
Am Fam Physician. 2019;99(7):422-423
Author disclosure: No relevant financial affiliations.
Clinical Question
Are direct oral anticoagulants safe and effective for preventing stroke and embolism in patients with atrial fibrillation and chronic kidney disease (CKD)?
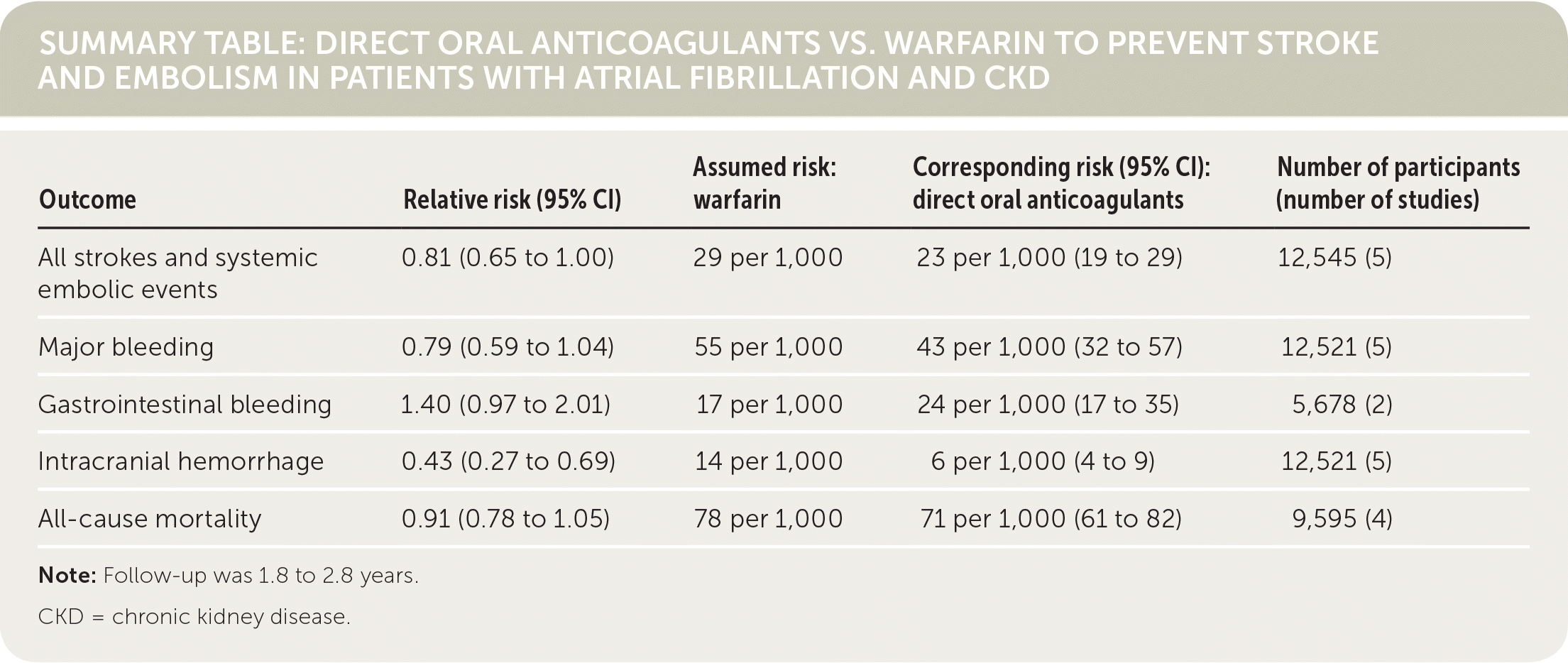
| Outcome | Relative risk (95% CI) | Assumed risk: warfarin | Corresponding risk (95% CI): direct oral anticoagulants | Number of participants (number of studies) |
|---|---|---|---|---|
| All strokes and systemic embolic events | 0.81 (0.65 to 1.00) | 29 per 1,000 | 23 per 1,000 (19 to 29) | 12,545 (5) |
| Major bleeding | 0.79 (0.59 to 1.04) | 55 per 1,000 | 43 per 1,000 (32 to 57) | 12,521 (5) |
| Gastrointestinal bleeding | 1.40 (0.97 to 2.01) | 17 per 1,000 | 24 per 1,000 (17 to 35) | 5,678 (2) |
| Intracranial hemorrhage | 0.43 (0.27 to 0.69) | 14 per 1,000 | 6 per 1,000 (4 to 9) | 12,521 (5) |
| All-cause mortality | 0.91 (0.78 to 1.05) | 78 per 1,000 | 71 per 1,000 (61 to 82) | 9,595 (4) |
Evidence-Based Answer
Direct oral anticoagulants are as likely as warfarin to prevent all strokes and systemic embolic events in patients with atrial fibrillation and CKD stage 3. They do not increase the risk of major bleeding events. The evidence remains insufficient to make recommendations for the use of direct oral anticoagulants in the management of patients with atrial fibrillation and CKD stage 4 or 5.1 (Strength of Recommendation: A, based on consistent, good-quality patient-oriented evidence.)
Practice Pointers
Atrial fibrillation and CKD are independent risk factors for stroke and embolic events.2 Current evidence suggests an improved health-related quality of life with the use of direct oral anticoagulants vs. traditional treatment with vitamin K antagonists (e.g., warfarin) for patients with an increased risk of stroke.3 The authors of this Cochrane review sought to determine the safety and effectiveness of stroke and embolism prevention with direct oral anticoagulants vs. warfarin in the management of chronic, nonvalvular atrial fibrillation in patients with CKD stage 3 and 4.1
This Cochrane review included five trials involving 12,545 patients. The follow-up time ranged from 1.8 to 2.8 years. Identified studies compared direct oral anticoagulants and warfarin to prevent stroke (including ischemic, hemorrhagic, or unspecified) and embolism in patients with nonvalvular atrial fibrillation and moderate CKD (i.e., stage 3 and 4), defined as a creatinine clearance between 15 and 60 mL per minute per 1.73 m2.
Patients who used direct oral anticoagulants seemed to have a decreased risk of stroke and embolic events vs. patients receiving warfarin, but these results did not reach statistical significance and thus these agents should be considered equivalent.
Various secondary outcomes were also evaluated. Patients using direct oral anticoagulants were at less risk of developing intracranial hemorrhage vs. those using warfarin (relative risk [RR] = 0.43; 95% CI, 0.27 to 0.69; number needed to treat = 125; 95% CI, 100 to 200). This review demonstrated a slight, although not statistically significant, increase in gastrointestinal bleeding with direct oral anticoagulant use vs. warfarin. Patients using direct oral anticoagulants seemed to have a slightly lower risk of major bleeding and all-cause mortality than those using warfarin, but again those results were not statistically significant, so these agents should be considered equivalent in this regard.
Subgroup analysis showed that patients with CKD stage 3 experienced the most benefit from direct oral anticoagulants in terms of risk reduction for stroke, whereas the risk reduction was less conclusive in the CKD stage 4 group (RR = 0.68; 95% CI, 0.23 to 2.0), despite U.S. Food and Drug Administration approval of its safety in this population. Further analysis evaluated dosages and various subtypes of direct oral anticoagulants; however, the available data were lacking to make meaningful conclusions.
Evidence supports the use of anticoagulation to treat concomitant nonvalvular atrial fibrillation and moderate CKD to lower the risk of stroke and embolic events.4 This Cochrane review provides support for the safety and effectiveness of direct oral anticoagulants in lowering the risk of stroke and embolic events in patients with atrial fibrillation and CKD.
The practice recommendations in this activity are available at http://www.cochrane.org/CD011373.
Editor's Note: The number needed to treat reported in this Cochrane for Clinicians was calculated by the authors based on comparison of assumed risk and corresponding risk.
The opinions and information provided in this article reflect the authors as individuals alone and do not reflect or represent any official opinions or statements of any component of the Department of Defense, U.S. Air Force, U.S. Army, or the Uniformed Services University of the Health Sciences.
