Summary of Recommendations
The USPSTF recommends 1-time screening for abdominal aortic aneurysm (AAA) with ultrasonography in men aged 65 to 75 years who have ever smoked (Table 1). B recommendation.
TABLE 1. Screening for AAA: Clinical Summary of the USPSTF Recommendation
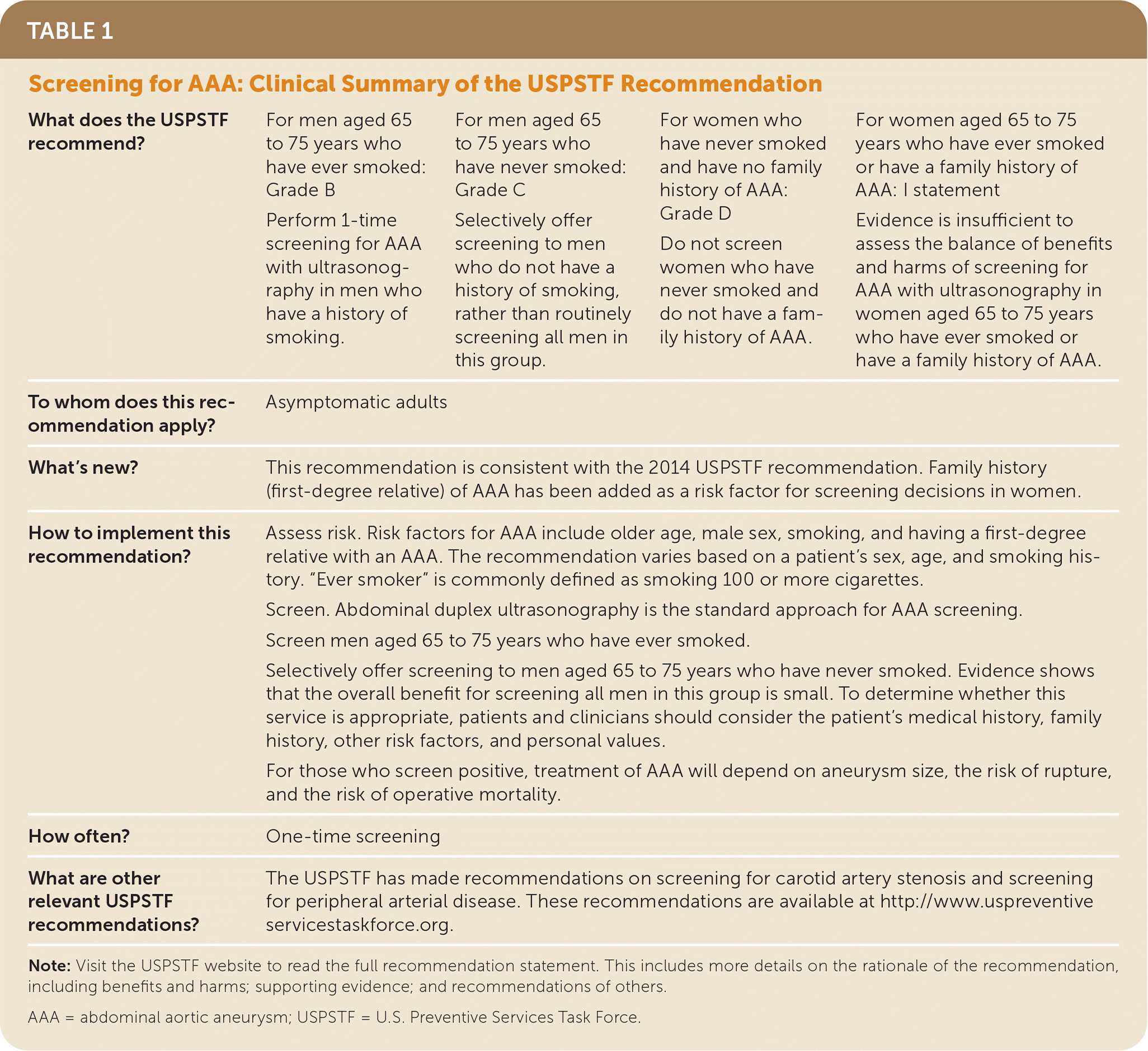
| What does the USPSTF recommend? | For men aged 65 to 75 years who have ever smoked: Grade B Perform 1-time screening for AAA with ultrasonography in men who have a history of smoking. | For men aged 65 to 75 years who have never smoked: Grade C Selectively offer screening to men who do not have a history of smoking, rather than routinely screening all men in this group. | For women who have never smoked and have no family history of AAA: Grade D Do not screen women who have never smoked and do not have a family history of AAA. | For women aged 65 to 75 years who have ever smoked or have a family history of AAA: I statement Evidence is insufficient to assess the balance of benefits and harms of screening for AAA with ultrasonography in women aged 65 to 75 years who have ever smoked or have a family history of AAA. |
| To whom does this recommendation apply? | Asymptomatic adults | |||
| What's new? | This recommendation is consistent with the 2014 USPSTF recommendation. Family history (first-degree relative) of AAA has been added as a risk factor for screening decisions in women. | |||
| How to implement this recommendation? | Assess risk. Risk factors for AAA include older age, male sex, smoking, and having a first-degree relative with an AAA. The recommendation varies based on a patient's sex, age, and smoking history. “Ever smoker” is commonly defined as smoking 100 or more cigarettes. Screen. Abdominal duplex ultrasonography is the standard approach for AAA screening. Screen men aged 65 to 75 years who have ever smoked. Selectively offer screening to men aged 65 to 75 years who have never smoked. Evidence shows that the overall benefit for screening all men in this group is small. To determine whether this service is appropriate, patients and clinicians should consider the patient's medical history, family history, other risk factors, and personal values. For those who screen positive, treatment of AAA will depend on aneurysm size, the risk of rupture, and the risk of operative mortality. | |||
| How often? | One-time screening | |||
| What are other relevant USPSTF recommendations? | The USPSTF has made recommendations on screening for carotid artery stenosis and screening for peripheral arterial disease. These recommendations are available at http://www.uspreventiveservicestaskforce.org. | |||
Note: Visit the USPSTF website to read the full recommendation statement. This includes more details on the rationale of the recommendation, including benefits and harms; supporting evidence; and recommendations of others.
AAA = abdominal aortic aneurysm; USPSTF = U.S. Preventive Services Task Force.
The USPSTF recommends that clinicians selectively offer screening for AAA with ultrasonography in men aged 65 to 75 years who have never smoked rather than routinely screening all men in this group. Evidence indicates that the net benefit of screening all men in this group is small. In determining whether this service is appropriate in individual cases, patients and clinicians should consider the balance of benefits and harms on the basis of evidence relevant to the patient's medical history, family history, other risk factors, and personal values. C recommendation.
The USPSTF recommends against routine screening for AAA with ultrasonography in women who have never smoked and have no family history of AAA. D recommendation.
The USPSTF concludes that the current evidence is insufficient to assess the balance of benefits and harms of screening for AAA with ultrasonography in women aged 65 to 75 years who have ever smoked or have a family history of AAA. I statement.
See the “Practice Considerations” section for more information on each of these populations.
Importance
An AAA is typically defined as aortic enlargement with a diameter of 3.0 cm or larger. The prevalence of AAA has declined over the past 2 decades among screened men 65 years or older in various countries such as the United Kingdom, New Zealand, Sweden, and Denmark.1–10 Population-based studies in men older than 60 years have found an AAA prevalence ranging from 1.2% to 3.3%.1–10 The reduction in prevalence is attributed to the decrease in smoking prevalence over time. Previous prevalence rates of AAA reported in population-based screening studies ranged from 1.6% to 7.2% of the general population 60 to 65 years or older.1 The current prevalence of AAA in the United States is unclear because of the low uptake of screening.1 Most AAAs are asymptomatic until they rupture. Although the risk for rupture varies greatly by aneurysm size, the associated risk for death with rupture is as high as 81%.1,11
USPSTF Assessment of Magnitude of Net Benefit
The USPSTF concludes with moderate certainty that screening for AAA in men aged 65 to 75 years who have ever smoked is of moderate net benefit (Table 1 and Table 2).
TABLE 2. Summary of USPSTF Rationale
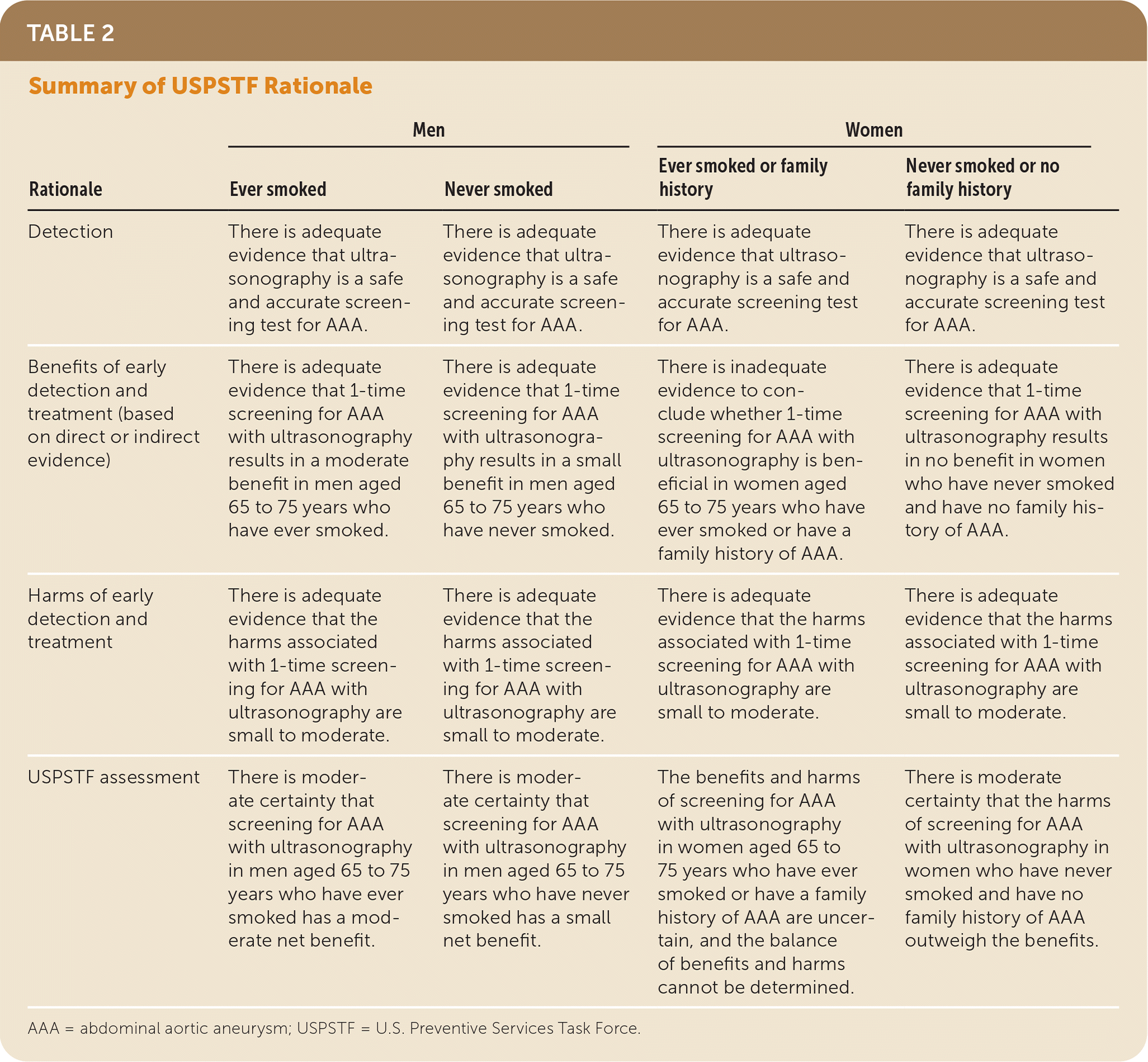
| Rationale | Men | Women | ||
|---|---|---|---|---|
| Ever smoked | Never smoked | Ever smoked or family history | Never smoked or no family history | |
| Detection | There is adequate evidence that ultrasonography is a safe and accurate screening test for AAA. | There is adequate evidence that ultrasonography is a safe and accurate screening test for AAA. | There is adequate evidence that ultrasonography is a safe and accurate screening test for AAA. | There is adequate evidence that ultrasonography is a safe and accurate screening test for AAA. |
| Benefits of early detection and treatment (based on direct or indirect evidence) | There is adequate evidence that 1-time screening for AAA with ultrasonography results in a moderate benefit in men aged 65 to 75 years who have ever smoked. | There is adequate evidence that 1-time screening for AAA with ultrasonography results in a small benefit in men aged 65 to 75 years who have never smoked. | There is inadequate evidence to conclude whether 1-time screening for AAA with ultrasonography is beneficial in women aged 65 to 75 years who have ever smoked or have a family history of AAA. | There is adequate evidence that 1-time screening for AAA with ultrasonography results in no benefit in women who have never smoked and have no family history of AAA. |
| Harms of early detection and treatment | There is adequate evidence that the harms associated with 1-time screening for AAA with ultrasonography are small to moderate. | There is adequate evidence that the harms associated with 1-time screening for AAA with ultrasonography are small to moderate. | There is adequate evidence that the harms associated with 1-time screening for AAA with ultrasonography are small to moderate. | There is adequate evidence that the harms associated with 1-time screening for AAA with ultrasonography are small to moderate. |
| USPSTF assessment | There is moderate certainty that screening for AAA with ultrasonography in men aged 65 to 75 years who have ever smoked has a moderate net benefit. | There is moderate certainty that screening for AAA with ultrasonography in men aged 65 to 75 years who have never smoked has a small net benefit. | The benefits and harms of screening for AAA with ultrasonography in women aged 65 to 75 years who have ever smoked or have a family history of AAA are uncertain, and the balance of benefits and harms cannot be determined. | There is moderate certainty that the harms of screening for AAA with ultrasonography in women who have never smoked and have no family history of AAA outweigh the benefits. |
AAA = abdominal aortic aneurysm; USPSTF = U.S. Preventive Services Task Force.
The USPSTF concludes with moderate certainty that screening for AAA in men aged 65 to 75 years who have never smoked is of small net benefit(Table 1 and Table 2).
The USPSTF concludes that the evidence is insufficient to determine the net benefit of screening for AAA in women aged 65 to 75 years who have ever smoked or have a family history of AAA (Table 1 and Table 2).
The USPSTF concludes with moderate certainty that the harms of screening for AAA in women aged 65 to 75 years who have never smoked and have no family history of AAA outweigh the benefits(Table 1 and Table 2).
For more details on the methods the USPSTF uses to determine the net benefit, see the USPSTF Procedure Manual.12
Practice Considerations
PATIENT POPULATION UNDER CONSIDERATION
Based on the scope of the evidence review, this recommendation applies to asymptomatic adults 50 years or older. However, the randomized trial evidence focuses almost entirely on men aged 65 to 75 years. In this Recommendation Statement, the recommendations are stratified by “men” and “women,” although the net benefit estimates are driven by biologic sex (i.e., male/female) rather than gender identity. Persons should consider their sex at birth to determine which recommendation best applies to them.
ASSESSMENT OF RISK
Important risk factors for AAA include older age, male sex, smoking, and having a first-degree relative with an AAA.13–16 Other risk factors include a history of other vascular aneurysms, coronary artery disease, cerebrovascular disease, atherosclerosis, hypercholesterolemia, and hypertension.17–19 Factors associated with a reduced risk include African American race, Hispanic ethnicity, Asian ethnicity, and diabetes.13,20–24 Risk factors for AAA rupture include older age, female sex, smoking, and elevated blood pressure.1 Clinicians should consider the presence of comorbid conditions and not offering screening if patients are unable to undergo surgical intervention or have a reduced life expectancy.
Smoking Status. Epidemiologic literature commonly defines an “ever smoker” as someone who has smoked 100 or more cigarettes. Indirect evidence shows that smoking is the strongest predictor of AAA prevalence, growth, and rupture rates.1 There is a dose-response relationship, as greater smoking exposure is associated with an increased risk for AAA.1
Family History. Family history of AAA in a first-degree relative doubles the risk of developing AAA.25 The risk of developing an AAA is stronger with a female first-degree relative (odds ratio [OR], 4.32) than with a male first-degree relative (OR, 1.61).1,25 However, evidence is lacking on whether persons with family history experience a different natural history or surgical outcomes than those without such a history.1
SCREENING TESTS
The primary method of screening for AAA is conventional abdominal duplex ultrasonography.26 Screening with ultrasonography is noninvasive, is simple to perform, has high sensitivity (94%–100%) and specificity (98%–100%) for detecting AAA,1,27–31 and does not expose patients to radiation. Computed tomography is an accurate tool for identifying AAA; however, it is not recommended as a screening method because of the potential for harms from radiation exposure.1 Physical examination has been used in practice but has low sensitivity (39%–68%) and specificity (75%) and is not recommended for screening.32
SCREENING INTERVALS
Evidence is adequate to support 1-time screening for men who have ever smoked. All of the population-based randomized clinical trials of AAA screening used a 1-time screening approach; 7 fair- to good-quality cohort studies and 1 fair-quality case-control study (n = 6785) show that AAA-associated mortality over 5 to 12 years is rare (< 3%) in men with initially normal results on ultrasonography (defined as an AAA < 3 cm in diameter).1
TREATMENT
Treatment of AAA depends on aneurysm size, the risk of rupture, and the risk of operative mortality. Larger size is associated with an increased risk of rupture. The annual risk for rupture is nearly 0% for persons with AAAs between 3.0 and 3.9 cm in diameter, 1% for those with AAAs between 4.0 and 4.9 cm in diameter, and 11% for those with AAAs between 5.0 and 5.9 cm in diameter.1 Surgical repair is standard practice for men with an AAA of 5.5 cm or larger in diameter or an AAA larger than 4.0 cm in diameter that has rapidly increased in size (defined as an increase of 1.0 cm in diameter over a 1-year period). Endovascular aneurysm repair has become the most common approach for elective AAA repair. Open repair is a time-tested, effective treatment for AAA. In the United States, 80% of intact AAA repairs and 52% of ruptured AAA repairs are performed using endovascular aneurysm repair.1
The majority of screen-detected AAAs (≥ 90%) are between 3.0 and 5.5 cm in diameter and thus below the usual threshold for surgery. The current standard of care for patients with stable smaller aneurysms is to maintain ultrasound surveillance at regular intervals because the risk of rupture is small. Recommended surveillance intervals for monitoring the growth of small AAAs vary across guideline groups, and adherence with surveillance guidelines has been reported to be as low as 65%.1 Repairing smaller aneurysms with a lower risk of rupture increases the harms and reduces the benefits of screening.
SUGGESTIONS FOR PRACTICE REGARDING THE I STATEMENT
Potential Preventable Burden. The estimated prevalence of AAA in women is reportedly less than that in men.1 The Chichester trial reported a prevalence in women that was one-sixth of the prevalence in men (1.3% vs. 7.6%), and most AAA-related deaths occurred in women 80 years or older (70% vs. < 50% in men).33 In women, small AAAs have an increased risk of rupture and rupture at an older age than in men.1 Studies estimate that one-fourth to one-third of women have an AAA with a diameter below the current 5.5-cm threshold at the time of rupture.1
Potential Harms. Operative mortality associated with AAA is higher in women than in men. Women had higher 30-day mortality rates (2.31%) than men (1.37%) after endovascular aneurysm repair procedures (OR, 1.67 [95% CI, 1.38–2.04]) and open repair (5.37% vs 2.82%; OR, 1.76 [95% CI, 1.35–2.30]).1,34 Women also experience higher rates of other harms, such as major surgical complications and hospital readmission, after elective open repair or endovascular aneurysm repair compared with men.1
Current Practice. Evidence is insufficient to accurately characterize current practice patterns related to screening for AAA in women.
The standard of care for elective repair is that patients with an AAA of 5.5 cm or larger in diameter should be referred for surgical intervention with either open repair or endovascular aneurysm repair.1 This recommendation is based on randomized clinical trials conducted in men. The AAA size needed for surgical intervention in women may differ. As a result, guidelines from the Society for Vascular Surgery recommend repairing AAAs between 5.0 and 5.4 cm in diameter in women.26 However, concerns about poorer surgical outcomes in women, who have more complex anatomy and smaller blood vessels, have led some to caution against lowering the threshold for surgical intervention in women.1
This recommendation statement was first published in JAMA. 2019;322(22):2211–2218.
The “Update of Previous USPSTF Recommendation,” “Supporting Evidence,” “Research Needs and Gaps,” and “Recommendations of Others” sections of this recommendation statement are available at https://www.uspreventiveservicestaskforce.org/Page/Document/RecommendationStatementFinal/abdominal-aortic-aneurysm-screening1.
The USPSTF recommendations are independent of the U.S. government. They do not represent the views of the Agency for Healthcare Research and Quality, the U.S. Department of Health and Human Services, or the U.S. Public Health Service.

