Expansion in the number of American medical schools since 2005 led to an absolute increase in graduates matching into family medicine (FM) residency programs from 2008 to 2018. Proportionally, however, FM training has become increasingly reliant on osteopathic physicians and U.S. citizens trained at international medical schools (U.S. international medical graduates [IMGs]). The proportion of allopathic students who undertake FM training has stayed relatively constant, whereas the share of foreign citizens trained at international medical schools (non-U.S. IMGs) who enter FM training has diminished.
Despite calls from the Council on Graduate Medical Education to increase the number of medical schools to address the primary care shortage,1 the United States lacks a coordinating function for graduate medical education (GME). Production of primary care physicians is determined by student and hospital interests, and market forces. Our review of data from the National Residency Matching Program (NRMP) tracks GME entry since 2008. Although the total number of U.S. graduates who entered FM through the NRMP rose 64.2% over the past 10 years, the annual proportion from U.S. allopathic schools (that grant MDs) remained around 50%. This is well short of the peak in 1996, when 72.5% of first-year positions were filled by U.S. allopathic graduates.2
Over the past decade, the entry of osteopathic physicians (DOs) into FM through the NRMP match has increased 164%, with a proportional rise from 11% of new residents in 2008 to 19.8% in 2018. Since 2016, there has been a sizeable increase in DO entry into FM because of progression toward a single GME accreditation system.3 This has led to more osteopathic physician positions being represented in the NRMP Match.
Since 2008, U.S. IMGs entering FM rose 85.0%, and proportionally increased from 16.6% of new trainees in 2008 to 20.9% in 2018. In contrast, there was a 33.0% overall decrease in non-U.S. IMGs entering FM, with a decline from 20.7% of residents in 2008 to 9.4% of all those entering training in 2018.
U.S. allopathic and osteopathic medical school expansion over the past 10 years has increased the numbers of graduates pursuing FM training. However, only osteopathic physicians and U.S. IMGs have risen as a proportion of new FM residents. The absence of a proportional rise in the number of U.S.-trained allopathic graduates challenges the assertion that an increase in allopathic graduate production will adequately address primary care shortages.
FIGURE 1
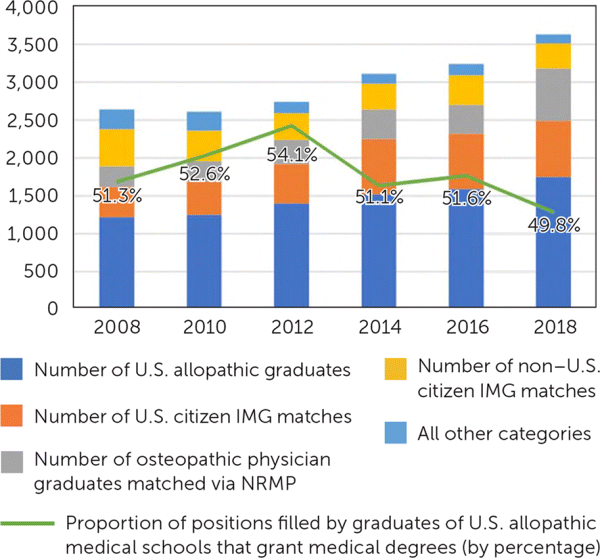
Entry into family medicine by category.
Data from the 2008 to 2018 NRMP. (NRMP = National Residency Matching Program; IMG = international medical graduate.)
The information and opinions in this article do not necessarily reflect the views or policy of the AAFP.

