Case Scenario
An 87-year-old patient was brought to my office by her daughter. She has been my patient for 22 years and was diagnosed with Alzheimer disease (AD) eight years ago. Most recent evaluation indicates that she is in stage 6 of the disease; she requires assistance with activities of daily living, has increasing periods of disorientation and aggressiveness, and needs reminding of her name and those of her children. She is currently receiving treatment for advanced heart disease, chronic obstructive pulmonary disease, and multiple myeloma. Her daughter asks about her mother's prognosis and the appropriateness of palliative care. How should determining prognosis and applicability of palliative care for her mother be done? What might be the core management challenges in providing care for her?
Commentary
Dementia is a family of conditions that is the sixth leading cause of death in the United States.1 The term covers several conditions including AD, vascular dementia, and dementia with Lewy bodies. AD is the most prevalent of these conditions and is rapidly increasing in the United States and worldwide. In 2017, more than 5 million Americans were living with AD. By 2025, the number is expected to grow by almost 35% to 7.1 million, with some projections of 16 million by 2050.1 Patients may have symptoms of AD for up to 20 years, although the mean is four to eight years.2
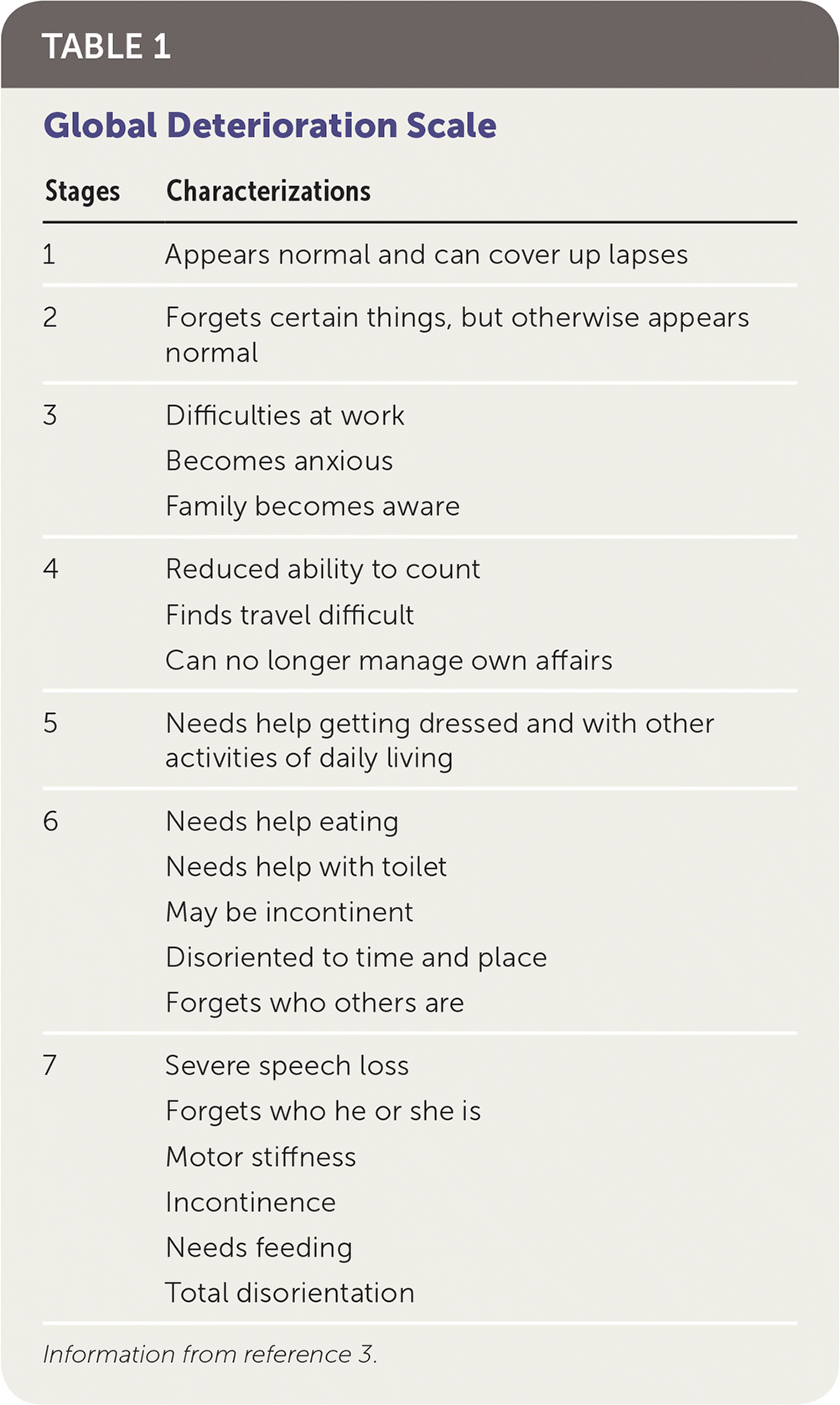
Determining the prognosis for a patient with dementia begins with establishing the current stage of the disease. AD and other dementias are progressive, with seven recognized stages.3 The Global Deterioration Scale is a validated instrument used for determining where the patient is along the progression timeline, and it mirrors the dementia stages (Table 1).3 Stage 1 usually begins when patients are in their 50s or 60s and is commonly not apparent, even to the patient. This stage is characterized by occasional lapses of memory. These lapses become more frequent and perhaps bothersome to the patient in stage 2, although the patient may appear to function normally. The lapses become problematic and may cause the patient increasing anxiety in stage 3. At this stage, family members and others start to notice the symptoms and effects of dementia. Memory and functional impairment proceed inexorably through the subsequent stages. By stage 7, the patient has incontinence, severe functional loss requiring assistance for activities of daily living, limited speech, and total disorientation. Median survival in stage 7 is 1.3 years. Most patients with advanced dementia spend a disproportionate amount of time (40%) in the most severe (stage 7) stage, often requiring placement in a skilled nursing facility, where two-thirds of these patients die. More than 80% of patients in stage 7 have notable difficulty eating, often requiring assistance; weight loss is common. Infections, primarily pneumonia and urinary tract infections, are common and carry a 40% or higher risk of mortality.4
TABLE 1 Global Deterioration Scale
| Stages | Characterizations |
|---|---|
| 1 | Appears normal and can cover up lapses |
| 2 | Forgets certain things, but otherwise appears normal |
| 3 | Difficulties at work |
| Becomes anxious | |
| Family becomes aware | |
| 4 | Reduced ability to count |
| Finds travel difficult | |
| Can no longer manage own affairs | |
| 5 | Needs help getting dressed and with other activities of daily living |
| 6 | Needs help eating |
| Needs help with toilet | |
| May be incontinent | |
| Disoriented to time and place | |
| Forgets who others are | |
| 7 | Severe speech loss |
| Forgets who he or she is | |
| Motor stiffness | |
| Incontinence | |
| Needs feeding | |
| Total disorientation |
Information from reference 3.
Estimating the prognosis in advanced dementia is problematic because of patients' fluctuating physical and mental status and the complex interaction of health, sociodemographic factors, and cognitive function. Two tools are available to help understand a patient's progression through AD dementia. The Advanced Dementia Prognostic Tool (ADEPT) predicts survival based on 11 variables in demographics, cognitive status, functional status, and active diagnoses.5,6 A risk score greater than 16 (on a scale of 1 to 32) suggests a six-month probability of dying at greater than 50%. Alternatively, Medicare hospice guideline criteria can be used to assess prognosis. If a patient meets Medicare hospice criteria, it is anticipated that the patient is likely to die within six months. These criteria require patients to meet the following conditions for hospice care: having significant functional limitation (stage 7 or beyond on the Functional Assessment Staging [FAST] scale,7 which is a variant of the Geriatric Depression Scale used by Medicare) and having at least one of six specific medical complications in the preceding year, including aspiration pneumonia, pyelonephritis, septicemia, multiple decubitus ulcers, recurrent fevers after antibiotic use, or inadequate hydration and caloric intake with at least 10% body weight loss during the previous six months (or a serum albumin level less than 2.5 g per dL [25 g per L]). Medicare publishes updated local coverage determinations that provide state-specific criteria for hospice eligibility (https://go.cms.gov/2Dxwz3q). When compared with ADEPT, the Medicare hospice guidelines are less reliable in predicting six-month mortality.6
Palliative care is appropriate at any point after dementia diagnosis and may be provided as early as stage 2.8,9 Palliative services include symptom management, prognosis and goals of care discussion, determination of code status, and psychosocial management.9,10 As the patient progresses along the dementia spectrum, palliative care challenges include pain management and advance care planning and communication.
Central to primary palliative care is understanding and aligning care to meet the needs and wishes of the patient (see Table 2 for resources). In the early stages of dementia, cognitive functioning may remain reasonably intact while memory is declining. In these stages, advance care discussions are appropriate with the patient and the patient's family. As the disease progresses and cognitive function declines, decision-making may be more difficult and may require assessing the capacity of the patient to comprehend and determine specific goals of care.11–13 Regardless of where the patient is on the dementia spectrum, if reasonable capacity of determining personal goals of care exists, the patient should have the opportunity in collaboration with family and loved ones to make decisions about his or her care. Several tools are available to assist in this process, and guidance can be found in the Institute for Healthcare Improvement Conversation Starter Kit.14 In 2017, the University of Washington released a dementia-specific advance directive.15 Conversations with the patient and designated surrogates should clearly define goals of care, desire for different forms of resuscitation, and identity of surrogate decision makers.
TABLE 2 Dementia Management Resources
| Alzheimer's Association |
| California Academy of Family Physicians: A Step-by-Step Guide for Family Physicians |
| National Hospice and Palliative Care Organization |
| National Institute on Aging |
Pain is the most common symptom among patients in palliative care, regardless of etiology, occurring in as many as 50% of patients.13 This pain may be neuropathic, nociceptive, or both.13 As a patient's dementia advances, and certainly in stage 7, detection and categorization of pain severity will become increasingly difficult. A number of tools can assist in detecting pain through evaluation of nonverbal cues.16 The Pain Assessment in Advanced Dementia scale (using a scale of 1 to 10) uses five observable indicators, including breathing, vocalization, expression, body language, and consolability.17,18 Agitation and dyspnea may be key presenting symptoms of pain in patients with advancing dementia, but they may be confused with progression of the dementia. Recognition of pain should lead to treatment that is targeted to the type and severity of pain.19
Recommendations
As a patient's dementia progresses through the seven stages, consider the following guidelines:
- Educate the caregiver on the nature of dementia as a progressive and ultimately fatal disease.
- Initiate advance care planning conversations early, and revisit them periodically.
- Ensure that the patient has an advance directive with an identified surrogate decision maker.
- Offer palliative care in addition to other medical care early or at least by stage 5 or 6.
- Manage all symptoms (neuropsychiatric, pain, incontinence, insomnia) appropriately.
- Recommend caregiver assistance and support early to avoid caregiver burnout and depression.
- Consider hospice evaluation at stage 7.
Regarding the patient and daughter in the case scenario, it is important to acknowledge that palliative care is appropriate for the mother at any point and certainly in her current state of illness. Assure the daughter that palliative care is supportive of other care and that her mother's other medical conditions will continue to be fully treated. Use of the FAST tool indicates that the patient is not hospice eligible at this point because she has a prognosis of more than six months to several years of life remaining. Explain that dementia is a leading cause of death in the United States; therefore, it is important to plan for end-of-life care. This includes advance care planning and designation of preference for life-sustaining treatment. Stress the importance of having a designated surrogate decision maker for end-of-life decisions. The patient is losing the ability of speech, but tools are available to help with advance care planning as well as to manage symptoms such as pain. Acknowledge that caregiving can be burdensome, and provide the daughter with resources that are available in the community for caregiver assistance.

