Key Clinical Issue
Does the use of telehealth for outpatients requiring subspecialty consultations improve clinical outcomes, reduce costs, or increase patient satisfaction?
Evidence-Based Answer
Telehealth consultations improve clinical outcomes in the areas of wound care, psychiatry, and certain chronic conditions. (Strength of recommendation [SOR]: B, based on inconsistent or limited-quality patient-oriented evidence.) Telehealth may increase patient satisfaction and may reduce cost and health care utilization. (SOR: B, based on inconsistent or limited-quality patient-oriented evidence.) There is insufficient evidence regarding potential harms of telehealth.1
CLINICAL BOTTOM LINE Outpatient Care Telehealth Consultations: Strength of Evidence
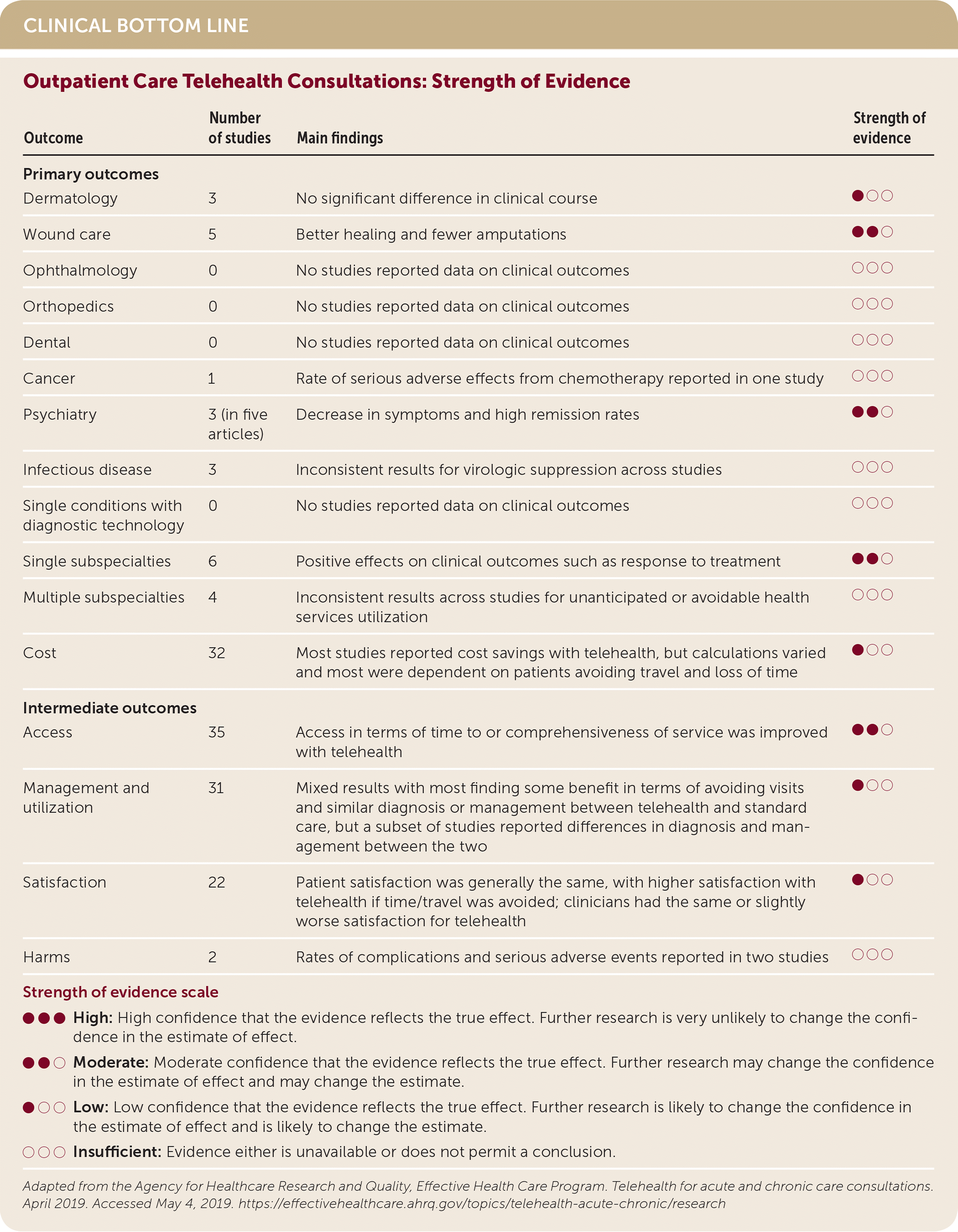
| Outcome | Number of studies | Main findings | Strength of evidence |
|---|---|---|---|
| Primary outcomes | |||
| Dermatology | 3 | No significant difference in clinical course | ● ○ ○ |
| Wound care | 5 | Better healing and fewer amputations | ● ● ○ |
| Ophthalmology | 0 | No studies reported data on clinical outcomes | ○ ○ ○ |
| Orthopedics | 0 | No studies reported data on clinical outcomes | ○ ○ ○ |
| Dental | 0 | No studies reported data on clinical outcomes | ○ ○ ○ |
| Cancer | 1 | Rate of serious adverse effects from chemotherapy reported in one study | ○ ○ ○ |
| Psychiatry | 3 (in five articles) | Decrease in symptoms and high remission rates | ● ● ○ |
| Infectious disease | 3 | Inconsistent results for virologic suppression across studies | ○ ○ ○ |
| Single conditions with diagnostic technology | 0 | No studies reported data on clinical outcomes | ○ ○ ○ |
| Single subspecialties | 6 | Positive effects on clinical outcomes such as response to treatment | ● ● ○ |
| Multiple subspecialties | 4 | Inconsistent results across studies for unanticipated or avoidable health services utilization | ○ ○ ○ |
| Cost | 32 | Most studies reported cost savings with telehealth, but calculations varied and most were dependent on patients avoiding travel and loss of time | ● ○ ○ |
| Intermediate outcomes | |||
| Access | 35 | Access in terms of time to or comprehensiveness of service was improved with telehealth | ● ● ○ |
| Management and utilization | 31 | Mixed results with most finding some benefit in terms of avoiding visits and similar diagnosis or management between telehealth and standard care, but a subset of studies reported differences in diagnosis and management between the two | ● ○ ○ |
| Satisfaction | 22 | Patient satisfaction was generally the same, with higher satisfaction with telehealth if time/travel was avoided; clinicians had the same or slightly worse satisfaction for telehealth | ● ○ ○ |
| Harms | 2 | Rates of complications and serious adverse events reported in two studies | ○ ○ ○ |
Strength of evidence scale
● ● ● High: High confidence that the evidence reflects the true effect. Further research is very unlikely to change the confidence in the estimate of effect.
● ● ○ Moderate: Moderate confidence that the evidence reflects the true effect. Further research may change the confidence in the estimate of effect and may change the estimate.
● ○ ○ Low: Low confidence that the evidence reflects the true effect. Further research is likely to change the confidence in the estimate of effect and is likely to change the estimate.
○ ○ ○Insufficient: Evidence either is unavailable or does not permit a conclusion.
Adapted from the Agency for Healthcare Research and Quality, Effective Health Care Program. Telehealth for acute and chronic care consultations. April 2019. Accessed May 4, 2019. https://effectivehealthcare.ahrq.gov/topics/telehealth-acute-chronic/research
Practice Pointers
For the purposes of this Agency for Healthcare Research and Quality (AHRQ) review, telehealth was defined as the use of information and telecommunications technology in health care delivery for a specific patient or group of patients that involves collaboration with a health care professional across distance or time to address a diagnosis, health condition, or the overarching needs of a patient.1 Telehealth has expanded in scope and scale in recent years, challenging traditional models of everything from health care delivery and reimbursement to ethics.2,3 Slow adoption of telehealth may be due to concerns about adverse outcomes and discrepancies in diagnosis and management between telehealth and in-person consultations. Other concerns for family physicians include lack of training, reimbursement, and liability issues.4
Research on the outcomes associated with telehealth is nascent but rapidly emerging. This AHRQ review included 106 studies evaluating telehealth for consultations in the outpatient setting. Studies compared telehealth with face-to-face consultation, telephone consultation, or no subspecialty consultation.
For some clinical outcomes, there was enough evidence to assess the effectiveness of telehealth. Five studies with moderate strength of evidence concluded that telehealth leads to better wound healing and fewer amputations. Three studies with moderate strength of evidence concluded that telehealth leads to decreased psychiatric symptoms and higher remission rates. However, three studies evaluating various aspects of patient recovery in those with dermatologic conditions showed no significant differences in clinical outcomes.
Telehealth had positive effects on chronic disease clinical outcomes in six studies with moderate strength of evidence. These studies focused on a single subspecialty and found positive responses to treatment in conditions such as diabetes mellitus, arthritis, hypertension, and chronic pain. These studies were generally small and mostly compared telehealth with face-to-face consultations.
A total of 35 studies with moderate strength of evidence found that telehealth improves access in terms of time to service and comprehensiveness of service. These studies showed reduced wait times, reduced time to treatment, and an increase in the number of patients receiving indicated diagnostic tests or treatments. Although these outcomes are desirable, they do not necessarily correlate with improved clinical outcomes. Telehealth reduced the numbers of in-person subspecialist visits, hospital visits, hospital admissions, and length of hospitalizations in most of the 31 studies with low strength of evidence.
According to 22 studies with low strength of evidence, patients may be more satisfied with telehealth than face-to-face encounters, especially if it saved the patient time and travel. However, differences were rarely statistically significant, calling this conclusion into question. In the same group of studies, clinician satisfaction was the same or slightly worse than for face-to-face clinical encounters.
Most studies that examined cost reported savings with telehealth. The 32 studies were graded as having a low strength of evidence because of inconsistency in calculations of patient travel and loss of time across studies.
There is insufficient evidence on complications and adverse events in telehealth. In the two studies reporting harms, there were lower complication rates with telehealth. One of these studies found fewer cancer complications and the other found fewer adverse events related to hepatitis C treatment. The exact mechanism by which harms were reduced in these studies is not clear. The authors pointed out that the overall lack of harms shown in the studies could be due to the relatively short follow-up intervals in most outpatient studies of telehealth.
The American Academy of Family Physicians' definition of telemedicine is similar to the one used in this review for telehealth: “the practice of medicine using technology to deliver care at a distance, over a telecommunications infrastructure, between a patient at an originating (spoke) site and a physician, or other practitioner licensed to practice medicine, at a distant (hub) site.”5 However, this review is limited to consultations among practitioners and does not include the use of telehealth to provide care directly to patients.
This AHRQ review supports the use of telehealth for selected clinical circumstances such as psychiatry and wound care. Evidence is limited for cost savings and patient satisfaction. Additional multisite studies are needed to better understand the overall impact on the U.S. health care system. As technology continues to evolve at a rapid pace, most existing literature on telehealth will quickly become antiquated and new evidence will need to be generated.
Editor's Note:American Family Physician SOR ratings are different from the AHRQ Strength of Evidence ratings. Dr.Seehusen is an assistant medical editor for AFP.

