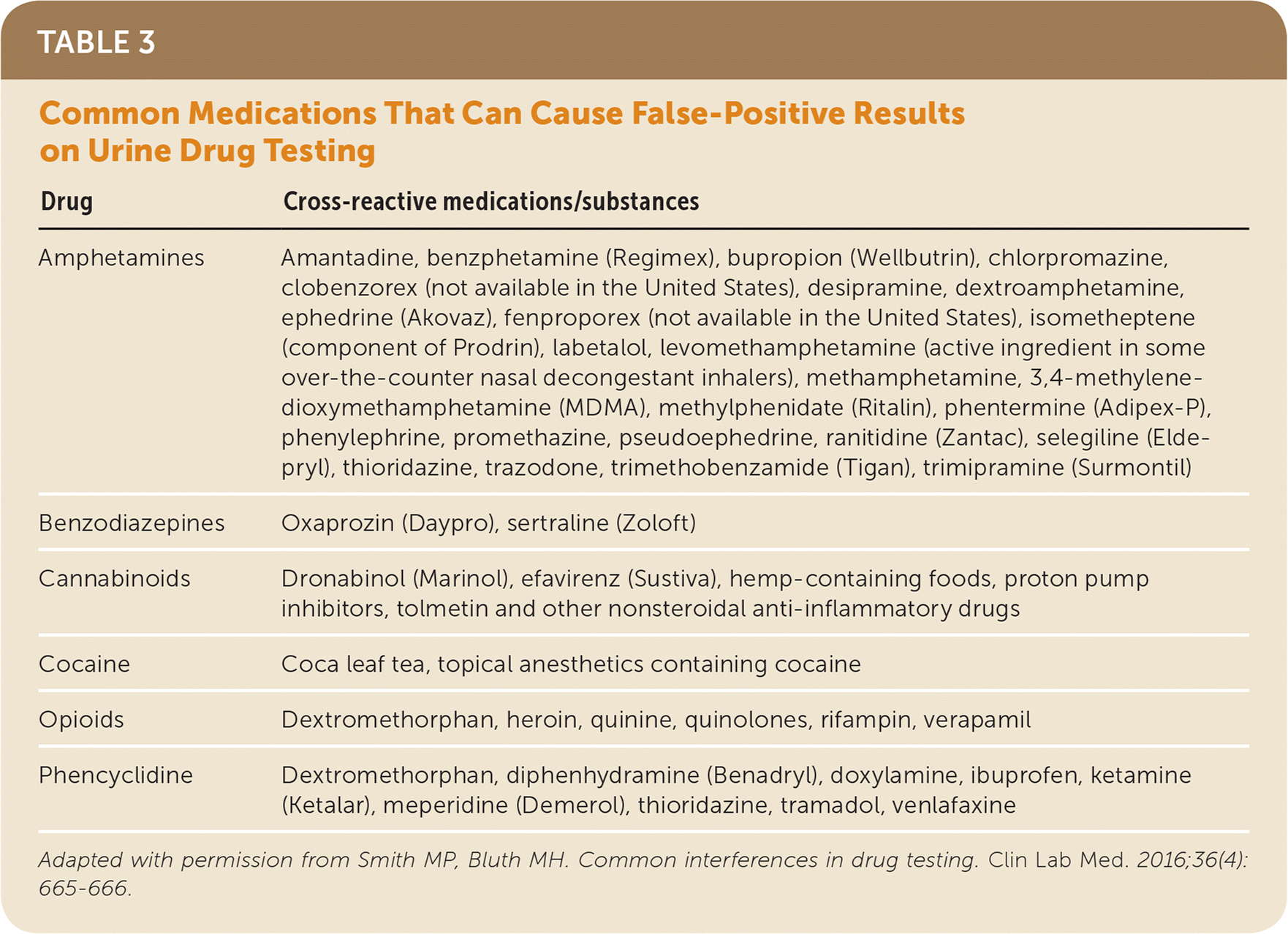
False-positive results can occur from cross-reactivity of commonly used medications with the assay. This a particular concern with immunoassays. Table 3 lists common medications that can cause false-positive results on urine drug testing.9 Negative results are particularly difficult to interpret, especially when a patient is receiving long-term opioid therapy and the physician expects a positive result. True-negative results occur when a patient is not taking the medication as prescribed and there is no drug present in the urine sample, or when the drug is metabolized so rapidly that the metabolites are eliminated before they can be detected. False-negative results occur when a drug or metabolite is present at such low levels that it is not detected. Confirmatory testing is essential to distinguish a true negative from a false negative. Contaminants can also interfere with the immunoassay's ability to detect the presence of drugs.
TABLE 3. Common Medications That Can Cause False-Positive Results on Urine Drug Testing
| Drug | Cross-reactive medications/substances |
|---|---|
| Amphetamines | Amantadine, benzphetamine (Regimex), bupropion (Wellbutrin), chlorpromazine, clobenzorex (not available in the United States), desipramine, dextroamphetamine, ephedrine (Akovaz), fenproporex (not available in the United States), isometheptene (component of Prodrin), labetalol, levomethamphetamine (active ingredient in some over-the-counter nasal decongestant inhalers), methamphetamine, 3,4-methylene-dioxymethamphetamine (MDMA), methylphenidate (Ritalin), phentermine (Adipex-P), phenylephrine, promethazine, pseudoephedrine, ranitidine (Zantac), selegiline (Eldepryl), thioridazine, trazodone, trimethobenzamide (Tigan), trimipramine (Surmontil) |
| Benzodiazepines | Oxaprozin (Daypro), sertraline (Zoloft) |
| Cannabinoids | Dronabinol (Marinol), efavirenz (Sustiva), hemp-containing foods, proton pump inhibitors, tolmetin and other nonsteroidal anti-inflammatory drugs |
| Cocaine | Coca leaf tea, topical anesthetics containing cocaine |
| Opioids | Dextromethorphan, heroin, quinine, quinolones, rifampin, verapamil |
| Phencyclidine | Dextromethorphan, diphenhydramine (Benadryl), doxylamine, ibuprofen, ketamine (Ketalar), meperidine (Demerol), thioridazine, tramadol, venlafaxine |
Adapted with permission from Smith MP, Bluth MH. Common interferences in drug testing. Clin Lab Med. 2016;36(4):665–666.
The use of heroin with concurrent prescription opioids is also a cause for concern. Although both substances will give a positive result for opioids, the presence of 6-monoacetylmorphine indicates heroin use. This metabolite has a short half-life, however, with a window of detection in urine of approximately two to eight hours. Acetylatedthebaine-4-metabolite glucuronide is a metabolite of thebaine, which is found in street heroin; it has been proposed as a new marker to differentiate morphine and codeine ingestion from heroin use.19,20 If concurrent opioid and heroin use is a concern, the pathologist or toxicologist at the local reference laboratory should be consulted to determine the appropriate ordering and testing procedure.
Tampering and Contamination of Urine Samples
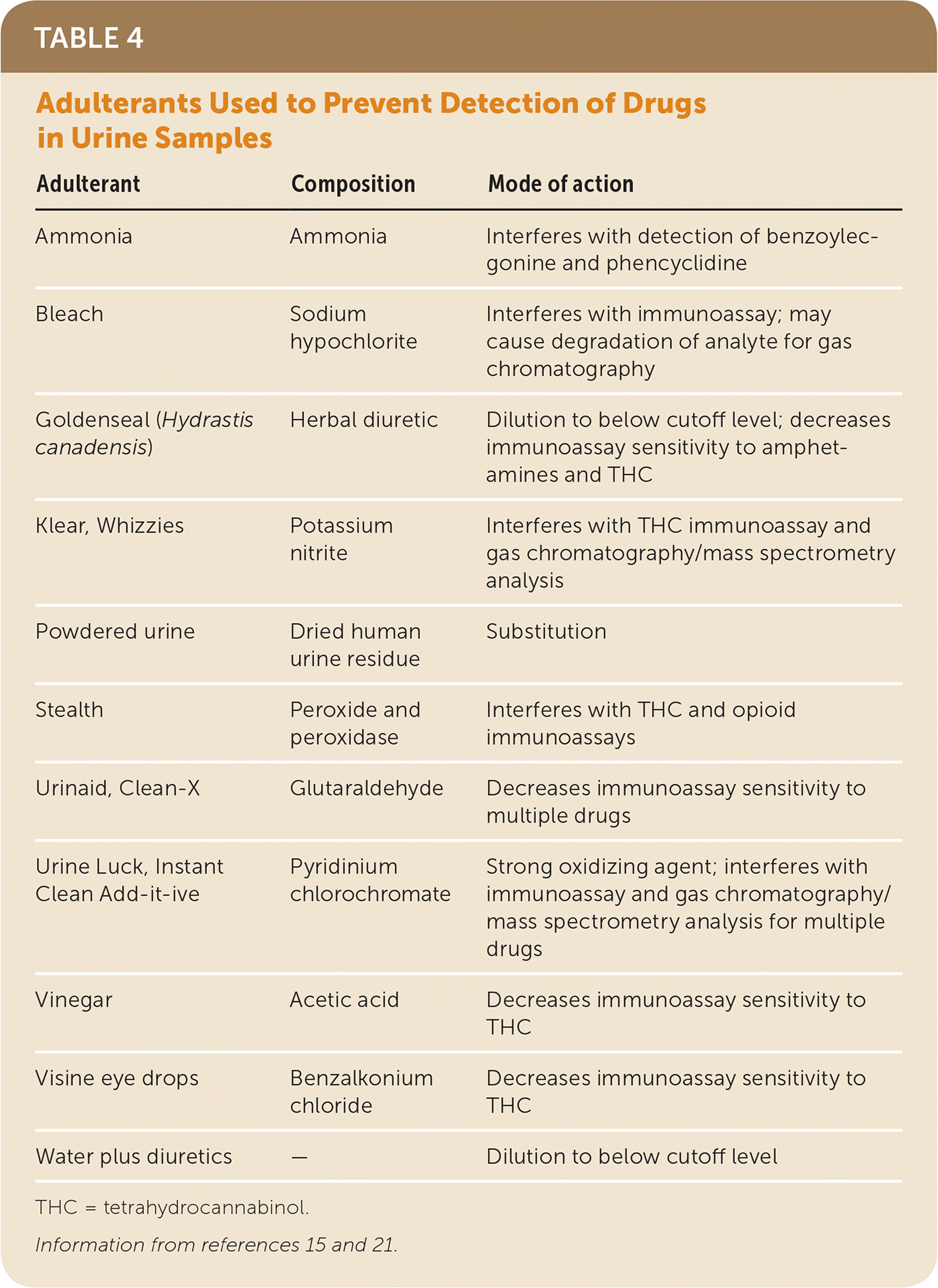
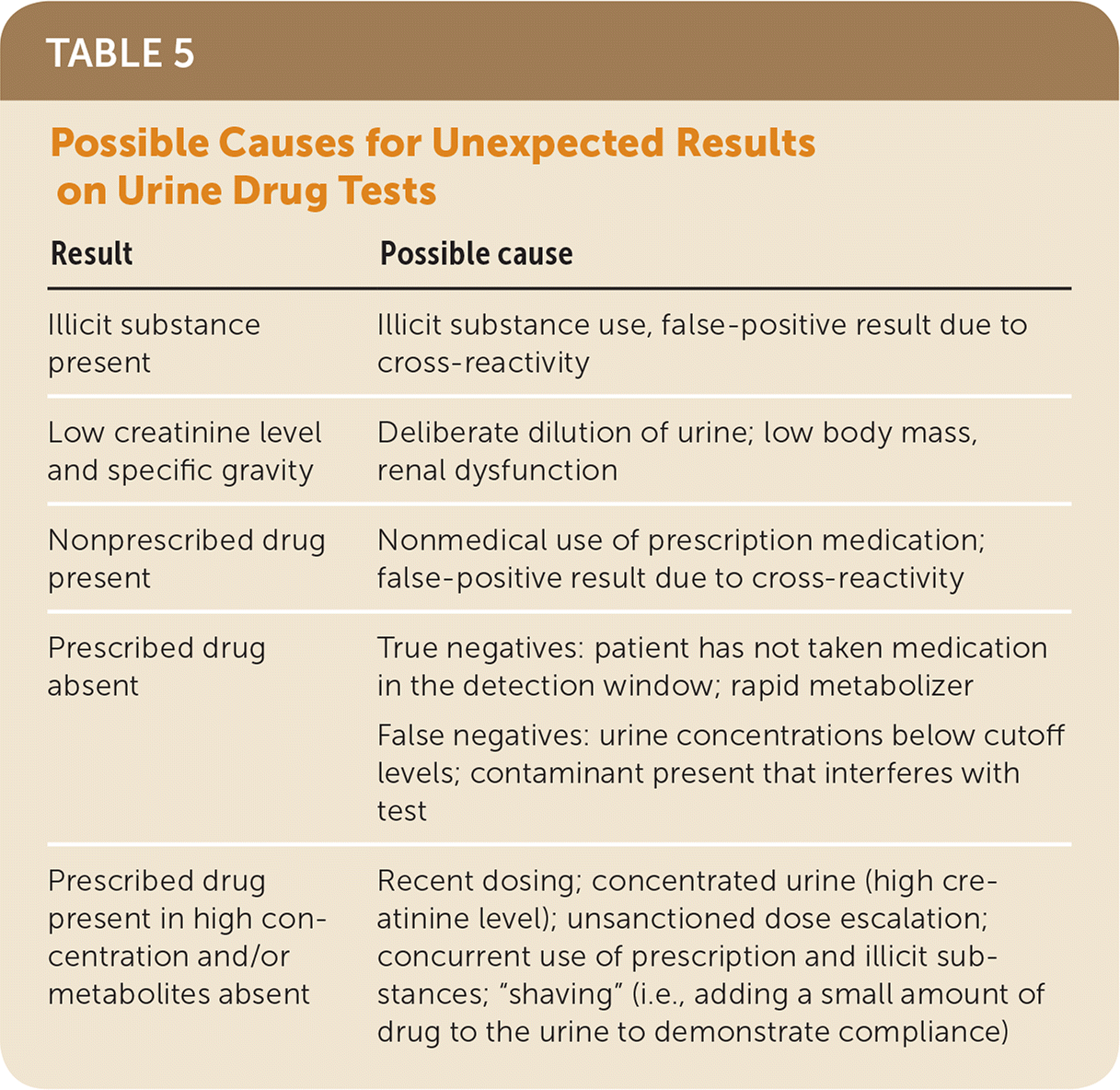
Urine samples are sometimes contaminated deliberately by ingestion or addition of a foreign substance to prevent detection of illicit drugs. Common methods of tampering include dilution with water, addition of extraneous substances, or substitution of samples. Table 4 lists commercially available agents marketed to help disguise the presence of illicit drugs in urine samples.15,21 Many laboratories now routinely check urine creatinine levels to determine whether the sample is excessively dilute and to check for the presence of adulterants. Several commercially available point-of-care systems check for the presence of adulterants in addition to the substances being tested for.21 Although these systems can detect adulterants, they cannot determine which substances are being concealed. The practice known as shaving can also confound drug test results: a patient who is not taking the prescribed drug will add a small amount of the drug directly to the urine specimen to avoid having a negative test result. In these cases, the urine will test positive for the drug—often at a high concentration—but not for its metabolite. Such results should raise suspicion of medication nonadherence. Table 5 lists possible unexpected results from urine drug tests and potential causes.
TABLE 4. Adulterants Used to Prevent Detection of Drugs in Urine Samples
| Adulterant | Composition | Mode of action |
|---|---|---|
| Ammonia | Ammonia | Interferes with detection of benzoylecgonine and phencyclidine |
| Bleach | Sodium hypochlorite | Interferes with immunoassay; may cause degradation of analyte for gas chromatography |
| Goldenseal (Hydrastis canadensis) | Herbal diuretic | Dilution to below cutoff level; decreases immunoassay sensitivity to amphetamines and THC |
| Klear, Whizzies | Potassium nitrite | Interferes with THC immunoassay and gas chromatography/mass spectrometry analysis |
| Powdered urine | Dried human urine residue | Substitution |
| Stealth | Peroxide and peroxidase | Interferes with THC and opioid immunoassays |
| Urinaid, Clean-X | Glutaraldehyde | Decreases immunoassay sensitivity to multiple drugs |
| Urine Luck, Instant Clean Add-it-ive | Pyridinium chlorochromate | Strong oxidizing agent; interferes with immunoassay and gas chromatography/mass spectrometry analysis for multiple drugs |
| Vinegar | Acetic acid | Decreases immunoassay sensitivity to THC |
| Visine eye drops | Benzalkonium chloride | Decreases immunoassay sensitivity to THC |
| Water plus diuretics | — | Dilution to below cutoff level |
THC = tetrahydrocannabinol.
TABLE 5. Possible Causes for Unexpected Results on Urine Drug Tests
| Result | Possible cause |
|---|---|
| Illicit substance present | Illicit substance use, false-positive result due to cross-reactivity |
| Low creatinine level and specific gravity | Deliberate dilution of urine; low body mass, renal dysfunction |
| Nonprescribed drug present | Nonmedical use of prescription medication; false-positive result due to cross-reactivity |
| Prescribed drug absent | True negatives: patient has not taken medication in the detection window; rapid metabolizer False negatives: urine concentrations below cutoff levels; contaminant present that interferes with test |
| Prescribed drug present in high concentration and/or metabolites absent | Recent dosing; concentrated urine (high creatinine level); unsanctioned dose escalation; concurrent use of prescription and illicit substances; “shaving” (i.e., adding a small amount of drug to the urine to demonstrate compliance) |
Unintentional Ingestions and Exposures
Ingestion of poppy seeds is sometimes claimed as a reason for an unexpected positive opioid test result. To study this claim, researchers recruited 15 volunteers to consume a poppy seed roll and raw poppy seeds before undergoing urine and oral fluid drug testing.22 Although the tests did detect morphine and codeine in the samples, the levels were far below the cutoff for commercial testing. Therefore, casual ingestion of a poppy seed–containing food will not cause a positive test result. Similarly, passive inhalation of marijuana smoke has been claimed as a cause for a positive tetrahydrocannabinol (THC) test result. Studies have shown that although casual passive inhalation of marijuana smoke does cause elimination of THC in urine samples, the amount excreted is far below the federal and commercial cutoffs for testing and should not cause a positive test.23 Extreme exposure and high room air concentrations of THC were required to cause positive urine screening results in test participants.
Cost of Urine Drug Testing
As more persons are required to undergo urine drug testing for monitoring long-term opioid therapy, the cost of testing and coverage by third-party payers are considerations that should be taken into account. Some insurers limit the number of tests they will cover in a year, and others do not pay for urine drug testing at all. The out-of-pocket cost for urine drug testing varies greatly depending on geographic region and the laboratory used. A popular health care cost comparison website lists the fair price for a urine drug screen as $128, with a range of $62 to $308.24 Medicare covers testing for patients with an appropriate indication; reimbursement ranges from $13 to $72 for the initial immunoassay, depending on the test used.25
This article updates a previous article on this topic by Standridge, et al.8
Data Sources: PubMed was the primary data source used. Multiple searches were conducted using the terms urine drug tests, urine drug screen, pharmacokinetics, metabolism plus the individual drug names, urine drug screen adulterants, and urine drug screen interpretation. Google Scholar, the Cochrane database, and the websites for the Agency for Healthcare Research and Quality and U.S. Preventive Services Task Force were also searched. Search dates: September 2017, and January and April 2018.

