Adolescent use of illicit substances imposes an enormous burden on individuals, families, and communities. The types of illicit substances adolescents are using have changed drastically over the past decade with decreases in alcohol use (including binge alcohol use) offset by increases in electronic cigarette, marijuana, and opioid use. Primary care physicians have the opportunity to identify adolescents who use illicit substances. The U.S. Preventive Services Task Force and the American Academy of Family Physicians found insufficient evidence to assess the balance of benefits and harms of primary care–based behavioral interventions to prevent or reduce illicit substance use or nonmedical pharmaceutical use in children or adolescents. The American Academy of Pediatrics recommends that clinicians become familiar with Screening, Brief Intervention, and Referral to Treatment initiatives. Validated screening tools that may be used in primary care include the CRAFFT, POSIT, AUDIT, and NIAAA Screening Guide. During the clinical visit, a split-visit model encourages parents to participate in the visit for a limited time but also allows adolescents to have confidential conversations with physicians. Evidence-based treatment modalities range from school- and parent-based interventions to medication-assisted treatment. Brief interventions using components of motivational interviewing may be suitable for addressing substance use, even among adolescents not seeking treatment. Prevention efforts can supplement cessation programs to maximize program effectiveness.
Adolescent use of illicit substances imposes an enormous burden on individuals, families, and communities. Substance use has correlations with violence, including adolescent homicides1 and relationship victimization.2 Adolescence (typically encompassing youth 10 to 19 years of age)3 is a time of development, including ongoing maturing of the brain; therefore, it is essential to consider the pathophysiology of substance use.4,5 Adolescent brains are more vulnerable to the temptation to use substances and to the effects of these substances because reward pathways develop before prefrontal cognition.5 Sustained substance use can affect neuropsychological functioning, resulting in attention deficits, memory problems, and decreased cognitive flexibility.5
WHAT IS NEW ON THIS TOPIC
Adolescent Substance Use and Misuse
In 2017, e-cigarettes were the most commonly used nicotine-delivery product among high school students.
Approximately 27% of adolescents 13 to 18 years of age who drink alcohol mix it with energy drinks. These adolescents are at increased risk for using tobacco and marijuana and for nonmedical use of prescription stimulants.
Seventeen percent of adolescents have taken prescription drugs without a doctor's prescription.
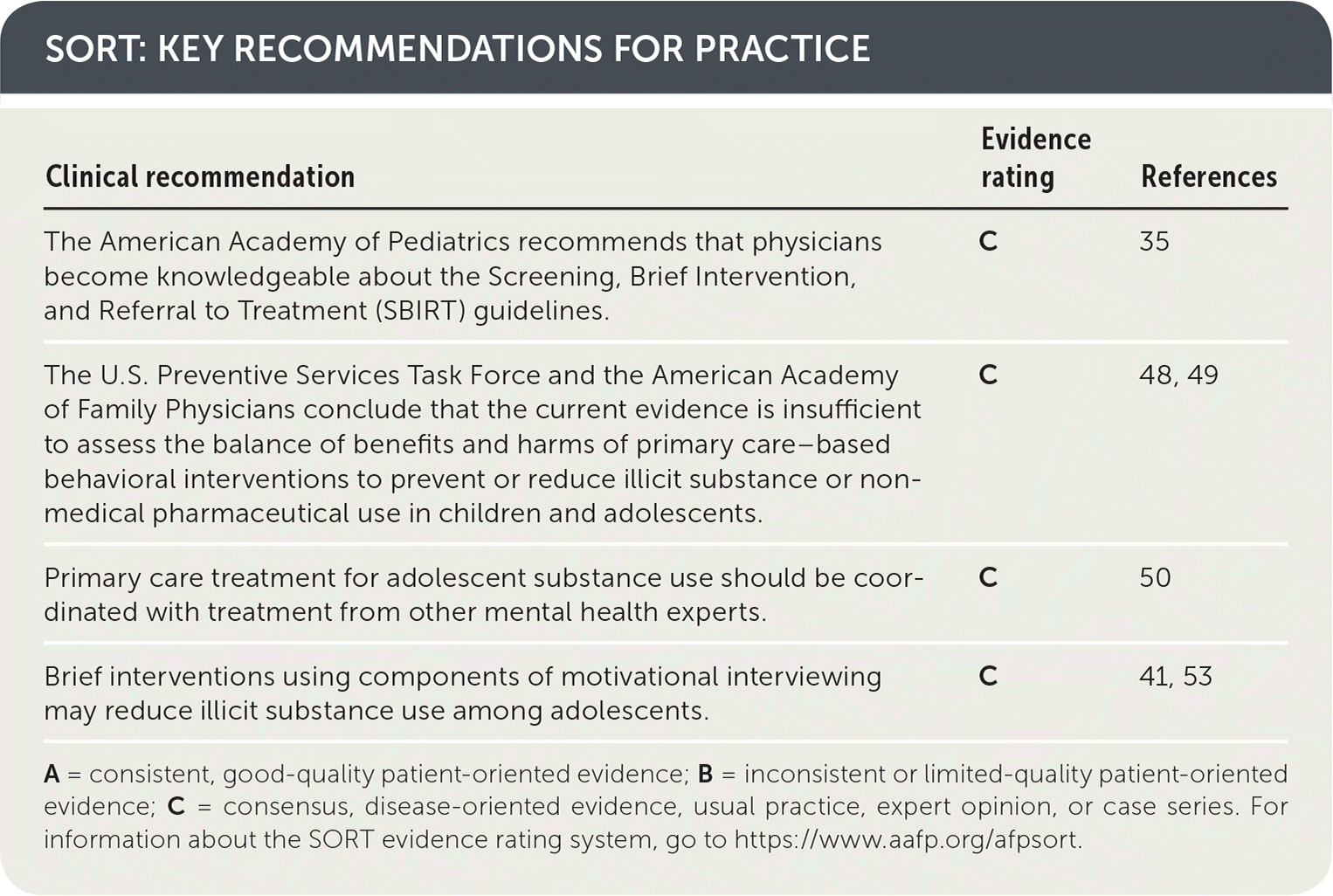
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| The American Academy of Pediatrics recommends that physicians become knowledgeable about the Screening, Brief Intervention, and Referral to Treatment (SBIRT) guidelines. | C | 35 |
| The U.S. Preventive Services Task Force and the American Academy of Family Physicians conclude that the current evidence is insufficient to assess the balance of benefits and harms of primary care–based behavioral interventions to prevent or reduce illicit substance or nonmedical pharmaceutical use in children and adolescents. | C | 48, 49 |
| Primary care treatment for adolescent substance use should be coordinated with treatment from other mental health experts. | C | 50 |
| Brief interventions using components of motivational interviewing may reduce illicit substance use among adolescents. | C | 41, 53 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Scope and Prevalence
Adolescents who participated in the Youth Risk Behavior Survey (a survey of students in grades 9 to 12) in 2015 indicated that 32.8% of them have used alcohol and that 10.8% of them have smoked cigarettes in the past 30 days.6 Nearly 10% of high school students have used two or more tobacco products in the past 30 days,7 and dual users (i.e., users of two or more tobacco products) are at greater risk of engaging in other risky behaviors (e.g., other substance use) compared with nontobacco users and single-product users.8
One in five U.S. adolescents had used marijuana in 2015,6 and Monitoring the Future (a survey of 8th, 10th, and 12th graders) results indicated a significant increase in adolescent marijuana use in 2017 because of adolescents' lowered risk perceptions.9 Alcohol is the substance most consumed by adolescents; however, the Youth Risk Behavior and Monitoring the Future surveys show decreases in 30-day, annual, and lifetime use in 2015, including significant declines in current and binge drinking.10 Approximately 27% of alcohol-using adolescents 13 to 18 years of age mix alcohol with energy drinks, which is a risk factor for tobacco, marijuana, and nonmedical use of prescription stimulants.11
In 2015, adolescent use of illicit substances was reported to be 2.1% for heroin, 5.2% for cocaine, 6.4% for hallucinogens, and 9.2% for synthetic marijuana.6 National estimates indicate that approximately 5% of adolescents had used ecstasy/methylenedioxymethamphetamine (MDMA).6 Other research, however, indicates that the estimate could be as high as 8% because many adolescents do not realize that the substance they know as Molly is a form of ecstasy.12 Approximately 16.8% of adolescents have taken prescription drugs without a physician's prescription (nonmedical use of prescription drugs).6 In some high school seniors, the nonmedical use of prescription stimulants is associated with substance use disorders (SUDs) in adulthood,13 and lifetime nonmedical use of prescription opioids is a risk factor for lifetime heroin use among adolescents.14
The opioid epidemic does not spare the younger population. From 1997 to 2012, hospitalizations for prescription opioid poisoning in children and adolescents increased 165% (1.40 to 3.71 per 100,000); for adolescents older than 15 years, hospitalizations for heroin and methadone poisoning increased 161% (0.96 to 2.51 per 100,000) and 950% (0.10 to 1.05 per 100,000), respectively.15 Nonmedical consumption of codeine cough syrup is sometimes an introduction to opioid misuse among youth.16 The cough syrup is typically mixed with soda or occasionally alcohol and is colloquially known as lean, sizzurp, or purple drank.17 Previous research showed that misuse of codeine cough syrup was primarily by black youth. Other research, however, indicates that the use of lean is also high among Hispanic and Native American youth; males; homosexual, bisexual, and transgender individuals; and youth from urban areas.17
The types of products and the ways in which they are used have changed drastically over the past decade. Traditional cigarette use is low and declining, but high school students' use of any tobacco product within 30 days (19.6%) has not changed significantly from 2011 to 2017,18 primarily because of the increase in hookah and electronic cigarette (e-cigarette) use. The use of cigarillos (smaller, unfiltered cigars) is also prevalent. Cigarillo users often empty the tobacco and replace the contents with marijuana, creating a blunt.19
In 2017, e-cigarettes were the most commonly used nicotine-delivering product among high school students.18 E-cigarette usage, or vaping, has also become a method for administering marijuana; in national and community samples of high school students, rates of vaporizing marijuana by using e-cigarettes were high (10%9 to 29.2%20). In 2018, 21% of U.S. 12th graders reported vaping nicotine in the past 30 days.21 A JUUL is a popular vaping tool that delivers high concentrations of nicotine and has a sleek appearance similar to a computer flash drive.22 JUUL products are promoted on social media platforms whose primary audiences are youth or young adults. JUUL Labs, Inc., and retailers selling the JUUL product have received warning letters from the U.S. Food and Drug Administration22 and have been subjected to fines for illegally selling these products to minors.23
Physicians are valued as a trustworthy source of information, so they may be asked to provide information about vaping and e-cigarettes to patients and their families.24 The role of e-cigarettes as a form of nicotine delivery continues to be debated, but physicians can provide accurate information on meaningful differences in product risks.25
Sociodemographic Differences
Between 2002 and 2014, male and female adolescents 12 to 17 years of age had similar 12-month prevalence rates of SUDs and decreasing trends in use of illicit substances. Male adolescents are typically more likely to use most illicit substances; female adolescents are more likely to use nonmedical amphetamines and tranquilizers.10 Risk factors for illicit substance use include dropping out of high school and ease of access to substances.26 Rural adolescents reported easier access to tobacco products and steroids; urban adolescents reported greater access to alcohol, marijuana, cocaine, methamphetamines, inhalants, ecstasy, hallucinogens, and prescription drugs.27 Neighborhood economic disadvantage, social disorder, and high unemployment rates may play a larger role than individual-level factors in the variance of alcohol and illicit substance use among black adolescents compared with white adolescents.28
Screening and Diagnosis
Mild, moderate, or severe SUD is identified in persons who meet criteria in the Diagnostic and Statistical Manual of Mental Disorders, 5th ed., indicating significant clinical and/or functional impairment (Table 1).29 Because 81% of patients seeking SUD treatment had been seen by a primary care physician during the previous year, primary care physicians have the opportunity to identify adolescents who use substances.30 However, few primary care physicians screen adolescents according to guidelines,30 likely because of low reported levels of preparedness,31 knowledge,30 and low perceived confidence32 to identify and treat substance use.
TABLE 1 Diagnostic Criteria for Substance Use Disorder

A. A problematic pattern of use of an intoxicating substance not able to be classified within the alcohol; caffeine; cannabis; hallucinogen (phencyclidine and others); inhalant; opioid; sedative, hypnotic, or anxiolytic; stimulant; or tobacco categories and leading to clinically significant impairment or distress, as manifested by at least two of the following, occurring within a 12-month period:
|
| Specify if: |
| In early remission: After full criteria for other (or unknown) substance use disorder were previously met, none of the criteria for other (or unknown) substance use disorder have been met for at least 3 months but for less than 12 months (with the exception that Criterion A4, “Craving, or a strong desire or urge to use the substance,” may be met). |
| In sustained remission: After full criteria for other (or unknown) substance use disorder were previously met, none of the criteria for other (or unknown) substance use disorder have been met at any time during a period of 12 months or longer (with the exception that Criterion A4, “Craving, or a strong desire or urge to use the substance,” may be met). |
| Specify if: |
| In a controlled environment: This additional specifier is used if the individual is in an environment where access to the substance is restricted. |
Reprinted with permission from American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 5th ed. Washington, DC: American Psychiatric Association; 2013:577–578.
To assist physicians in managing substance use in adolescents, the Substance Abuse and Mental Health Services Administration (SAMHSA) launched the Screening, Brief Intervention, and Referral to Treatment (SBIRT) initiative.33 Screening flowcharts based on the SBIRT model are available (http://pediatrics.aappublications.org/content/128/5/e1330 and http://pediatrics.aappublications.org/content/138/1/e20161211). The American Academy of Pediatrics (AAP) recommends that physicians become familiar with adolescent SBIRT practices.34,35
SCREENING TOOLS
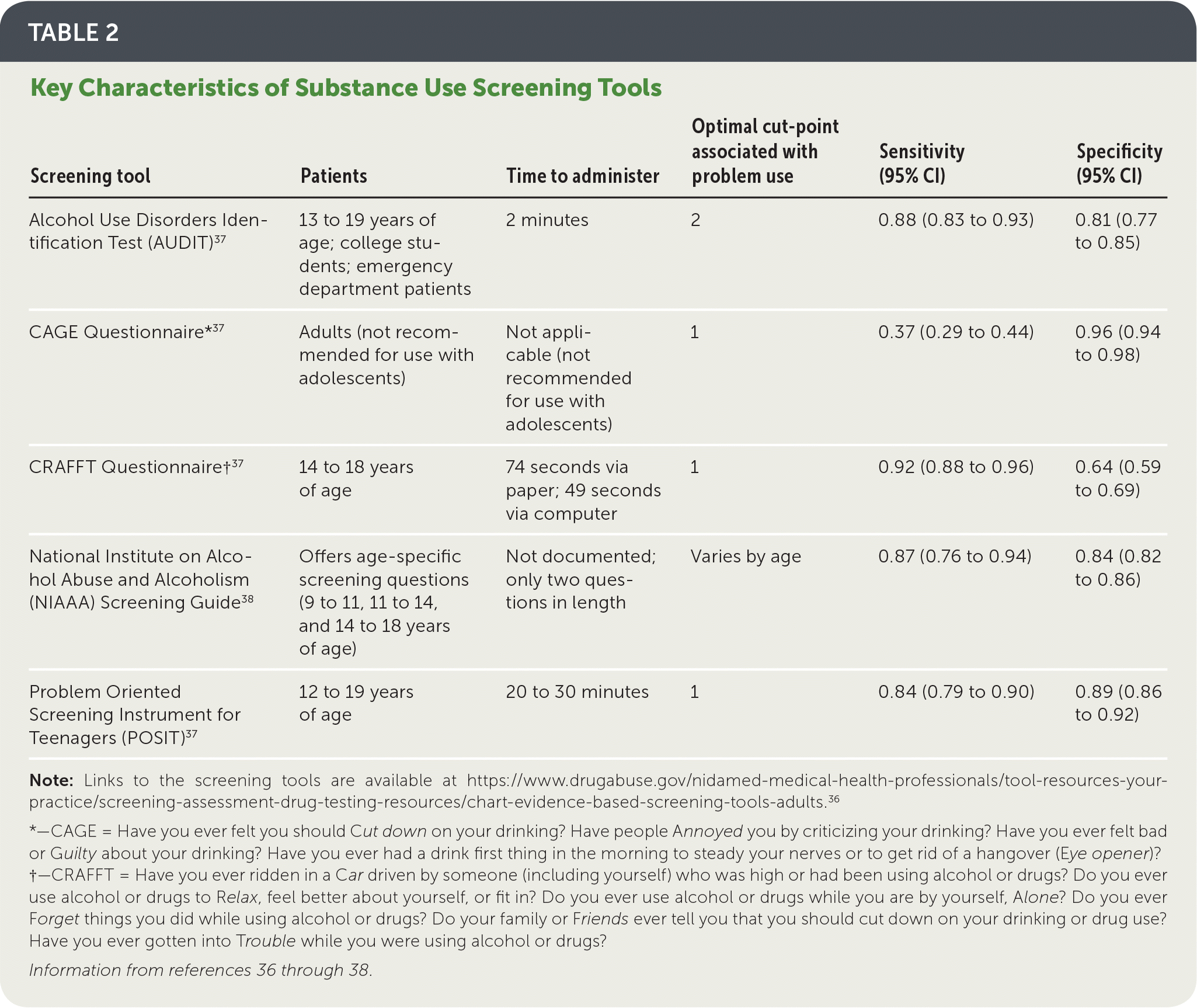
Several validated screening tools that may be used in primary care,29,36 including the CRAFFT questionnaire, Problem Oriented Screening Instrument for Teenagers (POSIT), Alcohol Use Disorders Identification Test (AUDIT), and the National Institute on Alcohol Abuse and Alcoholism Screening Guide, are reviewed in Table 236–38; the CAGE questionnaire is not recommended for use with adolescents because of its low sensitivity. Self-administered computer screening may be a valid and time-efficient alternative to in-person screening.39 Physicians who choose to screen adolescents for substance use may want to provide examples of specific drugs (e.g., if querying ecstasy use, indicate that the substance known as Molly is a form of ecstasy; if querying e-cigarette use, indicate this includes the use of vapes or JUULs).
TABLE 2 Key Characteristics of Substance Use Screening Tools
| Screening tool | Patients | Time to administer | Optimal cut-point associated with problem use | Sensitivity (95% CI) | Specificity (95% CI) |
|---|---|---|---|---|---|
| Alcohol Use Disorders Identification Test (AUDIT)37 | 13 to 19 years of age; college students; emergency department patients | 2 minutes | 2 | 0.88 (0.83 to 0.93) | 0.81 (0.77 to 0.85) |
| CAGE Questionnaire*37 | Adults (not recommended for use with adolescents) | Not applicable (not recommended for use with adolescents) | 1 | 0.37 (0.29 to 0.44) | 0.96 (0.94 to 0.98) |
| CRAFFT Questionnaire†37 | 14 to 18 years of age | 74 seconds via paper; 49 seconds via computer | 1 | 0.92 (0.88 to 0.96) | 0.64 (0.59 to 0.69) |
| National Institute on Alcohol Abuse and Alcoholism (NIAAA) Screening Guide38 | Offers age-specific screening questions (9 to 11, 11 to 14, and 14 to 18 years of age) | Not documented; only two questions in length | Varies by age | 0.87 (0.76 to 0.94) | 0.84 (0.82 to 0.86) |
| Problem Oriented Screening Instrument for Teenagers (POSIT)37 | 12 to 19 years of age | 20 to 30 minutes | 1 | 0.84 (0.79 to 0.90) | 0.89 (0.86 to 0.92) |
Note: Links to the screening tools are available at https://www.drugabuse.gov/nidamed-medical-health-professionals/tool-resources-your-practice/screening-assessment-drug-testing-resources/chart-evidence-based-screening-tools-adults.36
*—CAGE = Have you ever felt you should Cut down on your drinking? Have people Annoyed you by criticizing your drinking? Have you ever felt bad or Guilty about your drinking? Have you ever had a drink first thing in the morning to steady your nerves or to get rid of a hangover (Eye opener)?
†—CRAFFT = Have you ever ridden in a Car driven by someone (including yourself) who was high or had been using alcohol or drugs? Do you ever use alcohol or drugs to Relax, feel better about yourself, or fit in? Do you ever use alcohol or drugs while you are by yourself, Alone? Do you ever Forget things you did while using alcohol or drugs? Do your family or Friends ever tell you that you should cut down on your drinking or drug use? Have you ever gotten into Trouble while you were using alcohol or drugs?
CONFIDENTIALITY
Confidentiality in adolescent health care visits is a significant predictor of the number and subject matter of health topics discussed.40 Adolescents particularly fear that alcohol, tobacco, or illicit substance use may be disclosed to their parents and/or legal authorities.41 Physicians should be aware of federal and state laws that apply to adolescent minor confidentiality because these may differ among states42 (https://www.guttmacher.org/state-policy/explore/overview-minors-consent-law). Parental support for adolescent confidentiality can be mixed, so research suggests a split-visit model. This model encourages parents to participate in the clinical visit for a limited time but then requests that parents leave the examination room to allow for an adolescent-physician confidential conversation.40 The American Academy of Family Physicians supports offering adolescents examinations and counseling separate from parents.42 It is essential for physicians and other health care professionals to explain the benefits of this model and to clarify adolescent and parent expectations and boundaries.40,43,44
LABORATORY TESTING
Laboratory (urine or serum) testing has limited use for diagnostic purposes and documenting history of substance use.45 Guidelines on the use of drug testing in children and adolescents are not clear, although the AAP supports further study of its safety and effectiveness.46 The AAP further recommends against implementing school- and home-based testing and supports informing concerned parents about the limitations of such testing.47
Prevention and Treatment
The U.S. Preventive Services Task Force and American Academy of Family Physicians have found insufficient evidence to assess the balance of benefits and harms of primary care–based behavioral interventions to prevent or reduce illicit substance use or nonmedical pharmaceutical use in children or adolescents.48,49
Although early identification is ideal, screening and interventions can be useful at any stage of illicit substance use.50 Prevention and treatment strategies often go together; prevention efforts can supplement cessation programs to maximize program effectiveness.51 Prevention programming aims to decrease risk and to promote protective factors while considering specific population characteristics, cultural influences, and determinants of health.29 Among Monitoring the Future survey participants, 40% of past year users of narcotics stated that they were originally prescribed their narcotics.52 To deter nonmedical use of prescription drugs by adolescent patients, prescribing physicians should consider reducing the number of prescriptions or amount in the prescription. As in treatment planning and delivery, prevention strategies focus on families, schools, and communities (Table 3). Treatment should address the needs of the whole person.50 Coexisting mental health problems should be identified and treated in conjunction with SUD,50 and primary care physicians should refer, as appropriate, to child/adolescent psychiatrists. Evidence-based treatment modalities range from school- and parent-based interventions that seek to involve the family in treatment to medication-assisted treatment (such as buprenorphine and naltrexone [Revia] in the treatment of opioid use disorder; Table 4).50
TABLE 3 Adolescent Substance Use Resources
| General information | |
| The Community Guide: Adolescent Health | |
| https://www.thecommunityguide.org/topic/adolescent-health?field_recommendation_tid=All&items_per_page=5 | |
| National Institute on Drug Abuse: Children & Teens | |
| https://www.drugabuse.gov/children-and-teens | |
| SAMHSA | |
| https://www.samhsa.gov/ | |
| Support and treatment | |
| American Academy of Addiction Psychiatry: Find a Specialist | |
| http://www.aaap.org/?page_id=658?sid=658 | |
| American Academy of Child and Adolescent Psychiatry: Child and Adolescent Psychiatrist Finder | |
| http://www.aacap.org/AACAP/Families_and_Youth/Resources/CAP_Finder.aspx | |
| American Society of Addiction Medicine: Search Membership Directory | |
| https://asam.ps.membersuite.com/directory/SearchDirectory_Criteria.aspx | |
| National Institute on Alcohol Abuse and Alcoholism Screening Guide | |
| https://pubs.niaaa.nih.gov/publications/Practitioner/YouthGuide/YouthGuidePocket.pdf | |
| SAMHSA: Behavioral Health Treatment Services Locator | |
| 800-662-4357 (800-662-HELP) | |
| https://www.findtreatment.samhsa.gov | |
| SAMHSA – TIP 31: Screening and Assessing Adolescents for Substance Use Disorders | |
| https://store.samhsa.gov/product/TIP-31-Screening-and-Assessing-Adolescents-for-Substance-Use-Disorders/SMA12-4079 | |
| Cultural awareness | |
| SAMHSA – TIP 59: Improving Cultural Competence | |
| https://store.samhsa.gov/system/files/sma14-4849.pdf | |
SAMHSA = Substance Abuse and Mental Health Services Administration; TIP = treatment improvement protocol.
TABLE 4 Principles of Substance Use Disorder Treatment

| Behavioral approach | ||
| Helps adolescents participate actively in recovery from illicit substance use; may include referral to community agencies that provide the following services: | ||
| 12-step facilitation | ||
| Adolescent community reinforcement | ||
| Cognitive behavior therapy | ||
| Contingency management | ||
| Group therapy | ||
| Motivational enhancement therapy | ||
| Family-based approach | ||
| Highlights the need to engage the adolescent's family in treatment; may include assisting the family to access agencies that offer the following services: | ||
| Brief strategic family therapy | ||
| Family behavior therapy | ||
| Functional family therapy | ||
| Multidimensional family therapy | ||
| Multisystemic therapy | ||
| Addiction medications | ||
| Can be effective, but none are approved by the U.S. Food and Drug Administration to specifically treat adolescents; some physicians use the following off-label for older adolescents: | ||
| Alcohol use disorders | ||
| Acamprosate (Campral) | ||
| Disulfiram (Antabuse) | ||
| Naltrexone | ||
| Nicotine use disorders | ||
| Bupropion (Zyban) | ||
| Nicotine replacement therapies | ||
| Varenicline (Chantix) | ||
| Opioid use disorders | ||
| Buprenorphine | ||
| Methadone | ||
| Naltrexone (Revia) | ||
| Recovery support services | ||
| Used to reinforce gains made in treatment and to improve quality of life; physicians can make referrals to these services, including the following: | ||
| Assertive continuing care | ||
| Mutual help groups | ||
| Peer recovery support | ||
| Recovery high schools | ||
Information from reference 50.
MOTIVATIONAL INTERVIEWING
Motivational interviewing is a way to develop conditions for positive behavior change53 and is especially suitable for communication with adolescents.41 It has a patient-centered focus and is designed to help individuals explore and resolve ambivalence around behavior change, including illicit substance use.53 Brief interventions using components of motivational interviewing may be suitable for addressing substance use, even among adolescents not seeking treatment for SUD.33 A previous AFP article (https://www.aafp.org/afp/2018/1215/p719.html; Tables 5, 6, and 7) provides examples of motivational interviewing.
Current and future initiatives for further reduction of adolescent substance use include SBIRT programs, increased training of primary care physicians, and expansion of integrated primary care and behavioral health systems to overcome the fragmented nature of our current health care system and the way provision of and payment for treatment have been managed.54 Public and private social welfare initiatives that work to safeguard vulnerable youth may help to mitigate or prevent health care disparities in child and adolescent populations.55
This article updates a previous article by Griswold, et al.4
Data Sources: We searched Medline using the key words adolescent, youth, substance use, substance abuse, alcohol, drug(s), tobacco, prevention, screening, treatment, primary care, physician. We repeated our search using Cochrane Database of Systematic Reviews and governmental websites, including SAMHSA, NIDA, and NIAAA. Search dates: October 2017 and December 2018.
Portions of this work were supported by the Health Resources Services Administration award number T32HP30035 (PI: L. Kahn) in support of Jessica A. Kulak.
The authors gratefully acknowledge the suggestions made by Dr. Gregory Homish, Dr. Linda Kahn, and Joan Kernan. We thank Angela Henke for her expert assistance on this manuscript.

