A 44-year-old woman with a 30-pack-year smoking history presented with blisters on the sole of her foot that appeared one month prior. She noticed that the skin on her feet had thickened and had dark brown spots, small pustules, and areas of scale throughout. She had no itching or pain. There was no improvement after two four-week courses of topical clotrimazole and naftifine (Naftin). She subsequently developed a similar rash on the palm of her hand.
Examination showed a well-demarcated rash on the sole of the left foot (Figure 1). Results of potassium hydroxide testing were negative.
FIGURE 1
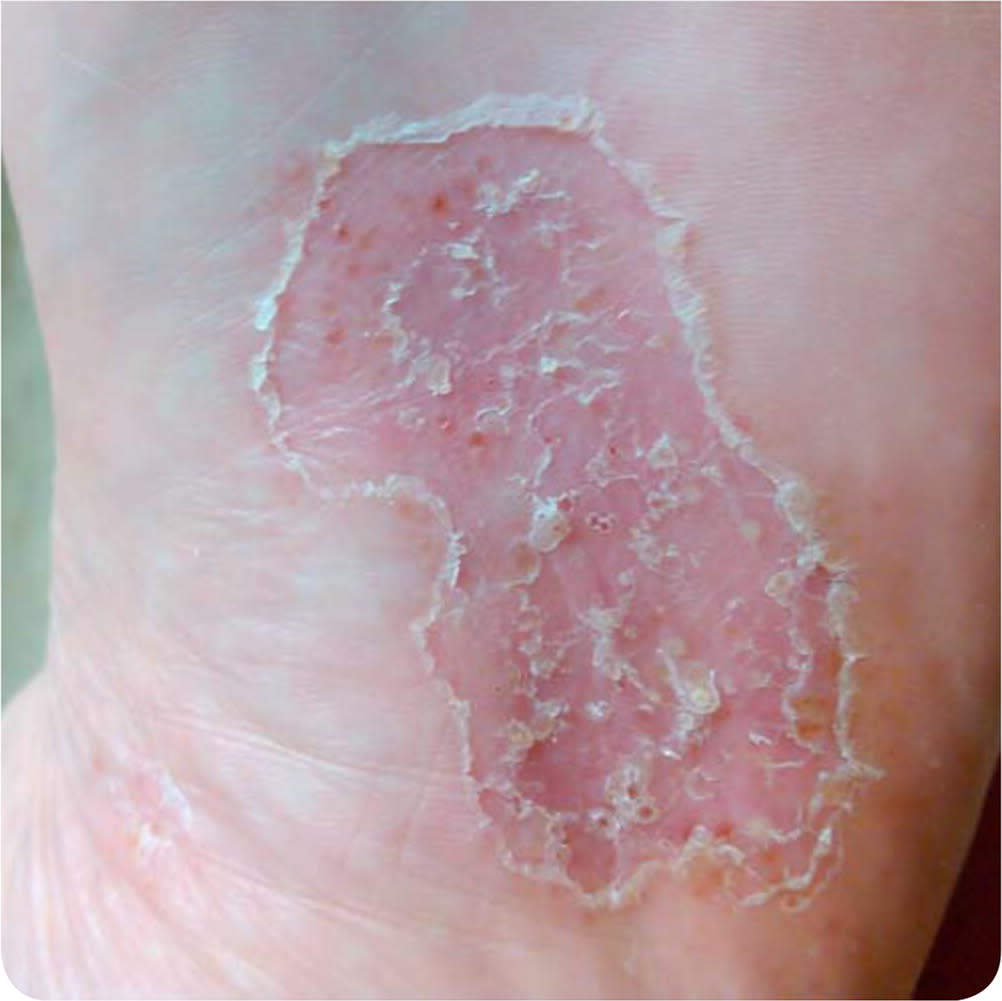
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Allergic dermatitis.
B. Bullous tinea pedis.
C. Dyshidrotic eczema.
D. Palmoplantar pustulosis.
E. Pitted keratolysis.
Discussion
The answer is D: palmoplantar pustulosis. This chronic inflammatory skin disease is characterized by sterile pustules and red, scaly skin on the palms and soles. The pustules typically erupt and progress to yellow-brown macules. Hyperkeratosis, scaling, and fissures are also common. The condition occurs mostly in middle-aged adults and has a strong association with smoking. Other risk factors include thyroid disease, stress, medication use (i.e., tumor necrosis factor alpha inhibitors), and streptococcal infections. Metal allergies can exacerbate the condition.1,2 Palmoplantar pustulosis may have a considerable effect on quality of life because burning, pain, and pruritus may lead to difficulty with walking and activities of daily living.3 The condition is also known as pustular psoriasis. Although the relationship of palmoplantar pustulosis to psoriasis is unclear, some regard it as a manifestation of psoriasis.1,2
The diagnosis of palmoplantar pustulosis can be made clinically. A skin biopsy is not usually necessary but can confirm the diagnosis.2 A potassium hydroxide test of the roof of blisters (not merely a scraping of the overlying skin) should be performed to rule out cutaneous fungal infection.
Treatment includes high-potency topical steroids, oral retinoids, calcipotriene (Dovonex), and photochemotherapy. Second-line agents include immunosuppressants such as cyclosporine (Sandimmune) and methotrexate. Adjunctive therapies include skin moisturization, avoidance of irritants, and smoking cessation.2
Allergic contact dermatitis usually presents as an intensely pruritic rash in response to an allergen exposure.4
Bullous tinea pedis classically affects the instep of the foot. It is characterized by a pruritic, sometimes painful, vesicular or bullous eruption with underlying erythema. A potassium hydroxide test of the roof of blisters (full-thickness) should be performed.4
Dyshidrotic eczema typically presents as multiple tiny vesicles on the lateral aspect of the digits. Erythema and intense pruritus may occur.4
Pitted keratolysis is a superficial bacterial skin infection confined to the pressure-bearing areas of the feet. It is characterized by profound malodor and clusters of brownish “punched-out” pits.4
SUMMARY TABLE
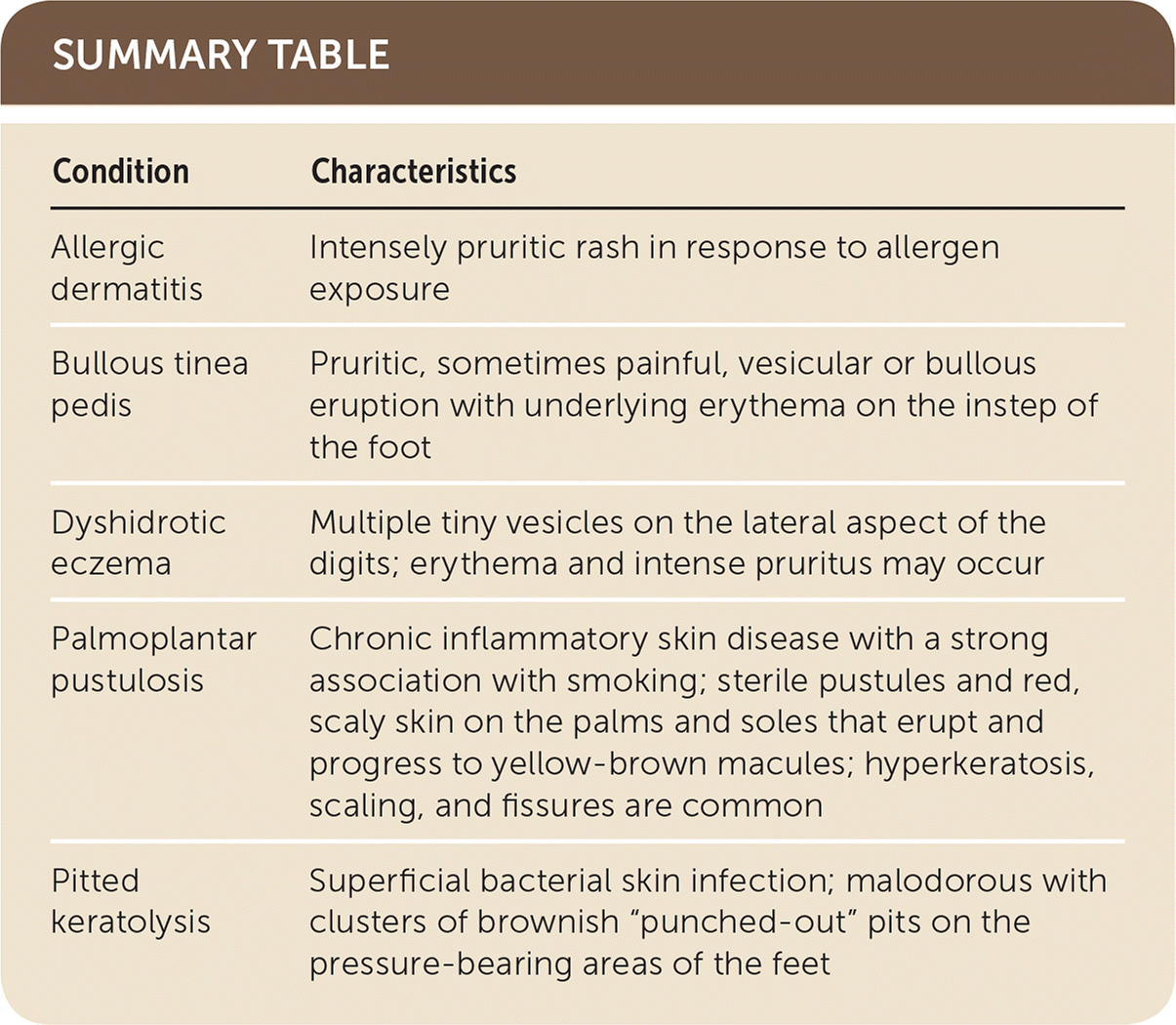
| Condition | Characteristics |
|---|---|
| Allergic dermatitis | Intensely pruritic rash in response to allergen exposure |
| Bullous tinea pedis | Pruritic, sometimes painful, vesicular or bullous eruption with underlying erythema on the instep of the foot |
| Dyshidrotic eczema | Multiple tiny vesicles on the lateral aspect of the digits; erythema and intense pruritus may occur |
| Palmoplantar pustulosis | Chronic inflammatory skin disease with a strong association with smoking; sterile pustules and red, scaly skin on the palms and soles that erupt and progress to yellow-brown macules; hyperkeratosis, scaling, and fissures are common |
| Pitted keratolysis | Superficial bacterial skin infection; malodorous with clusters of brownish “punched-out” pits on the pressure-bearing areas of the feet |
The views expressed in this article are those of the authors and do not necessarily reflect the official policy or position of the Department of the Navy, the Department of Defense, or the U.S. government.

