A seven-year-old boy presented with abnormal growth of his fingernails that began two weeks prior. He had no other symptoms, including pain or pruritus on his hands or around his nails. He did not have fevers, chills, nausea, vomiting, or change in activity. He had hand-foot-and-mouth disease two months earlier that was diagnosed based on vesicular lesions in his mouth and on his hands and feet. The lesions completely resolved, and his mother reported that he returned to normal activity.
On physical examination, the patient appeared well and active. The nails on both hands were discolored and looked like they were peeling (Figure 1 and Figure 2). He had no other skin lesions, and the rest of the physical examination was unremarkable.
FIGURE 1
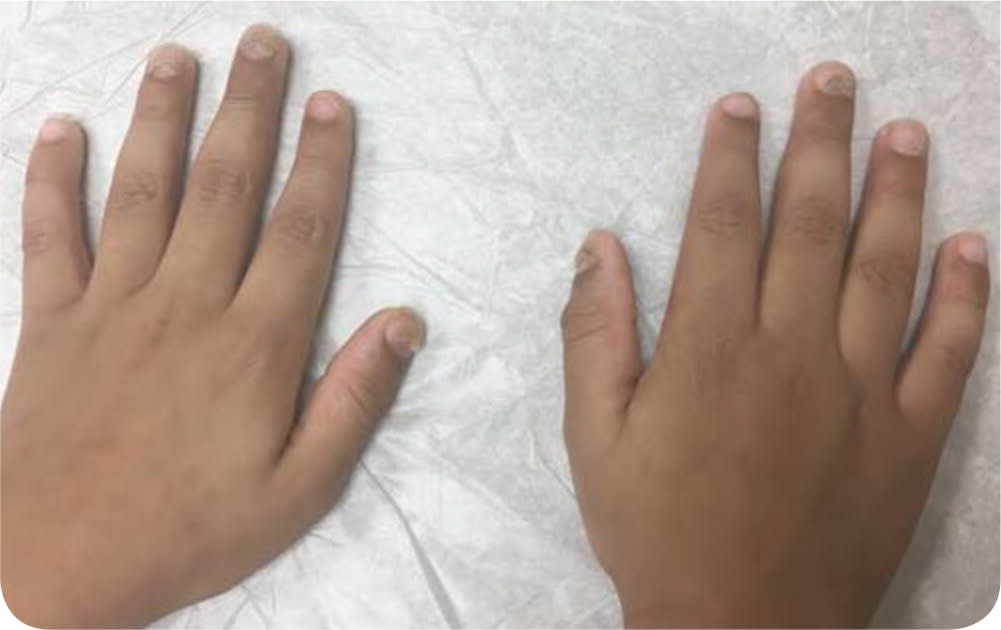
FIGURE 2
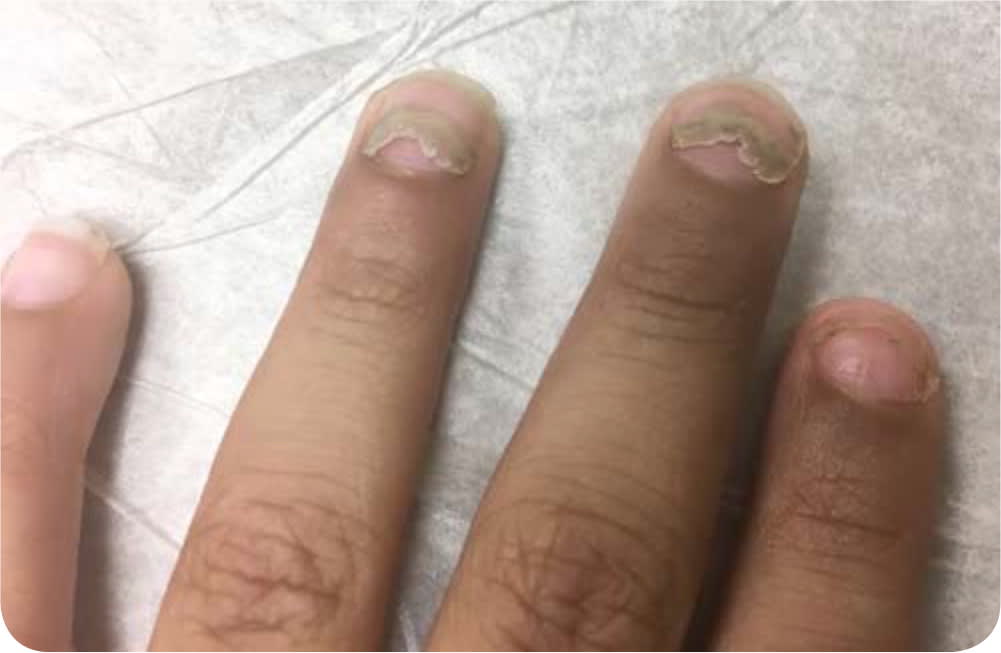
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Child abuse.
B. Onycholysis.
C. Onychomadesis.
D. Onychomycosis.
E. Pathologic grooming.
Discussion
The answer is C: onychomadesis. Onychomadesis is a phenomenon in which the nail plate separates from the nail bed because of cessation of activity in the nail matrix, usually followed by incomplete shedding of the nail.1 Onychomadesis can develop 28 to 56 days after hand-foot-and-mouth disease, which is most often caused by Coxsackie virus infection.2 Changes in the nails are not permanent, and normal nail growth typically occurs within one to four months.2 The characteristic disruption of the nail plate and proximal nail bed gives the nails a peeling appearance.
Nail abnormalities during childhood are generally uncommon.2 Other causes of onychomadesis include trauma or injury, systemic disease, infection, drug use, radiation, and chemotherapy.1–3 Onychomadesis following hand-foot-and-mouth disease can occur on the nails of the hands or feet, even on digits not affected by the illness. In this patient, the previous diagnosis within the appropriate time frame makes onychomadesis the most likely diagnosis.
It is important to maintain child abuse in the differential diagnosis of any injury to a child. Suspicion should be higher if the history provided does not explain the child's injury or is inconsistent among guardians, there is delay in seeking treatment, or the child has multiple injuries in different stages of healing.4
Onycholysis is the separation of the nail from the nail bed with subsequent colonization of the nail space by environmental flora such as Candida albicans.5 Causes of onycholysis include trauma, manicures, and occupational or self-induced behavior.5 It may occur with diseases such as psoriasis.5 Onycholysis usually starts at the distal end of the nail or the sides and not the proximal nail bed.
Onychomycosis is an infection of the nail, usually caused by a dermatophyte, that affects about 10% of the U.S. population.6 Onychomycosis is not life-threatening but can cause pain and negatively affect quality of life.6 Onychomycosis usually leads to thickened, discolored, brittle nails, but the nails do not separate from the nail bed.
Pathologic grooming includes excessive hair pulling (trichotillomania), skin picking (dermatillomania), nail biting (onychophagia), and nail picking (onychotillomania). Nail picking is not as well studied as other body-focused repetitive behavior disorders.7 Pathologic grooming causes significant impairment in quality of life and may be associated with a psychological disorder.5 With nail picking or biting, there is usually damage to the surrounding skin, and most nails are affected, making this a less likely diagnosis for this patient.
SUMMARY TABLE
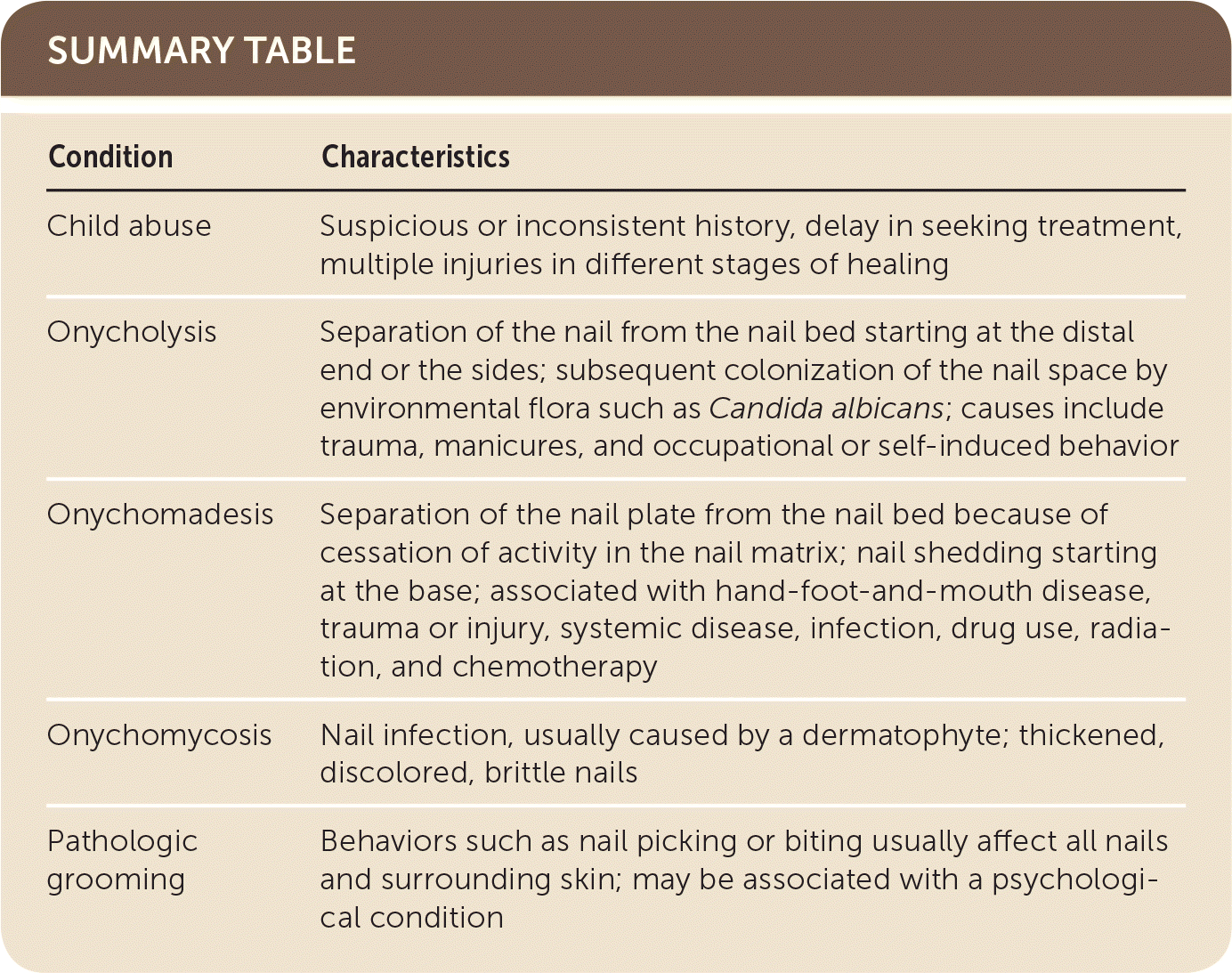
| Condition | Characteristics |
|---|---|
| Child abuse | Suspicious or inconsistent history, delay in seeking treatment, multiple injuries in different stages of healing |
| Onycholysis | Separation of the nail from the nail bed starting at the distal end or the sides; subsequent colonization of the nail space by environmental flora such as Candida albicans; causes include trauma, manicures, and occupational or self-induced behavior |
| Onychomadesis | Separation of the nail plate from the nail bed because of cessation of activity in the nail matrix; nail shedding starting at the base; associated with hand-foot-and-mouth disease, trauma or injury, systemic disease, infection, drug use, radiation, and chemotherapy |
| Onychomycosis | Nail infection, usually caused by a dermatophyte; thickened, discolored, brittle nails |
| Pathologic grooming | Behaviors such as nail picking or biting usually affect all nails and surrounding skin; may be associated with a psychological condition |

