Eighty percent of adults requiring long-term care currently live at home in the community, and unpaid family caregivers provide 90% of their care. Family caregivers serve as a critical extension of the U.S. health care system, and the demand for family caregivers is expected to increase during the next few decades. Caring for loved ones is associated with several benefits, including personal fulfillment; however, caregiving is also associated with physical, psychological, and financial burdens. Family physicians can aid in the identification, support, and treatment of caregivers by offering caregiver assessments—interviews directed at identifying high levels of burden—as soon as caregivers are identified. Repeat assessments may be considered when there is a change in the status of the caregiver or the care recipient. Caregivers should be directed to appropriate resources for support, including national caregiving organizations, local elder care agencies, websites, and respite care. Psychoeducation, skills training, and therapeutic counseling interventions for caregivers have shown small to moderate success by decreasing caregiver burden and increasing caregiver quality of life. Additional research is needed to further identify strategies to offset caregiver stress, depression, and poor health outcomes. Support and anticipatory guidance for the caregiver is especially helpful during care transitions and at the care recipient's end of life.
A family caregiver is broadly defined as a friend or relative who provides unpaid assistance for a person with a chronic or disabling condition.1 Eighty percent of adults requiring long-term care currently live at home in the community, and unpaid family caregivers provide 90% of their care.2 These caregivers fill an important role for the family and provide a substantial cost savings of an estimated $470 billion nationwide in 2013.3 Family caregivers serve as a critical extension of the U.S. health care system, and supporting this “invisible and isolated army” has emerged as a national public health priority.3,4
WHAT IS NEW ON THIS TOPIC
Caregiver Care
Online interactive programs significantly reduce patient physical symptoms and decrease caregiver burden and depressive symptoms.
In caregivers of people with dementia, a meta-analysis showed that multicomponent interventions (e.g., education, resiliency training, problem solving) can reduce depressive symptoms, improve quality of life, and reduce caregiver burden.
The National Family Caregiver Support Program is the first federally funded program to formally recognize caregivers. However, in 2016, the program received only $150 million in federal funding, approximately one-twentieth of one percent of the estimated value of caregiver contributions to the health system.
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| All caregivers should be offered assessment to identify high levels of caregiver burden. | C | 1, 12, 16 |
| Encouraging caregivers to take a break, take care of their own health, seek preventive health care, join a support group, and seek respite care when needed are key ways that a family physician can provide direct caregiver support. | C | 5 |
| Caregivers identified as having unmet educational or informational needs should be directed to appropriate resources for support. | C | 1, 6, 13, 16 |
| Psychoeducational, skills training, and therapeutic counseling interventions for caregivers of patients with chronic conditions (e.g., dementia, cancer, stroke, heart failure) have small to moderate success in decreasing caregiver burden and increasing caregiver quality of life. | B | 34, 35, 37–39 |
| Anticipatory guidance, assistance with advance care planning, and information about appropriate resources should be provided to the care recipient and caregiver during care transitions and at the end of life. | C | 36, 37, 43 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
In the next few decades, the demand for family caregivers is expected to increase.5 This growing demand is attributed to shorter hospital stays, limited hospital discharge planning, and an aging U.S. population. By 2030, one in five adults will be 65 years or older, and a significant number of these older adults will require assistance with instrumental activities of daily living or activities of daily living.5 Table 1 lists common characteristics of care recipients.6
TABLE 1 Characteristics of Care Recipients

| Average age: 69 years |
| Behavioral problems (7%) |
| Female (65%) |
| Hospitalized in past 12 months (53%) |
| Memory problems (26%) |
| Need assistance with activities of daily living (59%) |
| Need assistance with instrumental activities of daily living (99%) |
Information from reference 6.
Caregiver Burden
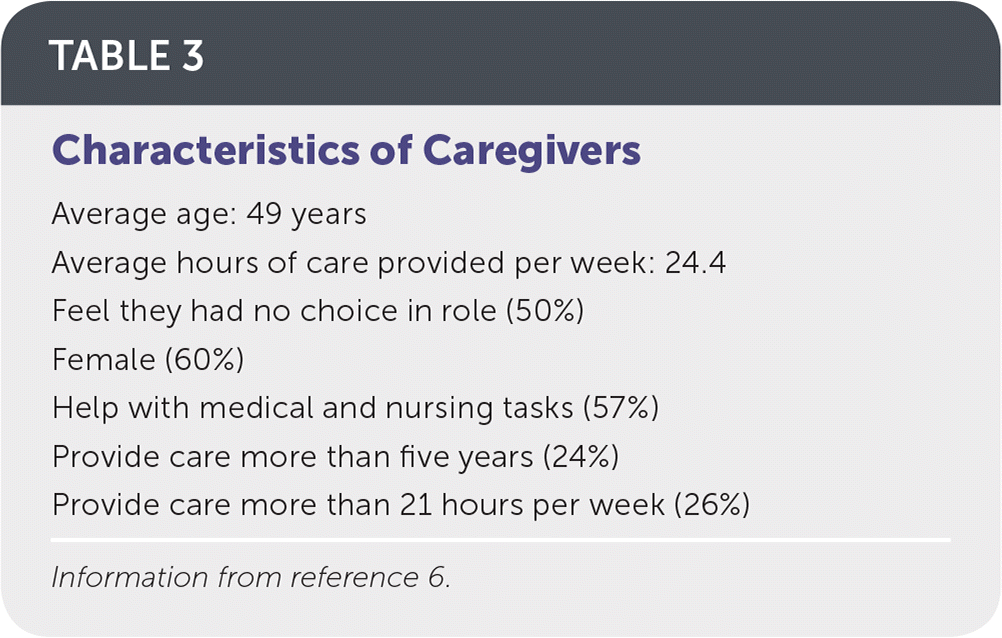
Caring for loved ones is associated with several benefits, including personal satisfaction in relieving another's discomfort, feeling useful and needed, and finding more meaning in life. Caregiving is also associated with significant physical, psychological, and financial burden for care providers (Table 2).1,3,6–12 Stressors associated with caregiving situations are often persistent, uncontrollable, and unpredictable, and one-third of all caregivers describe a high burden of care. Caregivers reporting the highest burden are more likely to be less educated, to live with the care recipient, to provide more than 21 hours of caregiving per week, to care for someone with cognitive impairment or difficult to manage behaviors, and to perceive they had no choice in assuming the caregiver role (Table 3).6 It is less common to have multigenerational family homes in the United States, which may place a more direct burden on one family member. Spousal caregivers are at high risk of caregiver burden, often providing a high number of care hours and assisting with medical tasks, and they are less likely to have additional help.6 Most caregivers report having less time for family and friends, having increased emotional stress, and neglecting self-care, such as healthy sleep, exercise, and dietary habits.5,13
TABLE 2 Elements of Caregiver Burden

| Financial effects6 |
| Increased absenteeism or reduced work hours |
| Increased self-reported financial strain |
| Loss of promotional and training opportunities |
| Loss of salary and benefits |
| Reduction in retirement savings and Social Security benefits |
| Health effects |
| Higher inflammatory burden and other biomarkers of poor health in caregivers for people with dementia7 |
| Higher rates of insomnia and depression8 |
| Higher risk of serious illness9 |
| Increased mortality for spousal caregivers10 |
| Less likely to engage in preventive care10 |
| Subjective sense of worsening health11 |
| Inadequate preparation, knowledge, and skills |
| Lack of information on how to care for recipient: safety, activities of daily living1,3,12 |
| Lack of information on self-care: coping with stress, finding time for self1,3,12 |
| Lack of information on support services1,3,12 |
TABLE 3 Characteristics of Caregivers
| Average age: 49 years |
| Average hours of care provided per week: 24.4 |
| Feel they had no choice in role (50%) |
| Female (60%) |
| Help with medical and nursing tasks (57%) |
| Provide care more than five years (24%) |
| Provide care more than 21 hours per week (26%) |
Information from reference 6.
Caregiver Assessment
Caregiver assessment refers to a systematic, family-centered process of gathering information about a caregiver situation to identify needs and resources. Assessment can be performed by the family physician or other health care team member.1 Ideally, caregivers and care recipients should be interviewed together and separately to allow assessment of confidential information such as elder abuse or caregiver stress.14
Initial assessment may be performed as soon as a person self-identifies as a caregiver. This may include the primary caregiver as well as other family members, friends, or neighbors who consider themselves caregivers. Repeat assessments can be offered as the care recipient's or caregiver's condition changes. These changes may be triggered by the diagnosis of a medical condition associated with high burden (i.e., care requiring more than 21 hours per week), change in functional status of a caregiver or care recipient, or care transitions, and should involve development of a care plan for additional support and resources.12 The National Consensus Development Conference for Caregiver Assessment developed practice guidelines that have been incorporated in the Guided Care model15 and promoted by numerous national organizations.1,12,16,17 See a caregiver assessment table at https://www.caregiver.org/caregivers-count-too-section-3-caregiver-assessment-table for practical in-office questions,16 and the Modified Caregiver Strain Index at https://consultgeri.org/try-this/general-assessment/issue-14.pdf.18 The adapted Zarit Burden Interview is another validated tool that can be used to assess caregiver burden; see appendix at https://bit.ly/2Hso3qt.19
Caregiver Support
Despite many published research trials showing effective interventions, such as multidimensional and psychoeducational interventions,20–22 there has been a delay in translating the research into resources that are readily accessible to caregivers. This requires development of best practices, assessment of clinical relevance, and restructuring of reimbursements to allow for sustainability. Until this happens, family physicians can focus on practical, individualized interventions aimed at assisting caregivers.23
Caregivers should be encouraged to take a break, join a support group, and pursue their own interests. They should be encouraged to take care of their own health, including preventive health care, and to seek respite care when needed.5
Family physicians should provide accurate, disease-specific education and resources for obtaining more information1,6,13,16 (Table 4). Online toolkits, such as the AARP's Prepare to Care: A Planning Guide for Families, can be easily accessed and provided during an office visit.24 Caregivers should be offered training in medical tasks and specific care needs with the help of therapists and nurses. Referrals should be made to appropriate resources such as local elder care agencies, home health care services, adult day programs, and meal delivery services.
TABLE 4 Caregiver Resources
| Organization | Website | Resources |
|---|---|---|
| National organizations | ||
| AARP | https://www.aarp.org/caregiving/ | Prepare to Care guide, legal and financial information, local resources |
| American Academy of Family Physicians | https://familydoctor.org/caregiver-stress/ | General information on caregiver self-care |
| Caregiver Action Network | https://caregiveraction.org/ | Scenario-specific tips and toolbox, caregiver connections |
| Family Caregiver Alliance, National Center on Caregiving | https://www.caregiver.org/ | Disease- and issue-specific fact and tip sheets, caregiver connections, policy and advocacy information |
| Mather Lifeways Institute on Aging | https://www.matherlifewaysinstituteonaging.com/category/caregiving/ | Caregiver-specific articles, senior housing initiatives |
| National Institute on Aging | https://www.nia.nih.gov/health/caregiving | Caregiving tips with focus on dementia and older adults |
| Rosalynn Carter Institute for Caregiving | http://rci.gsw.edu | Caregiver workshops and resources, research |
| Caregiver education and respite care | ||
| Alzheimer's Association and AARP | https://www.communityresourcefinder.org | Programs, resources for housing, caregivers |
| American Elder Care Research Organization | https://www.payingforseniorcare.com | Resources for paying for care, managing insurance, reducing costs |
| ARCH National Respite Network and Resource Center | https://archrespite.org/ | Respite locator and funding by state |
| AssistGuide Information Services | http://www.agis.com | Explanation of government resources, Medicare/Medicaid, assistive devices |
| Caring Today | http://caringtoday.com/blog/ | Caregiver blog |
| Family Caregiver Alliance Camp for Caring | https://www.caregiver.org/camp-caring | Respite camp for caregivers and recipients |
| Hospice Foundation of America | https://www.hospicefoundation.org | Information about hospice care |
| United Hospital Fund Next Step in Care | https://www.nextstepincare.org | Focus on helping caregivers with transitions in care, communication with health care teams |
| U.S. Administration on Aging | https://www.eldercare.gov | Local community resources |
| U.S. Administration on Aging | https://www.longtermcare.gov | Resources for long-term care placement |
| Specific caregiving scenarios | ||
| Caregiving.com | https://www.caring.com/support-groups/caring-for-a-spouse | Caregiver blog for spouses, topics including finances, intimacy, and managing symptoms |
| Centers for Disease Control and Prevention | https://www.cdc.gov/ncbddd/disabilityandhealth/family.html | Tips for caregivers of people with disabilities |
| National Organization for Rare Disorders | https://rarediseases.org/for-patients-and-families/connect-others/find-patient-organization/ | Disease-specific resource for support groups |
| Parent to Parent | http://www.p2pusa.org/ | Resources with local options for families of children who have special needs |
| U.S. Department of Veterans Affairs | https://www.caregiver.va.gov/ | Resource for caregivers, mentoring program, hotlines, access to support coordinator |
| Well Spouse Association | https://wellspouse.org | Support group locator, national conference, social community |
Family physicians should encourage caregivers to participate in the health care of the recipient. Evidence suggests that when care recipients and caregivers are treated as a dyad, outcomes for both are improved.25 Caregivers often know the most about the needs of the care recipient and can be vital allies in the care management plan. Evidence shows that caregiver involvement and agreement with the care plan increases adherence to recommendations.26
There is strong evidence that early palliative care interventions for patients with serious illness improve quality of life and family satisfaction, and can reduce caregiver burden.27 Family physicians are uniquely positioned to provide primary palliative care, such as facilitating goals of care discussions and advance care planning. Addressing the care recipient's symptoms of chronic illness can improve the caregiver's quality of life and help relieve the caregiver's distress over the recipient's discomfort.28
Caregiver care often necessitates offering innovations in self-management through technology. Family caregivers can now access educational materials as well as connect with other caregivers online.13 Websites and apps are available to schedule tasks and help families coordinate caregivers, meal delivery, and appointments. Wearable technology and remote monitoring systems are expanding and hold promise for improving the lives of caregivers.29 Online interactive programs have shown reductions in patient physical symptoms and in caregiver burden and depressive symptoms.30,31 Advancements in smart home environments allow caregivers to monitor care recipients from remote locations, detecting changes and preventing adverse events in the care recipient.32 Telehealth options are expanding and offer real-time access to health care teams. Table 5 lists apps and services recommended by reputable online resources such as AARP and the National Alliance on Caregiving. Despite potential benefits of new technologies, these innovations may be limited by the ability of caregivers to access and learn how to operate new devices, overcome cost barriers, and avoid the perception of depersonalized care.32
TABLE 5 Technology and Apps for Caregivers
| Organization | Website | Resources |
|---|---|---|
| General information | ||
| AARP | https://www.aarp.org/caregiving/home-care/info-2017/technology-apps-ag.html | Tips for choosing caregiving apps |
| Family coordination | ||
| AARP Caregiving App | https://states.aarp.org/aarp-caregiving-app | Calendar, caregiver coordination |
| CareZone | https://carezone.com/home | Caregiver coordination health care record keeping, scheduling |
| Caring Bridge | https://www.caringbridge.org | Calendar, scheduling, forum for updates, fundraising |
| Caring Village | https://www.caringvillage.com | Calendar, communication, document storage, to-do lists |
| Evernote | https://evernote.com | Organization, to-do lists |
| Google Calendar, Google Docs | https://www.google.com | Calendar and shared documents |
| Lotsa Helping Hands | https://lotsahelpinghands.com | Calendar, forum for updates |
| Transportation | ||
| AARP Transportation Services | https://www.aarp.org/caregiving/home-care/transportation-services/?intcmp=CAR-LRS-R3-C2 | General information |
| Arrive | https://arriverides.com | Links to Uber and Lyft without need for smartphone |
| GoGoGrandparent | https://gogograndparent.com | |
| Remote monitoring | ||
| Blipcare (blood pressure monitoring) | http://www.blipcare.com | Various monitoring tools using wearable devices |
| eCare 21 | https://ecare21.com | |
| GPS SmartSole (trackable shoes) | http://gpssmartsole.com/gpssmartsole | |
| Luna Lights (automated lighting) | https://lunalights.org | |
| SafeinHome (alerts) | http://www.safeinhome.com | |
| Consumer Reports: Medical Alert Systems | https://www.consumerreports.org/medical-alert-systems/how-to-choose-a-medical-alert-system | How to choose medical alert system |
| Medication management | ||
| Medisafe | https://medisafe.com | Medication management, reminders |
| MyMeds | https://www.my-meds.com | |
| MyMedSchedule | https://secure.medactionplan.com/mymedschedule | |
| Telehealth services | ||
| AARP Telehealth Services | https://www.aarp.org/caregiving/health/telehealth-services/?intcmp=CAR-LRS-R3-C1 | General information |
Specialized Caregiving
CANCER
Changes in health care and insurance reimbursement have led to much of cancer care being provided at home, with the family assuming more responsibilities.33 A 2017 meta-analysis found that psychoeducational interventions were the most common intervention researched; however, they often require significant time, making them hard to translate to clinical practice.34 Pain management skills and symptoms assessment are the largest caregiver needs.34 A 2015 study found that interdisciplinary palliative care interventions such as educational sessions and self-care plans improved caregivers' social well-being scores, lowered psychological distress scores, and significantly reduced caregiver burden.35 Continued research with a focus on palliative care interventions, the effect on caregivers, and ways to increase the availability of these services is needed.
DEMENTIA
Caregiving for a person with dementia is associated with high levels of strain caused by associated behavior disturbances, intense physical tasks, and the need for constant vigilance. High caregiver strain has been identified as a predictor of long-term care placement in these patients; therefore, family physicians should identify caregivers early and provide support.36 Fact sheets available from Family Caregiver Alliance are free, easy to download, and provide practical guidance on topics such as understanding and managing dementia behaviors, controlling frustration, self-care, and end-of-life decision-making.1
Evidence to support caregiver interventions in this subgroup is fairly robust.37–39 Structured education provided in home and telephone-based sessions to improve caregiver coping skills and management of behaviors have decreased caregiver burden and improved quality of life for the caregiver and care recipient.37 A meta-analysis showed that multicomponent interventions (e.g., education, resiliency training, problem solving) can reduce depressive symptoms, improve quality of life, and reduce caregiver burden.38 Interventions are cost saving or cost neutral by helping to keep care recipients in the community longer.39 Additional resources are needed to translate these interventions into opportunities accessible to all caregivers.
HEART FAILURE
Caregivers of patients with heart failure report similar issues as those caring for patients with other chronic illnesses.40 The most burdensome aspects of care are enforcing dietary restrictions and monitoring for signs and symptoms of heart failure.40,41 Care recipients with heart failure may have frequent exacerbations requiring hospitalization and a more uncertain clinical trajectory that can increase caregiver strain. During the past decade, there have been significant advances in the availability of advanced heart failure therapies (e.g., left ventricular assist devices, inotropic medications) that can lower hospitalization and mortality rates. Availability of these therapies may increase life expectancy, but often leave care recipients with a higher degree of functional disability, thereby increasing the burden of caregiving.42 Overall, few interventions have been thoroughly studied to effectively support caregivers of patients with heart failure.43 Given the high level of symptom monitoring, caregiver burden, and uncertainty in disease trajectory, many experts are calling for earlier and concurrent involvement of palliative care with the goal of improving caregiver education and confidence, assistance with management of symptoms, and skilled advanced care planning.43
STROKE
Stroke is the leading cause of serious long-term disability, and most stroke survivors return home.44 These care recipients often require significant assistance with activities of daily living and instrumental activities of daily living.44 A review of caregiver interventions shows that those with a focus on dyad interventions may help survivor outcomes; however, interventions targeted specifically toward caregivers are needed to improve caregiver outcomes.45 Skill-building interventions (e.g., problem solving, tips for communicating with health care professionals, strategies for lifting) were more effective at improving caregiver outcomes than providing information about the diagnosis alone.45 Appropriate referrals to home health care, skilled therapy, and respite care should be offered by the family physician in addition to options for home modifications.
TRANSITIONS IN CARE
Many caregivers experience a decrease in depressive symptoms after the death of a care recipient, which may mark the end of the care recipient's discomfort. The placement of a care recipient into a long-term care facility is not associated with positive effects on the caregiver and may be accompanied by an increase in caregiver anxiety.46 This implies that the relief of the daily caregiving burden does not account for the reduction in depressive symptoms in bereaved caregivers. To ease these care transitions, family physicians should provide anticipatory guidance, assistance with advance care planning, and appropriate resources for respite, long-term, and end-of-life care.36,37,43 It may be more useful to intensify resources and support in the time preceding death rather than afterwards.47
Public Policy
Providing optimal care for the patient and caregiver mandates an understanding of financial reimbursement strategies. The Family and Medical Leave Act allows qualified employees to take up to 12 weeks of continuous or intermittent unpaid leave to provide care. The United States is one of the few developed economies that does not offer mandatory paid leave, a topic that has emerged as a new public policy interest. The National Family Caregiver Support Program was the first federally funded program to formally recognize caregivers. However, in 2016, the program received only $150 million in federal funding, approximately one-twentieth of one percent of the value of caregiver contributions.47 Consumer-, participant-, and self-directed care programs are now available in nearly every state, allowing informal caregivers, such as a spouse or other family member, to be paid for the services they provide. Most programs are based on Medicaid home- and community-based service waiver programs that provide in-home assistance for nursing home–eligible care recipients who qualify for Medicaid services. However, options have expanded to include non-Medicaid programs, veterans' programs, life insurance, and long-term care insurance to allow family members to be paid caregivers.48
This article updates previous articles on this topic by Parks and Novielli,49 and by the authors.50
Data Sources: A PubMed search was completed using Clinical Queries and the key terms caregiver, burden, and stress. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. Also searched were the Agency for Healthcare Research and Quality evidence reports, Clinical Evidence, the Cochrane database, and the Institute for Clinical Systems Improvement. Search dates: February 15, 2018, and January 2, 2019.

