Clinical Question
Are complementary and integrative treatments such as massage, thermal interventions, and relaxation techniques effective and safe for managing pain during labor?
Evidence-Based Answer
There is evidence that all of the studied interventions have some benefit in labor, but the evidence is of low to very low quality. Massage, thermal interventions (warm and cold packs), relaxation techniques, yoga, and music reduce pain during latent labor, but not during active labor.1,2 Thermal interventions and yoga shorten the duration of labor, with a mean difference (MD) of 66 minutes (95% confidence interval [CI], 40 to 92 minutes) for warm packs, 78 minutes (95% CI, 37 to 119 minutes) for cold or intermittent warm and cold packs, and 140 minutes (95% CI, 27 to 252 minutes) for yoga vs. usual care.1,2 Yoga improves satisfaction with pain relief (MD = –1.3 on a 10-point visual analog scale [VAS]; 95% CI, –0.5 to –1.7), and relaxation techniques increase the likelihood that patients will report high satisfaction with pain control (number needed to treat [NNT] = 3; 95% CI, 1 to 200).2 Massage also improved satisfaction with the labor experience (NNT = 3; 95% CI, 2 to 40).1 (Strength of Recommendation: B, based on inconsistent or limited-quality patient-oriented evidence.)
Practice Pointers
Complementary therapies are popular for pain management in labor. In one study, 70% of patients reported using a nonmedical therapy for labor pain, with 50% of patients using at least two.3 Two recent Cochrane analyses were produced to discern whether these pain management techniques are safe and effective for use in labor.
The first Cochrane review described massage and manual therapies for pain management in labor, evaluating 10 trials involving 1,055 women.1 Trials were performed in various countries, with more than half conducted in Iran. Interventions were compared with usual care in all studies. Low-quality evidence from all 10 trials showed that massage moderately reduced pain during latent labor (NNT = 2; 95% CI, 1 to 3). Massage also mildly improved patients' sense of control in labor and satisfaction with childbirth (NNT = 3; 95% CI, 2 to 40). Very low-quality evidence from a single trial showed that thermal interventions with warm or cold packs reduced pain in latent labor (MD = –1.4 points on a 10-point VAS; 95% CI, –2.2 to –0.6). Thermal intervention also reduced labor duration by 66 minutes (95% CI, 40 to 92 minutes) for warm packs and 78 minutes (95% CI, 37 to 119 minutes) for cold or intermittent warm and cold packs. The primary quality limitation in all studies was due to lack of blinding and small trial sizes, which led to high heterogeneity in results. These therapies did not increase adverse outcomes compared with usual care.
Another recent Cochrane review studied relaxation techniques for pain management in labor, evaluating 15 studies involving 1,731 women.2 Instruction on relaxation mildly reduced latent labor pain (MD = –1.3 on VAS; 95% CI, –1.7 to –0.5) and led to higher satisfaction with pain relief (NNT = 3; 95% CI, 1 to 200). Yoga mildly reduced latent labor pain (MD = –0.6 on VAS; 95% CI, –1.2 to –0.1), and slightly improved satisfaction with pain relief (MD = 0.8 on VAS; 95% CI, 0.2 to 1.4) and childbirth (MD = 6 on maternal comfort scale with a range of 35 to 210; 95% CI, 0.3 to 12). Two small trials demonstrated that yoga also reduced the duration of labor by 140 minutes (95% CI, 27 to 252 minutes) when compared with usual care in one trial and by 191 minutes (95% CI, 139 to 244 minutes) when compared with supine positioning in another trial.
Mindfulness increased patients' sense of control during labor (MD = 31 on the Childbirth Self-Efficacy Inventory with a range of 0 to 150; 95% CI, 2 to 61) based on a small trial with very low-quality evidence. Music slightly reduced latent labor pain compared with usual care based on two trials (MD = –0.7 on 10-point VAS; 95% CI, –1.0 to –0.5) and during transition to active labor based on one trial (MD = –0.7 on 10-point VAS; 95% CI, –0.9 to –0.5). All evidence was low to very low quality, based primarily on lack of blinding and small sample sizes leading to high heterogeneity of results. There was no increase in adverse outcomes in patients treated with relaxation techniques compared with usual care.
Previous Cochrane reviews have reported on the use of hypnosis, acupuncture, and acupressure in labor.4,5 These reviews also showed inconsistent evidence of benefit because of small studies limited by lack of blinding. Hypnosis reduces the use of pain medications in labor but does not affect reported pain or satisfaction.4 Acupuncture reduces pain compared with no intervention, but not compared with usual care.5 Acupressure mildly reduces pain compared with placebo and reduces labor duration.6
Guidelines from the National Institute for Health and Care Excellence recommend supporting a pregnant woman's choice in using relaxation or massage techniques.6 The American College of Obstetricians and Gynecologists recommends consideration of nonpharmacologic techniques to optimize pain control or coping, including massage, relaxation techniques, acupuncture, and hypnosis.7
SUMMARY TABLE: IMPORTANT EFFECTS OF COMPLEMENTARY AND INTEGRATIVE TREATMENTS ON LABOR OUTCOMES
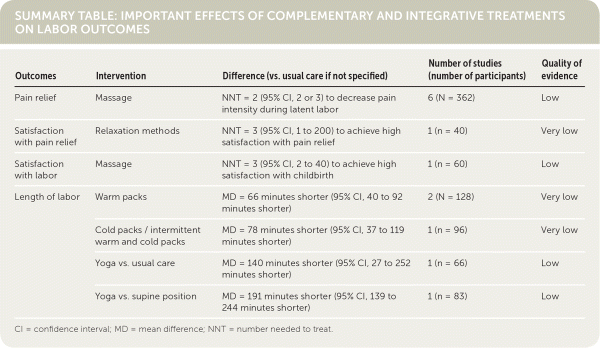
| Outcomes | Intervention | Difference (vs. usual care if not specified) | Number of studies (number of participants) | Quality of evidence |
|---|---|---|---|---|
| Pain relief | Massage | NNT = 2 (95% CI, 2 or 3) to decrease pain intensity during latent labor | 6 (N = 362) | Low |
| Satisfaction with pain relief | Relaxation methods | NNT = 3 (95% CI, 1 to 200) to achieve high satisfaction with pain relief | 1 (n = 40) | Very low |
| Satisfaction with labor | Massage | NNT = 3 (95% CI, 2 to 40) to achieve high satisfaction with childbirth | 1 (n = 60) | Low |
| Length of labor | Warm packs | MD = 66 minutes shorter (95% CI, 40 to 92 minutes shorter) | 2 (N = 128) | Very low |
| Cold packs / intermittent warm and cold packs | MD = 78 minutes shorter (95% CI, 37 to 119 minutes shorter) | 1 (n = 96) | Very low | |
| Yoga vs. usual care | MD = 140 minutes shorter (95% CI, 27 to 252 minutes shorter) | 1 (n = 66) | Low | |
| Yoga vs. supine position | MD = 191 minutes shorter (95% CI, 139 to 244 minutes shorter) | 1 (n = 83) | Low |
CI = confidence interval; MD = mean difference; NNT = number needed to treat.
The practice recommendations in this activity are available at http://www.cochrane.org/CD009290 and at http://www.cochrane.org/CD009514.
Editor's Note: The numbers needed to treat reported in this Cochrane for Clinicians were calculated by the authors based on raw data provided in the original Cochrane review.
The views expressed in this article are those of the authors and do not necessarily reflect the official policy or position of the Department of the Navy, the Uniformed Services University of the Health Sciences, the Department of Defense, or the U.S. government.

