School-aged children (five to 12 years) are establishing patterns of behavior that may last a lifetime; therefore, during health maintenance visits, it is important to counsel families on healthy lifestyle practices. Children should eat a diet high in fruits, vegetables, whole grains, low-fat or nonfat dairy products, beans, fish, and lean meats, while limiting sugar, fast food, and highly processed foods. Children should engage in 60 minutes of moderate to vigorous physical activity each day. A Family Media Use Plan should be used to individualize screen time limits and content for children. Nine to 12 hours of sleep per night is recommended for school-aged children. Inadequate sleep is associated with behavioral issues, difficulty concentrating at school, high blood pressure, and obesity. Children should brush their teeth twice per day with a pea-sized amount of toothpaste containing fluoride. Unintentional injury is the leading cause of death in this age group in the United States, and families should be counseled on vehicle, water, sports, firearm, home, environmental, and social safety. Because high-risk behaviors may start in early adolescence, many experts recommend discussing tobacco, alcohol, and drug use, including prescription drugs, beginning at 11 years of age. Sexually active adolescents should be counseled about the risk of sexually transmitted infections, and they should be screened for these infections if indicated.
Anticipatory guidance is appropriate at all ages, but it is particularly important in school-aged children (five to 12 years) because they are establishing patterns of behavior that may last a lifetime. This article, part II of a two-part series, discusses counseling recommendations in school-aged children. Part I, in this issue of American Family Physician, focuses on history, physical examination, screening, and immunization recommendations.1
SORT: KEY RECOMMENDATIONS FOR PRACTICE
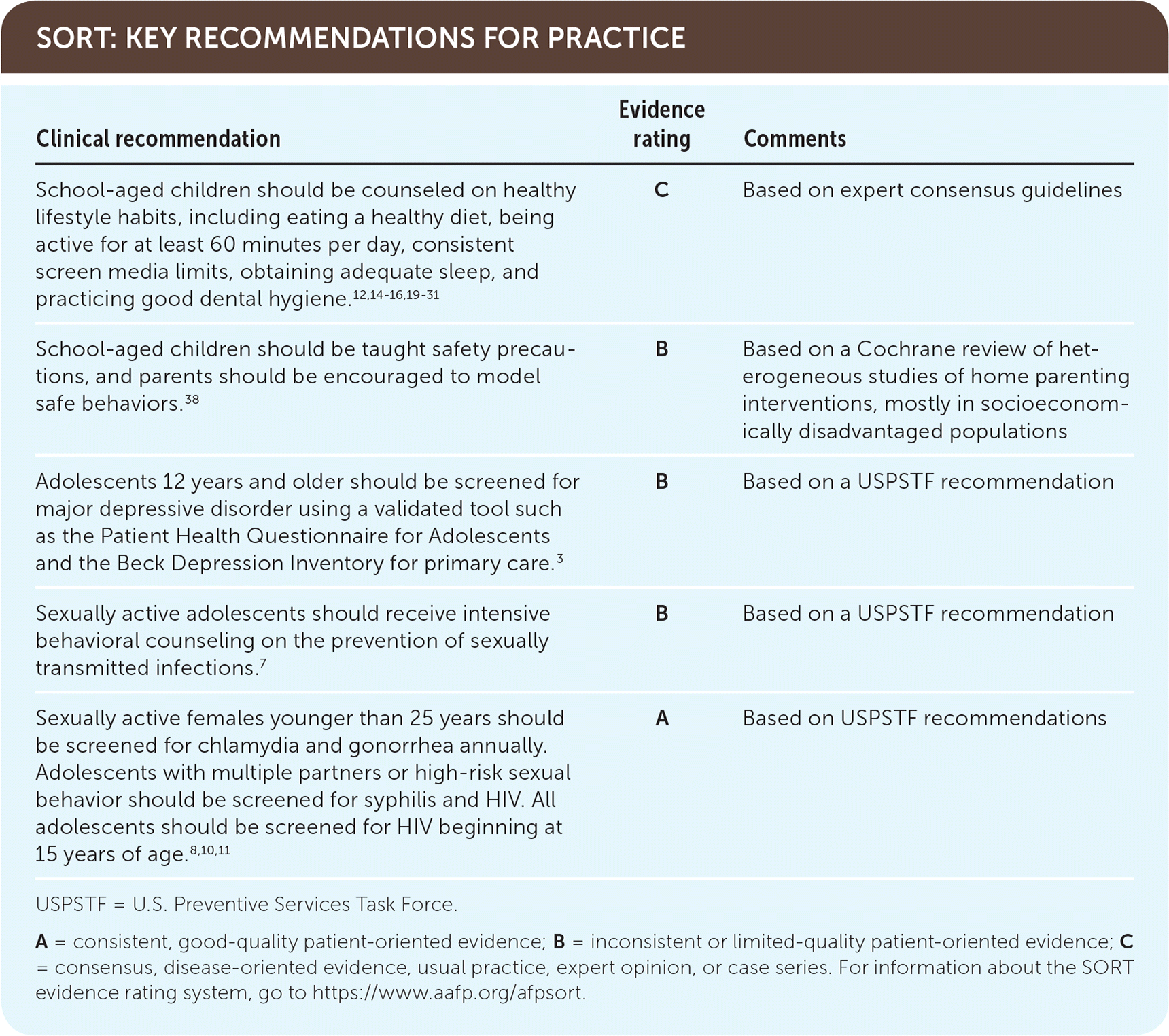
USPSTF = U.S. Preventive Services Task Force.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Families of school-aged children should receive counseling and education to optimize health and wellness, focusing on the issues most relevant to the individual child. School-aged children are concrete thinkers, and counseling should be direct and straightforward. Healthy lifestyle practices and accident prevention should be discussed with all children. The American Academy of Pediatrics (AAP) recommends discussing high-risk behaviors, such as tobacco, alcohol, and drug use, and addressing sexual activity beginning at 11 years of age.2 Physicians may also consider involving school-based health programs. Table 1 lists screening and counseling recommendations for school-aged children and adolescents.2–11
TABLE 1 Screening and Counseling Recommendations for High-Risk Behaviors in School-Aged Children and Adolescents
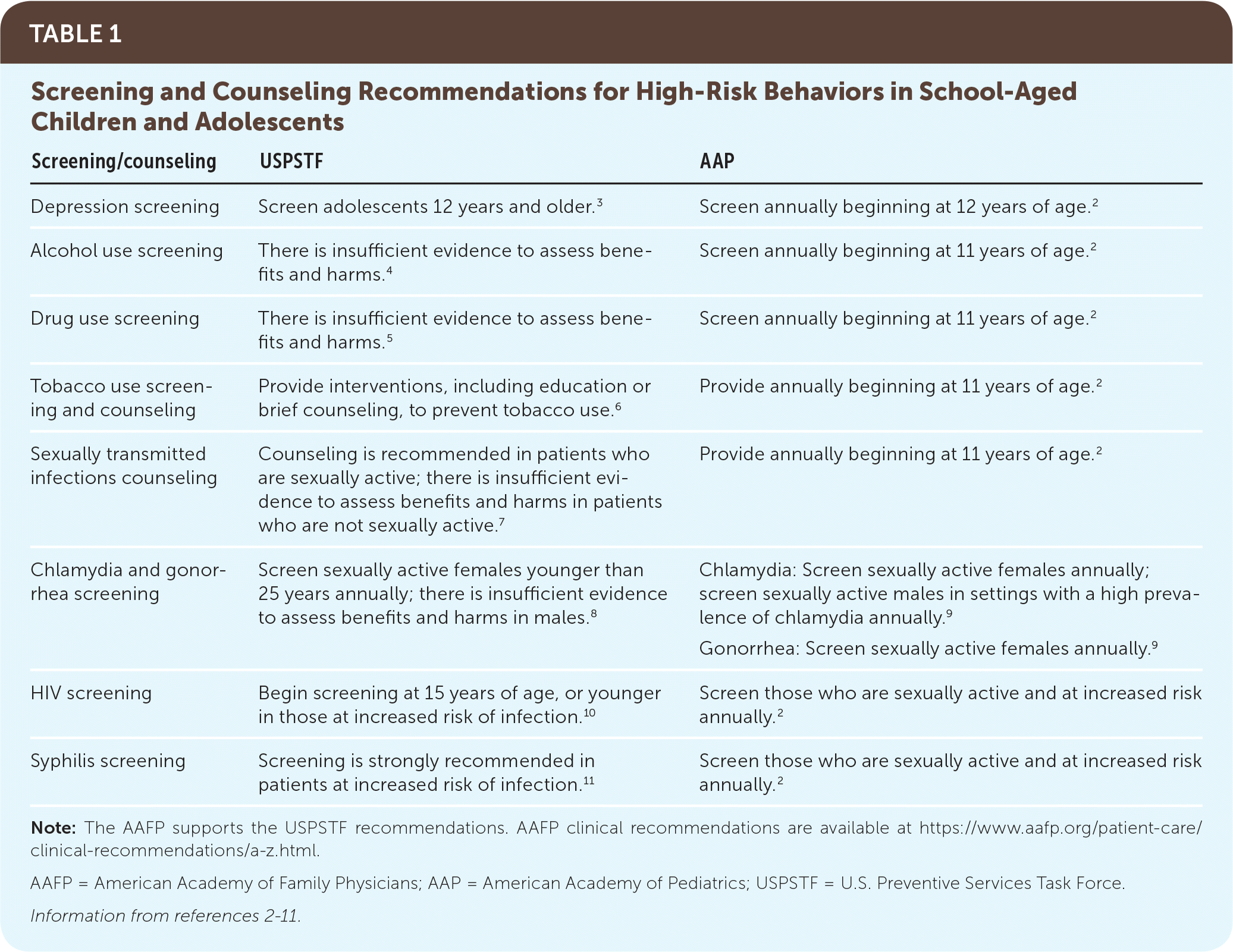
| Screening/counseling | USPSTF | AAP |
|---|---|---|
| Depression screening | Screen adolescents 12 years and older.3 | Screen annually beginning at 12 years of age.2 |
| Alcohol use screening | There is insufficient evidence to assess benefits and harms.4 | Screen annually beginning at 11 years of age.2 |
| Drug use screening | There is insufficient evidence to assess benefits and harms.5 | Screen annually beginning at 11 years of age.2 |
| Tobacco use screening and counseling | Provide interventions, including education or brief counseling, to prevent tobacco use.6 | Provide annually beginning at 11 years of age.2 |
| Sexually transmitted infections counseling | Counseling is recommended in patients who are sexually active; there is insufficient evidence to assess benefits and harms in patients who are not sexually active.7 | Provide annually beginning at 11 years of age.2 |
| Chlamydia and gonorrhea screening | Screen sexually active females younger than 25 years annually; there is insufficient evidence to assess benefits and harms in males.8 | Chlamydia: Screen sexually active females annually; screen sexually active males in settings with a high prevalence of chlamydia annually.9 Gonorrhea: Screen sexually active females annually.9 |
| HIV screening | Begin screening at 15 years of age, or younger in those at increased risk of infection.10 | Screen those who are sexually active and at increased risk annually.2 |
| Syphilis screening | Screening is strongly recommended in patients at increased risk of infection.11 | Screen those who are sexually active and at increased risk annually.2 |
Note: The AAFP supports the USPSTF recommendations. AAFP clinical recommendations are available at https://www.aafp.org/patient-care/clinical-recommendations/a-z.html.
AAFP = American Academy of Family Physicians; AAP = American Academy of Pediatrics; USPSTF = U.S. Preventive Services Task Force.
Health maintenance visits for school-aged children are typically conducted with a parent present. However, sensitive issues, such as substance use and sexual activity, should be discussed without the parent in the room to allow for a sense of privacy. Confidentiality laws should be addressed with the patient and the parent before initiating these discussions to promote open communication.
Healthy Lifestyle
DIETARY COUNSELING
Most experts recommend providing some dietary counseling to children and their families at the health maintenance visit, focusing on maximizing intake of fruits and vegetables, and emphasizing whole grains, lowfat and nonfat dairy products, beans, fish, and lean meats. Families should also be advised to limit sugar, fast food, and highly processed foods, and be educated on appropriate portion sizes.
Table 2 includes American Heart Association dietary counseling recommendations for school-aged children,12 which are endorsed by the AAP. Table 3 provides additional dietary counseling resources for families and physicians, including the Hunger Vital Sign tool to screen for food insecurity.
TABLE 2 Dietary Counseling Recommendations for School-Aged Children

| Balance dietary calories with physical activity to maintain normal growth. |
| Consume low-fat or nonfat (skim) milk and dairy products daily. |
| Consume olive oil, nuts, and other foods low in saturated fat and trans fat. |
| Eat fish, especially oily fish, that is broiled or baked. |
| Eat vegetables and fruits daily, and limit juice intake. |
| Eat whole grain breads and cereals instead of refined grains. |
| Minimize consumption of sugary beverages and foods. |
| Minimize salt intake, including salt from processed foods. |
Adapted with permission from Gidding SS, Dennison BA, Birch LL, et al.; American Heart Association; American Academy of Pediatrics. Dietary recommendations for children and adolescents: a guide for practitioners: consensus statement from the American Heart Association [published corrections appear in Circulation. 2005;112(15):2375, and Circulation. 2006;113(23):e857]. Circulation. 2005;112(13):2062.
TABLE 3 Dietary Counseling Resources for Physicians and Families of School-Aged Children and Adolescents
| American Academy of Pediatrics | |
| http://www.healthychildren.org/english/healthy-living/nutrition/ | |
| Centers for Disease Control and Prevention | |
| https://www.cdc.gov/healthyschools/nutrition/facts.htm | |
| Familydoctor.org | |
| https://familydoctor.org/nutrition-tips-for-kids/ | |
| Harvard School of Public Health | |
| http://www.nutritionsource.org | |
| Hunger Vital Sign | |
| http://childrenshealthwatch.org/public-policy/hunger-vital-sign/ | |
| National Institutes of Health | |
| https://www.niddk.nih.gov/health-information/diet-nutrition | |
| U.S. Department of Agriculture | |
| https://www.choosemyplate.gov/ | |
Although many studies have addressed diet and weight control, few give definitive evidence on how to best advise patients and families. The most effective methods for weight loss in obese children are comprehensive, intensive behavioral interventions composed of more than 26 contact hours of counseling over six months, typically at a specialty center. Less intensive interventions have not been shown to significantly affect weight loss.13
PHYSICAL ACTIVITY
Children should engage in 60 minutes of moderate to vigorous physical activity each day.14,15 Table 4 lists physical activity recommendations from the Physical Activity Guidelines for Americans.15 Play is encouraged for younger children over structured activities, and parents modeling an active lifestyle can be helpful. Community efforts, such as providing children with a safe place to play and emphasizing physical activity at school, may also increase physical activity in children.16
TABLE 4 Physical Activity Recommendations for School-Aged Children and Adolescents

| At least 60 minutes of physical activity per day, including: | |
| Moderate-intensity aerobic activity, such as walking, running, skipping, playing on the playground, playing basketball, and biking, on most days | |
| Vigorous-intensity aerobic activity, such as running, doing jumping jacks, and swimming fast, at least three days per week | |
| Muscle-strengthening activities, such as climbing trees, playing tug-of-war, and doing push-ups and pull-ups, at least three days per week | |
| Bone-strengthening activities, such as hopping, skipping, doing jumping jacks, playing volleyball, and working with resistance bands, at least three days per week | |
Information from reference 15.
SCREEN TIME
Children five to eight years of age spend about two hours watching television and one hour viewing other screens daily.17 Excluding time spent on schoolwork, children eight to 12 years of age have, on average, more than 4.5 hours per day of screen time (e.g., television shows, movies, online videos, video games, social media).18
Increased screen time is adversely associated with obesity, poor sleep quality, depression, myopia, impaired concentration, and academic performance.19–24 Randomized controlled trials have demonstrated that reduction of screen time leads to a lower rate of obesity and less aggression.19,25 Other potential risks of screen media use include exposure to inaccurate information, cyberbullying, and sexual predators, whereas benefits include access to valid educational content and social support communities.26 Social media in particular can have effects on mental health, both positive and negative.27
Recognizing the risks and benefits of screen media use, the AAP issued a 2016 policy statement recommending that screen time be limited to one hour daily for children two to five years of age, and recommending that physicians encourage families to adopt a Family Media Use Plan (online tool available at http://www.healthychildren.org/mediauseplan) for school-aged children.27 A Family Media Use Plan provides guidance to individualize limits on screen time and content and facilitates parental supervision.27 This policy statement replaced the prior AAP recommendation that screen time be limited to two hours daily for children two years and older. The AAP now recommends setting consistent limits, scheduling dedicated screen-free time, and ensuring that media does not interfere with healthy behaviors such as sleep or physical activity. The AAP recommends that screens be kept out of school-aged children's bedrooms for better sleep and that these children not have screen time in the hour before sleep.27
SLEEP
The average school-aged child sleeps 9.4 hours per night, although experts recommend nine to 12 hours per night.28,29 As children age, their sleep needs decrease; therefore, younger school-aged children will need closer to 12 hours and older children closer to nine hours. Physicians should counsel families on sleep recommendations, because inadequate sleep can lead to behavioral issues, difficulty concentrating at school, high blood pressure, and obesity.30,31 Snoring or excessive daytime sleepiness may be a sign of sleep apnea and should prompt further assessment.
DENTAL CARE
School-aged children should have a dental home in addition to a medical home and should see a dentist twice per year for a checkup and cleaning. Sugary foods and beverages should be limited, particularly between meals, and children should brush their teeth twice per day with a pea-sized amount of toothpaste containing fluoride. The AAP also recommends flossing daily as soon as two teeth touch each other.32
SAFETY
Unintentional injury is the leading cause of death for school-aged children in the United States, mainly due to motor vehicle crashes, followed by drowning, firearm fatalities, and fires/burns.33 Falls are the leading cause of nonfatal injury in this age group.34 Effective strategies to prevent falls include parent education and environmental modifications (e.g., adding railings and window guards).35
Firearms are kept in approximately one out of three U.S. households and are stored locked and unloaded in only three out of 10 households with children.36 A recent editorial in American Family Physician (https://www.aafp.org/afp/2018/1101/p560.html) summarizes the evidence showing that counseling and motivational interviewing improve rates of safe gun storage and reduce children's access to firearms.
Most injuries are thought to be preventable and predictable, and outpatient counseling on injury prevention has been shown to decrease injury rates in children.37 School-aged children should be taught safety precautions, and parents should be encouraged to model safe behaviors.38 The AAP recommends counseling families on safety topics (Table 5).27,39–53
TABLE 5 Safety Counseling Recommendations for School-Aged Children and Adolescents

| Environmental Children should use sunscreen with an SPF of 15 or higher when outside.39 |
| Firearm The presence of firearms in the home should be assessed.40 If firearms are kept in the home, they should be securely locked (e.g., using trigger locks or gun safes) and stored separately from ammunition.40 |
| Home Working smoke detectors should be installed on each floor of the home near bedrooms.41,42 Children should be taught predetermined family fire escape plans.41,42 Children should be taught safe behaviors when encountering smoke (stay low and crawl) or fire (stop, drop, and roll).41,42 Carbon monoxide detectors should be installed near sleeping areas.41 |
| Social Parents should monitor their children's internet use.27 Parents should ask children about being bullied.43 Parents should ask about and know their children's friends.43 Children should be taught that other people should not ask to see or touch their private parts or tell them to keep secrets from their parents.43 |
| Sports Appropriate sports-specific safety and protective equipment should be used.44,45 Helmets should be worn for sports such as biking, skiing and snowboarding, horseback riding, skateboarding, and riding a scooter.45–48 |
| Vehicle A booster seat secured with a lap and shoulder seat belt should be used until the child is at least eight years of age and 4 ft, 9 in tall; smaller children may initially need a forward-facing child safety seat with a harness.*49 When a child outgrows the booster seat, a securely fitting lap and shoulder seat belt should be worn.*49 Children younger than 13 years should not ride in the front seat of a motor vehicle.49 No one should ride in the bed of a pickup truck.50 Children younger than 16 years should not drive all-terrain vehicles.51,52 Children should be taught how to safely cross streets.43 |
| Water Children five years and older should learn how to swim.53 Personal flotation devices should be worn during all boating activities.53 Children should have continuous adult supervision near water.53 Pools should be surrounded by a safety fence.53 |
SPF = sun protection factor.
*—Each state has individual laws regarding use of booster seats and when children may begin using adult seat belts.
High-Risk Behaviors
DEPRESSION
Depression can contribute to safety issues and risk-taking behaviors. The U.S. Preventive Services Task Force (USPSTF) recommends screening for major depressive disorder in adolescents 12 years and older. Recommended validated screening tools for depression in adolescents include the Patient Health Questionnaire for Adolescents and the Beck Depression Inventory for primary care. The USPSTF concludes that there is insufficient evidence to assess the benefits and harms of depression screening in children 11 years and younger.3
TOBACCO, ALCOHOL, AND DRUG USE
Tobacco, alcohol, and illicit drug use may begin in early adolescence. According to a 2017 survey of youth in the United States, 16% of those younger than 13 years had tried alcohol, 10% had tried a cigarette, and 7% had tried marijuana.54 There are no specific data on vaping or e-cigarettes before 13 years of age, although teenagers are more likely to use e-cigarettes than cigarettes.55 A 2016 survey showed that 3.5% of those 12 to 17 years of age misused prescription pain relievers; a friend or relative was usually the source of the medication.56 Although there are no specific guidelines for counseling about prescription and nonprescription drug abuse in school-aged children, physicians should consider both as drugs of potential abuse. Early alcohol and substance abuse increases the risk of unintentional injuries, motor vehicle crashes, and substance abuse and dependence in adulthood.57
The USPSTF recommends interventions, including education or brief counseling, for prevention of tobacco use but concludes that there is insufficient evidence to assess the benefits and harms of physician counseling for avoidance of alcohol and illicit drugs.4–6 The American Academy of Family Physicians supports the USPSTF recommendations58 but recognizes that avoidance of tobacco, alcohol, and illicit drugs in adolescents is desirable.59 The AAP recommends asking adolescents directly about tobacco (including smokeless tobacco), alcohol, and drug use as part of an age-appropriate comprehensive history starting at 11 years of age.2 If the patient reports substance use, additional questioning about duration, amount, and frequency is appropriate.
The CRAFFT questionnaire is one brief screening tool that has been validated in the primary care setting to screen for substance abuse in adolescents60:
- Car: Have you ever ridden in a car driven by someone who was “high” or had been using alcohol or drugs?
- Relax: Do you ever use alcohol or drugs to relax, feel better about yourself, or fit in?
- Alone: Do you ever use alcohol or drugs when you are by yourself, or alone?
- Forget: Do you ever forget things you did while you were using alcohol or drugs?
- Family or friends: Do family or friends ever tell you that you should cut down on your drinking or drug use?
- Trouble: Have you ever gotten into trouble while you were using alcohol or drugs?
At least two “yes” answers should prompt concern for substance abuse or dependence. A downloadable form is available at https://bit.ly/30sxNp5.
SEXUAL ACTIVITY
Family physicians should consider screening early adolescents for sexual activity. More than 3% of youths in the United States are sexually active before 13 years of age, and this is even more common in those who identify as gay, lesbian, and bisexual.54 Sexual activity between an adolescent and a partner who is at least three years older is considered statutory rape in many states and is a reportable offense even if it is consensual.61 In many states, discussions of contraception and sexually transmitted infection diagnosis and treatment between physicians and patients 12 years and older are protected under confidentiality laws.62 Physicians need to be aware of their own state laws governing sexual activity in adolescents. The Rape, Abuse, and Incest National Network provides a useful online reference (https://www.rainn.org/about-sexual-assault).
All sexually active adolescents are at risk of sexually transmitted infections. Therefore, the USPSTF recommends that these patients receive intensive behavioral counseling on prevention.7,63 Although there is insufficient evidence to recommend for or against counseling for adolescents who are not sexually active, the USPSTF found no good evidence that counseling in these patients caused inadvertent harm or increased sexual activity.7,63
Sexually active females younger than 25 years should be screened for chlamydia and gonorrhea annually.8 Because cervical cancer screening is not recommended until 21 years of age, chlamydia and gonorrhea screening in female adolescents can be performed using urine testing, which does not include a pelvic examination.64 Adolescents with multiple partners or high-risk sexual behavior should be screened for HIV infection and syphilis.10,11,63 All adolescents should be screened for HIV infection beginning at 15 years of age.10,63
This article updates a previous article on this topic by Riley, et al.65
Data Sources: A PubMed search was performed using the key terms well child, health maintenance, prevention, children, and pediatrics and various other terms as relevant to topics. The search included meta-analyses, randomized controlled and other clinical trials, systematic reviews, and national evidence-based guidelines. We also searched relevant POEMs, Cochrane reviews, and Essential Evidence Plus, including a review of the evidence referenced in those publications. Search dates: July 2018 to May 2019.

