Case Scenario
A 56-year-old patient recently came in for a six-month follow-up for some well-controlled medical conditions. He has been my patient for more than 20 years and has generally been upbeat at his visits. Over the past few years, he has shared freely about his wife's battle with metastatic colon cancer. When asked how he was handling her declining health, he typically responded, “I'm hanging in there.” At this visit, the veneer of keeping things together had vanished. He shared through teary eyes that his wife had died about a month ago. He was visibly upset, barely made eye contact, and spoke with a shaky voice. He tried to maintain his composure, but emotions got the better of him. I offered comfort and condolences as best I could; however, I didn't believe that I helped much. Other than referring him for grief counseling, what are some recommendations for busy primary care physicians when helping grieving patients?
Commentary
The loss of a loved one, especially a spouse or a child, is perhaps one of the most difficult events a person will experience in a lifetime. The resulting grief can be overwhelming and incapacitating for a time. Family physicians can be sources of comfort to those who grieve the loss of someone close to them.
The knowledge of several terms is useful when helping a patient who is facing the experience of a loss or who has experienced a loss (Table 1). Individuals caring for a loved one often feel anticipatory grief, bereavement, grief, mourning, and, in extreme circumstances, complicated grief.1,2
TABLE 1. Description of Grief-Related Terms
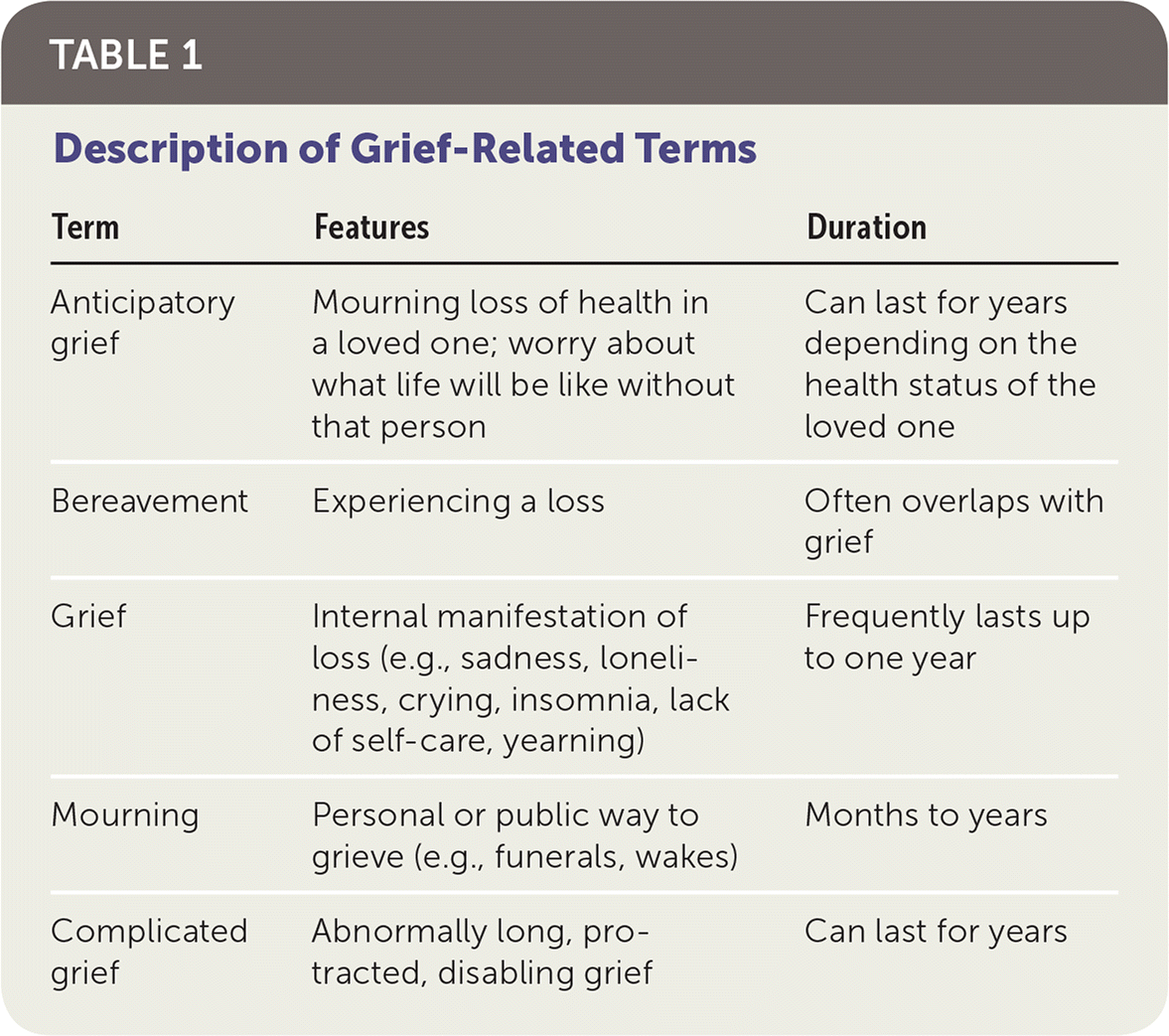
| Term | Features | Duration |
|---|---|---|
| Anticipatory grief | Mourning loss of health in a loved one; worry about what life will be like without that person | Can last for years depending on the health status of the loved one |
| Bereavement | Experiencing a loss | Often overlaps with grief |
| Grief | Internal manifestation of loss (e.g., sadness, loneliness, crying, insomnia, lack of self-care, yearning) | Frequently lasts up to one year |
| Mourning | Personal or public way to grieve (e.g., funerals, wakes) | Months to years |
| Complicated grief | Abnormally long, protracted, disabling grief | Can last for years |
Bereavement, grief, and mourning are all normal experiences. Symptoms of grief can include sadness, loneliness, yearning for the deceased, insomnia, crying, relief, anger, and social withdrawal.3 The intensity of these symptoms lessens with time, and most people are over the worst of it after one to two years. For many people, grief is a process that includes different emotions of varying intensities along the way. For others, grief occurs in stages, although this is not a universally accepted paradigm.4,5
Little well-designed research exists to support any bereavement interventions,6,7 which include individual and group counseling through mental health or palliative care services. Even less is known about the role of primary care physicians in addressing bereavement.8 Given the lack of guidance from reliable evidence, most reviews recommend tailoring the intervention to the cues and perceived needs of the bereaved. Most of the time, those without underlying mental disorders do not require any specific treatment, such as medication or grief counseling.9 Early intervention is not recommended because it may interfere with the grieving process.7 Patients with extended grief or grief complicated by depression may receive greater benefit from counseling.7 Family physicians might consider the following steps to support their bereaved patients.
Schedule a Dedicated Visit. Address anticipatory grief in detail by scheduling a separate, dedicated visit. It can be helpful to discuss the grieving process at this time. During anticipatory or actual grieving, patients may find it helpful to have someone else state some of the emotions they are experiencing, and they may appreciate their physician's support.
Provide Support. Responding to patients' cues can provide appropriate support after a loss. Kind, compassionate words spoken with empathy go a long way in comforting someone in the midst of loss. A short phone call a couple days after the visit to check in or a personal note can be of tremendous comfort.1 An appropriately timed visit with the patient after spousal death can be helpful. Patients can be reassured that their emotions, feelings, and pain are normal and that everyone experiences grief and loss a little differently. Individuals manifest a variety of emotions and behaviors. It can be comforting to the patient to be assured that the intensity of these emotions will diminish with time. There will be times of intense sadness, but these can be punctuated by episodes of cheerfulness.9,10 Most people will be making significant progress by six months and many are back to relatively normal functioning by one year. Emotions can vary over time, often flaring at unexpected times.
Provide Information About Support Groups and Other Resources. Interventions have not been shown to alter the grief trajectory, but individuals do not have to cope with their loss alone. Physicians can help by referring the patient to support groups and other resources. For instance, others who have previously experienced loss have written road maps of their experiences, which can be comforting to others. Physicians could have a short list of topical reading materials or websites to provide to patients (Table 2).
TABLE 2. Resources for Bereaved Patients
| Books |
| Lewis CS. A Grief Observed. 2nd ed. London: CrossReach Publications; 2016. |
| Zonnebelt-Smeenge SJ, De Vries RC. Getting to the Other Side of Grief: Overcoming the Loss of a Spouse. Grand Rapids, Mich.: Baker Books; 2019. |
| Websites |
| AARP |
| Candlelighters – Childhood Cancer Family Alliance |
| The Compassionate Friends – Supporting family after a child dies |
| GriefNet – Community of persons coping with grief, death, trauma, or major loss |
| National Widowers' Organization – Toolkit for men coping with the loss of a loved one |
Attend to Health Effects and Comorbidities. Grief is usually self-limiting and is considered normal, but it can have associated morbidity, including myocardial infarction. The mechanism is unknown, but altered hemodynamic changes have been shown to occur in early grief.11,12 An increased risk of excessive alcohol intake, involuntary weight loss, and insomnia sometimes occurs.6,13 The bereaved sometimes have a lack of interest in their own health and tend to socially withdraw.9 This can last for several months after experiencing a loss.6 Because of these conditions, it is important to encourage the patient to get enough exercise and sleep and to eat well and avoid excessive alcohol intake.
Address Social Isolation. Maintaining social interactions can be helpful for patients and should be encouraged. Support groups known as Buddy Groups in the United Kingdom have helped the bereaved be less socially isolated.14
Recognize Complicated Grief. The prevalence of complicated grief is 10% to 20% after the loss of a romantic partner and even higher after the loss of a child.2 This grief can be debilitating and is associated with excessive thoughts about the one who has been lost, prolonged grieving, or difficulty controlling one's emotions. Individuals never truly get over the loss of a loved one, whether that be a spouse, child, parent, or friend; however, emotional intensity of grief abates over time. If it does not, this complicated grief should be addressed.
Regarding the patient in the case scenario, the original reason for the routine follow-up visit is secondary to a more pressing one—that of helping a patient in the midst of a crisis. By reading cues from the patient, the physician could give kind and compassionate support; provide the patient with a handout detailing appropriate websites, books, and support groups; and then schedule a time in a couple of days to write a personal note or to make a phone call. It is incumbent on all physicians to practice the aphorism we learned in medical school: to cure sometimes, to relieve often, to comfort always. This is not always easily done in the face of so many demands as physicians.

