A 60-year-old woman presented with cough and hemoptysis. She reported anorexia and a 30-lb weight loss that occurred over several months. She had no significant medical history. Although she smoked more than one pack of cigarettes per day for many years, she had recently decreased her smoking to six or seven cigarettes per day. Subcutaneous nodules had developed on her chest wall and left and right abdominal wall over several months. These nodules were increasing in size and tender to palpation.
On physical examination, the most prominent nodule measured approximately 4.5 × 4 cm (Figure 1). It was located on the left upper abdominal wall and appeared fixed to the underlying muscle. Computed tomography of the chest showed mediastinal and hilar lymphadenopathy with a soft tissue mass in the hilar and perihilar region with collapse of the right middle lobe.
FIGURE 1
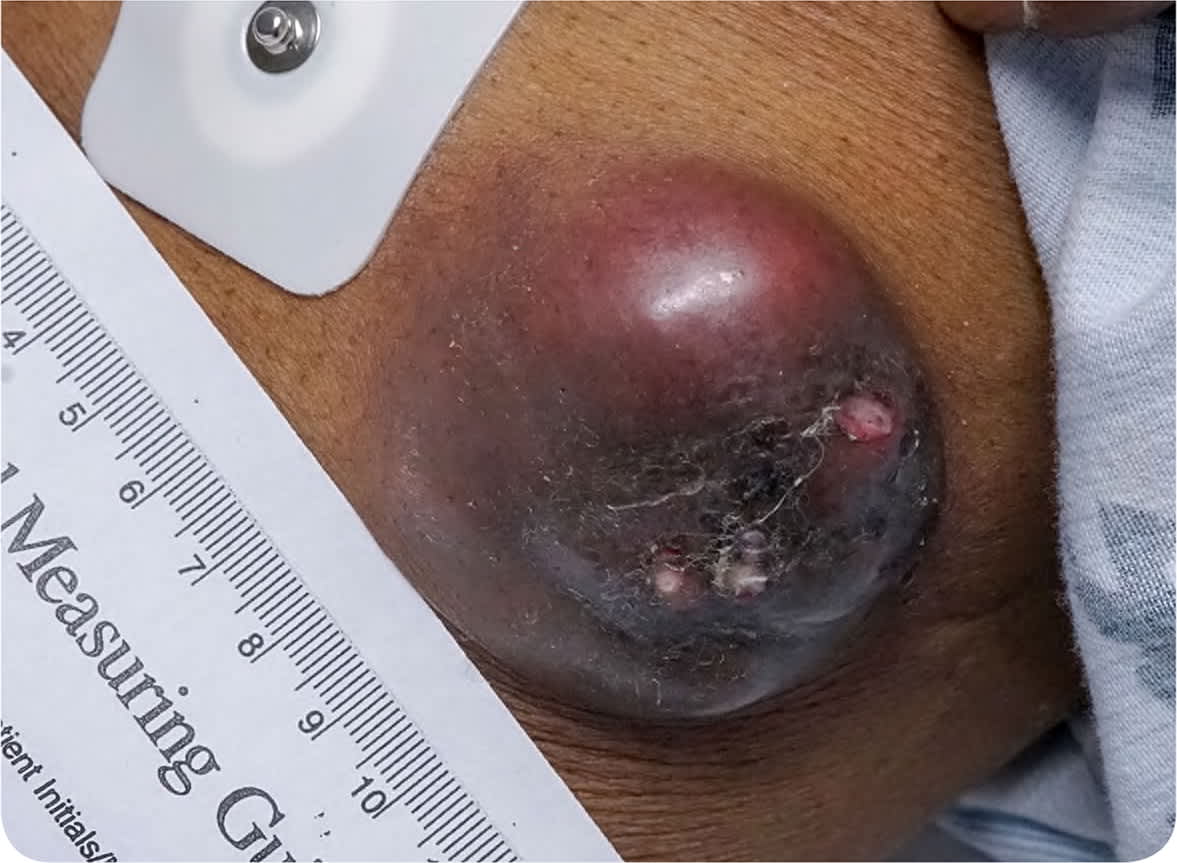
Question
Based on the patient's history, physical examination, and imaging findings, which one of the following is the most likely diagnosis?
A. Cutaneous metastasis.
B. Dermatofibroma.
C. Keratoacanthoma.
D. Lipoma.
E. Neurofibromatosis.
Discussion
Answer is A: cutaneous metastasis of adenocarcinoma of the lung. Lung cancer is a common malignancy with a high mortality rate. Lung cancer can metastasize to virtually any organ, most commonly the hilar lymph nodes, brain, liver, adrenal glands, and skeleton.1,2 Metastasis of internal cancers to the skin is uncommon, occuring in 1% to 12% of individuals with lung cancer.2,3 However, skin lesions may be the initial sign of disease in 7% to 24% of those with lung cancer.3,4 The most common sites for cutaneous metastasis of lung cancer are the anterior chest and abdominal wall, although metastasis to the head and neck has also been reported.2–5
Cutaneous metastasis of lung cancer presents as firm, round or oval nodules that are fixed or mobile. They may be skin-colored, pink, red, purple, or bluish-black.4,6 The nodules are typically painless but may be painful and ulcerate.
Fine-needle aspiration with differential immunohistochemical staining techniques is a relatively fast, noninvasive, inexpensive, and simple method for early diagnosis of subcutaneous nodules.7 The diagnosis of cancer is typically based on clinical information and histology; however, immunohistochemistry may also be helpful in establishing the diagnosis using special stains, such as antithyroid transcription factor and cytokeratins 7 and 20.2
Cutaneous metastasis of lung cancer usually presents in late stages of the disease; therefore, the prognosis is poor, with a survival rate of about five to seven months.2,3,8 Chemotherapy and radiation therapy are usually effective only as palliative therapy in such cases.3 When there are multiple cutaneous metastases, chemotherapy is the preferred treatment option.2,3 Chemotherapy may be less helpful for cutaneous metastases than for the primary tumor because the blood supply to the skin is relatively poor.5 Palliative radiation therapy may be beneficial for bleeding or painful skin lesions.2,3 Surgical excision is indicated if it can improve the patient's quality of life (e.g., the cutaneous metastases cause cosmetic or functional problems or significant pain).9
Dermatofibromas are common, benign tumors that most often develop in young adults. They commonly occur on the limbs. They may be solitary or multiple. The color is variable, but they are often brown and less commonly pink, red, or skin-colored. The edges of the lesions are poorly defined.10
Keratoacanthomas are rapidly growing, dome-shaped, symmetrical lesions. They can be large, reaching several centimeters in size within days or weeks. The lesions are surrounded by a smooth wall of inflammation and are capped with keratin and debris. They usually occur on sun-exposed skin10
Lipomas are common, benign tumors that can appear on any body surface. They are typically soft and rubbery to palpation and are skin-colored. They are usually slow-growing and painless. Lipomas can undergo malignant transformation into a sarcoma, although this is uncommon.10
Neurofibromas are well-circumscribed nodules that are typically softer than the surrounding connective tissue and often create a “buttonhole” invagination when a finger is rubbed lightly over the surface. Neurofibromas are slow-growing tumors that arise from the peripheral nerve sheath. They are associated with café au lait spots.10
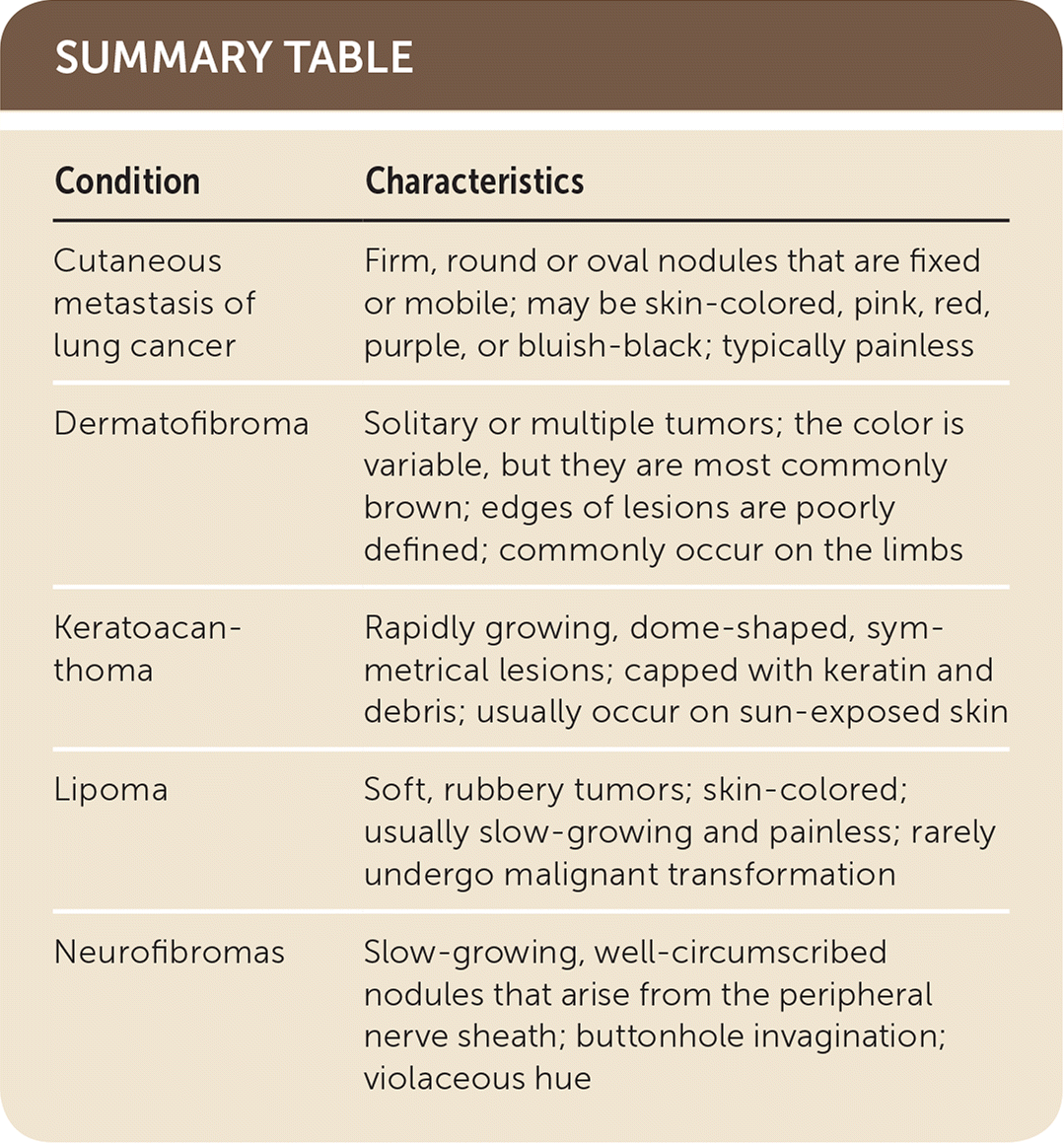
SUMMARY TABLE
| Condition | Characteristics |
|---|---|
| Cutaneous metastasis of lung cancer | Firm, round or oval nodules that are fixed or mobile; may be skin-colored, pink, red, purple, or bluish-black; typically painless |
| Dermatofibroma | Solitary or multiple tumors; the color is variable, but they are most commonly brown; edges of lesions are poorly defined; commonly occur on the limbs |
| Keratoacanthoma | Rapidly growing, dome-shaped, symmetrical lesions; capped with keratin and debris; usually occur on sun-exposed skin |
| Lipoma | Soft, rubbery tumors; skin-colored; usually slow-growing and painless; rarely undergo malignant transformation |
| Neurofibromas | Slow-growing, well-circumscribed nodules that arise from the peripheral nerve sheath; buttonhole invagination; violaceous hue |

