Family physicians are experts in caring for patients with chronic diseases and recognizing how stress impacts health. These skills naturally complement one another, as attested by research into the connection between chronic disease and stress. Stressors often include adverse childhood experiences, which are traumatic events or chronic stressors experienced in childhood, such as physical or sexual abuse, witnessed domestic violence, loss or incarceration of a parent, and poverty.1 A history of adverse childhood experiences correlates with the development of diabetes mellitus, cardiovascular disease, asthma, and cancer.2,3 Stress in adulthood can precipitate or exacerbate mood disorders, functional gastrointestinal disorders, and chronic pelvic pain.4–6 When we make the stress-disease connection for our patients, they can benefit greatly from our compassionate support.
Identifying past or present stressors is an important first step that can be challenging for physicians because they must actively engage patients who are often hesitant to share these details.3 Physicians may be concerned about the time involved in asking these questions.7 Having a high index of suspicion is key, as is a willingness to gently explore the details of our patients' lives. This process does not have to be time-consuming, and the time spent is often justified by addressing important contributors to our patients' illnesses. The BATHE technique (i.e., inquiring about a patient's background, how it affects them, what troubles them most, what helps them handle it, and providing an empathetic response) is one way to explore these issues and typically takes less than five minutes (Table 1).7
TABLE 1. BATHE Technique for Addressing Health Risk Behavior
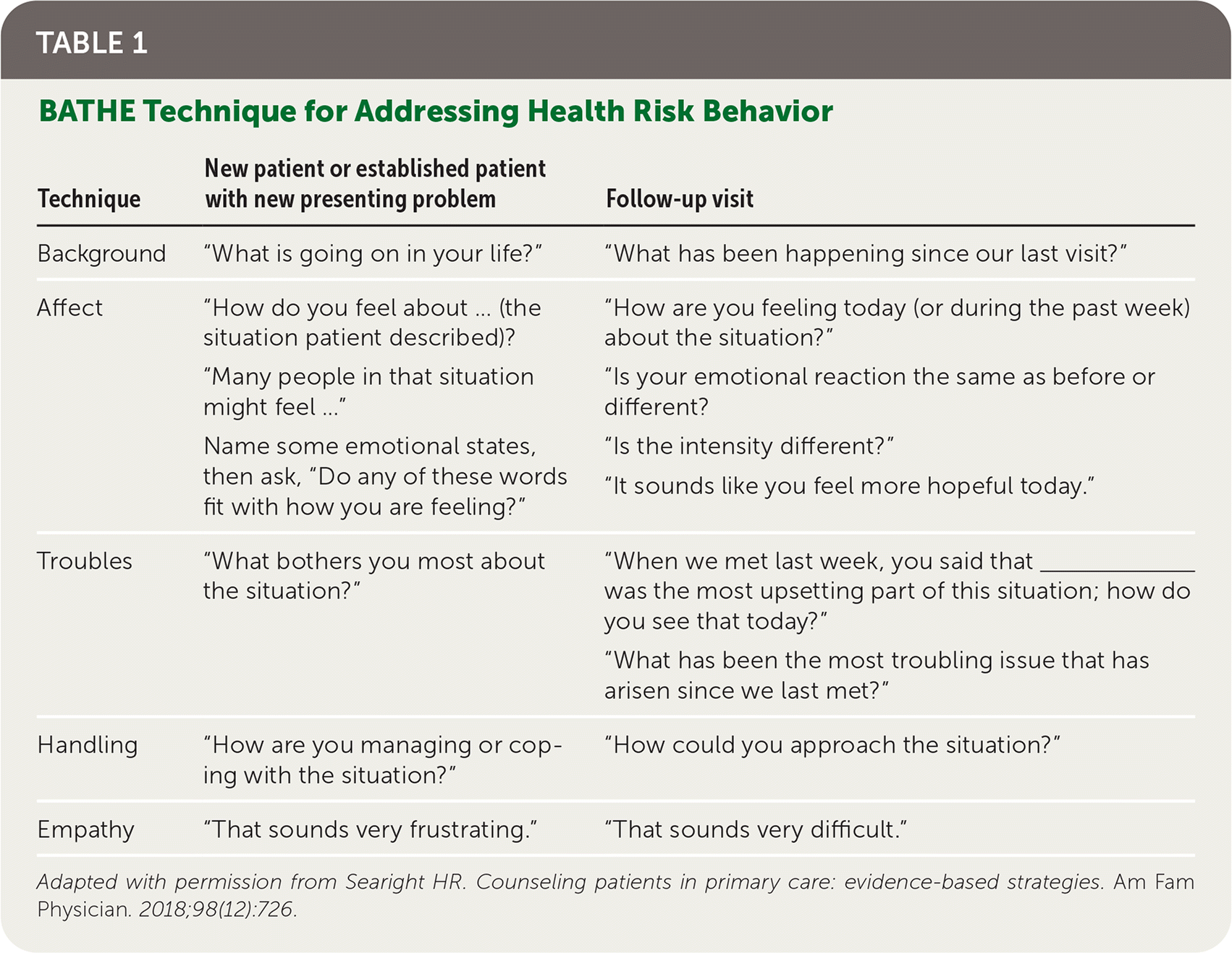
| Technique | New patient or established patient with new presenting problem | Follow-up visit |
|---|---|---|
| Background | “What is going on in your life?” | “What has been happening since our last visit?” |
| Affect | “How do you feel about … (the situation patient described)? “Many people in that situation might feel …” Name some emotional states, then ask, “Do any of these words fit with how you are feeling?” | “How are you feeling today (or during the past week) about the situation?” “Is your emotional reaction the same as before or different? “Is the intensity different?” “It sounds like you feel more hopeful today.” |
| Troubles | “What bothers you most about the situation?” | “When we met last week, you said that _______ was the most upsetting part of this situation; how do you see that today?” “What has been the most troubling issue that has arisen since we last met?” |
| Handling | “How are you managing or coping with the situation?” | “How could you approach the situation?” |
| Empathy | “That sounds very frustrating.” | “That sounds very difficult.” |
Adapted with permission from Searight HR. Counseling patients in primary care: evidence-based strategies. Am Fam Physician. 2018;98(12):726.
Tools for assessing current and past stressors can augment patient histories and can easily be incorporated into office workflows. The American Academy of Family Physicians' EveryONE Project includes screening tools for a wide range of social determinants of health, including food insecurity and financial strain.8 The Centers for Disease Control and Prevention has a toolkit to screen for intimate partner violence.9 The American Academy of Pediatrics' Resilience Project has tools to screen children, adolescents, and parents for adverse childhood experiences. 10 Once we identify issues of concern, we can work with patients to see which next steps, if any, they would like to pursue. A supportive ear may be all some patients want. For those interested in more support, we do not have to solve these challenges alone, but we do need to know where to refer patients in our communities. The Aunt Bertha website (https://www.auntbertha.com) is one starting point that provides a comprehensive list of resources by zip code for mental health care, housing assistance, legal aid, and more.
Emotional health and physical health are deeply intertwined, and patients who have experienced difficult events or persistent stressors may struggle to cope in a healthy way. Helping our patients recognize the connection between physical and mental well-being allows us to validate patients' underlying feelings and promote healthier coping practices. Meeting with a counselor, choosing a positive outlook, engaging in relaxation techniques, and making healthy lifestyle choices can boost resilience and wellness.11 Discussion of this mind-body connection should not be confused with dismissing patients' symptoms as being “all in their head.” Instead, this connection is ideally a path to patient empowerment. When patients believe they are heard and are provided with resources to address their challenges, meaningful healing may be more likely to occur.
A deeper understanding of these stressors may also strengthen our relationships and help us to maintain positive regard for patients who may be among our most challenging to treat. If we are to fully care for the whole person as family physicians, then responding to the stressors our patients face is critical to providing holistic, compassionate, and effective care.
Editor's Note: Dr. Middleton is a contributing editor for AFP.

