Polypharmacy, defined as regular use of at least five medications, is common in older adults and younger at-risk populations and increases the risk of adverse medical outcomes. There are several risk factors that can lead to polypharmacy. Patient-related factors include having multiple medical conditions managed by multiple subspecialist physicians, having chronic mental health conditions, and residing in a long-term care facility. Systems-level factors include poorly updated medical records, automated refill services, and prescribing to meet disease-specific quality metrics. Tools that help identify potentially inappropriate medication use include the Beers, STOPP (screening tool of older people's prescriptions), and START (screening tool to alert to right treatment) criteria, and the Medication Appropriateness Index. No one tool or strategy has been shown to be superior in improving patient-related outcomes and decreasing polypharmacy risks. Monitoring patients' active medication lists and deprescribing any unnecessary medications are recommended to reduce pill burden, the risks of adverse drug events, and financial hardship. Physicians should view deprescribing as a therapeutic intervention similar to initiating clinically appropriate therapy. When deprescribing, physicians should consider patient/caregiver perspectives on goals of therapy, including views on medications and chronic conditions and preferences and priorities regarding prescribing to slow disease progression, prevent health decline, and address symptoms. Point-of-care tools can aid physicians in deprescribing and help patients understand the need to decrease medication burden to reduce the risks of polypharmacy.
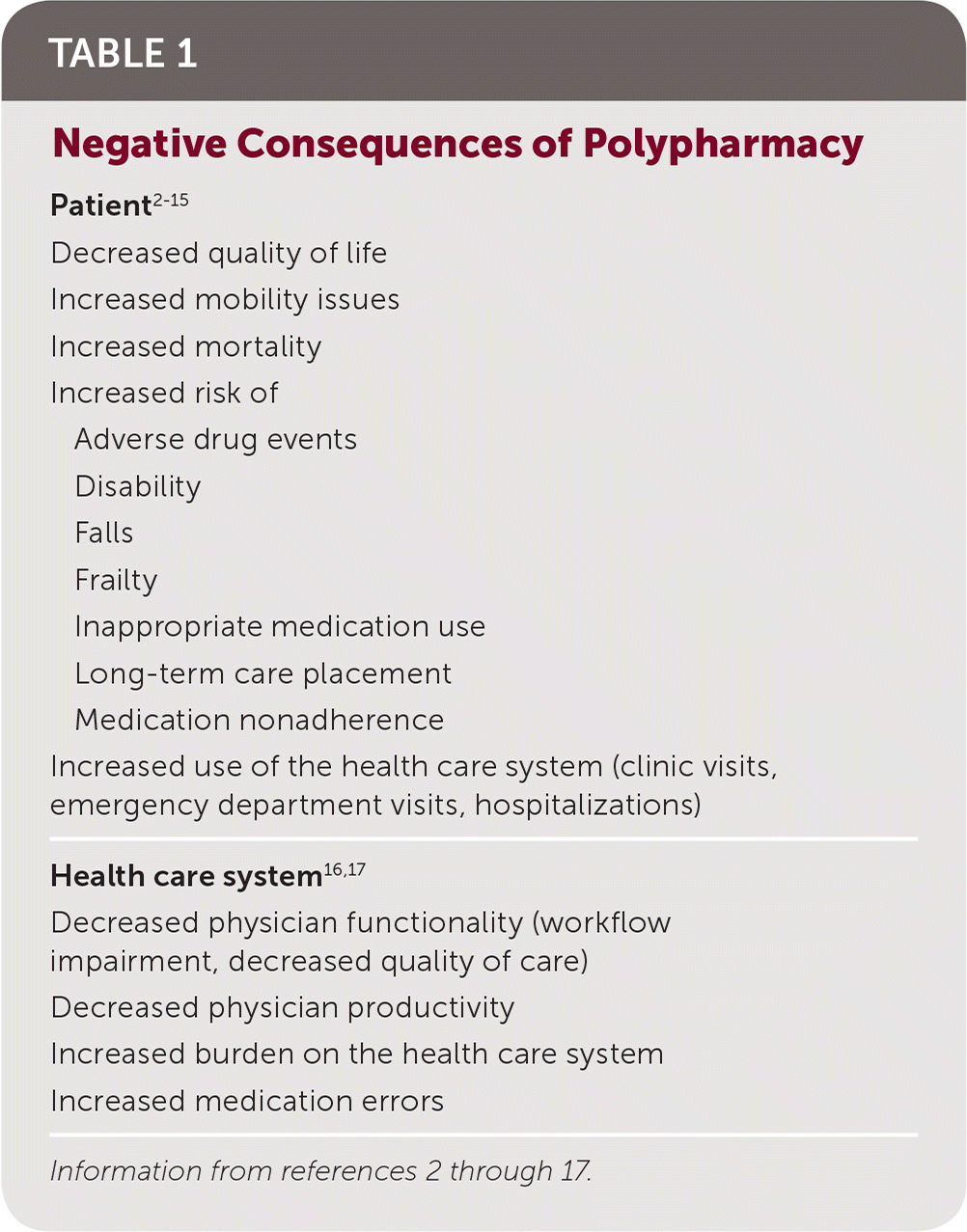
As the size of the older adult population (those older than 62) and the number of younger people with complex health conditions have increased in the United States, polypharmacy has become a growing problem.1 Polypharmacy has negative consequences for patients and the health care system (Table 1).2–17 For example, patients taking more than four medications have an increased risk of injurious falls, and the risk of falls increases significantly with each additional medication, regardless of medication type.18
SORT: KEY RECOMMENDATIONS FOR PRACTICE
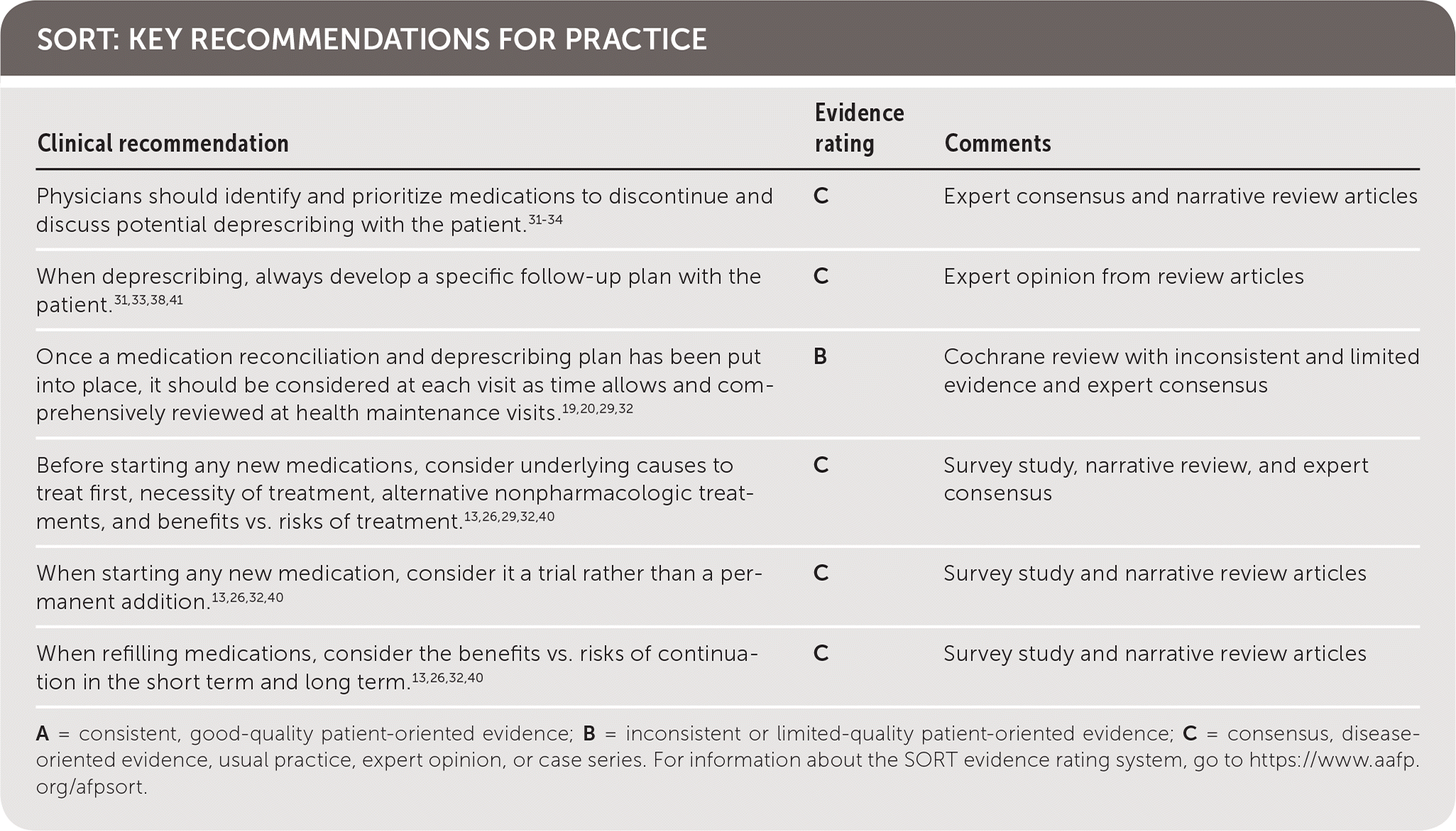
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN PHARMACOLOGY

| Recommendation | Sponsoring organization |
|---|---|
| Do not prescribe medications for patients currently on five or more medications, or continue medications indefinitely, without a comprehensive review of their existing medications, including over-the-counter medications and dietary supplements, to determine whether any of the medications or supplements should or can be discontinued. | American Society of Health-System Pharmacists |
| Do not prescribe a medication without conducting a drug regimen review. | American Geriatrics Society |
Source: For more information on the Choosing Wisely Campaign, see http://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
TABLE 1. Negative Consequences of Polypharmacy
| Patient2–15 |
| Decreased quality of life |
| Increased mobility issues |
| Increased mortality |
Increased risk of
|
| Increased use of the health care system (clinic visits, emergency department visits, hospitalizations) |
| Health care system16,17 |
| Decreased physician functionality (workflow impairment, decreased quality of care) |
| Decreased physician productivity |
| Increased burden on the health care system |
| Increased medication errors |
Although there is no standard definition for polypharmacy, the definition widely used in the literature is the regular use of at least five medications.19 This threshold does not account for whether the medications are appropriate per the Beers criteria.20 Multiple medications may be indicated in patients with certain complex medical conditions, such as heart disease or diabetes mellitus. In these cases, polypharmacy may be appropriate. However, prescribing to meet disease-specific quality metrics could increase polypharmacy for patients with multiple medical conditions, which increases the risk of adverse consequences and increases the patient's financial burden.21
Risk Factors for Polypharmacy
Polypharmacy is most recognized in older adults, because patients with one or more chronic conditions have longer medication lists.21,22 Older adults with multiple subspecialist physicians and no primary care physician are particularly vulnerable to polypharmacy. Adults residing in long-term care facilities are also at risk, because they are more frail than community-dwelling populations and have multiple medical issues and cognitive impairment that often warrant pharmacologic treatment. Up to 91% of patients in long-term care take at least five medications daily.23
Younger adults with chronic pain, such as fibromyalgia, or with developmental disabilities, especially those with additional chronic medical conditions, may experience polypharmacy because of multiple treatments and modalities.22 Other conditions associated with polypharmacy in younger patients include diabetes, heart disease, stroke, and cancer.24
A population often overlooked with regard to polypharmacy is patients with mental health conditions.22,25 These patients are often prescribed psychotropic medications with adverse effects, and more medications may be added to mitigate side effect profiles. Although patients with chronic mental health and medical issues may require multiple medications to achieve maximal functioning and prevent disease sequelae, this appropriate polypharmacy can still increase the risk of adverse drug events.
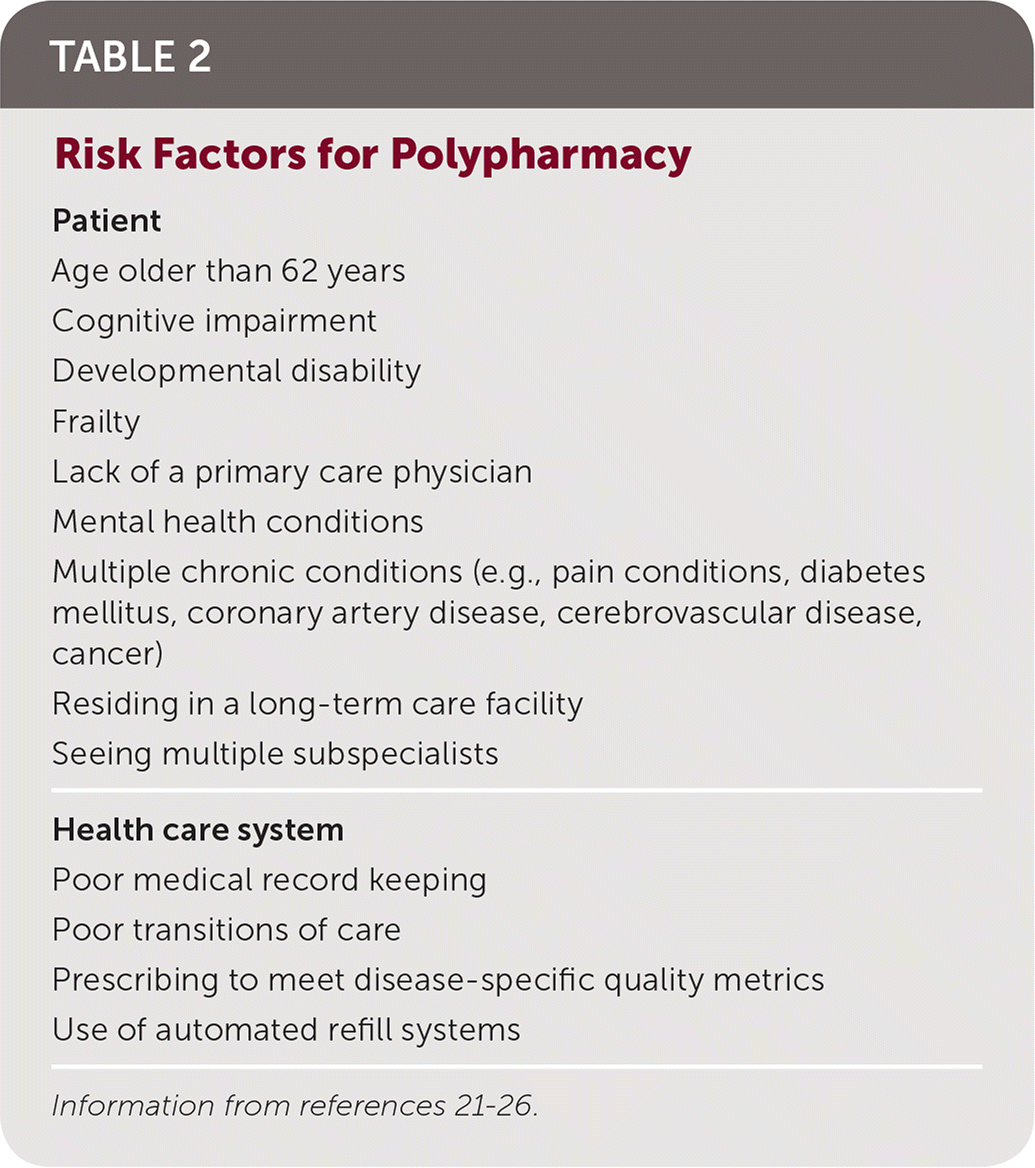
Polypharmacy risk factors can occur at the patient level and at the health care system level (Table 2).21–26 For example, poor medical record keeping can lead to polypharmacy if discontinued medications are not removed from the record and are refilled automatically or if a physician receives an automated refill request for a discontinued medication.
TABLE 2. Risk Factors for Polypharmacy
| Patient |
| Age older than 62 years |
| Cognitive impairment |
| Developmental disability |
| Frailty |
| Lack of a primary care physician |
| Mental health conditions |
| Multiple chronic conditions (e.g., pain conditions, diabetes mellitus, coronary artery disease, cerebrovascular disease, cancer) |
| Residing in a long-term care facility |
| Seeing multiple subspecialists |
| Health care system |
| Poor medical record keeping |
| Poor transitions of care |
| Prescribing to meet disease-specific quality metrics |
| Use of automated refill systems |
Assessment Tools for Polypharmacy
No validated tool or strategy has been proven superior in improving polypharmacy-related patient outcomes. Also, no one validated tool assesses all aspects of potentially inappropriate medication use or polypharmacy.19 Based on a 2018 Cochrane review, it is unclear if interventions to reduce inappropriate polypharmacy improve patient-oriented outcomes.19 Although interventions may reduce potential prescribing omissions, this needs to be validated in future trials.19
Assessment tools may be explicit, implicit, or mixed.27 Explicit tools, such as the Beers, STOPP (screening tool of older people's prescriptions), and START (screening tool to alert to right treatment) criteria, have rigid standards, and clear criteria assist with quick and easy decision-making. However, patient complexity is not considered in the decision-making process.20,28 These tools allow for comparison of a patient's medication list to a set of potentially inappropriate medications and to check for medication duplication; medication and disease interactions; and medication adjustments required for certain disease states, such as renal impairment. The recently updated Beers criteria list potentially inappropriate medications by drug class and disease state.20 The STOPP and START criteria are used together to identify medications that may be inappropriate (STOPP) and alternative medications that can be started to safely treat a disease (START).28
Implicit tools, such as the Medication Appropriateness Index, are more time-consuming, because they are based on physician judgment rather than set criteria, but they are more patient-centered and consider patient complexity. Implicit tools are inherently limited by the physician's knowledge, experiences, and attitudes and are less reliable than explicit tools in clinical studies.27,29 The Medication Appropriateness Index (https://globalrph.com/medcalcs/medication-appropriateness-index-calculator/) includes 10 questions that address medication need; optimal therapy for diseases and conditions; medication duplications; appropriateness of dosage, formulation, and duration of treatment; medication and disease interactions; and directions for use.30 Although the questions are clear and straightforward, it can take considerable time to apply the Medication Appropriateness Index to each medication prescribed.
Approach to Deprescribing
Physicians should identify and prioritize medications to discontinue and discuss potential deprescribing with the patient.31–34 There are many definitions for deprescribing. One definition is: a systematic process to identify and discontinue medications in instances in which existing or potential harms outweigh potential benefits within the context of an individual patient's care goals, current level of functioning, life expectancy, values, and preferences.31 Deprescribing discontinues medications, decreases medication dosages, and changes medications to optimize clinical outcomes.31,35–38 Evidence is lacking that a structured approach to decreasing the absolute number of medications, as opposed to discontinuing potentially inappropriate medications, improves patient outcomes.19,20,31,35,39 This is likely because deprescribing efforts are focused, patient-specific interventions with considerable variability in patient characteristics and medications used. Guidelines often discuss how to initiate therapies but rarely discuss when and how to discontinue them. Judicious prescribing is as important as judicious deprescribing (Table 3).13,26,32,40
TABLE 3. Considerations for Judicious Prescribing

Before starting any new medication ask:
|
When starting any new medications, consider it a trial rather than a permanent addition.
|
| When renewing refills, consider the benefits vs. the risks of continuation (long term and short term). |
Physicians should view deprescribing as initiating a “therapeutic intervention” similar to initiating clinically appropriate therapy.31,33,41 When deprescribing, it is imperative to consider patient/caregiver perspectives on goals of therapy, including views on medications and chronic conditions and preferences and priorities regarding prescribing to slow disease progression, prevent health decline, and address symptoms.38 Only one-third of older adults specifically discuss health care decision-making priorities with their primary care physicians.39 However, patients are more likely to consider deprescribing if the physician recommends it.42–44 Physicians should also examine specific therapy goals at every patient visit—disease control (primary/secondary prevention, symptom control/management) vs. acute symptom management.38 A specific follow-up plan for deprescribing should be developed with the patient.31,33,38,41 Furthermore, practices and health systems should adopt streamlined approaches to medication reconciliation and tracking, because up-to-date medication lists might help identify potential medications for deprescribing and reduce physician, staff, and patient burden. Figure 1 presents an approach to deprescribing.10,13,31,32,34,35,38,40
FIGURE 1.

An approach to deprescribing. (ADME = absorption, distribution, metabolism, and excretion.)
Information from references 10, 13, 31, 32, 34, 35, 38, and 40.
Once a medication reconciliation and deprescribing plan has been put into place, it should be considered at each visit as time allows and comprehensively reviewed at health maintenance visits.19,20,29,32 There are several resources available that physicians can use at the point of care to help identify problems with medication prescribing (Table 4).
TABLE 4. Point-of-Care Resources for Deprescribing
| Resource | Comments |
|---|---|
| Beers criteria20 | List of medications that pose the highest risk to older adults, as well as alternatives |
| Bruyère Research Institute and the Canadian Deprescribing Network: https://deprescribing.org | Guidelines, shared decision-making aids, up-to-date research, and algorithms for discontinuing proton pump inhibitors, antihyperglycemics, antipsychotics, benzodiazepines, cholinesterase inhibitors, and memantine (Namenda) |
| Electronic health records, such as Epic or NextGen | Autodiscontinuation of expired medications, which may help reduce polypharmacy |
| Epocrates: https://www.epocrates.com | Check for drug-drug or drug-herbal interactions |
| MedStopper: http://medstopper.com | Allows users to enter a medication list and receive recommendations regarding which medications might be discontinued or switched |
Challenges to Deprescribing
The benefits of deprescribing and shortened medication lists are recognized at the patient, physician, and system levels. However, time constraints, patient resistance, and lack of systematic support hinder acceptance of deprescribing as routine medical care. Patients may be reluctant to discontinue medications, even when presented with evidence that the medications are not beneficial and may cause physiologic harm and financial distress. Patients taking chronic medications may worry about conditions worsening and resist discontinuing medications despite new guidelines (e.g., concurrent use of opioids and benzodiazepines is now discouraged).45 Patients taking medications prescribed by previous physicians may fear contradicting the original care plan by stopping their medications.33 Automated refills of discontinued medications may confuse patients and delay deprescribing because of unclear communication.
Primary care physicians may feel pressured to address multiple issues per visit and may not have adequate time to counsel patients on polypharmacy or to deprescribe through shared decision-making. Additionally, pressure from patients who desire medications with unclear benefit may cause physicians to prescribe medications to minimize interruption in clinic workflow.
Patients with multiple prescribers may be reluctant for one physician to stop medications prescribed by another. Such deprescribing must occur with clear interphysician communication to formulate a comprehensive patient care plan.
Three professional organizations in the American Board of Internal Medicine Foundation's Choosing Wisely campaign (American Geriatrics Society, American Society of Health-System Pharmacists, and American Psychiatric Association) specifically mention polypharmacy and the need to review medications regularly, question the utility of adding new medications, and deprescribe when appropriate.32 Such recommendations can persuade physicians to consider deprescribing and can reassure patients that deprescribing medications is evidence based and beneficial.
Data Sources: A PubMed search was completed using the key terms polypharmacy, multiple medications, risks, potentially inappropriate medications, and deprescribing. The search included randomized controlled trials, clinical trials, reviews, and meta-analyses, as well as case reports and evidence-based guidelines. Searches were also performed in the Cochrane Database of Systematic Reviews, UpToDate, the Canadian Task Force on Preventive Health Care, the ABIM Foundation's Choosing Wisely website, the Centers for Disease Control and Prevention guideline on prescribing opioids for chronic pain, and the U.S. Preventive Services Task Force recommendations. Search dates: July and August 2018, and February 2019.

